Some affected mothers and infants have inherited long-chain 3-hydroxyacyl-CoA dehydrogenase (LCHAD) deficiency
Top Differential Diagnoses
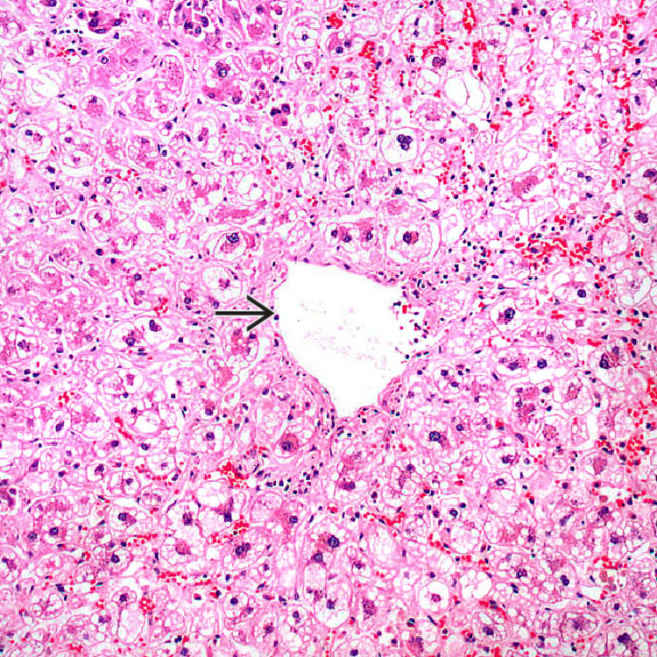
Extensive microvesicular steatosis involves the centrilobular or zone 3 hepatocytes. A central vein
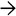 is present in the center of the image.
is present in the center of the image.
High-power view demonstrates the extensive microvesicular steatosis typical of fatty liver of pregnancy. Numerous small steatotic vacuoles
 surround and focally indent the hepatocyte nucleus.
surround and focally indent the hepatocyte nucleus.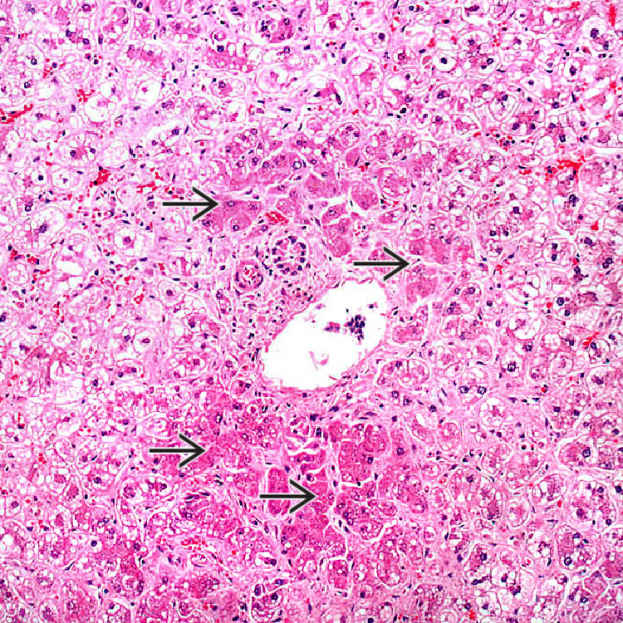
There is a background of extensive microvesicular steatosis, but there is relative sparing of a small rim of periportal hepatocytes
 .
.



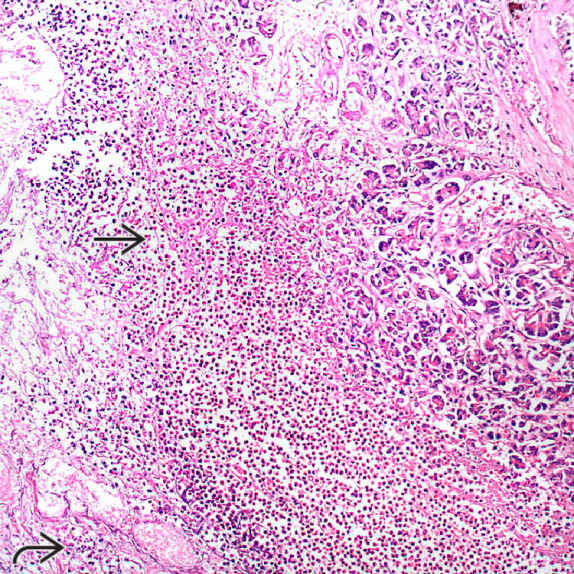
 with necrosis
with necrosis 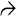 may also occur in patients with fatty liver of pregnancy.
may also occur in patients with fatty liver of pregnancy.


