and John E. Skandalakis1
(1)
Centers for Surgical Anatomy and Technique, Emory University School of Medicine Piedmont Hospital, Atlanta, GA, USA
Abstract
The extrahepatic biliary tract includes the right, left, and common hepatic ducts; cystic duct; common bile duct; hepatocystic triangle; and the gallbladder. Anomalous hepatic ducts can be a surgically significant source of bile leakage.
Detailed step-by-step technique is presented for operative cholangiogram, common bile duct exploration, cholecystectomy, sphincteroplasty, choledochoduodenostomy, choledochocystectomy, and laparoscopic cholecystectomy.
Anatomy
Right, Left, and Common Hepatic Ducts
The right and left hepatic ducts join soon after emerging from the liver to form the common hepatic duct (Fig. 14.1b). The junction lies 0.25–2.5 cm from the surface of the liver. The left duct is longer (1.7 cm, average) than the right duct (0.9 cm, average). In some cases, intrahepatic junction of the hepatic ducts is the result of liver enlargement (Fig. 14.1a); retraction of the liver may then be necessary to expose the junction.
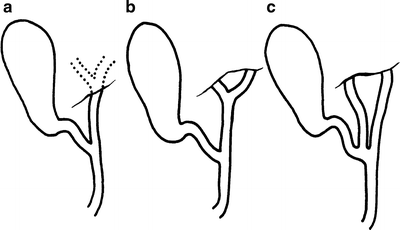

Figure 14.1.
Variations of the hepatic ducts. (a) Intrahepatic union of left and right hepatic ducts; (b) usual extrahepatic union of left and right hepatic ducts; (c) distal union of hepatic ducts producing absence of the common hepatic duct (by permission of JE Skandalakis, SW Gray, RR Ricketts, et al. The extrahepatic biliary ducts and the gallbladder. In: JE Skandalakis and SW Gray. Embryology for Surgeons, 2nd ed. Baltimore: Williams & Wilkins, 1994).
Measurements of the common hepatic duct are highly variable. The duct is said to be absent if the cystic duct enters at the junction of the right and left hepatic ducts (Fig. 14.1c). In most individuals, the duct is between 1.5 and 3.5 cm long.
Three types of cystohepatic junction have been described: angular (Fig. 14.1a, b), parallel (Fig. 14.2a), and spiral (Fig. 14.2b, c).
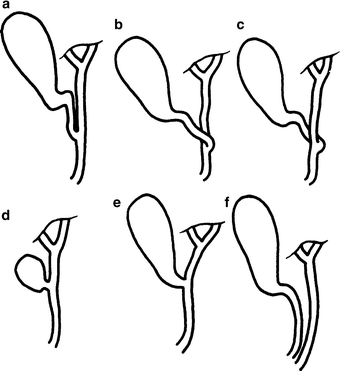

