and John E. Skandalakis1
(1)
Centers for Surgical Anatomy and Technique, Emory University School of Medicine Piedmont Hospital, Atlanta, GA, USA
Abstract
The classic anatomic divisions of the colon are the cecum, colon proper, rectum, and anal canal. A surgical unit, the right colon, is composed of the cecum, ascending colon, and hepatic flexure. The surgical unit of the left colon consists of the distal transverse colon, splenic flexure, and descending and sigmoid colons. The layers of the wall of the large intestine are essentially similar to those of the wall of the small intestine. Evacuation is accomplished by the pelvic splanchnic nerves; continence is maintained by the pudendal and the pelvic splanchnic nerves.
A “decalogue of good colon surgery” introduces detailed step-by-step technique for performing cecopexy (colostomies), colon resection, (colectomies), abdominoperineal resections, and laparoscopic colectomies. Procedures of the surgical anal canal and perianal regions include repair of anal fissure, ligation of intersphincteric fistula tract (LIFT), hemorrhoidectomy (internal, external, thrombosed, band ligation), and excision of pilonidal cyst.
Anatomy
General Description of Colon and Anorectum
The large intestine, or colon, about 144 cm long, extends from the terminal ileum to the anus. The classic divisions are the cecum, colon proper, rectum, and anal canal. A surgical unit, the right colon, is composed of the cecum, ascending colon, and hepatic flexure. The surgical unit of the left colon consists of the distal transverse colon, splenic flexure, and descending and sigmoid colons.
Cecum
The cecum—the first 5 cm of the large bowel just below the ileocecal valve—lies in the right iliac fossa, and in about 60 % of living, erect individuals, it lies partly in the true pelvis. In approximately 20 %, almost the entire posterior surface of the cecum is attached to the posterior abdominal wall, and, at the other extreme, in approximately 24 %, the cecum is wholly unattached. Among the latter are cases of pathologically mobile cecum, in which the lower part of the ascending limb, in addition to the cecum, is unattached.
A fold of peritoneum from the mesentery of the terminal ileum may cross the ileum to attach to the lower colon and the cecum. This fold, the mesentery, and the ileum may form a superior ileocecal fossa. Below is an inferior ileocecal fold and an inferior ileocecal fossa (Fig. 12.1). These folds are inconstant, and the associated fossae can be shallow or absent. Occasionally a retrocecal fossa is present. In some subjects a fixed terminal ileum may be present and, rarely, a common ileocecal mesentery.
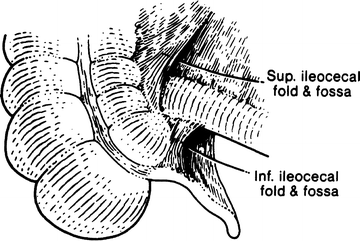

Figure 12.1.
Superior and inferior ileocecal folds forming fossae (By permission of JE Skandalakis, SW Gray, and JR Rowe. Anatomical Complications in General Surgery. New York: McGraw-Hill, 1983).
Colon Proper
The ascending limb of the colon proper is normally fused to the posterior body wall and covered anteriorly by the peritoneum. There are variations of incomplete fusion ranging from a deep lateral paracolic groove to the persistence of an entire ascending mesocolon (Fig. 12.2). A mesocolon long enough to permit volvulus occurs in approximately 11 %. In cadavers, the ascending colon may be mobile in approximately 37 % of cases. A mobile cecum, together with a mobile right colon, may be present.
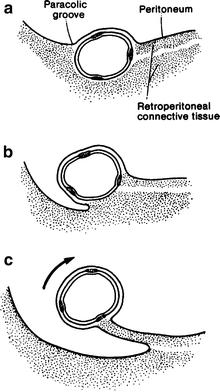

Figure 12.2.
Degrees of attachment of the right colon to the abdominal wall. (a) Normal retroperitoneal location of the colon. (b) Paracolic gutter. (c) Mobile colon with mesentery (By permission of JE Skandalakis, SW Gray, and JR Rowe. Anatomical Complications in General Surgery. New York: McGraw-Hill, 1983).
Where the mesocolon is present, the cecum and the proximal ascending colon are unusually mobile. It is this condition that is termed mobile cecum and which can result in volvulus of the cecum and the right colon (Fig. 12.3) as well as cecal bascule.
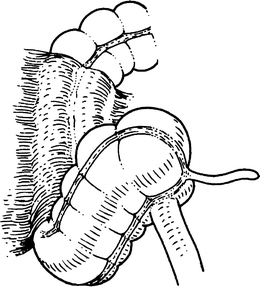

