and John E. Skandalakis1
(1)
Centers for Surgical Anatomy and Technique, Emory University School of Medicine Piedmont Hospital, Atlanta, GA, USA
Abstract
The vascular system of the pancreas is complex and nontypical. Embryologically, anatomically, and surgically, the head of the pancreas, the common bile duct, and the duodenum form an inseparable unit. Their relations and blood supply make it impossible for the surgeon to remove completely the head of the pancreas without removing the duodenum and the distal part of the common bile duct or to leave a rim of pancreas along the medial border of the duodenum to preserve the duodenal blood supply.
Operating room steps for evaluation of resectability of the pancreas are presented. There are several possible routes to exploration of the pancreas, which may be used individually or in combination, each with particular advantages and disadvantages. Step-by-step technique for the Puestow procedure, pancreatectomies, and pancreaticoduodenectomy (Whipple procedure) is provided. An enlarged and revised section on laparoscopic resection of the pancreas includes laparoscopic distal pancreatectomy, transduodenal-pancreatic biopsy, drainage of pancreatic pseudocyst, and repair of pancreatic trauma.
Anatomy
General Description of the Pancreas
The pancreas lies transversely in the retroperitoneal sac, between the duodenum on the right and the spleen on the left. It is related to the omental bursa above, the transverse mesocolon anteriorly, and the greater sac below. For all practical purposes, the pancreas is a fixed organ.
Anteriorly, the pancreas is related to other organs from right to left as follows (Fig. 9.1):
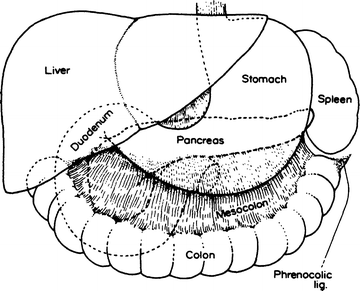

Figure 9.1.
Anterior relationships of the pancreas (By permission of JE Skandalakis, SW Gray, JS Rowe, et al. Contemp Surg. 1979;15(5):17–40).
ABOVE: Duodenum, pylorus, liver, stomach, spleen
BELOW: Duodenum, jejunum, transverse colon, spleen
INTERMEDIATE: Transverse colon, mesocolon, transverse mesocolon, spleen
On the anterior surface of the head of the pancreas and across the duodenum, the transverse mesocolon is very short, so that the colon itself is attached to the underlying organ.
The second and third parts of the duodenum are overlapped by the head of the pancreas; therefore, there is a pancreatic “bare area” of the duodenum (Fig. 9.2) that is not covered by peritoneum. A second bare area exists on the anterior surface of the second portion of the duodenum, where the transverse colon is attached. With pancreatic cancer or pancreatitis, the pancreas and the mesocolon, together with its middle colic artery, become firmly fixed.
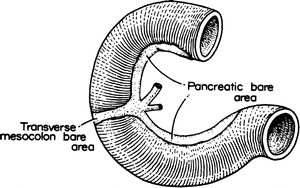

Figure 9.2.
Bare areas of the duodenum. The entire concave surface is in intimate contact with the pancreas; the attachment of the transverse mesocolon crosses the anterior surface of the second portion (By permission of JE Skandalakis, SW Gray, JS Rowe, et al. Contemp Surg. 1979;15(5):17–40).
Posteriorly the pancreatic bed in the retroperitoneal space consists of an area between the hilum of the right kidney, the hilum of the spleen, the celiac artery, and the inferior mesenteric artery. From right to left, the area contains the hilum of the right kidney, the inferior vena cava, the portal vein, the superior mesenteric vein, the aorta, the left kidney, and the hilum of the spleen (Fig. 9.3).
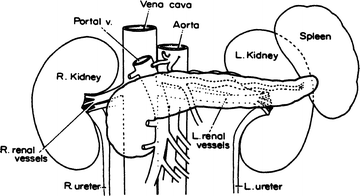