Figure 14.2.
Types of cystohepatic junction. (a) Parallel type. (b, c) Spiral types. (d, e) Short cystic ducts. (f) A long cystic duct ending in the duodenum. This may also be called “absence of the common bile duct” (by permission of JE Skandalakis, SW Gray, RR Ricketts, et al. The extrahepatic biliary ducts and the gallbladder. In: JE Skandalakis and SW Gray. Embryology for Surgeons, 2nd ed. Baltimore: Williams & Wilkins, 1994).
Anomalous Hepatic Ducts: Surgically Significant Sources of Bile Leakage (Fig. 14.3)
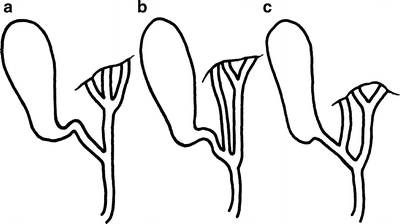
Figure 14.3.
Accessory hepatic ducts. (a) Accessory duct joins the common duct along with the usual left and right hepatic ducts. (b) Accessory duct joins at the intersection of the cystic duct. (c) Accessory duct enters the cystic duct directly. Additional, minute hepatic ducts are not unusual (by permission of JE Skandalakis, SW Gray, RR Ricketts, et al. The extrahepatic biliary ducts and the gallbladder. In: JE Skandalakis and SW Gray. Embryology for Surgeons, 2nd ed. Baltimore: Williams & Wilkins, 1994).
An aberrant hepatic duct is a normal segmental duct that joins the biliary tract just outside the liver instead of just within; it drains a normal portion of the liver. Such a duct passing through the hepatocystic triangle is important because it is subject to inadvertent section with subsequent bile leakage (Fig. 14.3).
Subvesicular bile ducts, found in approximately 35 % of individuals, are small blind ducts emerging from the right lobe of the liver and lying in the bed of the gallbladder. They do not communicate with the gallbladder.
Hepatocystic ducts drain bile from the liver directly into the body of the gallbladder or into the cystic duct.
Occasionally, the right, left, or even both hepatic ducts enter the gallbladder. This is an argument in favor of removing the gallbladder at the fundus, from above downward.
Cystic Duct
The cystic duct is about 3 mm in diameter and about 2–4 cm long. If surgeons are unprepared for a short duct (Fig. 14.2e), they may find themselves inadvertently entering the common bile duct. If they underestimate the length, they may leave too long a stump, predisposing to the cystic duct remnant syndrome.
Very rarely, the cystic duct is absent and the gallbladder opens directly into the common bile duct. In such a case, the common bile duct might be mistaken for the cystic duct.
Gallbladder
The gallbladder is located on the visceral surface of the liver in a shallow fossa at the plane dividing the right lobe from the medial segment of the left lobe (the GB-IVC line). The gallbladder is separated from the liver by the connective tissue of Glisson’s capsule. Anteriorly, the peritoneum of the gallbladder is continuous with that of the liver, and the fundus is completely covered with peritoneum.
The body of the gallbladder is in contact with the first and second portions of the duodenum. The body is also related to the transverse colon. Only in the rare presence of a mesentery (wandering gallbladder), a prerequisite for acute torsion, is the body completely covered by peritoneum. Several other anomalous peritoneal folds connected with the body of the gallbladder—cholecystogastric, cholecystoduodenal, and cholecystocolic—are redundancies of the lesser omentum.
The infundibulum is the angulated posterior portion of the body between the neck and the point of entrance to the cystic artery. When this portion is dilated, with eccentric bulging of its medial aspect, it is called a Hartmann’s pouch. When this pouch achieves considerable size, the cystic duct arises from its upper left aspect rather than from what appears to be the apex of the gallbladder. The pouch is often associated with chronic or acute inflammation due to lithiasis and often accompanies a stone impacted in the infundibulum.
The neck of the gallbladder is S-shaped and lies in the free border of the hepatoduodenal ligament. The mucosa lining the neck is a spiral ridge said to be a spiral valve, but not to be confused with the spiral valve of the cystic duct (the valve of Heister).
A deformity of the gallbladder seen in 2–6 % of individuals is the Phrygian cap (Fig. 14.4a). Hartmann’s pouch (Fig. 14.4b) is probably a normal variation rather than a true deformity.
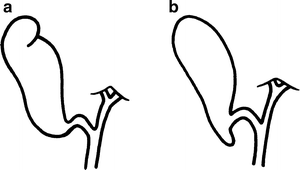

Figure 14.4.
Deformities of the gallbladder. (a) “Phrygian cap” deformity; (b) Hartmann’s pouch (by permission of JE Skandalakis, SW Gray, RR Ricketts, et al. The extrahepatic biliary ducts and the gallbladder. In: JE Skandalakis and SW Gray. Embryology for Surgeons, 2nd ed. Baltimore: Williams & Wilkins, 1994).
Common Bile Duct
The length of the common bile duct begins at the union of the cystic and common hepatic ducts and ends at the papilla of Vater in the second part of the duodenum. It varies from 5 to 16 cm depending on the actual position of the ductal union. The duct can be divided into four portions (Fig. 14.5): supraduodenal, retroduodenal, pancreatic, and intramural (intraduodenal).
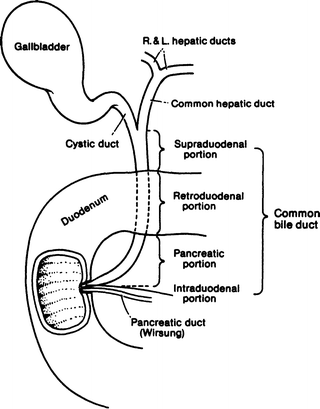

Figure 14.5.
The extrahepatic biliary tract and the four portions of the common bile duct (by permission of JE Skandalakis, SW Gray, and JR Rowe. Anatomical Complications in General Surgery. New York: McGraw-Hill, 1983).
The supraduodenal portion lies between the layers of the hepatoduodenal ligament in front of the epiploic foramen of Winslow, to the right or left of the hepatic artery, and anterior to the portal vein.
The retroduodenal portion is between the superior margin of the first portion of the duodenum and the superior margin of the head of the pancreas. The gastroduodenal artery lies to the left. The posterior superior pancreaticoduodenal artery lies anterior to the common bile duct. The middle colic artery lies anterior to the duct and other arteries.
The common bile duct may be partly covered by a tongue of pancreas (44 %) (Fig. 14.6a, b); completely within the pancreatic substance (30 %) (Fig. 14.6c); uncovered on the pancreatic surface (16.5 %) (Fig. 14.6d); or completely covered by two tongues of pancreas (9 %) (Fig. 14.6e). Even when completely covered, the groove or tunnel occupied by the duct may be palpated by passing the fingers of the left hand behind the second part of the duodenum after mobilization with the Kocher maneuver.
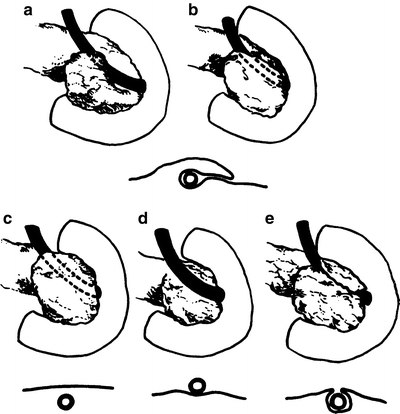

Figure 14.6.
Relation of the pancreas and the common bile duct. (a, b) The duct is partially covered by a tongue of pancreas (44 %). (c) The duct is completely covered by the pancreas (30 %). (d) The duct lies free on the surface of the pancreas (16.5 %). (e) The duct is covered by two tongues of pancreas with a cleavage plane between (by permission of JE Skandalakis, SW Gray, JS Rowe, et al. Contemp Surg 15(5):17–40, 1979).
The normal outside diameter of the first three regions of the common bile duct is variable, but a common bile duct more than 8 mm in diameter is definitely enlarged and, therefore, pathological.
The fourth, or intramural (sometimes called intraduodenal), portion of the common bile duct (see Fig. 9.9) passes obliquely through the duodenal wall together with the main pancreatic duct. Within the wall, the length averages 15 mm. As it enters the wall, the common duct decreases in diameter. The two ducts usually lie side by side with a common adventitia for several millimeters. The septum between the ducts reduces to a thin mucosal membrane before the ducts become confluent (see Chap. 9).
Hepatocystic Triangle and Triangle of Calot
The hepatocystic triangle is formed by the proximal part of the gallbladder and cystic duct to the right, the common hepatic duct to the left, and the margin of the right lobe of the liver superiorly (Fig. 14.7). The triangle originally described by Calot defined the upper boundary as the cystic artery. The area included in the triangle has enlarged over the years. Within the boundaries of the triangle as it is now defined are several structures that must be identified before they are ligated or sectioned.
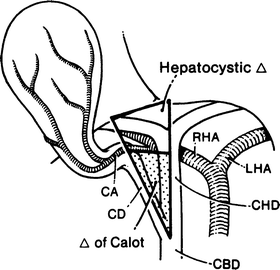

