and John E. Skandalakis1
(1)
Centers for Surgical Anatomy and Technique, Emory University School of Medicine Piedmont Hospital, Atlanta, GA, USA
Abstract
Successful esophageal surgery requires knowledge of the anatomy of the esophagus and mediastinum. The esophageal wall has two anatomically weak areas. Step-by-step technique for repair of pharyngoesophageal diverticulum, achalasia, and cardiospasm is detailed, along with transhiatal esophagectomy [including preparation of the gastric conduit (neoesophagus) and anastomosis].
Depending on presentation, surgical resection for carcinoma of the esophagus can be performed by Ivor Lewis, Ivor Lewis-McKeown (three-stage), or left thoracoabdominal esophagectomy. The colon may be harvested and used as an esophageal substitute in situations where the stomach is not usable.
Anatomy
General Description of the Esophagus
Length of the Esophagus
The esophagus is about 25 cm in length. The most useful reference point is the upper incisors, which are about 15 cm above the pharyngoesophageal junction; if the external nares are included, 2–3 cm must be added. In defining the esophagus, it is adequate to divide it into cervical, thoracic, and abdominal segments.
Constrictions of the Esophagus
Major Constrictions
There are three major constrictions:
The cricopharyngeal or pharyngoesophageal constriction (diameters 1.7 × 2.3 cm).
The bronchoaortic constriction. Anatomically there are two separate constrictions: the aortic at the level of T4 with diameters of 1.9 × 2.3 cm and the bronchial at the level of T5 with diameters of 1.7 × 2.3 cm.
The diaphragmatic constriction at the level of T9 or T10 with a diameter of 2.3 cm.
These constrictions define two regions of dilatation: superior (between the cricopharyngeal and bronchoaortic constrictions) and inferior (between the bronchoaortic and diaphragmatic constrictions).
Minor Constrictions (Seen Occasionally)
A retrosternal constriction may lie between the pharyngoesophageal and the aortic constrictions.
A cardiac constriction may lie behind the pericardium and is produced if right atrial enlargement is present, as in mitral stenosis.
A supradiaphragmatic constriction may be produced by a tortuous, arteriosclerotic aorta.
Curves of the Esophagus
The esophagus has three gentle curves: in the neck, behind the left primary bronchus; below the bifurcation of the trachea; and behind the pericardium. In terms of vertebral levels, the esophagus is to the left of the midline at T1, to the right at T6, and to the left again at T10.
Remember the three Cs: three constrictions and three curves. Most esophageal pathology (e.g., lodgment of foreign bodies, burns from caustic chemicals, and cancer) is located at or close to these constrictions. The bronchoaortic constriction is the most frequently involved.
Topography and Relations of the Esophagus
The tubercle of the cricoid cartilage is the single constant landmark of the upper esophageal opening.
Pharyngoesophageal Junction
The muscular pharyngeal wall is formed by three overlapping muscles: the superior, middle, and inferior pharyngeal constrictors. The inferior constrictor muscle (Fig. 6.1) blends inferiorly with the sphincter-like transverse cricopharyngeal muscle, which blends with the circular, muscular esophageal wall. Between the two parts of the cricopharyngeal muscle is the weak area (triangle) of Killian. There is another weak area between the lower transverse and the muscular coat of the esophagus (Fig. 6.1). These weak areas may become the site of acquired pulsion diverticula (Zenker’s, above; Laimer’s, below). They also are the sites of possible perforation by an esophagoscope.
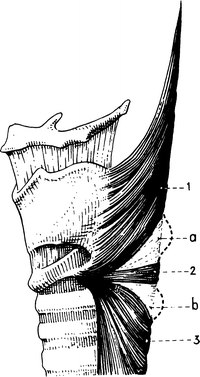

Figure 6.1.
The lateral aspect of the pharyngoesophageal junction showing (a) the upper weak area; (b) the lower weak area; (1) the oblique fibers of the inferior constrictor muscle; (2) the cricopharyngeal muscle; (3) the muscularis of the esophagus (From J Terracol and RH Sweet. Diseases of the Esophagus. Philadelphia: Saunders, 1958).
Two anatomical entities at this point contribute to narrowing of the esophageal lumen: internally the hypopharyngeal fold and externally the cricopharyngeal muscle. At this location perforation by instruments, lodging of foreign bodies, spasm, and neoplasms tend to occur.
