and John E. Skandalakis1
(1)
Centers for Surgical Anatomy and Technique, Emory University School of Medicine Piedmont Hospital, Atlanta, GA, USA
Abstract
The stomach is part of two almost-separate organ systems, each with its special pathology and surgical approach. The “proximal gastric surgical unit” contains the proximal stomach, distal esophagus, and esophageal hiatus of the diaphragm; the “distal gastric surgical unit” includes the gastric antrum, pylorus, and the first part of the duodenum. Identification of the basic configuration and variations of the vagus nerves is essential for successful vagotomy.
Step-by-step technique for gastrostomy, gastrojejunostomy, and pyloroplasty is presented. Guidelines for successful gastrectomies are detailed. Most gastric neoplasms are malignant; a perforated gastric ulcer can be of benign or malignant origin.
Anatomy
Two Gastric Units
From the viewpoint of a surgeon, the stomach is part of two almost-separate organ systems, each with its special pathology and surgical approach. The first can be called the “proximal gastric surgical unit.” It contains the proximal stomach, distal esophagus, and esophageal hiatus of the diaphragm (Fig. 7.1). The second is the “distal gastric surgical unit,” which includes the gastric antrum and pylorus, together with the first part of the duodenum (Fig. 7.2).
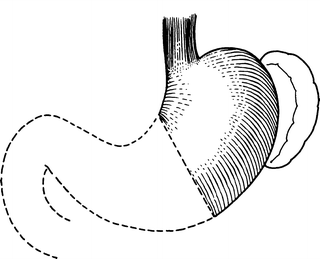
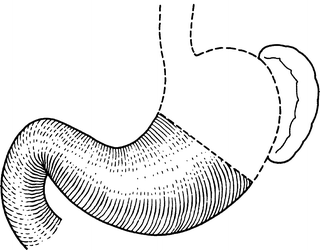

Figure 7.1.
The proximal gastric surgical unit. The two ends of the stomach acquire different lesions, and operations require different methods (By permission of JE Skandalakis, SW Gray, and JR Rowe. Anatomical Complications in General Surgery. New York: McGraw-Hill, 1983).

Figure 7.2.
The distal gastric surgical unit. Most gastric surgery takes place in this area (By permission of JE Skandalakis, SW Gray, and JR Rowe. Anatomical Complications in General Surgery. New York: McGraw-Hill, 1983).
Proximal Gastric Surgical Unit
The length of the abdominal esophagus ranges from 0.5 to 2.5 cm. Its relations with surrounding structures are:
ANTERIOR: Posterior surface of left lobe of liver
POSTERIOR: Right crus of diaphragm, and aorta
RIGHT: Caudate (spigelian) lobe of liver
LEFT: Fundus of stomach
The cardiac orifice is the gastroesophageal junction. The fundus, for all practical purposes, is the upper part of the body which, in the supine position, augments upward. The body is the part of the stomach between the antrum and the fundus.
Distal Gastric Surgical Unit
The gastric antrum, pylorus, and first portion of the duodenum form a unit from an embryologic, physiologic and, certainly, a surgical viewpoint.
Gastric Antrum
In the opened stomach, the antrum is easily distinguished from the body of the stomach by its mucosa, which is flatter and without rugae. It is histologically distinct, being without chief or parietal (acid-producing) cells. The margin of the antrum is irregular, but definite. Externally the antrum is difficult to demarcate. The boundary on the lesser curvature usually lies at the incisura angularis; it is usually found in textbook drawings, but in the operating room it is inconstant and often absent.
Surgeons not planning a gastrotomy to locate the antral margin can use the “crow’s foot” of the anterior descending vagal trunk as a landmark. The antrum can be expected to begin 3–4 cm cranial to the crow’s foot, about 8–10 cm proximal to the pylorus. On the greater curvature, there is no good landmark. In most cases the boundary extends from a point on the lesser curvature 2/5 of the way from the pylorus to the esophagus to a point on the greater curvature 1/8 of the distance from the pylorus to the esophagus.
Pylorus
The pylorus is a region of the stomach variously called the pyloric canal, pyloric ring, and pyloric valve. Proximally, it merges into the gastric antrum without a definite external boundary; distally, it ends abruptly at the thin-walled duodenum.
