and John E. Skandalakis1
(1)
Centers for Surgical Anatomy and Technique, Emory University School of Medicine Piedmont Hospital, Atlanta, GA, USA
Abstract
Several structures lying close to the esophageal hiatus of the diaphragm may be injured in surgical procedures on the hiatus. The anatomic proximity of the lower third of the esophagus to the right pleura creates the risk of accidental entrance into the pleural cavity during abdominal operations on the esophageal hiatus.
Hiatus hernia is a protrusion of a portion of the stomach into the thoracic mediastinum through the esophageal hiatus of the diaphragm. Anatomic descriptions and step-by-step technique are provided for the treatment of various types of hiatus hernia (sliding hiatus, paraesophageal hiatus, combined sliding and paraesophageal, congenital short esophagus, and traumatic diaphragmatic). Laparoscopic Nissen fundoplication has replaced the traditional open operation; newly revised material details this procedure.
Anatomy
The diaphragm is a musculomembranous entity separating the thorax from the abdomen. The muscular part originates anteriorly from the xiphoid process, laterally from the inner surface of the six lower cartilages, and posteriorly from the medial and lateral lumbosacral arches, the median arcuate ligament, and the bodies of the three upper lumbar vertebrae. The muscular part inserts on the central tendon.
Crura
The crura arise from the anterior surface of the first to fourth lumbar vertebrae on the right, the first two or three lumbar vertebrae on the left, and from the intervertebral disks and the anterior longitudinal ligament. The crural fibers pass superiorly and anteriorly, forming the muscular arms that surround the openings for the aorta and the esophagus. They then insert on the central tendon. At their origins from the vertebrae, the crura are tendinous, becoming increasingly muscular as they ascend into the diaphragm proper (Fig. 5.1). Studies have found that in 90 % of cadavers, posteriorly and medially, from their vertebral origins to the level of the tenth thoracic vertebra, the crura are tendinous. Sutures to approximate the crura should always be placed through the tendinous portions.
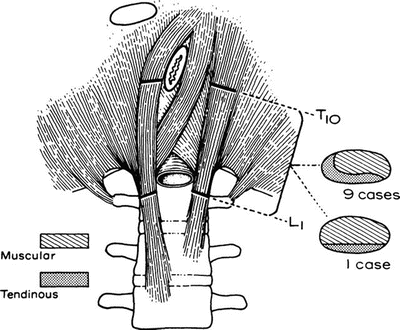

Figure 5.1.
The crura consist of both tendinous and muscular tissue; only the tendinous portion holds sutures. In nine out of ten persons, the medial edge of the crura is tendinous. From SW Gray, JS Rowe, and JE Skandalakis. Surgical anatomy of the gastroesophageal junction. Am Surg 45(9):575–587, 1979. Reprinted with permission from American Surgeon.
The pattern of the crural arms at the esophageal hiatus is variable. In one-half or more, both right and left arms arise from the right crus (Fig. 5.2a). In another one-third or more, the left arm arises from the right crus and the right arm arises from both crura (Fig. 5.2b). The remaining individuals present a variety of uncommon patterns. Hiatal hernia is not associated with any specific hiatal pattern.


Figure 5.2.
The most common patterns of the diaphragmatic crura. (a–1) and (b–1) seen from below. (a–2, a–3) and (b–2, b–3) seen from above. E esophagus, A aorta (By permission of JE Skandalakis, SW Gray, JS Rowe, et al. In: LM Nyhus, and RJ Baker. Mastery of Surgery, 2nd ed. Boston: Little, Brown, 1992, pp. 377–396).
Openings of the Diaphragm
Hiatus of the Inferior Vena Cava
The hiatus of the inferior vena cava lies in the right dome of the central tendon about 2.5 cm to the right of the midline and at the level of the eighth thoracic vertebra. The margins of the hiatus are fixed to the vena cava, which is accompanied by branches of the right phrenic nerve (Fig. 5.3).
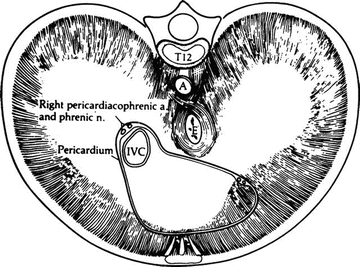