The cricopharyngeal muscle and the lower border of the cricoid cartilage demarcate the end of the pharynx and the start of the esophagus. The so-called inferior constrictor of the pharynx, the cricopharyngeal muscle, originates from the thyroid and cricoid cartilages. It is composed of two parts, the upper oblique and the lower transverse; the lower transverse is probably the cricopharyngeal sphincter.
Logically, a diverticulum above the transverse portion of the cricopharyngeal muscle should be recognized as pharyngeal, and one originating below as esophageal. However, in the literature this distinction is not always made (Fig. 6.2). For example, a diverticulum originating above the junction, which should be called Zenker’s, may instead be referred to as pharyngoesophageal or esophageal, causing confusion.
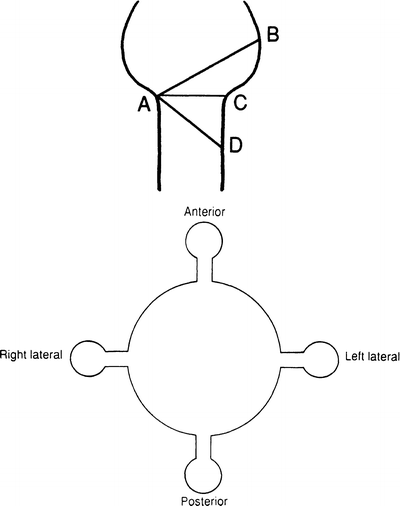

Figure 6.2.
Top: highly diagrammatic presentation of the musculature of the pharyngoesophageal junction. AB = oblique muscle; AC = transverse muscle; AD = muscular coat. Sites of potential diverticula are as follows: ABC = Killian’s triangle (1908) = pharyngeal diverticulum; ABD = Zenker’s diverticulum (1878) = pharyngoesophageal diverticulum; ACD = esophageal weakness = esophageal diverticulum. A congenital diverticulum has a wide neck and includes all layers. An acquired diverticulum has a narrow neck and no muscular coat. Bottom: highly diagrammatic presentation of diverticula. Note: The anterior diverticulum is a rare congenital condition.
Cervical Esophagus
The cervical esophagus is approximately 5–6 cm long and extends from C6 to T1, or from the cricoid cartilage and cricopharyngeal muscle to the thoracic inlet at the level of the sternoclavicular joints. The carotid tubercle (of Chassaignac), which is the palpable anterior tuberosity of the transverse process of C6, is a good anatomical landmark. It projects somewhat to the left of the trachea, and incisions are commonly made on this side to approach the esophagus.
Anteriorly, the cervical esophagus is covered by the larynx and trachea.
Anterolaterally, there are four anatomical entities related to the esophageal wall on each side (see Fig. 2.15). From the periphery inward they are: the carotid sheath, the inferior thyroid artery, the lobe of the thyroid gland, and the recurrent laryngeal nerve. Also related to the distal cervical esophagus on the left side is the thoracic duct.
Posteriorly, the cervical esophagus is related to: the alar fascia, the prevertebral fascia, the longissimus cervicis muscle, and the vertebrae.
Between the alar fascia and the prevertebral fascia is the retrovisceral space, the so-called danger space that extends down the mediastinum and ends approximately at the level of T4.
Pretracheal Space
The space in front of the trachea is not related directly to the esophagus. It is related clinically, however, since perforations of the anterior esophageal wall may open into the pretracheal space and therefore the mediastinum, producing a serious or even fatal mediastinitis.
Thoracic Esophagus
The thoracic portion of the esophagus extends from the level of T1 to T10 or T11.
Successful esophageal surgery requires knowledge of the anatomy of the mediastinum; we remind the reader that the thoracic esophagus is located in the superior and posterior mediastinum. The key structure of the superior mediastinum is the aortic arch. The posterior mediastinum displays venous structures on the right and arterial structures on the left.
The anterior relations of the thoracic esophagus from above downward consist of the following structures: trachea and aortic arch, right pulmonary artery, left main bronchus, esophageal plexus below the tracheal bifurcation, pericardium and left atrium, anterior vagal trunk, esophageal plexus, and esophageal hiatus.
