Chapter Five The physics of anatomy
Joint movement
Introduction
In Chapter 4, we encountered a wide variety of joint types and also explored some ways in which the basic templates are modified from joint to joint to meet the specific needs of regional biomechanics. Now, we shall explore these variations and the strictures they place on movement in more detail.
Whilst we do this, there are two fundamental principles that we should keep in mind.
Stability and mobility are mutually exclusive
If you take, as an example, the shoulder and the hip, both are ball and socket joints and both are moved by similar groups of muscles; unsurprising when you consider man’s evolution from quadrupedal forebears. However, the hip has a high degree of stability at the expense of the mobility that is demonstrated by the shoulder; by contrast, only professional contortionists can scratch their back with their toes and walking on one’s hands is difficult and tiring.
Degrees of freedom
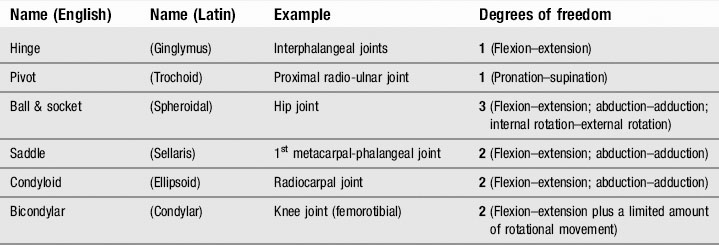
As a rule, each class of synovial joint has a set number of degrees of freedom and these are given in Table 5.1. Plane (gliding) joints can translate, although these movements are usually heavily curtailed by ligamentous attachments. Usually plane joints such as the zygapophyseal, intertarsal and intercarpal joints have two degrees of translational freedom, although some authorities declare joint gapping to represent a third degree of freedom.
Arthrokinematics
Roll and glide
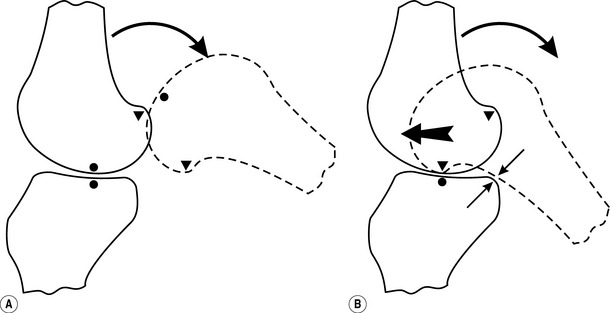
So far, we have considered joint movement in terms of pure rotation; of course, although this model is entirely acceptable from a functional standpoint, it does not reflect how joints actually work. If a joint were to rotate and only rotate, it would simply roll out of its socket and dislocate (Fig. 5.1A).
Obviously, this does not happen; instead, a combination of the ligamentous attachments, the line of force of the articular muscles and the lubricating effect of the synovial fluid allow the joint to roll and simultaneously slide (or glide), so that the joint moves in the desired fashion without losing its articular integrity (Fig. 5.1B).
Spin
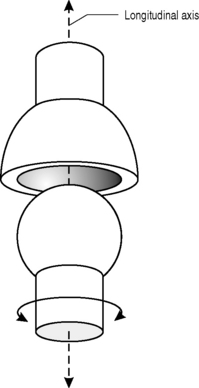
There is an additional intraarticular motion that we need to consider: spin. This is rotary motion of the distal part of the kinematic chain about the longitudinal axis of the proximal part – a concept better understood if visualized (Fig. 5.2).
Spin can occur alone or in conjunction with roll and glide: in pronation–supination of the forearm, it occurs independently; in flexion–extension of the knee it accompanies roll and glide and, as we shall subsequently discover, plays an important part in the knee’s stability.