Figure 5.3.
The diaphragm viewed from above. The area in contact with the pericardium is indicated. The pericardial fibrous tissue is continuous with that of the diaphragm (By permission of JE Skandalakis, SW Gray, JS Rowe, et al. In: LM Nyhus, and RJ Baker. Mastery of Surgery, 2nd ed. Boston: Little, Brown, 1992, pp. 377–396).
Esophageal Hiatus
The elliptical esophageal hiatus is in the muscular portion of the diaphragm 2.5 cm or less to the left of the midline at the level of the tenth thoracic vertebra (Figs. 5.4 and 5.5). The anterior and lateral margins of the hiatus are formed by the muscular arms of the diaphragmatic crura. The posterior margin is formed by the median arcuate ligament (Fig. 5.6). The anterior and posterior vagal trunks and the esophageal arteries and veins from the left gastric vessels pass through the hiatus with the esophagus.
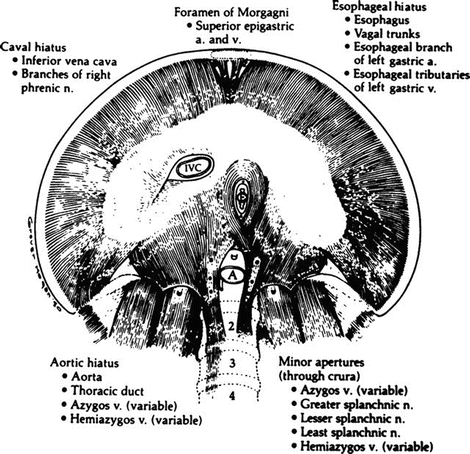
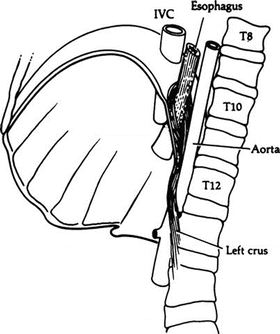
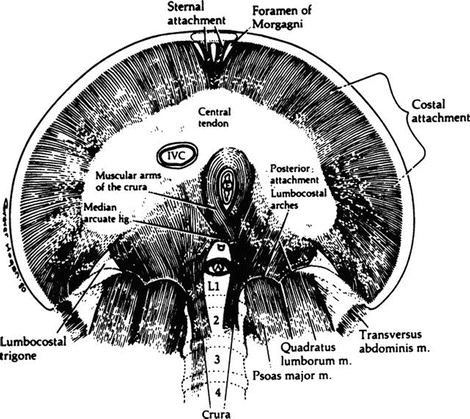

Figure 5.4.
The apertures of the diaphragm seen from below and the structures traversing them (By permission of JE Skandalakis, SW Gray, JS Rowe, et al. In: LM Nyhus, and RJ Baker. Mastery of Surgery, 2nd ed. Boston: Little, Brown, 1992, pp. 377–396).

Figure 5.5.
The diaphragmatic openings for the inferior vena cava (IVC), the esophagus, and the aorta as seen from the left (By permission of JE Skandalakis, SW Gray, JS Rowe, et al. In: LM Nyhus, and RJ Baker. Mastery of Surgery, 2nd ed. Boston: Little, Brown, 1992, pp 377–396).