At the pyloroduodenal junction, the continuity of the circular musculature is interrupted by an annular septum that arises from the connective tissue of the submucosa. Proximal to this ring, the circular muscle layer is thickened to form the pyloric sphincter. Distal to the ring, the circular muscle coat at the duodenum is thinner.
First Part of the Duodenum
The distal gastric surgical unit includes only the first 2.5 cm of the duodenum (for more information, see Chap. 8.)
Relations of the Distal Gastric Surgical Unit
Posteriorly the unit is related to the:
Floor of lesser sac
Transverse mesocolon
Head and neck of pancreas
Aorta and celiac trunk and its branches
Celiac ganglion and plexus
Hepatic triad
Gastroduodenal artery
Anteriorly the unit is related to the:
Anterior abdominal wall
Medial segment of left lobe and anterior segment of right lobe of liver
Transverse mesocolon
Neck of gallbladder (if stomach is empty)
Gastric Wall
The gastric wall consists of the serosa, the muscular layer, submucosal layer, and mucosal layer.
The distal esophagus is lined by stratified squamous epithelium; the abdominal esophagus is lined with mucous cells. Simple columnar cells compose the mucosal layer of the cardia. The mucosal layer of the fundus and body consists of two types of cells: parietal (oxyntic) acid-secreting cells and chief pepsin-secreting cells.
Ligaments
Hepatogastric Ligament (Lesser Omentum)
The hepatogastric ligament is the proximal part of the lesser omentum. It extends from the porta hepatis to the lesser curvature of the stomach and upward as the ventral mesentery of the abdominal esophagus. The ligament contains:
REGULARLY: Left gastric artery and vein; hepatic division of the anterior vagal trunk; anterior and posterior gastric divisions of the vagal trunks (nerves of Latarjet); lymph nodes and vessels.
OCCASIONALLY: An aberrant left hepatic artery (23 % of individuals) in proximal part of hepatogastric ligament; distally and to the right, branches of the right gastric artery and vein. In this region also are the common hepatic artery and portal vein; here they rise ventrally to gain their positions in the hepatoduodenal segment of the lesser omentum.
Hepatoduodenal Ligament
The hepatoduodenal ligament is the distal part of the lesser omentum, extending from the liver to the first 2.5 cm of the duodenum. The free edge envelops the hepatic triad (the proper hepatic artery, portal vein, and extrahepatic biliary ducts) as well as the hepatic plexus and lymph nodes.
Gastrocolic Ligament
The gastrocolic ligament is a portion of the greater omentum passing from the greater curvature of the stomach and the first part of the duodenum to the transverse colon.
Gastrophrenic Ligament
The gastrophrenic ligament is continuous with the hepatogastric ligament to the left of or, perhaps, opposite the esophagus. It has an avascular area through which the surgeon’s finger can safely pass and through which a Penrose drain can be inserted around the cardia to pull down the esophagus. This is a useful maneuver in vagotomy. The upper part of the ligament is avascular, and the lower part contains short gastric arteries and veins, and lymph nodes.
Vascular System of the Stomach (Fig. 7.3)
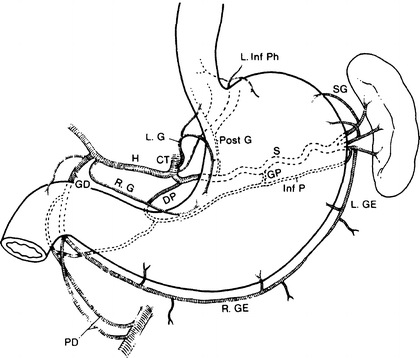
Figure 7.3.
The arterial supply to the stomach: L. Inf Ph left inferior phrenic artery, SG short gastric artery, L. GE left gastroepiploic artery, R. GE right gastroepiploic artery, S splenic artery, GP great pancreatic artery, Inf P inferior pancreatic artery, PD pancreaticoduodenal artery, DP dorsal pancreatic artery, GD gastroduodenal artery, R. G right gastric artery, H hepatic artery, CT celiac trunk, L. G left gastric artery, Post G posterior gastric artery (By permission of JE Skandalakis, SW Gray, and JR Rowe. Anatomical Complications in General Surgery. New York: McGraw-Hill, 1983).
Arterial Supply
Following is a summation of all the arteries that supply the stomach. Each of the principal arteries of supply originates from the celiac trunk.