Figure 12.3.
Mobile cecum, distal ileum, and proximal right colon. This configuration is subject to volvulus (By permission of JE Skandalakis, SW Gray, and JR Rowe. Anatomical Complications in General Surgery. New York: McGraw-Hill, 1983).
Two conditions must be present for right colon volvulus to occur: (1) an abnormally mobile segment of colon and (2) a fixed point around which the mobile segment can twist.
The transverse colon begins where the colon turns sharply to the left (the hepatic flexure) just beneath the inferior surface of the right lobe of the liver. It ends at a sharp upward and then downward bend (the splenic flexure) related to the posterolateral surface of the spleen. The tail of the pancreas is above. The anterior surface of the left kidney lies medially.
The transverse colon has a mesentery which has fused secondarily with the posterior wall of the omental bursa (see Fig. 8.1). At the splenic flexure, the colon is supported by the phrenocolic ligament, a part of the left side of the transverse mesocolon.
The descending colon is covered anteriorly and on its medial and lateral sides by peritoneum. It normally has no mesentery. When a mesentery exists, it is rarely long enough to permit a volvulus to occur.
At the level of the iliac crest, the descending colon becomes the sigmoid colon and acquires a mesentery. The sigmoid colon is described as having two portions: iliac (fixed) and pelvic (mobile). The average length of the attachment and the average breadth of the mesentery are shown in Fig. 12.4a. The left ureter passes through the base of the sigmoid mesocolon through the intersigmoid mesenteric recess (Fig. 12.4b).
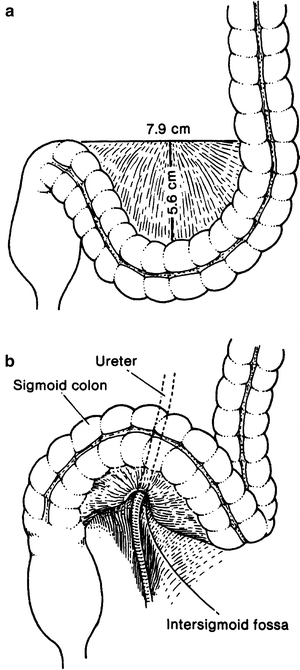

Figure 12.4.
(a) Average measurements of the sigmoid mesocolon. (b) The relation of the base of the sigmoid mesocolon to the left ureter (By permission of JE Skandalakis, SW Gray, and JR Rowe. Anatomical Complications in General Surgery. New York: McGraw-Hill, 1983).
Rectum and Anal Canal
There are many definitions of the junction between the sigmoid colon and the rectum that are inconsistent with each other. Most surgeons consider the rectosigmoid junction to be at the level of the sacral promontory. Anatomists consider the rectosigmoid junction to be located at the level of S3. Others consider the rectosigmoid junction to be the narrowest portion of the large intestine where the teniae fuse together to form a single anterior tenia. The haustra and mesocolon terminate and the diverticula are no longer able to form.
The surgeon considers the anal canal to be the region lying distal to the insertion of the levator ani muscle. The surgical anal canal has a length of 4 cm: 2 cm above the pectinate line and 2 cm below (Fig. 12.5). The functional anal canal extends for 4 cm from the anorectal ring to the intersphincteric groove.
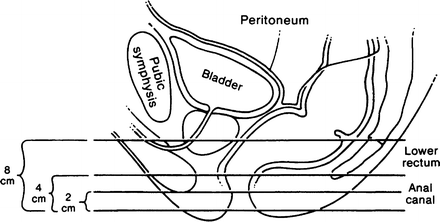

Figure 12.5.
The line of peritoneal reflection on the rectum; lateral view in the male. More of the rectum is covered anteriorly than posteriorly. The measurements of the anal canal and lower rectum from the anal verge are approximate (By permission of JE Skandalakis, SW Gray, and JR Rowe. Anatomical Complications in General Surgery. New York: McGraw-Hill, 1983).
Layers of Wall of Large Intestine
Colon
The layers of the wall of the large intestine are essentially similar to those of the wall of the small intestine. The chief differences are (1) the absence of mucosal villi, (2) longitudinal muscularis externa in three discrete bands (teniae) rather than in a continuous cylinder, (3) the presence of epiploic appendices (appendages); and (4) the presence of haustra or sacculations.
The epiploic appendages are of interest to the surgeon because they may be the sites of diverticula (Fig. 12.6a). Fat may conceal the presence of the diverticulum on inspection, but fecaliths in the diverticula are frequently palpable. The appendages are also subject to infarction and torsion; both produce symptoms of an acute abdomen. Epiploic appendages should be ligated without traction. This prevents unintentional pulling of a loop of a long colic artery into the appendiceal neck and its accidental inclusion in the ligation (Fig. 12.6b).
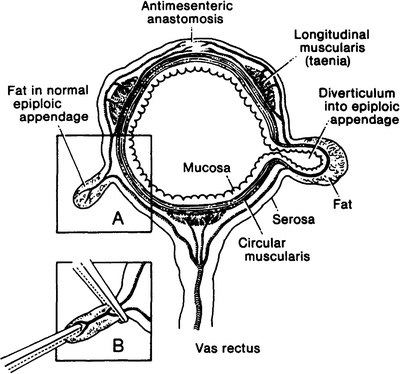

