http://evolve.elsevier.com/McCuistion/pharmacology/
Various drugs are used to maintain or decrease blood lipid concentrations and promote dilation of vessels. Drugs that lower blood lipids are called antihyperlipidemics, antilipidemics, antilipemics, and hypolipidemics. In this chapter, drugs used to lower lipoproteins are called antihyperlipidemics. Drugs that improve blood flow are called peripheral vasodilators as they dilate vessels that have been narrowed by vasospasm and blood viscosity reducer agents, which decrease viscosity of blood and increase erythrocyte flexibility.
Lipoproteins
Lipids—cholesterol, triglycerides, and phospholipids—are bound in the inner shell of protein, a carrier that transports lipids in the bloodstream. When there is an excess of one or more lipids in the blood, the condition is known as hyperlipidemia or hyperlipoproteinemia. The four major categories of lipoprotein are high-density lipoprotein (HDL), low-density lipoprotein (LDL), very-low-density lipoprotein (VLDL), and chylomicrons. HDL, also known as “friendly” or “good” lipoprotein, is the smallest and densest lipoprotein, meaning that it contains more protein and less fat than the others. The function of HDL is to remove cholesterol from the bloodstream and deliver it to the liver for excretion in bile. LDL, the “bad” lipoprotein, contains 50% to 60% of cholesterol in the bloodstream. With an elevated LDL, the risk is greater for developing atherosclerotic plaques and heart disease. VLDL carries mostly triglycerides and less cholesterol. The chylomicrons are large particles that transport fatty acids and cholesterol to the liver. They are composed mostly of triglycerides.
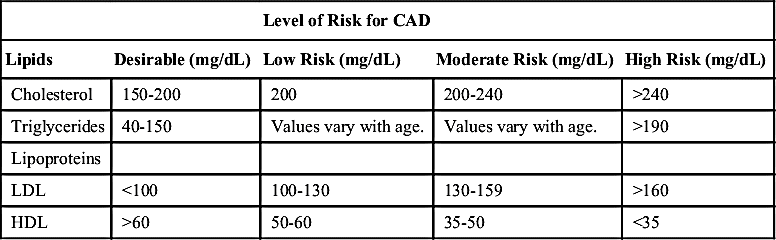
Serum cholesterol and triglyceride measurements are frequently part of a regular physical examination or readmission evaluation and are used as baseline test results. If the levels are high, a 12- to 14-hour fasting lipid profile may be ordered. When cholesterol, triglycerides, and LDL are elevated, the patient is at increased risk for coronary artery disease (CAD). Table 41.1 lists the various serum lipids and their reference values (normal serum levels) according to risk classification.
Apolipoproteins
Apolipoproteins are within the lipoprotein shell and contain apolipoprotein (apo) A-1, B, and E. The major component of apoA-1 is HDL. The major component of apoB is LDL, which exists in two forms, apoB-100 and apoB-48. ApoB-100 has VLDL as well as LDL and is a better indicator of risk for CAD than LDL alone.
Nonpharmacologic Methods of Cholesterol Reduction
Before drugs to lower LDL and raise HDL are prescribed, nondrug therapy should be initiated to decrease cholesterol. Saturated fats and cholesterol in the diet should be reduced. Total fat intake should be 30% or less of caloric intake, and cholesterol intake should be 300 mg/day or less. The patient should be advised to read labels on containers and buy appropriate foods. Patients should choose lean meats, especially chicken and fish.
In many cases, diet alone will not lower blood lipid levels. Because 75% to 85% of serum cholesterol is endogenously (internally) derived, dietary modification alone will typically lower total cholesterol levels by only 10% to 30%. This and the fact that adherence to dietary restrictions is often short-lived explains why many patients do not respond to diet modification alone.
Exercise is an important aspect of the nonpharmacologic method to reduce cholesterol and increase HDL. For the older adult, exercise can be walking and bicycling. Smoking is another risk factor that should be eliminated. Smoking increases LDL cholesterol and decreases HDL.
If nonpharmacologic methods are ineffective for reducing LDL and VLDL cholesterol, and hyperlipidemia remains, antihyperlipidemic drugs are prescribed to lower blood lipid levels. It must be emphasized to the patient that dietary changes need to be made, and an exercise program followed, even after drug therapy is initiated. The type of antihyperlipidemics ordered depends on the lipoprotein phenotype (Table 41.2).