The posterior relations of the thoracic esophagus are: vertebral column, longus colli muscle, right posterior intercostal arteries, left thoracic duct obliquely from T7 to T4, right pleural sac, azygos vein, hemiazygos vein, accessory hemiazygos vein, anterior wall of the aorta, esophageal plexus of the vagus nerve below the tracheal bifurcation, and sometimes the posterior vagal trunk.
The lateral relations on the right are mediastinal pleura, azygos vein, right main bronchus, root of right lung, right vagus nerve, and esophageal plexus (Fig. 6.3).
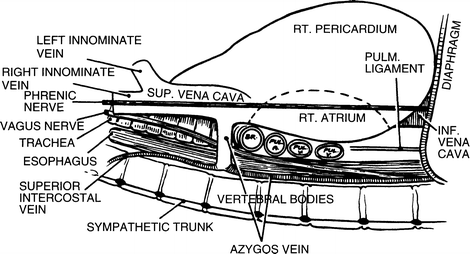

Figure 6.3.
Highly diagrammatic view of the right mediastinum showing the disposition of its contents. BR bronchus, PUL pulmonary (By permission of JE Skandalakis, SW Gray, and LJ Skandalakis. In: GG Jamieson. Surgery of the Esophagus. Edinburgh: Churchill Livingstone, 1988, pp. 19–35).
The lateral relations on the left are aortic arch, left subclavian artery, left recurrent laryngeal nerve, left vagus nerve, thoracic duct from T4 to C7, pleura, and descending thoracic aorta (Fig. 6.4).
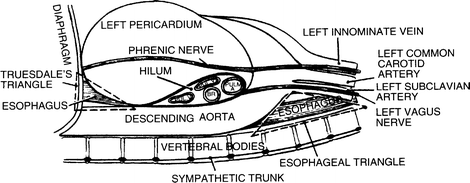

Figure 6.4.
Highly diagrammatic view of the left mediastinum showing the disposition of its contents. BR bronchus, PUL pulmonary (By permission of JE Skandalakis, SW Gray, and LJ Skandalakis. In: GG Jamieson. Surgery of the Esophagus. Edinburgh: Churchill Livingstone, 1988, pp. 19–35).
The following structures are between the esophagus and the left mediastinal pleura: left common carotid artery, left subclavian artery, aortic arch, and descending aorta. The entire length of the thoracic esophagus is directly related to the right mediastinal pleura except where the arch of the azygos vein crosses above the right main bronchus.
Surgical Considerations
✓ From a surgical standpoint, lesions of the upper half of the thoracic esophagus should be explored through a right thoracotomy to avoid technical problems with the aortic arch. Lesions of the lower half of the thoracic esophagus can be explored through a left or a right thoracotomy.
✓ With the right-sided approach, the azygos vein should be ligated and divided where it crosses the right wall of the esophagus to empty into the posterior wall of the superior vena cava. The azygos vein may be ligated with impunity. However, ligation of the superior vena cava between the atrium and the azygos vein cannot be tolerated if the azygos vein has been ligated.
✓ The esophageal triangle in the left side of the mediastinum is formed by the descending arch of the aorta, the subclavian artery, and the vertebral column. The floor of the triangle is formed by the left mediastinal pleura beneath which the esophagus is located (Fig. 6.4).
✓ The lower end of the thoracic esophagus, which is covered by pleura, may be found in the triangle of Truesdale. The triangle of Truesdale is formed by the diaphragm below, the pericardium above and anteriorly, and the descending aorta posteriorly (Fig. 6.4). The posterior approximation of the right and left pleurae between the esophagus and the aorta forms the so-called meso-esophagus. The right pleura is in contact with the lower one-third of the esophagus, almost to the diaphragmatic hiatus. This proximity of the right pleura to the hiatus introduces the risk of pneumothorax during abdominal operations on the hiatus. The anterior approximation of the two pleurae is at the sternal angle (see Fig. 5.10).
Anatomic Weak Points
Two anatomically weak areas of the esophageal wall—one above and one below the cricoid muscle—have been mentioned. They can become the sites of pulsion diverticula. Another weak area, the left lateral posterior wall of the esophagus near the diaphragm, is occasionally the site of spontaneous idiopathic rupture of the healthy esophagus.