Left gastric
Ascending branch (gives rise to esophageal)
Descending branch (gives rise to gastric)
Hepatic
Right gastric
Gastroduodenal
Anterior superior pancreaticoduodenal
Retroduodenal
Posterior superior pancreaticoduodenal
Supraduodenal
Right gastroepiploic (major branches)
Splenic
Posterior gastric
Short gastrics
Left gastroepiploic (major branches)
The stomach can survive after ligation of all but one of its primary arteries, and extragastric ligation will not control bleeding from a gastric ulcer.
Venous Drainage
The veins, for all practical purposes, follow the arteries.
Lymphatic Drainage
The lymphatic drainage of the stomach consists of four zones as follows (Fig. 7.4):
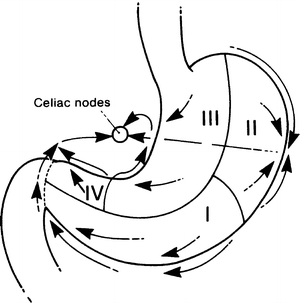

Figure 7.4.
Diagram of the lymphatic drainage of the stomach. Most of the drainage finds its way to the celiac nodes: the “vortex of the metastatic whorl” (By permission of JE Skandalakis, SW Gray, and JR Rowe. Anatomical Complications in General Surgery. New York: McGraw-Hill, 1983).
Zone I (inferior gastric): drains into the subpyloric and omental nodes
Zone II (splenic): drains into the pancreaticosplenic nodes
Zone III (superior gastric): drains into the superior gastric nodes
Zone IV (hepatic): drains into the suprapyloric nodes
Parasympathetic Nerves (Vagus Nerves)
The left and right vagus nerves descend parallel with the esophagus and contribute to a rich external esophageal nerve plexus between the level of the tracheal bifurcation and the level of the diaphragm. From this plexus, two vagal trunks—anterior and posterior—form and pass through the esophageal hiatus of the diaphragm. Each trunk subsequently separates into two divisions (Fig. 7.5).
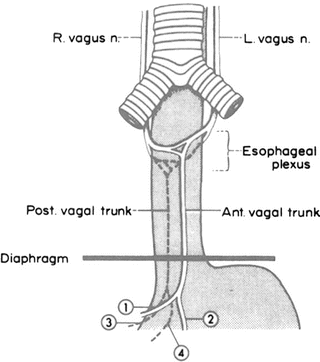

Figure 7.5.
The terminology of vagal structures of the thorax and abdomen. In this example, two vagal trunks pass through the hiatus to enter the abdomen. 1 = hepatic division; 2 = anterior gastric division; 3 = celiac division; 4 = posterior gastric division (By permission of JE Skandalakis, JS Rowe, and SW Gray. Surgery 75(2):233–237, 1974).
From the anterior vagal trunk, the hepatic division passes to the right in the lesser omentum, branching before it enters the liver. One branch turns downward to reach the pylorus and, sometimes, the first part of the duodenum. The second division, the anterior gastric, descends along the lesser curvature of the stomach, giving branches to the anterior gastric wall.
From the posterior trunk arise the celiac division, which passes through the celiac plexus, and the posterior gastric division, which supplies branches to the posterior gastric wall.
Identification of Vagal Structures at the Hiatus
The basic configuration and variations of the vagus nerves at the esophageal hiatus are well known, but the thoracic pattern is not visible to the abdominal surgeon, who must proceed on the basis of the structures that can be seen. A study of components of the esophageal hiatus in 100 cadavers found the following:
Two vagal structures only (88 %) (Fig. 7.5). The usual structures at the esophageal hiatus are the anterior and posterior vagal trunks, which have not yet split to form the four typical divisions discussed above. Both trunks are usually to the right of the midline of the esophagus. The posterior trunk lies closer to the aorta than to the esophagus (Fig. 7.6).
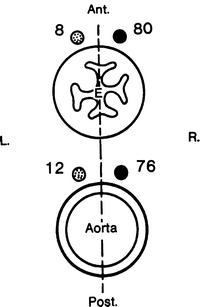
Figure 7.6.