Figure 12.6.
Diagram of the transverse colon showing long and short branches of the vasa recta. On the left is a normal epiploic appendage; on the right, a diverticulum extending into an epiploic appendage. Inset: Effect of too much traction on an epiploic appendage resulting in injury to a long branch of a vas rectus followed by antimesenteric ischemia (By permission of JE Skandalakis, SW Gray, and JR Rowe. Anatomical Complications in General Surgery. New York: McGraw-Hill, 1983).
Rectum
Grossly, the rectum has no teniae, epiploic appendages, or haustra. The rectum is 12–15 cm in length. It passes through the levator ani to become the anal canal. After surgical mobilization, the rectum can be stretched to 15–20 cm in length. The valves/folds straighten out and contribute to the extra length.
The upper rectum contains one to four crescentic plicae, the rectal folds, or valves of Houston. Typically there are three folds: left superior, right middle, and left inferior. The folds are encountered by the sigmoidoscope at 4–7, 8–10, and 10–12 cm from the anal verge. The middle rectal fold corresponds to the level of the anterior peritoneal reflection
Anal Canal
The Musculature of the Wall of the Anal Canal
The anorectal ring (palpable as the puborectalis) is located at the junction of the internal anal sphincter and the levator ani complex. The anal canal is approximately 4 cm long.
Two layers of smooth muscle surround the anal canal. The innermost layer is formed by a greatly thickened circular coat which is continuous with the circular muscularis externa of the colon. This is the internal sphincter of the anal canal (Fig. 12.7). The second smooth muscle layer is composed of longitudinal fibers continuous with the fibers of the teniae coli. It descends between the internal and external anal sphincters. The lowest portions traverse the external anal sphincters.
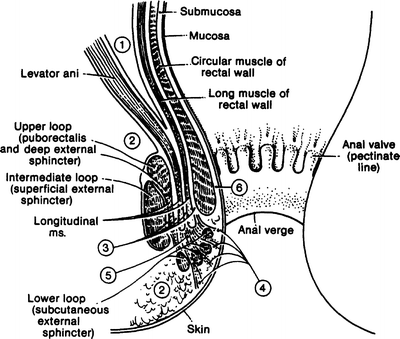

Figure 12.7.
The spaces of the anus and rectum: (1) pelvirectal space; (2) ischiorectal space; (3) intersphincteric spaces; (4) subcutaneous space; (5) central space; (6) submucous space (By permission of JE Skandalakis, SW Gray, and JR Rowe. Anatomical Complications in General Surgery. New York: McGraw-Hill, 1983).
The longitudinal muscle fibers prevent separation of the sphincteric elements from each other and also permit a telescopic movement between internal and external sphincters. We witness this in the operating room when the external sphincter rolls back and the internal sphincter rolls forward.
Composed of striated muscle, the external sphincter has three separate fiber bundles or loops: subcutaneous, superficial, and deep. It is useful to consider the three parts separately (Figs. 12.8 and 12.9), but the three loops together form an efficient anal closure. Any single one of the loops is capable of maintaining continence to solid stools but not to fluid or gas. The subcutaneous portion surrounds the outlet of the anus, attaching to the perianal skin anteriorly. Some fibers completely encircle the anus.
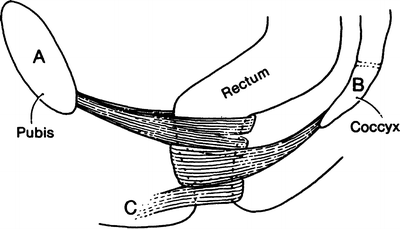
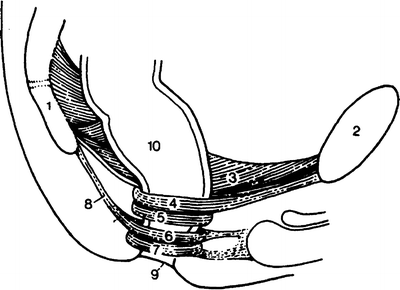

Figure 12.8.
The three loops of the external anal sphincter. Each loop is a separate sphincter with distinct attachments, muscle bundles, and innervations. Continence depends on the preservation of at least one of the three. Some subcutaneous muscle fibers encircle the anus; some attach to the perianal skin anteriorly at C (By permission of JE Skandalakis, SW Gray, and JR Rowe. Anatomical Complications in General Surgery. New York: McGraw-Hill, 1983).

Figure 12.9.
Diagram of the extrinsic muscles of the surgical anal canal. (1) Coccyx; (2) pubis; (3) levator ani muscle; (4) puborectalis muscle; (5) deep external sphincter; (6) superficial external sphincter; (7) subcutaneous external sphincter; (8) anococcygeal ligament; (9) anal verge; (10) rectum (By permission of JE Skandalakis, SW Gray, and JR Rowe. Anatomical Complications in General Surgery. New York: McGraw-Hill, 1983)
The superficial portion surrounds the anus and continues within the anococcygeal ligament, which attaches posteriorly to the coccyx. This creates the small triangular space of Minor behind the anus. Anteriorly, some fibers insert into the transverse perineal muscles at the perineal body, creating a potential space toward which anterior midline fistulas may point. The deep portion surrounds the canal, with no obvious anterior or posterior attachments. In Shafik’s view, the deep portion and the puborectalis muscle are a single unit.
Lining of the Surgical Anal Canal
There are three histologic regions of the anal canal, which extend from the anal verge to approximately 1 cm above the dentate line. The cutaneous zone, up to the anal verge (anocutaneous line), is covered by pigmented skin that has hair follicles and sebaceous glands. Above the anal verge is the transitional zone, which consists of modified skin that has sebaceous glands without hair. It extends to the pectinate line defined by the free edges of the anal valves. Above the line begins the true mucosa of the anal canal (Fig. 12.10).
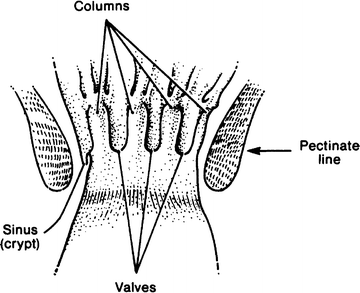