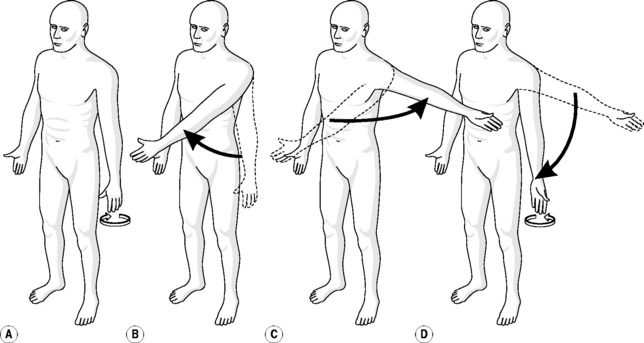
When roll, glide and spin act together, it can have an interesting effect on joint motion. For example, we can externally rotate the shoulder by the simple action of resting our palm against the thigh and then turning the palm outwards so that it faces forwards; this motion is a combination of roll and glide. We can achieve the same effect by starting in the same position and then flexing the shoulder to 90°, horizontally abducting it by 90° and then adducting it back to our thigh (Fig. 5.3). The translation of the glide component, in conjunction with the rotation of the roll and spin components has caused an external rotation of 90°; the palm is now facing forwards, it is no longer resting against our thigh even though no specific rotation has taken place.
Joint features
Most of our consideration of joints so far has been generalized; however, there are specific joints that have special or unusual features or are of particular clinical interest and, in this section, we shall consider them in turn.
The lower extremity
Knee
The knee is the largest joint in the body. It is a remarkably stable joint; this ability to bear several times the body’s own weight arises from what happens when the joint is fully extended. To understand this, there is a new concept that needs to be introduced, the close-packed position (Fig. 5.4). The fit of reciprocal convex–concave surfaces is precise only at one end of the most common excursion of the joint, which is the key feature of the close-packed position. In all other positions the surfaces are not fully congruent, and the joint is said to be loose-packed.
As the knee approaches full extension, the femur rotates internally with respect to the tibia; the last 10° of extension is accompanied by approximately 6° of rotation. This rotation seats the femoral condyles in the rings of the medial and lateral menisci, also bringing the ligaments to tension.
The upper extremity
Shoulder
The shoulder is the most complicated joint in the body. It is in fact a complex of three joints (glenohumeral, acromioclavicular and sternoclavicular) and one articulation (the movement of the scapula across the superior seven ribs). It also contains over two dozen bursae, a similar number of ligaments and is controlled by a dozen or so muscles. Somewhat surprisingly, the whole complex is uniquely controlled by a single nerve root (C5) – every other joint has dual supply; the hip is controlled by three contiguous levels.
The spine and pelvis
where R is the resistance to compression and Nc is the number of curves.
SCOLIOSIS
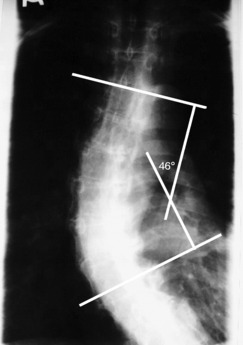
As well as the normal anteroposterior curves of the spine, a significant number of people develop a lateral curve(s) – scoliosis. These are generally defined as C-curves (convex either to the left or right) or S-curves (one curve convex in one direction followed by a second curve convex to the other side). A scoliosis is defined clinically by its range, the upper and lower limits; its angulation, most commonly measured by the Cobb angle (Fig. 5.5); and its apex.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree




 CLINICAL FOCUS
CLINICAL FOCUS CLINICAL FOCUS
CLINICAL FOCUS CLINICAL FOCUS
CLINICAL FOCUS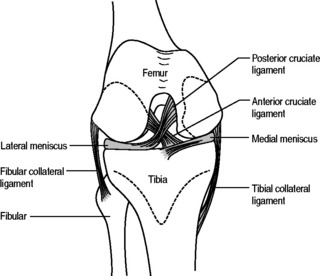
 CLINICAL FOCUS
CLINICAL FOCUS CLINICAL FOCUS
CLINICAL FOCUS


 DICTIONARY DEFINITION
DICTIONARY DEFINITION