Figure 9.3.
Posterior relationships of the pancreas. Anterior view (By permission of JE Skandalakis, SW Gray, JS Rowe, et al. Contemp Surg. 1979;15(5)17–40)
Parts of the Pancreas
The pancreas may be arbitrarily divided into five parts: head, uncinate process, neck, body, and tail (Fig. 9.4).
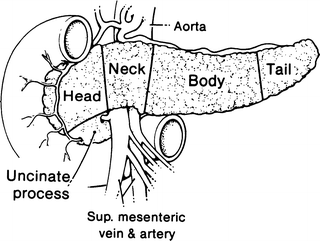

Figure 9.4.
The five parts of the pancreas. The line between the body and the tail is arbitrary (By permission of JE Skandalakis, SW Gray, and JR Rowe. Anatomical Complications in General Surgery. New York: McGraw-Hill; 1983).
Head
The head of the pancreas is that portion lying to the right of the superior mesenteric artery and vein. The head adheres to the duodenal loop.
The anterior pancreaticoduodenal arcade can be seen upon the ventral surface of the head of the pancreas, coursing roughly parallel with the duodenal curvature. The posterior pancreaticoduodenal vascular arcade is a major entity on the posterior surface of the head. This surface is close to the hilum and medial border of the right kidney, right renal vessels and the inferior vena cava, the right crus of the diaphragm, and the right gonadal vein. The head may be related to the third part of the common bile duct in a variety of ways.
Uncinate Process
The uncinate (“hooklike”) process is an extension of the head of the pancreas and is highly variable in size and shape. It passes downward and slightly to the left from the principal part of the head. It further continues behind the superior mesenteric vessels and in front of the aorta and inferior vena cava. In sagittal section, the uncinate process lies between the aorta and the superior mesenteric artery, with the left renal vein above and the duodenum below (see Fig. 8.14).
The uncinate process may be absent or may completely encircle the superior mesenteric vessels (Fig. 9.5). If the process is well developed, the neck of the pancreas must be sectioned from the front to avoid injury to the vessels. Short vessels from the superior mesenteric artery and vein supply the uncinate process and must be carefully ligated.
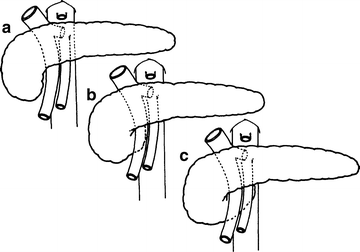

Figure 9.5.
Variations in the extent of the uncinate process of the pancreas. (a) Does not reach superior mesenteric vessels. (b) Reaches across superior mesenteric vein almost to superior mesenteric artery. (c) Reaches beyond superior mesenteric artery (By permission of JE Skandalakis, SW Gray, JS Rowe, et al. Contemp Surg. 1979;15(5):17–40).
Neck
The neck, from 1.5 to 2 cm in length, can be defined as the site of passage of the superior mesenteric vessels and the beginning of the portal vein dorsal to the pancreas.
The gastroduodenal artery passes to the right of the neck and provides origin for the anterior superior pancreaticoduodenal artery. Posterior to the neck, the portal vein is formed by the confluence of the superior mesenteric and splenic veins. Near the inferior margin of the pancreatic neck, one can often see the terminations of the inferior pancreaticoduodenal vein and right gastroepiploic vein where they drain into the superior mesenteric or splenic veins or into the portal vein proper.
The inferior mesenteric vein drains, with essentially equal frequency, into the splenic vein, the superior mesenteric vein, or the site of formation of the portal vein. Careful elevation of the neck and ligation of anterior tributaries, if present, are necessary. Bleeding can make it difficult to evaluate the structures lying beneath the neck.
The portal vein receives the posterior superior pancreaticoduodenal, right gastric, left gastric, and pyloric veins. It is fairly common for an anomalous vein to enter the anterior surface.
Body
The anterior surface of the body of the pancreas is covered by the double layer of peritoneum of the omental bursa that separates the stomach from the pancreas. The body is related to the transverse mesocolon, which divides into two leaves: the superior leaf covers the anterior surface and the inferior leaf passes inferior to the pancreas. The middle colic artery emerges from beneath the pancreas to travel between the leaves of the transverse mesocolon (see Fig. 8.14).
Posteriorly, the body of the pancreas is related to the aorta, the origin of the superior mesenteric artery, the left crus of the diaphragm, the left kidney and its vessels, the left adrenal gland, and the splenic vein (Fig. 9.3). Small vessels from the pancreas enter the splenic vein and, during pancreatectomy, must be ligated in order to preserve the vein and the spleen.
Tail
The tail is relatively mobile. Its tip reaches the hilum of the spleen in 50 % of cases. Together with the splenic artery and the origin of the splenic vein, the tail is contained between two layers of the splenorenal ligament.
The outer layer of this ligament is the posterior layer of the gastrosplenic ligament. Careless division of this ligament may injure the short gastric vessels. The ligament itself is almost avascular, but digital manipulation should stop at the pedicle. Commonly a caudate branch arises from the left gastroepiploic or an inferior splenic polar branch and passes to the tip of the tail of the pancreas. Anticipate this branch in the pancreaticosplenic ligament.
Pancreatic Ducts
The main pancreatic duct (of Wirsung) and the accessory duct lie anterior to the major pancreatic vessels. Pathological ducts are readily palpated and opened from the anterior surface.
Because of the developmental origin of the two pancreatic ducts, several variations are encountered; most can be considered normal. The usual configuration is seen in Fig. 9.6a:
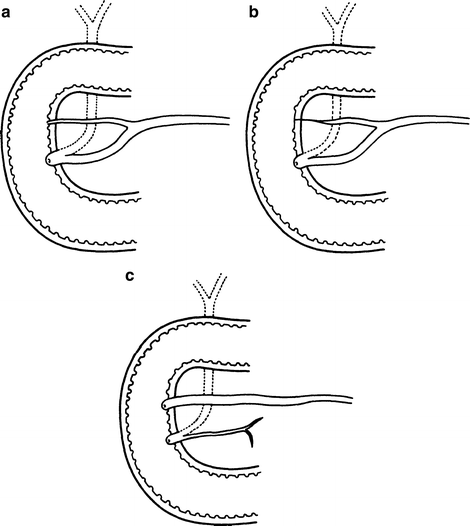