Figure 12.10.
The interior of the anal canal showing the rectal columns, anal valves, and anal sinuses (crypts). They form the pectinate line (By permission of JE Skandalakis, SW Gray, and JR Rowe. Anatomical Complications in General Surgery. New York: McGraw-Hill, 1983).
The pectinate line is formed by the margins of the anal valves—small mucosal pockets between the five and ten vertical folds of the mucosa known as the anal columns of Morgagni. An anal pit or sinus is located above each valve, draining the anal glands. These columns extend upward from the pectinate line to the upper end of the surgical anal canal, at the level of the puborectalis sling. They are formed by underlying parallel bundles of the muscularis mucosae. The actual junction of stratified squamous and columnar epithelia is usually just above the pectinate line; hence, the mucocutaneous line is not precisely equivalent to the pectinate line.
The pectinate line is the most important landmark in the anal canal. It marks the transition between the visceral area above and the somatic area below. The arterial supply, the venous and lymphatic drainage, the nerve supply, and the character of the lining all change at or very near the pectinate line (Table 12.1).
Table 12.1
The pectinate line and changes in the surgical anal canal
Below the pectinate line | Above the pectinate line | |
|---|---|---|
Embryonic origin | Ectoderm | Endoderm |
Anatomy | ||
Lining | Stratified squamous | Simple columnar |
Arterial supply | Inferior rectal artery | Superior rectal artery |
Venous drainage | Systemic, by way of inferior rectal vein | Portal, by way of superior rectal vein |
Lymphatic drainage | To inguinal nodes | To pelvic and lumbar nodes |
Nerve supply | Inferior rectal nerves (somatic) | Autonomic fibers (visceral) |
Physiology | Excellent sensation | Sensation quickly diminishes |
Pathology | ||
Cancer | Squamous cell carcinoma | Adenocarcinoma |
Varices | External hemorrhoids | Internal hemorrhoids |
Peritoneal Reflections
The entire upper one-third of the rectum is covered by peritoneum (Fig. 12.5). The peritoneum leaves the rectum and passes anteriorly and superiorly over the posterior vaginal fornix and the uterus in females or over the superior ends of the seminal vesicles and the bladder in males. This creates a depression, the rectouterine or rectovesical pouch.
Fascial Relations and Tissue Spaces
Shafik recognized six potential spaces around the rectum. They are important because they may become sites of infection. Knowledge of the spaces will avert injury during surgery. The fascial layers that bound these spaces help limit the spread of both infection and neoplastic disease, although all the spaces are potentially confluent with one another (Figs. 12.7 and 12.11).
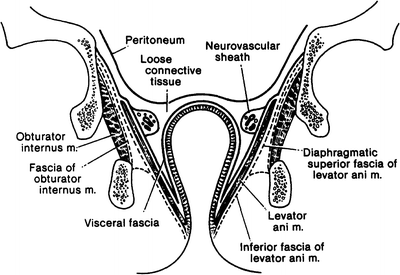

Figure 12.11.
Diagram of some of the fasciae of the pelvis seen in coronal section (By permission of JE Skandalakis, SW Gray, and JR Rowe. Anatomical Complications in General Surgery. New York: McGraw-Hill, 1983).
The perianal space surrounds the anal canal along the anal verge and is surrounded laterally by fat. The perianal space connects to the superficial postanal space, which is the space located below the anococcygeal ligament. The perianal space also communicates with the intersphincteric space, which is located between the anal sphincters. The intersphincteric space contains most of the anal glands. The ischiorectal space is lateral to the perianal space and contains the pudendal nerves and vessels. The apex of the ischiorectal space is formed by the levator and obturator muscles. The ischiorectal space is bound anteriorly by the transverse perineal muscles and bound posteriorly by the gluteal skin. Posteriorly, the ischiorectal space communicates with the deep postanal space, deep to the anococcygeal ligament. An infection communicating in this space is the horseshoe abscess.
Pelvic Diaphragm and Continence
The floor of the pelvis is the pelvic diaphragm (Fig. 12.12), which is composed of two paired muscles: the levator ani and the coccygeus. The levator ani can be considered to be made up of three muscles: the iliococcygeus, the pubococcygeus, and the puborectalis.
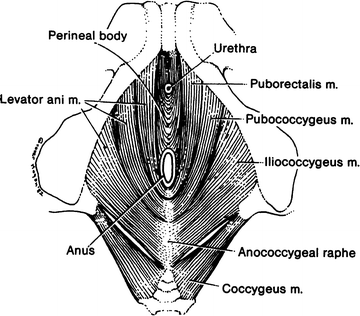