The relation of the anterior and posterior vagal trunks to the aorta and the esophagus, showing the number of specimens with vagal trunks lying to the right or left of the midline. In most but not all of the 88 specimens, the trunks are to the right of the midline. Note that the anterior trunks are closer to the esophagus than are the posterior trunks (By permission of JE Skandalakis, JS Rowe, and SW Gray. Surgery 75(2):233–237, 1974).
Four vagal structures (7 %) (Fig. 5.16a). The four divisions of the vagal trunks (hepatic, celiac, anterior gastric, and posterior gastric) appear when division has occurred above the diaphragm.
More than four structures (5 %). When there are more than four structures at the hiatus, these may be divisions and branches of divisions (Fig. 5.16b) (the anterior and posterior trunks lie entirely within the thorax), or elements of the esophageal vagal plexus (Fig. 5.16c) (the anterior and posterior trunks lie entirely within the abdomen).
Distribution of the Vagus Nerves to the Stomach
Anterior Gastric Division
The separation of the anterior gastric and hepatic divisions occasionally occurred above the diaphragm, but the divisions usually lay on the abdominal esophagus or the cardia.
In almost all cases, a major branch of the anterior gastric division formed the principal anterior nerve of the lesser curvature (anterior nerve of Latarjet). It usually lay from 0.5 to 1.0 cm from the lesser curvature.
From 2 to 12 branches pass from the principal nerve to the stomach wall. The average in the subjects in the above-mentioned study was six.
Constant landmarks on the stomach are difficult to obtain. The position of the incisura angularis often has to be estimated. Although we have often seen the nerve of Latarjet branch in the “crow’s foot” formation, this pattern is far from constant, being equivocal in some cases and absent in many (Fig. 7.7).
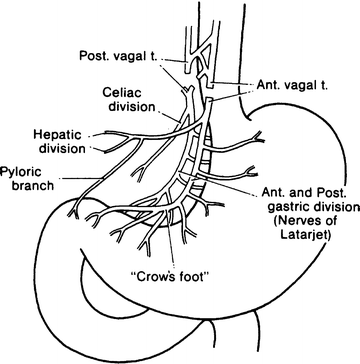

Figure 7.7.
Truncal vagotomy results in vagal denervation of all abdominal organs. A concomitant drainage procedure is required for gastric stasis (By permission of JE Skandalakis, SW Gray, and JR Rowe. Anatomical Complications in General Surgery. New York: McGraw-Hill, 1983).
Hepatic Division
The hepatic division of the anterior vagal trunk usually separates from the anterior gastric division at the level of the abdominal esophagus (Fig. 7.8). It lies between the leaflets of the avascular portion of the hepatogastric ligament. It is frequently found in multiple branches that are usually closely parallel.
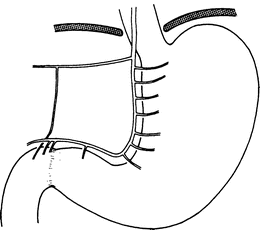

Figure 7.8.
“Typical” distribution of anterior gastric and hepatic divisions of the vagus (modified by permission of JE Skandalakis, SW Gray, RE Soria, et al. Am Surg 46(3):130–139, 1980).
Posterior Gastric Division
In most subjects, the posterior gastric division forms the principal posterior nerve of the lesser curvature (posterior nerve of Latarjet). As a rule, the posterior nerve appears to terminate slightly higher on the lesser curvature and possesses fewer gastric branches than does the anterior nerve. In no case has a posterior nerve been observed to reach the duodenum.
Celiac Division
The celiac division is the largest of the four vagal divisions. It lies in the gastropancreatic peritoneal fold. In all cases, it is single and leads directly to the celiac plexus. The celiac division may follow the left gastric artery or the right crus of the diaphragm or take an intermediate position in the triangle bounded by the artery, the crus, and the right margin of the stomach.
Sympathetic Nerves
The sympathetic chains, the thoracic splanchnic nerves containing afferent and efferent fibers, and the celiac ganglia form the basic elements for the sympathetic innervation of the stomach and duodenum.
Technique
Gastrostomy
Stamm Gastrostomy
The surgeon chooses the type of incision, and a good preoperative evaluation helps greatly in the decision. The authors favor a small upper-midline incision, which may be extended, if necessary.
Step 1. With Babcock clamps, elevate the anterior wall of the stomach approximately 6–10 cm from the gastroduodenal junction. Place and tie two purse-string sutures of 3-0 silk or Vi cryl 120° from each other (Fig. 7.9).