Antihyperlipidemics
Drugs that lower lipid levels include bile-acid sequestrants, fibrates (fibric acid), nicotinic acid, cholesterol absorption inhibitors, and hepatic 3-hydroxy-3-methylglutaryl-coenzyme A (HMG-CoA) reductase inhibitors, better known as statins. The statin drugs have fewer adverse effects and are well tolerated.
One of the first antihyperlipidemics, cholestyramine is a bile-acid sequestrant that reduces LDL cholesterol (LDL-C) levels by binding with bile acids in the intestine. It is effective against hyperlipidemia type II. This group may be used as an adjunct to the statins. The drug comes in a gritty powder that is mixed thoroughly in water or juice. Colestipol is another resin antihyperlipidemic similar to cholestyramine. Both are effective in lowering cholesterol. Colesevelam, another bile acid sequestrant similar to cholestyramine and colestipol, is an agent that has fewer side effects (less constipation, flatulence, and cramping). Colesevelam also has less effect on the absorption of fat-soluble vitamins than the older agents and is usually the first-choice bile-acid sequestrant drug.
Gemfibrozil is a fibric acid derivative that is more effective for reducing triglyceride and VLDL levels than for reducing LDL. It is used primarily to reduce hyperlipidemia type IV, but it can also be used for type II hyperlipidemia. This drug is highly protein bound and should not be taken with anticoagulants because they compete for protein sites. The anticoagulant dose should be reduced during antihyperlipidemic therapy, and the international normalized ratio (INR) should be closely monitored. Fenofibrate has similar actions and some of the same side effects as gemfibrozil. If taken with warfarin, bleeding might occur. Both fenofibrate and gemfibrozil are highly protein bound.
Niacin (vitamin B3) reduces VLDL and LDL. Niacin is actually very effective at lowering cholesterol levels, and its effect on the lipid profile is highly desirable. Because it has numerous side effects and large doses are required, as few as 20% of patients can initially tolerate niacin. However, with proper counseling, careful drug titration, and concomitant use of aspirin, this number can be increased to as much as 60% to 70%.
Ezetimibe is a cholesterol absorption inhibitor that acts on the cells in the small intestine to inhibit cholesterol absorption. It decreases cholesterol from dietary absorption, reducing serum cholesterol, LDL, triglycerides, and apoB levels. Ezetimibe causes only a small increase in HDL. It must be combined with a statin (e.g., simvastatin) for optimum effect.
Statins
The statin drugs inhibit the enzyme HMG-CoA reductase in cholesterol biosynthesis, thus statins are called HMG-CoA reductase inhibitors. By inhibiting cholesterol synthesis in the liver, this group of antihyperlipidemics decreases the concentration of cholesterol, decreases LDL, and slightly increases HDL cholesterol. Reduction of LDL cholesterol may be seen as early as 2 weeks after initiating therapy. The statin group has been useful in decreasing CAD and reducing mortality rates.
TABLE 41.2
Hyperlipidemia: Lipoprotein Phenotype
| Type∗ | Major Lipids |
| I | Increased chylomicrons and increased triglycerides; uncommon |
| IIA | Increased low-density lipoprotein (LDL) and increased cholesterol; common |
| IIB | Increased very low-density lipoprotein (VLDL), increased LDL, increased cholesterol and triglycerides; very common |
| III | Moderately increased cholesterol and triglycerides; uncommon |
| IV | Increased VLDL and markedly increased triglycerides; very common |
| V | Increased chylomicrons, VLDL, and triglycerides; uncommon |
Numerous statins have been approved since statins were first introduced. The present group of statins includes atorvastatin calcium, fluvastatin, lovastatin, pravastatin sodium, simvastatin, and rosuvastatin. Lovastatin was the first statin used to decrease cholesterol. It is effective for lowering LDL (hyperlipidemia type II) within several weeks. Gastrointestinal (GI) disturbances, headaches, muscle cramps, and fatigue are early complaints. With all statins, serum liver enzymes should be monitored, and an annual eye examination is needed because cataract formation may result. The patient should report immediately any muscle aches or weakness, which can lead to rhabdomyolysis, a muscle disintegration that can become fatal.