Figure 12.12.
Diagram of the pelvic diaphragm from below. Note that the levator ani is composed of three muscles: puborectalis, pubococcygeus, and iliococcygeus. Some authors would exclude the puborectalis from the levator ani (By permission of JE Skandalakis, SW Gray, and JR Rowe. Anatomical Complications in General Surgery. New York: McGraw-Hill, 1983).
The puborectalis, the superficial and deep parts of the external sphincter, and the proximal part of the internal sphincter form the so-called anorectal ring. This ring can be palpated; since cutting through it will produce incontinence, it must be identified and protected during surgical procedures. The puborectalis is essential to maintaining rectal continence and is considered by some authors to be part of the external sphincter and not a part of the levator ani. The puborectalis is attached to the lower back surface of the symphysis pubis and the superior layer of the deep perineal pouch (urogenital diaphragm). Fibers from each side of the muscle pass posteriorly and then join posterior to the rectum, forming a well-defined sling (Fig. 12.12). The puborectalis passes adjacent to the vagina where it attaches laterally and is known as the pubovaginalis, supporting the rectum and vagina. It also supports the bladder and the urethra, pulling these anteriorly with contractions. When the puborectalis is lax, the levator sags, the anorectal angle becomes obtuse, and the pelvic floor muscles can relax. Over time, the pelvic floor weakens, a change that can lead to pelvic organ prolapse and incontinence.
Vascular System of the Colonand Rectum
Arteries of the Colon
Superior Mesenteric Artery
The cecum and the ascending colon receive blood from two arterial branches of the superior mesenteric artery: the ileocolic and right colic arteries (Fig. 12.13). These arteries form arcades from which vasa recta pass to the medial colonic wall.
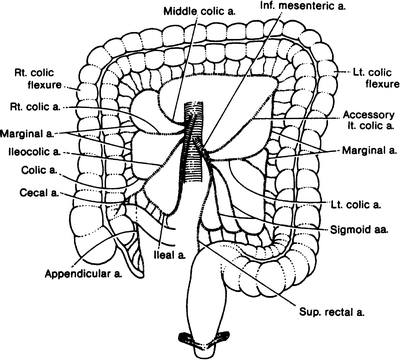

Figure 12.13.
Schema of the blood supply to the large intestine. There are many variations of this basic pattern (By permission of JE Skandalakis, SW Gray, and JR Rowe. Anatomical Complications in General Surgery. New York: McGraw-Hill, 1983).
As the vasa recta reach the surface of the colon, they divide into short and long branches, the former serving the medial or mesenteric side of the colon and the latter serving the lateral and antimesenteric side. The long branches send twigs into the epiploic appendages (see Fig. 12.6).
Middle Colic Artery
The transverse colon is similarly supplied by the middle colic artery from the superior mesenteric artery. A study found that in about one-third of cases the splenic flexure was supplied by the middle colic artery; in the remainder, the flexure and the left portion of the transverse colon were supplied by the left colic artery, a branch of the inferior mesenteric artery.
Inferior Mesenteric Artery
The inferior mesenteric artery arises from the aorta opposite the lower portion of the third lumbar vertebra. The length of the artery prior to its first branch varies from 1.5 to 9.0 cm.
The branches of the inferior mesenteric artery are the left colic artery, with its ascending and descending branches for the descending colon, one to nine sigmoid arteries for the sigmoid colon, and the superior rectal (hemorrhoidal) artery for the rectum (Figs. 12.13 and 12.14c). An accessory middle colic artery is present in roughly 40 % of subjects.
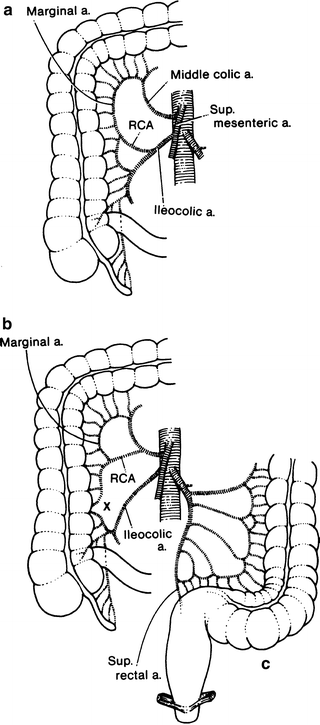