Figure 9.6.
Variations of the pancreatic ducts. (a) Both ducts open into the duodenum. (b) The accessory duct ends blindly in the duodenal wall. (c) The main duct is smaller than the accessory duct and they are not connected (modified by permission of JE Skandalakis, SW Gray, JS Rowe, et al. Contemp Surg. 1979;15(5):17–40).
The greatest diameter of the main pancreatic duct is in the head of the pancreas, just before the duct enters the duodenal wall.
Less than 3 ml of contrast medium will fill the main pancreatic duct in the living patient, and 7–10 ml will fill the branches and the smaller ducts.
Duodenal Papilla
The duodenal papilla (of Vater) lies at the end of the intramural portion of the common bile duct. It is on the posteromedial wall of the second part of the duodenum, to the right of the second or third lumbar vertebra in most cases. On endoscopy, the papilla was found to the right of the spine at the level of the second lumbar vertebra in most patients. The distance of the papilla from the pylorus is highly variable, ranging from 1.5 to 12 cm. Inflammation of the proximal duodenum may shorten the distance; the pylorus is not a useful landmark.
The present concept of musculature is that there is a complex of four sphincters composed of circular or spiral smooth muscle fibers surrounding the intramural portion of the common bile and pancreatic ducts. The complex may be broken into four separate sphincters, as shown in Fig. 9.7.
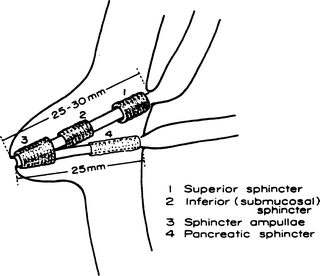

Figure 9.7.
Diagram of the four entities composing the sphincter of Boyden (measurements from White TT. Surgical anatomy of the pancreas. In: Carey LC (ed). The Pancreas. St Louis: CV Mosby Co; 1973) (By permission of JE Skandalakis, SW Gray, JS Rowe, et al. Contemp Surg. 1979.15(5):17–40).
The sphincteric complex varies from 6 to 30 mm in length, depending on the obliquity of the ducts. In some individuals, the complex may extend into the pancreatic portion of the common bile duct. This is important to know, because complete anatomical transection of all elements of the complex may not be necessary for satisfactory function. Incision by 5-mm steps while testing with a suitable dilator will help limit the incision to the shortest length necessary to obtain the desired results. On the mucosal surface of the duodenum, the duodenal papilla of Vater is found where a longitudinal mucosal fold meets a transverse fold to form a T (Fig. 9.8).
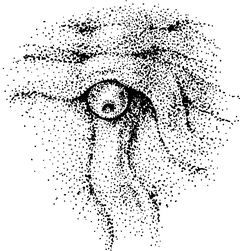