Figure 14.7.
The hepatocystic triangle and the triangle of Calot. The upper boundary of the hepatocystic triangle is the margin of the liver; that of the triangle of Calot is the cystic artery; the triangle of Calot is stippled. CA cystic artery, CD cystic duct, CBD common bile duct, RHA right hepatic artery, LHA left hepatic artery, CHD common hepatic duct (by permission of JE Skandalakis, SW Gray, RR Ricketts, et al. The extrahepatic biliary ducts and the gallbladder. In: JE Skandalakis and SW Gray. Embryology for Surgeons, 2nd ed. Baltimore: Williams & Wilkins, 1994).
The hepatocystic triangle contains the right hepatic artery (and sometimes an aberrant right hepatic artery), the cystic artery, and sometimes an aberrant (accessory) bile duct.
In 87 % of individuals, the right hepatic artery enters the triangle posterior to the common hepatic duct, and in 13 % it enters anterior to it. In one study of cadavers, the right hepatic artery could have been mistaken for the cystic artery 20 % of the time. As a rule of thumb, any artery more than 3 mm in diameter within the triangle will probably not be a cystic artery.
In 18 %, there was an aberrant right hepatic artery. In 83 % of these specimens, the cystic artery arose from the aberrant artery within the triangle. In 4 %, the aberrant artery was accessory to a normal right hepatic artery, and in 14 %, it was a replacing artery, the only blood supply to the right lobe of the liver (see Fig. 13.8).
The cystic artery usually arises from the right hepatic artery or an aberrant right hepatic artery within the hepatocystic triangle. At the neck of the gallbladder, the cystic artery divides into a superficial and a deep branch (Table 14.1).
Table 14.1
Origin of the cystic artery
Origin | Percent |
|---|---|
Right hepatic artery | |
Normal | 61.4 |
Aberrant (accessory) | 10.2 |
Aberrant (replacing) | 3.1 |
Left hepatic artery | 5.9 |
Bifurcation of common hepatic artery | 11.5 |
92.1 | |
Common hepatic artery | 3.8 |
95.9 | |
Gastroduodenal artery | 2.5 |
Superior pancreaticoduodenal artery | 0.15 |
Right gastric artery | 0.15 |
Celiac trunk | 0.3 |
Superior mesenteric artery | 0.9 |
Right gastroepiploic artery | Rare |
Aorta | Rare |
99.9 | |
In 16 %, there were aberrant (accessory) bile ducts within the hepatocystic triangle that may cause bile to leak into the abdominal cavity.
Vascular System of the Extrahepatic Biliary Tract
Arterial Supply
In general, the major blood vessels in the area of the extrahepatic biliary tree are posterior to the ducts, but in a number of cases they may lie anteriorly. The surgeon must recognize and preserve these arteries. Table 14.2 shows the frequency with which specific arteries are found anterior to segments of the biliary tract.
Table 14.2
Segments of the biliary tract and the frequency of arteries lying anterior to them
Segment | Artery anterior | Percent frequency |
|---|---|---|
Right and left hepatic ducts | Right hepatic artery | 12–15 |
Cystic artery | <5 | |
Common hepatic duct | Cystic artery | 15–24 |
Right hepatic artery | 11–19 | |
Common hepatic artery | <5 | |
Supraduodenal common bile duct | Anterior artery to common bile duct | 50 |
Posterior superior pancreaticoduodenal artery | 12.5 | |
Gastroduodenal artery | 5.7–20a | |
Right gastric artery | <5 | |
Common hepatic artery | <5 | |
Cystic artery | <5 | |
Right hepatic artery
Stay updated, free articles. Join our Telegram channel
Full access? Get Clinical Tree
 Get Clinical Tree app for offline access
Get Clinical Tree app for offline access

|