Figure 12.14.
Variations of the arteries to the right colon. RCA right colic artery (a) Usual pattern. (b) The marginal artery is incomplete at “X.” (c) Arteries to the left colon. There may be fewer sigmoid arteries than shown here (By permission of JE Skandalakis, SW Gray, and JR Rowe. Anatomical Complications in General Surgery. New York: McGraw-Hill, 1983).
Division of the inferior mesenteric artery close to its root has been shown to increase the reach of the colon to the pelvis after proctectomy, leading to less tension on the colorectal or coloanal anastomosis.
Marginal Artery (of Drummond)
The marginal artery is composed of a series of anastomosing arcades between branches of the ileocolic, right colic, middle colic, left colic, and sigmoidal arteries. These form a single, looping vessel. The marginal artery courses roughly parallel with the mesenteric border of the large intestine, from 1 to 8 cm from the intestinal wall (Fig. 12.14a–c). It may or may not terminate at the superior rectal artery (Fig. 12.14c). Occasionally, however, the continuity of this artery is disrupted in one or more points.
Arteries of the Rectum and Anal Canal
The arteries of the rectum and anal canal are the unpaired superior rectal artery, the paired middle and inferior rectal arteries, and median sacral rectal arteries (Fig. 12.15). The superior rectal (hemorrhoidal) artery arises from the inferior mesenteric artery and descends to the posterior wall of the upper rectum. Supplying the posterior wall, it divides and sends right and left branches to the lateral walls of the middle portion of the rectum down to the pectinate (dentate) line.
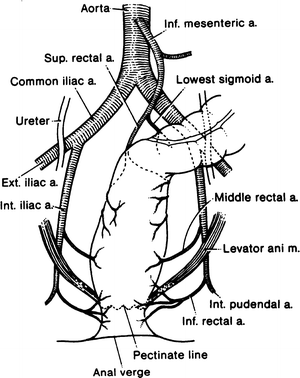

Figure 12.15.
Diagram of the arterial supply to the rectum and anus. The median sacral artery supplying a few small branches to the posterior wall of the rectum is not shown in this figure (By permission of JE Skandalakis, SW Gray, and JR Rowe. Anatomical Complications in General Surgery. New York: McGraw-Hill, 1983).
One study has found that the main trunk of the middle rectal artery was inferior to the rectal stalk and could be endangered when the rectum is separated from the seminal vesicle, prostate, or vagina. In our experience, the middle rectal artery is usually absent in the female. It is probably replaced by the uterine artery. In the male, the chief beneficiaries of the artery are the rectal musculature and the prostate gland.
The inferior rectal (hemorrhoidal) arteries arise from the internal pudendal arteries and proceed ventrally and medially to supply the anal canal distal to the pectinate line.
The median sacral artery arises just above the bifurcation of the aorta and descends beneath the peritoneum on the anterior surface of the lower lumbar vertebrae, the sacrum, and the coccyx. It sends several very small branches to the posterior wall of the rectum.
Venous Drainage of the Colon, Rectum, and Anus
The veins of the colon follow the arteries. On the right, the veins join to form the superior mesenteric vein. The superior rectal vein drains the descending and sigmoid colon; it passes upward to form the inferior mesenteric veins.
The rectum is drained by the superior rectal veins, which enter the inferior mesenteric veins. This drainage is to the portal system. The middle and inferior rectal veins enter the internal iliac vein and thus drain into the systemic circulation (Fig. 12.16).
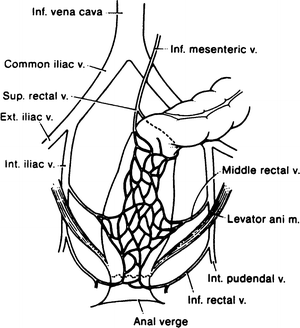

Figure 12.16.
Diagram of the venous drainage of the rectum and anus. The superior rectal vein drains to the portal system, and the middle and inferior rectal veins drain to the systemic veins. The venous plexus between the veins forms a portacaval shunt (By permission of JE Skandalakis, SW Gray, and JR Rowe. Anatomical Complications in General Surgery. New York: McGraw-Hill, 1983).
Remember:
✓ Anastomoses occur between the superior rectal vein (portal) and the middle and inferior rectal veins (systemic), constituting a potential portosystemic shunt.
Lymphatic Drainage of the Colon
The lymph nodes of the large intestine have been divided into four groups: epicolic, under the serosa of the wall of the intestine; paracolic, on the marginal artery; intermediate, along the large arteries (superior and inferior mesenteric arteries); and principal, at the root of the superior and inferior mesenteric arteries (Fig. 12.17). This last group includes mesenteric root nodes (which also receive lymph from the small intestine), aortic nodes, and left lumbar nodes.
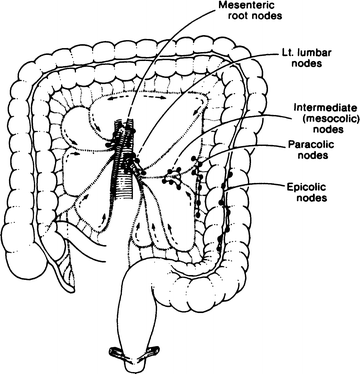