Figure 9.8.
The T arrangement of mucosal folds of the duodenum indicates the site of the major duodenal papilla. Mucosal fold may cover orifice of papilla in some cases. Major papilla is rarely this obvious (By permission of JE Skandalakis, SW Gray, JS Rowe, et al. Contemp Surg. 1979;15(5):17–40).
These are some practical considerations:
Too much lateral or distal traction on the opened duodenum may erase the folds and distort the T.
The papilla is often covered by a transverse fold. One must gently elevate the folds in the assumed location.
If the T is not apparent and the papilla cannot be palpated, the common bile duct must be probed from above.
A duodenal diverticulum lying close to the papilla may present difficulties for the surgeon or the endoscopist. The papilla has been found in a diverticulum; it separated from the duodenal wall and was immediately reimplanted.
The ampulla is the common pancreaticobiliary channel below the junction of the ducts within the papilla (Fig. 9.9a). If the septum between the ducts extends to the orifice of the papilla, there is no ampulla.
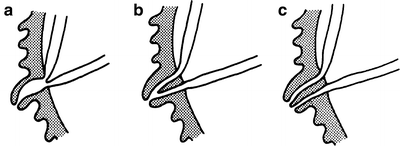

Figure 9.9.
Diagram of the relations of the pancreatic and common bile ducts. (a) Minimal embryonic absorption of the ducts into the duodenal wall; an ampulla is present. (b) Partial embryonic resorption of the ducts; no true ampulla is present. (c) Maximum embryonic resorption of the ducts; two separate orifices open on the papilla (By permission of JE Skandalakis, SW Gray, JS Rowe, et al. Contemp Surg. 1979;15(5):17–40).
The most useful classification is as follows:
Type 1. The pancreatic duct opens into the common bile duct at a variable distance from the orifice of the major duodenal papilla. The common channel may or may not be dilated (85 %) (Fig. 9.9a, b).
Type 2. The pancreatic and common bile ducts open separately on the major duodenal papilla (5 %) (Fig. 9.9c).
Type 3. The pancreatic and common bile ducts open into the duodenum at separate points (9 %).
Vascular System of the Pancreas
The vascular system of the pancreas is complex and nontypical. Nevertheless, a “general plan” is shown in the previous chapter in Figs. 8.4 and 8.5; remember that variations are common. The pancreas is supplied with blood from both the celiac trunk and the superior mesenteric artery.
In general, it appears that the blood supply is greatest to the head of the pancreas, less to the body and tail, and least to the neck. The head of the pancreas and the concave surface of the duodenum are supplied by two pancreaticoduodenal arterial arcades (anterior and posterior). Ligation of both vessels will result in duodenal ischemia and necrosis. All major arteries lie posterior to the ducts.
Pancreatic Arcades
The gastroduodenal artery divides to form the anterior superior and posterior superior pancreaticoduodenal arteries.
The anterior inferior pancreaticoduodenal artery arises from the superior mesenteric artery at or above the inferior margin of the pancreatic neck. It may form a common trunk with the posterior inferior artery. Ligation of the jejunal branch itself will endanger the blood supply to the fourth part of the duodenum.
Dorsal Pancreatic Arcade
The dorsal pancreatic arcade lies posterior to the neck of the pancreas and, often, posterior to the splenic vein.
Transverse Pancreatic Artery
The transverse (inferior) pancreatic artery is the left branch of the dorsal pancreatic artery, and it supplies the body and tail of the pancreas.
Branches of the Splenic Artery
The splenic artery is located on the posterior surface of the body and tail of the pancreas (see Fig. 8.5). From 2 to 10 branches of the splenic artery anastomose with the transverse pancreatic artery. The largest of these, the great pancreatic artery (of von Haller), is the main blood supply to the tail of the pancreas. Ligation of the splenic artery does not require splenectomy, but ligation of the splenic vein does.
Caudal Pancreatic Artery
The caudal pancreatic artery arises from the left gastroepiploic artery or from a splenic branch at the hilum of the spleen.
Venous Drainage
In general, the veins of the pancreas parallel the arteries and lie superficial to them. Both lie posterior to the ducts in the body and tail of the pancreas. The drainage is to the portal vein, splenic vein, and superior and inferior mesenteric veins (see Figs. 8.6 and 8.7).
The hepatic portal vein is formed behind the neck of the pancreas by the union of the superior mesenteric and splenic veins (see Fig. 8.7).
The portal vein lies behind the pancreas and in front of the inferior vena cava, with the common bile duct on the right and the common hepatic artery on the left.
Lymphatic Drainage
Figure 9.10 shows the chief groups of lymph nodes receiving lymphatic vessels from the pancreas. Lymphatic drainage may prove to be as complex and nontypical as the arterial supply.
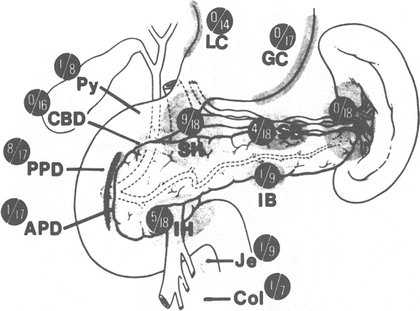

