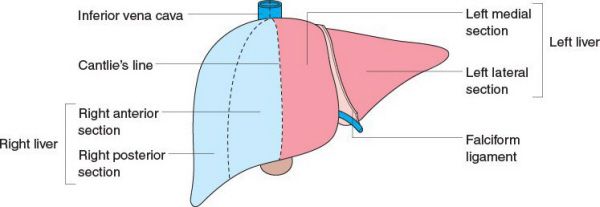
Segmental classification of the liver. (With permission from Mulholland MW, Lillemoe KD, Doherty GM, Maier RV, Upchurch GR, eds. Greenfield’s Surgery. 4th ed. Philadelphia, PA: Lippincott Williams & Wilkins; 2005.)
•Liver is divided into the right and left lobes
•Lobes are separated by Cantlie line, which runs from the gallbladder fossa to the inferior vena cava (IVC)
•The caudate lobe is distinct from the right and left lobes because its venous drainage is directly into the IVC
Lobar classification of the liver. (With permission from Mulholland MW, Lillemoe KD, Doherty GM, Maier RV, Upchurch GR, eds. Greenfield’s Surgery. 4th ed. Philadelphia, PA: Lippincott Williams & Wilkins; 2005.)
Other Perihepatic Structures
•Falciform ligament
•Separates the medial and lateral segments of the left lobe
•Attaches the liver to the abdominal wall
•Ligamentum teres
•Carries the obliterated umbilical vein
•Triangular ligaments
•Lateral and medial extensions of the coronary ligaments on the posterior surface of the liver
•Made of peritoneum
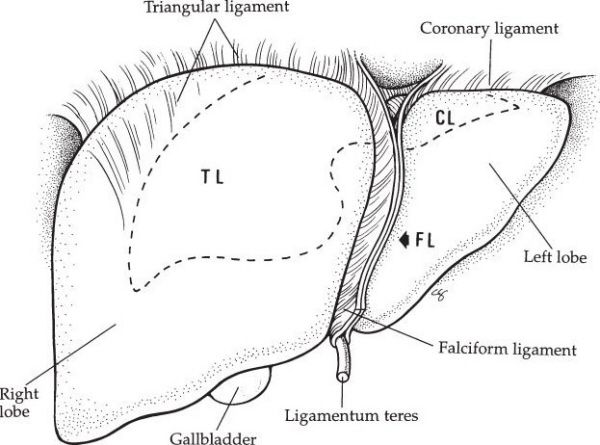
Perihepatic ligaments. (With permission from Fischer JE, Bland KI, Callery MP, et al., eds. Mastery of Surgery. 5th ed. Philadelphia, PA: Lippincott Williams & Wilkins; 2006.)
•Where the bile duct, portal vein, and hepatic artery meet (the portal triad)
•Foramen of Winslow
•Anterior—portal triad
•Posterior—IVC
•Inferior—duodenum
•Superior—liver
What cells in the liver are most susceptible to ischemic insult and what cells are most susceptible to toxic or chemical injury?
The hepatocytes are the most susceptible to ischemic injury, and the biliary ductule is the most susceptible to toxic or chemical injury.
Microscopic Anatomy of the Liver
•Acinar unit
•The functional unit of the liver
•Includes the biliary ductule, the hepatic arteriole, and the portal venule
•Zones are defined relative to oxygen and solute concentration gradients
•Zone 1
•Closest to portal triad
•Most susceptible to toxic injury, least susceptible to ischemia
•Zone 3
•Contains hepatocytes
•Adjacent to the terminal hepatic vein
•Most susceptible to ischemic injury
•Alkaline phosphatase is in the canalicular system
•Nutrient uptake occurs in the sinusoidal membrane
During a routine cholecystectomy, the gallbladder is very inflamed and due to poor visualization, the common hepatic artery is mistaken for the cystic artery and is ligated. What will be the remaining blood flow and oxygen supply to the liver?
The liver will still have 75% of its original blood flow, but only 50% of its original oxygen delivery.
Blood Supply of the Liver
•Portal vein
•Supplies 75% of the blood flow to the liver and 50% of the oxygen supply
•Formed by the superior mesenteric vein (SMV) and splenic veins
•Inferior mesenteric vein drains into the splenic veins (or occasionally, into the SMV)
•Hepatic artery
•Supplies 25% of the blood flow to the liver and 50% of the oxygen supply
•Becomes the proper hepatic artery after the gastroduodenal artery branches off, and then branches into the right and left hepatic arteries
•Approximately 10% of patients will have
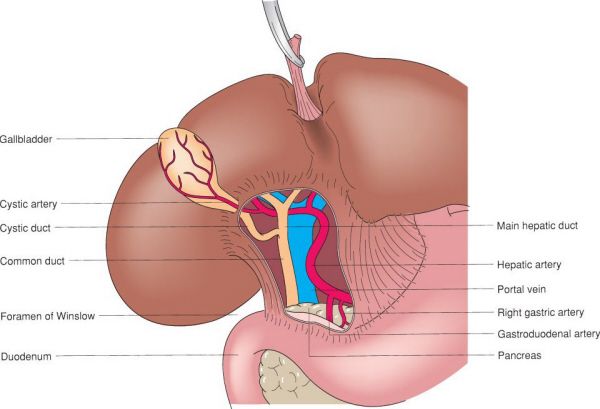
Periportal anatomy. (With permission from Mulholland MW, Lillemoe KD, Doherty GM, Maier RV, Upchurch GR, eds. Greenfield’s Surgery. 4th ed. Philadelphia, PA: Lippincott Williams & Wilkins; 2005.)