Figure 12.17.
The lymphatics of the colon follow the arteries and drain to the principal nodes at the root of the mesentery. The path is by way of the epiploic, paracolic, and mesocolic lymph nodes (By permission of JE Skandalakis, SW Gray, and JR Rowe. Anatomical Complications in General Surgery. New York: McGraw-Hill, 1983).
Wide resection of the colon should include the entire segment supplied by a major artery. This also will remove most, but not all, of the lymphatic drainage of the segment (Fig. 12.18).
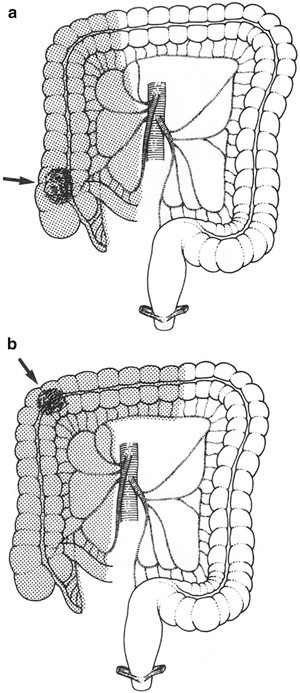
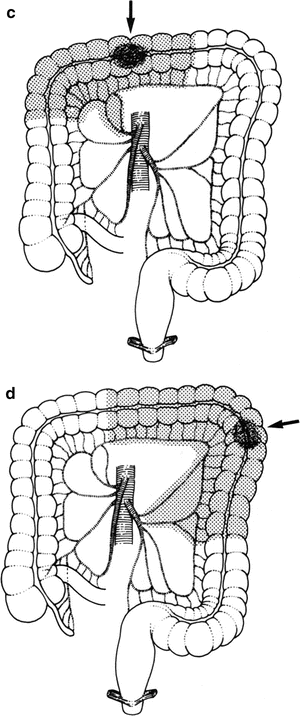
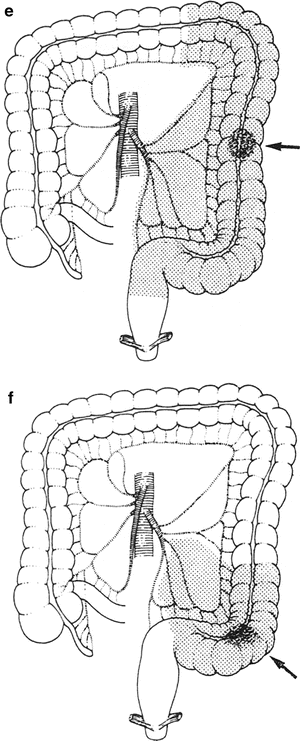



Figure 12.18.
Resection of the colon should include the entire area served by a major artery as well as the lesion itself. Most of the lymphatic drainage will be included. Areas of resection (shaded) for lesions in various segments of the colon are shown in (a–f). An arrow indicates the site of the lesion (By permission of JE Skandalakis, SW Gray, and JR Rowe. Anatomical Complications in General Surgery. New York: McGraw-Hill, 1983).
Lymphatic Drainage of the Rectum and Anal Canal
The lymph channels of the rectum and anal canal form two extramural plexuses, one above and one below the pectinate line. The upper plexus drains through the posterior rectal nodes to a chain of nodes along the superior rectal artery to the pelvic nodes (Fig. 12.19). Some drainage follows the middle and inferior rectal arteries to the hypogastric nodes. Below the pectinate line, the plexus drains to the inguinal nodes.
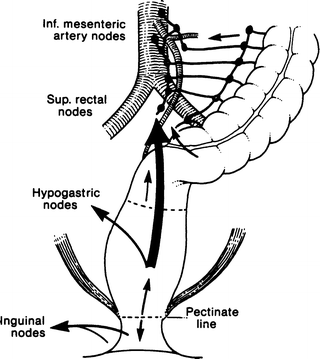

Figure 12.19.
Lymphatic drainage of the sigmoid colon, rectum, and anus. Above the pectinate line, drainage is to the inferior mesenteric nodes. Below the line, drainage is to the inguinal nodes (By permission of JE Skandalakis, SW Gray, and JR Rowe. Anatomical Complications in General Surgery. New York: McGraw-Hill, 1983).
The “watershed” of the extramural lymphatic vessels is at the pectinate line. The watershed for the intramural lymphatics is higher, at the level of the middle rectal valve (Fig. 12.20). These two landmarks may be kept in mind by the mnemonic “two, four, eight,” meaning:
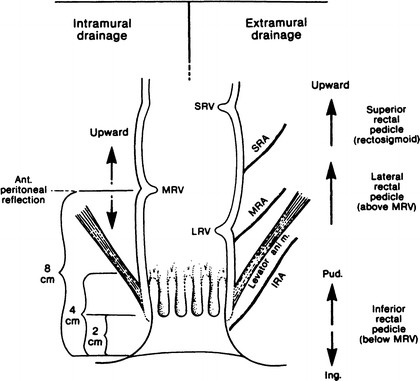