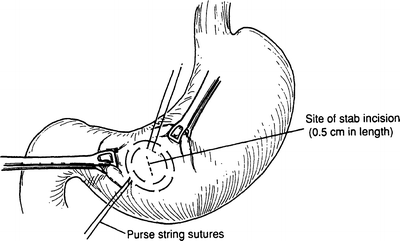
Figure 7.9.
Purse-string sutures at anterior wall of stomach.
Step 2. Make a very small stab incision (usually 0.5 cm in length) in the center of the designated area of the purse-string sutures and insert an 18–22 Foley balloon catheter (Fig. 7.9).
Step 3. Insert the catheter and inflate the balloon. Tie the inner purse string very tightly, then tie the outer purse string; do not cut it or remove the needles (Fig. 7.10).
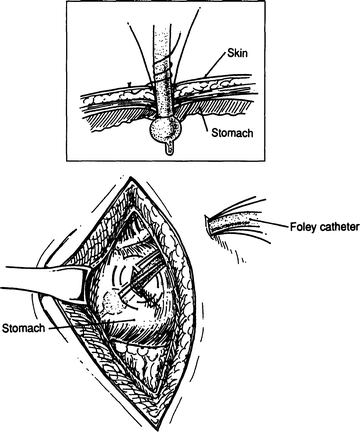
Figure 7.10.
Placement of catheter (Inset: detail of catheter and balloon).
Step 4. Pull the catheter until it reaches the gastric mucosa at the gastric stab wound. Use gentle movements to ensure that the balloon is well attached to the gastric mucosa. Stitch the purse-string sutures to the anterior abdominal wall. To make certain that dead space does not exist, use a third 3-0 silk suture to fix the gastric wall to the anterior abdominal wall. Close the skin and use a 2-0 silk suture to secure the gastrostomy tube to the skin of the abdominal wall.
Note:
✔ There are other types of gastrostomies, including Witzel and Janeway. They are seldom used today.
Gastrojejunostomy
Retrocolic
Step 1. Make an upper-midline incision or incision of the surgeon’s choice.
Step 2. The location of the stoma should be close to the pylorus at the most dependent area of the greater curvature. Place a Babcock clamp in an oblique fashion at the lesser curvature and at the greater curvature (Fig. 7.11).
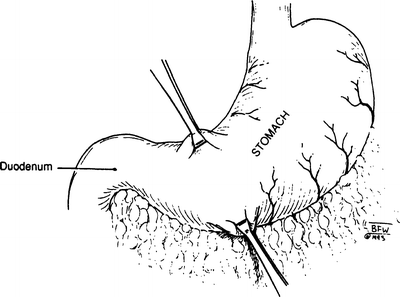
Figure 7.11.
Clamps placed at lesser curvature.
Step 3. Lift the transverse colon to evaluate its mesocolon. Protect the middle colic artery by noting its location. Identify an avascular area and incise it; in most cases, it will be to the left of the middle colic artery. The posterior wall of the stomach projects through the opening in such a way that the lesser curvature is located at the lowest corner of the mesenteric opening. Using interrupted 4-0 silk, suture the mesentery to the gastric wall at this point (Fig. 7.12).
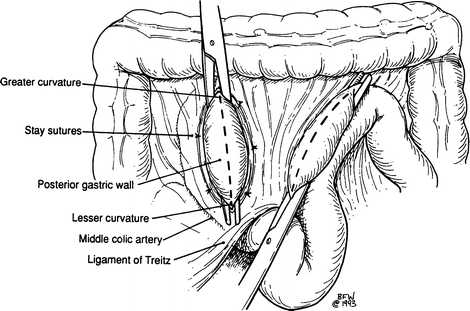
Figure 7.12.
Locating the avascular area prior to incision.
Step 4. Again using interrupted 4-0 silk sutures, attach to the gastric wall (proximal to the lesser curvature) a jejunal loop that is approximately 15 cm distal to the ligament of Treitz. Anastomose the loop to the posterior gastric wall in two layers using a running 3-0 chromic suture for the mucosal layer and a 3-0 silk interrupted suture for the seromuscular layer (Figs. 7.13, 7.14, and 7.15).