•A replaced/accessory right hepatic artery arising from the superior mesenteric artery that travels posterolateral to the common bile duct (CBD) in the porta hepatis
•A replaced/accessory left hepatic artery arising from the left gastric artery that travels through the gastrohepatic ligament into the falciform ligament
•Hepatic vein (HV)
•3 venous branches
•Left HV: Drains segments II, III, and IVA
•Right HV: Drains segments VI, VII, and VIII
•Middle HV: Drains segments IV and V
•Caudate lobe (segment I) drains directly into the IVC
What is the lymphatic drainage of the liver?
Lymphatic Drainage of the Liver
•Lymphatic drainage starts in perisinusoidal spaces of Disse and clefts of Mall
•These drain into the porta hepatis
•Porta hepatis drains to cisterna chili
•Cisterna chili drains into thoracic duct
•Lymphatics are on the right side of the CBD
•Pathophysiology of ascites
•Decreased permeability of sinusoidal epithelial cells  altered lymphatic drainage
altered lymphatic drainage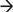 ascites
ascites
In addition to bile production and hemoglobin degradation, what are the physiologic functions of the liver?
The liver also does detoxification, nutrient storage, glucose, lipid and protein metabolism, and protein synthesis.
Detoxification
•Cytochrome P450 system
•Conversion of hydrophobic to hydrophilic compounds to improve solubility for secretion
•Reactions include reduction, hydroxylation, and hydrolysis to expose functional groups
•Phase II reactions
•Conjugation to alter solubility
Nutrient Storage
•Glycogen
•Triglycerides
•Vitamin B12
•Copper
•Fat-soluble vitamins
Protein Synthesis
•Coagulation factors: I, II, V, VII, IX, X, and XI, antithrombin III, protein C/S
•Factor VIII is made primarily by endothelial cells, but a small proportion is made in the liver
•Complement factors
•Acute phase proteins: Transferrin, CRP, fibrinogen, haptoglobin, albumin, ceruloplasmin
Protein, Lipid, and Glucose Metabolisms
•Glycogenesis and glycogenolysis + gluconeogenesis, depending on the body’s state of metabolism
•Lipogenesis (from amino acids and glucose)
•Deamination and transamination of amino acids
•Urea cycle—conversion of ammonia to urea
•Production of non-essential amino acids
A 63-year-old woman with a history of unresectable bile duct cancer (cholangiocarcinoma) status post biliary stenting presents with a 1-week history of fevers, chills, and jaundice. An abdominal CT reveals multiple rim-enhancing fluid collections in the liver. What is the most likely diagnosis?
A hepatic abscess usually presents following episodes of intra-abdominal infection or bacteremia and is characterized by a rim-enhancing fluid collection on CT scan. Common organisms include Escherichia coli, Klebsiella, Proteus, Staphylococcus, and Streptococcus. Fungus may be found in immunocompromised patients or in patients with multi-organism hepatobiliary infection. Amebic abscesses are caused by Entamoeba histolytica.
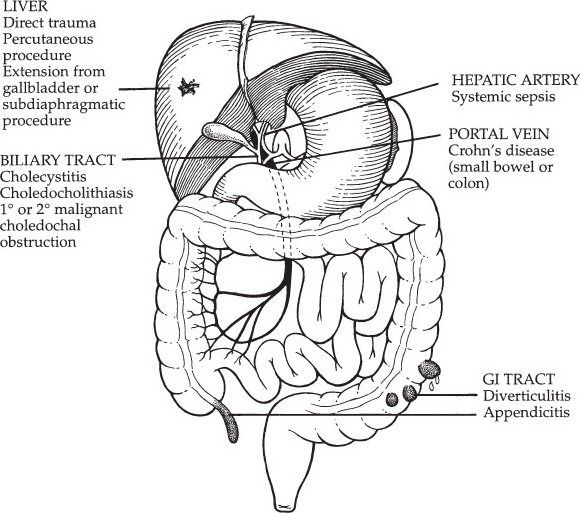
Pyogenic liver abscess. (With permission from Fischer JE, Bland KI, Callery MP, et al., eds. Mastery of Surgery. 5th ed. Philadelphia, PA: Lippincott Williams & Wilkins; 2006.)