Figure 5.6.
The attachments of the muscles of the diaphragm seen from below (By permission of JE Skandalakis, SW Gray, JS Rowe, et al. In: LM Nyhus, and RJ Baker. Mastery of Surgery, 2nd ed. Boston: Little, Brown, 1992, pp. 377–396).
Regardless of its components, the normal hiatus should admit one or two of the surgeon’s fingers if there is no folding of the peritoneum into the mediastinum.
The following means of narrowing the hiatus have been preferred:
Vertical posterior approximation of the crura (Fig. 5.7a). This is a commonly used method.
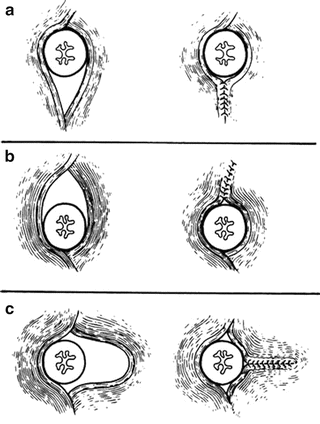
Figure 5.7.
Three methods of narrowing the esophageal hiatus. (a) Vertical with posterior approximation of the crura. (b) Vertical with anterior approximation of the crura. (c) Horizontal with shortening of one crus (By permission of JE Skandalakis, SW Gray, and JR Rowe Jr. Anatomical Complications in General Surgery. New York: McGraw Hill, 1983).
Vertical anterior approximation of the crura (Fig. 5.7b). Some surgeons recommend this type of repair. It has the following advantages: (1) it is easier than posterior approximation; (2) the crura are more tendinous anteriorly; and (3) the procedure accentuates the gastroesophageal angle.
Horizontal narrowing of the hiatus (Fig. 5.7c). In some patients, a transverse defect is apparent; hence a horizontal approximation is appropriate.
Aortic Opening
The oblique course of the aorta takes it behind the diaphragm rather than through it (Fig. 5.5). The thoracic duct and (usually) the azygos vein accompany the aorta through the “opening.” At the level of the 12th thoracic vertebra, the anterior border of the opening is bridged by the median arcuate ligament. Laterally the diaphragmatic crura form the margins of the opening.
Other Openings in the Diaphragm
Anteriorly, the superior epigastric vessels pass through the parasternal spaces (foramina of Morgagni). In the dome of the diaphragm, the phrenic nerves pierce the upper surface to become distributed over the lower surface between the muscle and peritoneum.
The azygos vein may pass behind the diaphragm with the aorta (to the right of the right crus), or it may pierce the right crus. Also passing through the crura are the greater, lesser, and least thoracic splanchnic nerves (Fig. 5.4).
Median Arcuate Ligament
The esophageal hiatus is separated from the aortic hiatus by fusion of the arms of the left and right crura. If the tendinous portions of the crura are fused, the median arcuate ligament is present as a fibrous arch passing over the aorta, connecting the right and left crura. If the fusion is muscular only, the ligament is ill defined or absent.
The median arcuate ligament passes in front of the aorta at the level of the first lumbar vertebra, just above the origin of the celiac trunk (Fig. 5.6). In 16 %, a low median arcuate ligament covers the celiac artery and may compress it.
In about 50 % of cadavers with hiatal hernia studied, the ligament was sufficiently well developed to use in surgical repair of the esophageal hiatus. In the remainder, there was enough preaortic fascia lateral to the celiac trunk to perform a posterior fixation of the gastroesophageal junction (GEJ). At operation surgeons must avoid the celiac ganglion, which is just below the arcuate ligament.
Diaphragmatic-Mediastinal Relations
The fibrous tissue of the central tendon is continuous with the fibrous pericardium over much of the anterosuperior surface of the diaphragm (Fig. 5.3).
In addition to the pericardium, the mediastinum on the right contains the inferior vena cava; right phrenic nerve and pericardiophrenic vessels; right pulmonary ligament; esophagus with the right vagal trunk; thoracic duct; azygos vein and azygos arch; vertebral bodies; greater and lesser right thoracic splanchnic nerves; right sympathetic trunk; and right posterior intercostal arteries (Fig. 5.8).
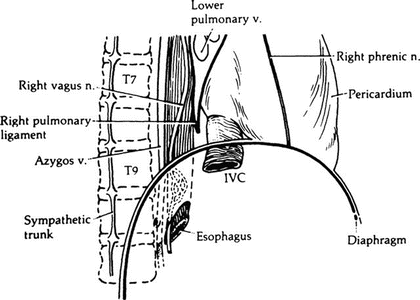

Figure 5.8.
Structures in the inferior portion of the right mediastinum (By permission of JE Skandalakis, SW Gray, JS Rowe, et al. In: LM Nyhus, and RJ Baker. Mastery of Surgery, 2nd ed. Boston: Little, Brown, 1992, pp. 377–396).
In the left mediastinum are the pericardium; left phrenic nerve and pericardiophrenic vessels; esophagus; left vagal trunk; descending aorta; vertebral bodies; hemiazygos vein, accessory hemiazygos vein, highest intercostal vein; greater and lesser left thoracic splanchnic nerves; and left sympathetic trunk.
The triangle (of Truesdale) formed by the pericardium, aorta, and diaphragm contains the left pulmonary ligament and the distal esophagus. In sliding hiatus hernia, the stomach is in this triangle (Fig. 5.9).
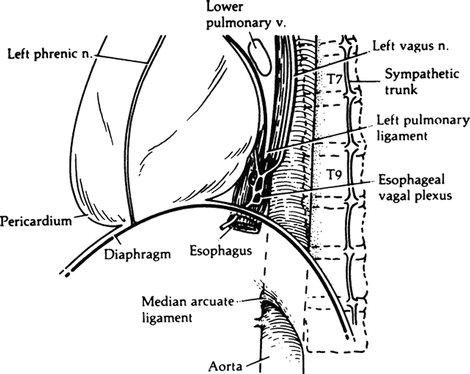