Figure 12.20.
Diagram of lymph drainage of the anus and rectum. The watershed for extramural drainage is at the pectinate line (Figure 12.19). The watershed for intramural drainage is at the level of the middle rectal valve, about 8 cm above the anal verge. IRA inferior rectal artery, MRA middle rectal artery, SRA superior rectal artery, LRV lower rectal valve, MRV middle rectal valve, SRV superior rectal valve (By permission of JE Skandalakis, SW Gray, and JR Rowe. Anatomical Complications in General Surgery. New York: McGraw-Hill, 1983).
2 cm = anal verge to pectinate line
4 cm = surgical anal canal (above and below the pectinate line)
8 cm = anal verge to middle rectal valve
Downward spread of lesions of the rectum is rare; perhaps only 2 % may spread downward. A margin of 2–3 cm distal to the tumor should be allowed in anterior resection.
Nerve Supply of the Rectum and Anus
Motor innervation of the internal rectal sphincter is supplied by sympathetic fibers that cause contraction and by parasympathetic fibers that inhibit contraction. The parasympathetic fibers are carried by pelvic splanchnic nerves which also convey the afferent nerve fibers that mediate the sensation of rectal distention. The external rectal sphincter is innervated by the inferior rectal branch of the internal pudendal nerve and by the perineal branch of the fourth sacral nerve.
The pelvic splanchnic nerves (parasympathetic and sensory) and the hypogastric nerve (sympathetic) supply the lower rectal wall. These two sources together form the rectal plexus. The levator ani muscles are supplied by the nerve to the levator ani, usually a branch from S4, with variant contributions from S3 and S5.
The inferior rectal branches of the internal pudendal nerve follow the inferior rectal arteries and supply the sensory innervation of the perianal skin.
Remember:
✔ The pudendal nerve innervates the external sphincter and possibly the puborectalis muscle. The sympathetic nerves have no influence on the muscular wall of the rectum. Evacuation is accomplished by the pelvic splanchnic nerves; continence is maintained by the pudendal and the pelvic splanchnic nerves.
Technique
Decalogue of Good Colon Surgery
1.
Bowel preparation of choice.
2.
Administer intravenous antibiotics within 1 h of making your incision during the surgery and for 24 h afterward.
3.
Use orogastric/nasogastric tube and Foley catheter when appropriate.
4.
Understand anatomy of blood supply and lymphatics. When performing cancer surgery, ligate vessels at their origins.
5.
Good technique for performing anastomosis includes:
a.
Observing whether the cut edges of the intestinal segments to be anastomosed have good texture and color and are bleeding slightly. Avoid formation of hematomata at the anastomotic area.
b.
Clearing all fatty tissue from the anastomotic area by removing, without traction, the mesenteric border and the epiploic appendages.
6.
Avoid tension on the anastomosis.
7.
Use headlight.
8.
Be familiar with all surgical procedures and their modifications.
9.
Identify the ureters to avoid injury.
10.
Reapproximate the mesentery to avoid internal hernias.
Cecopexy
Occasionally, the cecum and ascending colon are very mobile (Fig. 12.21). To avoid volvulus of the right colon and, therefore, intestinal obstruction, a cecopexy extending up to the ascending colon is performed. Suture the cecal and ascending tenia to the lateral peritoneum with interrupted 3-0 synthetic absorbable material or silk, and perform an appendectomy (Fig. 12.22).
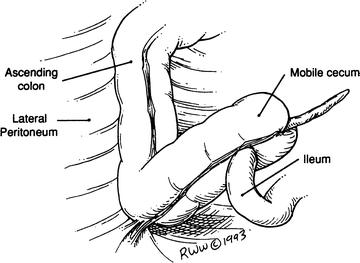
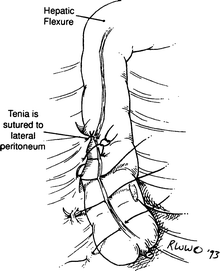

Figure 12.21.
Mobile cecum.

Figure 12.22.
Teniae have been sutured.
Colostomy
Loop Colostomy
A loop colostomy (Fig. 12.23) is feasible only in the transverse or sigmoid colon because a mesentery is required. If the transverse mesocolon is short, mobilization of the hepatic and splenic flexures will provide a more mobile loop.
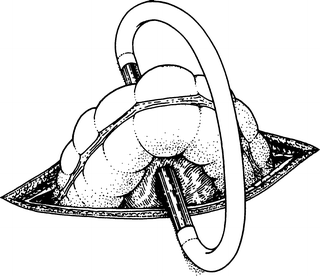

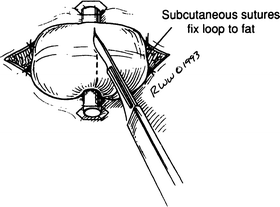
Figure 12.23.
Loop colostomy. The loop of colon has been brought through the incision, held in place by a glass tube with rubber tubing connecting its ends (By permission of JE Skandalakis, SW Gray, and JR Rowe. Anatomical Complications in General Surgery. New York: McGraw-Hill, 1983).
Sigmoid loop colostomy is, for practical purposes, left colon colostomy. The stoma should be located at the junction of the descending and the sigmoid colon so that the peritoneal fixation of the descending colon will protect the proximal stoma from prolapse.
Loop Transverse Colostomy
Step 1. Make a 4- to 6-cm transverse incision at the right, or occasionally left, lateral border of the rectus abdominis muscle (Fig. 12.24).
Figure 12.24.
Transverse incision.
Step 2. Divide the anterior rectus sheath, rectus abdominis muscle, and posterior sheath.
Step 3. Deliver the transverse colon into the wound outside the peritoneal cavity and form a small hole at the omentum and the mesenteric border of the colon to permit the entrance of a plastic rod (Fig. 12.25).
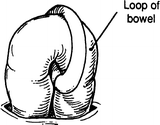
Figure 12.25.
Colon loop.
Step 4. Open the colon as shown and mature to the skin with 4-0 Vicryl sutures (Fig. 12.26). However, maturation of the colostomy in the operating room depends on the philosophy of the surgeon (Fig. 12.27).