Pyogenic Liver Abscess
•Causes
•Biliary instrumentation (most common)
•Biliary obstruction from stones, strictures, and tumors
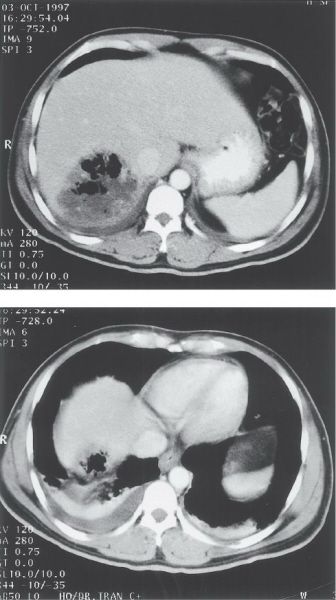
•Portal vein spread of gastrointestinal infections such as diverticulitis, appendicitis, or perforated ulcers
•Hematogenous spread via hepatic artery in the setting of systemic bacteremia
•Unknown etiology in up to 20% of patients
•Diagnosis
•Most common type of liver abscess in the United States
•Patients present with fever, chills, and right upper quadrant abdominal pain
•Jaundice, weight loss, nausea, and vomiting can also be seen
•Up to one-quarter of patients will be septic
•Lab tests show leukocytosis, elevated bilirubin, and alkaline phosphatase
•Plain abdominal films or abdominal CT may show gas in the abscess cavity and elevation of the right hemidiaphragm
•CT can also demonstrate contrast-enhancing, well-defined round masses with low internal density
•Ultrasound demonstrates hypoechoic lesions
•Treatment
•Percutaneous drainage is the treatment of choice
•Laparoscopic or open surgical drainage is used when percutaneous drainage is not possible or the source of infection is surgically correctable
•Microabscesses in patients in good condition can be treated with antibiotics alone
•Broad-spectrum antibiotics should be substituted with culture-guided antibiotics as soon as the organisms are identified
Causes of pyogenic liver abscess. (With permission from Fischer JE, Bland KI, Callery MP, et al., eds. Mastery of Surgery. 5th ed. Philadelphia, PA: Lippincott Williams & Wilkins; 2006.)
When choosing a method of drainage, factors that should be considered include the anesthetic risk and underlying clinical condition of the patient, as well as the local expertise in and availability of each drainage method.
Amebic Liver Abscess
•Most common cause of liver abscess worldwide
•Complication of intestinal amebiasis (E. histolytica) in 3% to 10% of cases; spreads to the liver via the portal vein
•Symptoms/history
•History of travel to a tropical climate
•Fever
•Abdominal pain and hepatomegaly
•Diarrhea is present in only 20% to 30% of the cases
•Often patients do NOT have jaundice
•The abscess can rupture into pleura, pericardium, or peritoneum
•Diagnosis
•Often a solitary lesion in the right lobe of the liver
•CT scan shows low internal density and smooth margins
•Serology (indirect hemagglutination and gel diffusion precipitation) is the most accurate test for diagnosis
•Stool testing for the cyst of the protozoan is negative in most cases
•Treatment
•Metronidazole is effective in most cases
•Aspiration may be required for larger abscesses
•Surgical drainage is reserved for patients with secondary infection, perforation with peritoneal irritation, or failure of metronidazole therapy
History of travel to a tropical area in a young patient with a solitary liver cavity should prompt serology investigation for an amebic abscess.
A 38-year-old man who recently emigrated from Sudan presents to the emergency department with nausea, vomiting, and jaundice. A CT scan reveals a large, solitary, calcified cyst in the right lobe of the liver. Serologic tests confirm infection with Echinococcus. What is the next step in the management of this cyst?
The cyst should be excised completely, including sterilization of the cyst and excision of the germinal layer.
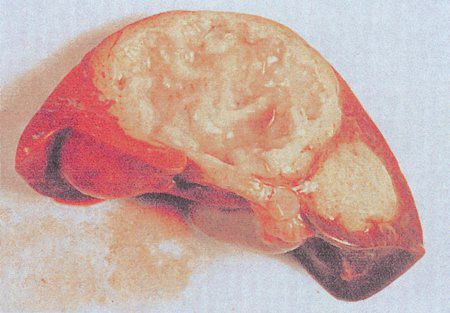
Echinococcal cyst. (With permission from Mulholland MW, Lillemoe KD, Doherty GM, Maier RV, Upchurch GR, eds. Greenfield’s Surgery. 4th ed. Philadelphia, PA: Lippincott Williams & Wilkins; 2005.)
Echinococcal Cyst
•Caused by the larval stage of the tapeworm Echinococcus
•Infection occurs through ingestion of parasite eggs
•Eggs are released in the feces of the definitive host (carnivores and rodents)
•Eggs hatch and migrate across the intestinal wall of the intermediate host, spreading to the liver (most commonly), brain, lungs, and bones
•Patients are often from endemic areas such as the Mediterranean and Baltic areas, Middle and Far East, South America and South Africa
•There is an asymptomatic phase of variable duration
•Clinical manifestations include fever, abdominal pain, jaundice, and weight loss
•Serology (indirect hemagglutination) has good sensitivity
•Can also have a positive Casoni skin test (intradermal injection of sterilized fluid from hydatid cysts that results in wheal response; high false positive rate limits its utility)
•Imaging with ultrasound or CT scan usually shows a unilocular or complex lesion with daughter cysts
•Thick calcified rims are seen in dead cysts
•Rupture, most commonly to the
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