Abdominal Esophagus and Gastroesophageal Junction (Fig. 6.5)
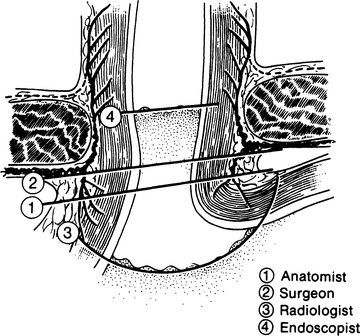
Figure 6.5.
Views of the “gastroesophageal junction” by four specialties. Each is correct (By permission of JE Skandalakis, SW Gray, and JR Rowe. Anatomical Complications in General Surgery. New York: McGraw-Hill, 1983).
External Junction
The gastroesophageal junction lies in the abdomen just below the diaphragm.
The abdominal esophagus is said to be from 0.5 to 2.5 cm in length and occasionally as long as 7 cm. The surgeon has access to an appreciable length of esophagus below the diaphragm.
The abdominal esophagus lies at the level of the 11th or 12th thoracic vertebra and is partially covered by peritoneum in front and on its left lateral wall. Relations with surrounding structures are as follows:
ANTERIOR: The posterior surface of the left lobe of the liver, the left vagal trunk, and the esophageal plexus
POSTERIOR: One or both crura of the diaphragm, the left inferior phrenic artery, and the aorta
TO THE RIGHT: The caudate lobe of the liver
TO THE LEFT: The fundus of the stomach
Internal Junction
The histological junction between esophagus and stomach is marked by an irregular boundary between stratified squamous epithelium and simple columnar epithelium. Above the boundary, islands of columnar gastric epithelium may be present at all levels of the esophagus. The lower esophagus may occasionally be lined by gastric mucosa. A biopsy specimen to identify histologic changes in the mucosa should be taken more than 2 cm above the epithelial junction to avoid most of these patches.
Part of the problem of defining the gastroesophageal junction is the fact that this mucosal boundary does not coincide with the external junction described above. In the living patient, the situation is even less simple. The submucosal connective tissue is so loose that the mucosa moves freely over the underlying muscularis. Even at rest, the junctional level may change. Figure 6.5 shows the internal gastroesophageal junction from the point of view of four specialties.
“Cardiac Sphincter”
There is a sphincter at the cardiac orifice of the stomach that normally permits swallowing but not reflux. A slight thickening of the circular musculature of the distal esophagus has been described.
Several other structures have been held responsible for closing the cardia: the angle (of His) at which the esophagus enters the stomach, the pinchcock action of the diaphragm, a plug of loose esophageal mucosa (mucosal rosette), the phrenoesophageal membrane, and the sling of oblique fibers of the gastric musculature.
Esophageal Hiatus and the Crura (See Chap. 5)
Surgical Considerations
Placing 0 silk sutures deep in the crura, including the attached pleura, is absolutely necessary for narrowing the hiatus. The surgeon must be certain the sutures are in the tendinous portions of the crura and not in the muscular part only.
Phrenoesophageal Ligament
Where the esophagus passes from the thorax into the abdomen through the diaphragmatic hiatus, a strong, flexible, airtight seal is necessary. The seal must be strong enough to resist abdominal pressure, which tends to push the stomach into the thorax, and flexible enough to give with the pressure changes incidental to breathing and the movement incidental to swallowing. A seal known as the phrenoesophageal ligament or membrane consists, in principle, of the following elements: pleura, subpleural (endothoracic) fascia, phrenoesophageal fascia (of Laimer), transversalis (endoabdominal subdiaphragmatic) fascia, and peritoneum (Fig. 6.6).
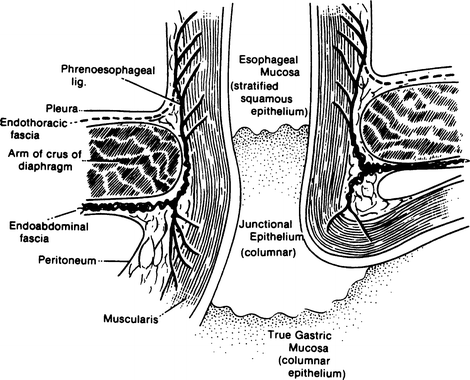

Figure 6.6.
Diagram of a coronal section through the gastroesophageal junction and the esophageal hiatus of the diaphragm (By permission of JE Skandalakis, SW Gray, and JR Rowe. Anatomical Complications in General Surgery. New York: McGraw-Hill, 1983).