Figure 5.9.
Structures in the inferior portion of the left mediastinum (By permission of JE Skandalakis, SW Gray, JS Rowe, et al. In: LM Nyhus, and RJ Baker. Mastery of Surgery. 2nd ed. Boston: Little, Brown, 1992, pp. 377–396).
The remainder of the superior surface of the diaphragm is covered with parietal pleura. The approximation of the right and left pleurae between the esophagus and the aorta forms the so-called mesoesophagus. The right pleura is in contact with the lower third of the esophagus almost as far down as the esophageal hiatus (Fig. 5.10). This proximity creates the risk of accidental entrance into the pleural cavity during abdominal operations on the esophageal hiatus. Even so, because surgeons work on the right side of the operating table, they are more likely to produce a pneumothorax or hemopneumothorax on the left.
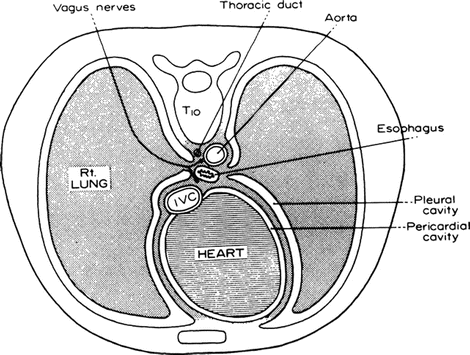

Figure 5.10.
Cross section through the thorax at the level of T10 showing the relation of the pleura to the distal esophagus. From SW Gray, JS Rowe, and JE Skandalakis. Surgical anatomy of the gastroesophageal junction. Am Surg 45(9):575–587, 1979. Reprinted with permission from American Surgeon.
Vascular System of the Diaphragm
Arterial Supply
The arterial supply to the superior surface of the diaphragm consists of two branches from the internal thoracic arteries—the pericardiophrenic and musculophrenic arteries—and two branches from the thoracic aorta—the superior phrenic arteries. All these branches are small.
The major blood supply to the diaphragm is to the inferior surface. It comes from the inferior phrenic arteries, which arise from the aorta or the celiac axis just below the median arcuate ligament of the diaphragm. In a small percentage of individuals, the right inferior phrenic artery arises from the right renal artery. The inferior phrenic arteries also supply branches to the suprarenal glands (Fig. 5.11).
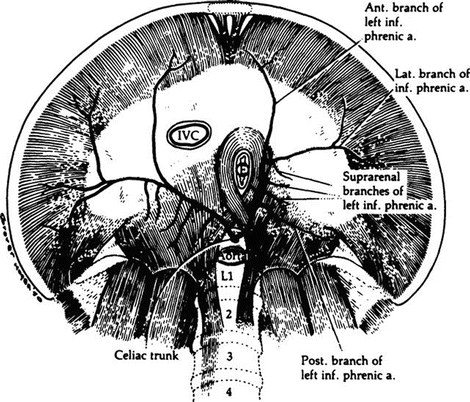

Figure 5.11.
Arterial supply of the diaphragm from below. The inferior phrenic arteries may arise from the celiac trunk or directly from the aorta (By permission of JE Skandalakis, SW Gray, JS Rowe, et al. In: LM Nyhus, RJ Baker. Mastery of Surgery, 2nd ed. Boston: Little, Brown, 1992, pp 377–396).
Venous Drainage
On the superior and inferior surfaces, the veins run with the arteries (Fig. 5.12).
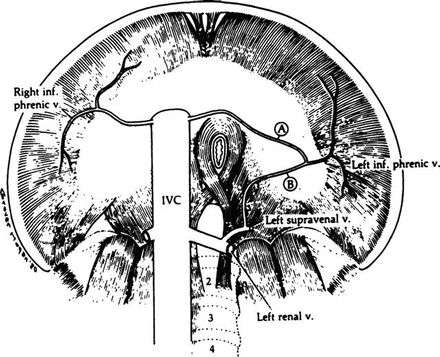

Figure 5.12.




Venous drainage of the diaphragm from below. The left inferior phrenic vein may enter the inferior vena cava (A), the left suprarenal vein (B), or both (By permission of JE Skandalakis, SW Gray, JS Rowe, et al. In: LM Nyhus, RJ Baker. Mastery of Surgery, 2nd ed. Boston: Little, Brown, 1992, pp. 377–396.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