Figure 9.10.
Chief groups of lymph nodes receiving lymphatic vessels from the pancreas. SH superior head, IH inferior head, PPD posterior pancreaticoduodenal, APD anterior pancreaticoduodenal, SB superior body, IB inferior body, S splenic, GC greater curvature, LC lesser curvature, Py pylorus, CBD common bile duct, Je jejunum, Col colon. In the Whipple resection (indicated by the stippled vertical line), the SB, IB, and S groups usually are not removed. From AL Cubilla, PJ Fitzgerald. Cancer of the exocrine pancreas: The pathologic aspects. CA Cancer J Clin. 1985;35(1):2–18. Reprinted with permission from Wiley.
Nerve Supply of the Pancreas
Innervation of the pancreas occurs by the sympathetic division of the autonomic nervous system through the splanchnic nerves and by the parasympathetic division through the vagus nerve. In general, these nerves follow blood vessels to their destinations.
The celiac ganglion is the central station of both sympathetic and parasympathetic innervation. Extirpation—surgical or chemical—of the celiac ganglion should interrupt afferent fibers of both sympathetic and parasympathetic systems.
Ectopic and Accessory Pancreas
Pancreatic tissue in the stomach, duodenal wall, ileal wall, Meckel’s diverticulum, or at the umbilicus is not unusual. Less common sites are the colon, appendix, gallbladder, omentum or mesentery, and in anomalous bronchoesophageal fistula. Most such pancreatic tissue is functional. Islet tissue is often present in gastric and duodenal heterotopia, but it is usually absent in accessory pancreatic tissue elsewhere in the body. Figure 9.11 shows the possible sites of heterotopic pancreatic tissue.
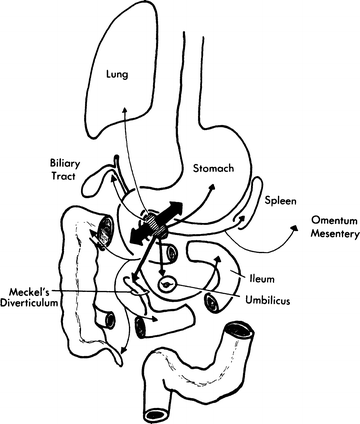

Figure 9.11.
Sites of pancreatic heterotopia. The relative frequency is indicated by the width of the arrows. The stomach and duodenum are by far the most common sites (By permission of JE Skandalakis, SW Gray, RR Ricketts, et al. The pancreas. In JE Skandalakis and SW Gray. Embryology for Surgeons. 2nd ed. Baltimore: Williams & Wilkins, 1994).
Technique
Evaluation of Resectability of the Pancreas
The authors strongly advise angiograms prior to surgery. Also, we suggest the following steps in the operating room:
1.




Good general exploration of the abdomen with special attention to the pancreas.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