The first and last of these elements provide the requirement for airtightness; the middle three provide flexibility and strength. The ligament exists in infants, is attenuated in adults, and does not exist in adult patients with hiatal hernia.
The development of the phrenoesophageal ligament can be summarized as follows:
In newborn infants, the phrenoesophageal ligament is present.
In adults, the ligament is attenuated and subperitoneal fat accumulates at the hiatus.
In adults with hiatal hernias, the ligament for all practical purposes does not exist.
SURGICAL CONSIDERATIONS: Dividing the phrenoesophageal ligament will mobilize the cardia, but the surgeon undertaking a Hill procedure must be prepared to find the ligament ill defined or absent.
Peritoneal Reflections
HEPATOGASTRIC (GASTROHEPATIC) LIGAMENT: The abdominal esophagus is contained between the two layers of the hepatogastric ligament. The ligament contains the following structures: left gastric artery and vein; hepatic division of left vagus trunk; lymph nodes; occasionally, both vagal trunks; occasionally, branches of the right gastric artery and vein; and the left hepatic artery when it arises from the left gastric artery (in 23 % of cases).
GASTROSPLENIC (GASTROLIENAL) LIGAMENT: The hepatogastric ligament encloses the abdominal esophagus on the right; its leaves rejoin on the left of the esophagus to form the gastrosplenic ligament. The lesser sac lies behind these ligaments (for more information, see Chap. 15).
Gastrophrenic Ligament (See Chap. 7, Stomach)
The Structure of the Esophageal Wall (Fig. 6.7)
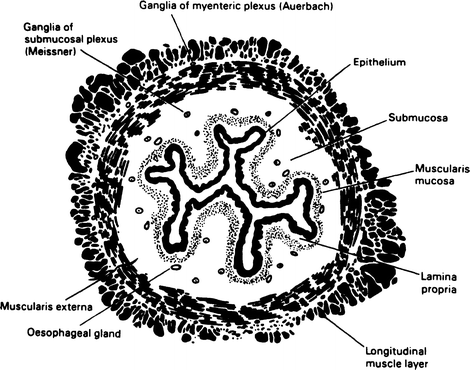
Figure 6.7.
Cross section of the esophagus showing the layers of the wall. The longitudinal and circular layers of the muscularis externa contain striated muscle fibers decreasing distally (By permission of JE Skandalakis, SW Gray, and LJ Skandalakis. In: GG Jamieson, Surgery of the Esophagus. Edinburgh: Churchill Livingstone, 1988, pp. 19–35).
Mucosa
The esophagus is lined with a thick layer of non-keratinizing, stratified squamous epithelium continuous with the lining of the oropharynx.
Submucosa
A layer of loose connective tissue lies external to the mucosa. The thick submucosa is the strongest part of the esophageal wall. It is this layer with the lamina propria that the surgeon must count on for a sound esophageal anastomosis.
Muscularis Externa
The chief muscles of the esophagus are an internal circular layer and an external longitudinal layer. Both layers in the upper quarter of the esophagus are large striated (voluntary) muscle fibers. In the second quarter, striated and smooth (involuntary) fibers are mingled; the lower half contains only smooth fibers (Fig. 6.8).
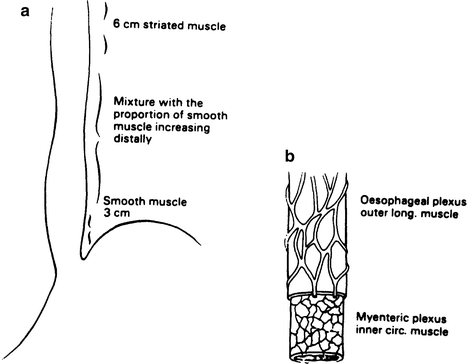

Figure 6.8.
(a) relative distribution of smooth and striated muscle in the esophagus. (b) the extrinsic and intrinsic nerves of the esophagus (By permission of JE Skandalakis, SW Gray, and LJ Skandalakis. In: GG Jamieson, Surgery of the Esophagus. Edinburgh: Churchill Livingstone, 1988, pp. 19–35).
Adventitia
The connective tissue of the mediastinum around the esophagus is not a true layer of that organ, and it does not provide the surgeon with a firm anchorage for sutures. It is the lack of a serosa that contributes to the complication of anastomotic disruption following esophageal resection and anastomosis.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