The statins have actions in decreasing serum cholesterol, LDL, VLDL, and triglycerides, and they slightly elevate HDL. Atorvastatin, lovastatin, rosuvastatin, and simvastatin are more effective at lowering LDL than the other statins. Rosuvastatin and atorvastatin are at the top of the list of most prescribed drugs in the United States.
The statin drugs can be combined with other drugs to decrease blood pressure and blood clotting and to enhance the antihyperlipidemic effect. Examples are atorvastatin and amlodipine, simvastatin and ezetimibe, and atorvastatin and ezetimibe. Table 41.3 lists these combination drugs and their dosages, uses, and considerations.
If antihyperlipidemic therapy is withdrawn, cholesterol and LDL levels return to pretreatment levels. The patient taking an antihyperlipidemic drug should understand that antihyperlipidemic therapy is a lifetime commitment for maintaining a decrease in serum lipid levels. Abruptly stopping the statin drug could cause a threefold rebound effect that may cause death from acute myocardial infarction (AMI).
Laboratory Tests
Reference values for homocysteine, an amino acid, are 4 to 17 mmol/L (fasting). Homocysteine is a by-product of protein and is found in eggs, chicken, beef, and cheddar cheese. A high level of homocysteine has been linked to cardiovascular disease, stroke, and Alzheimer disease. It may also promote blood clotting, and it has been stated that an increase in serum homocysteine can damage the inner lining of blood vessels and promote a thickening and loss of flexibility in the vessel. Three vitamins that can lower serum homocysteine levels are vitamin B6 (pyridoxine), vitamin B12 (cyanocobalamin), and folic acid.
High-sensitivity C-reactive protein (hsCRP) reference values are less than 0.175 mg/L; low risk is less than 1 mg/L, moderate risk is 1 to 3 mg/L, and high risk is less than 3 mg/L. The standard C-reactive protein (CRP) is produced in the liver in response to tissue injury and inflammation. The hsCRP is a highly sensitive test for detecting the inflammatory protein that can be associated with cardiovascular and peripheral vascular disease. This test is frequently ordered along with cholesterol screening. Approximately one third of persons who have had a heart attack have normal cholesterol levels and normal blood pressure. A positive hsCRP test can indicate that the patient is at high risk for CAD, making it a valuable test for predicting CAD. This test can detect an inflammatory process caused by the buildup of atherosclerotic plaque in the arterial system, particularly the coronary arteries.
Prototype Drug Chart 41.1 lists the pharmacologic data for a frequently prescribed antihyperlipidemic, rosuvastatin.
Pharmacokinetics
Rosuvastatin decreases LDL by 46% at a dose of 10 mg. It is highly protein bound, so it usually is prescribed as a once-daily dose. Rosuvastatin has a half-life of 20 hours.
Pharmacodynamics
The positive effect of lowering lipids with rosuvastatin is seen in about 2 weeks. The peak time after a dose of rosuvastatin is 3 to 5 hours; however, it takes 2 to 4 weeks to achieve therapeutic effect. When the patient is taking high doses of rosuvastatin or any other statin, myopathy and rhabdomyolysis—disintegration of striated muscle fibers—may occur. If the patient complains of muscle pain or tenderness, it should be reported immediately.
Side Effects and Adverse Reactions
Side effects and adverse reactions of cholestyramine include constipation and peptic ulcer. Constipation can be decreased or alleviated by increasing intake of fluids and foods high in fiber. Early signs of peptic ulcer are nausea and abdominal discomfort, followed later by abdominal pain and distension. To avoid GI discomfort, the drug must be taken with and followed by sufficient fluids.
The many side effects of niacin—which include GI disturbances, flushing of the skin, abnormal liver function (elevated serum liver enzymes), hyperglycemia, and hyperuricemia—decrease its usefulness. However, as mentioned, aspirin and careful drug titration can reduce side effects to a manageable level in most patients.
The statin drugs can cause a dose-related increase in liver enzyme levels. Serum liver enzyme levels (alkaline phosphatase [ALP], alanine aminotransferase [ALT], gamma-glutamyl transferase [GGT]) should be monitored. Baseline liver enzyme studies should be obtained before initiating statin therapy. A slight transient increase in serum liver enzyme levels may be within normal range for the patient, but it should be rechecked in 1 week or so. Patients with acute hepatic disorders should not take a statin drug.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree