http://evolve.elsevier.com/McCuistion/pharmacology/
Antidepressants are used for depressive episodes accompanied by feelings of hopelessness and helplessness. They can be prescribed for 1 month to 12 months or perhaps longer.
Mood-stabilizer agents such as lithium are effective for bipolar disorder. Drug therapy for treating bipolar disorder is discussed in this chapter.
Depression
Depression is the most common mental illness, affecting approximately 14.8 million Americans. Fewer than 50% of individuals with depression seek treatment despite the fact that about 70% of individuals with depression have a full remission with effective treatment. Women between the ages of 25 and 45 years are two to three times more likely than men to experience major depression. Depression is characterized primarily by mood changes and loss of interest in normal activities and is second only to hypertension as the most common chronic clinical condition.
Contributing causes of depression include genetic predisposition, social and environmental factors, and biologic conditions. Some signs of major depression include loss of interest in most activities, depressed mood, weight loss or gain, insomnia or hypersomnia, loss of energy, fatigue, feelings of despair, decreased ability to think or concentrate, and suicidal thoughts. Approximately 66% of all suicides are related to depression. Depressed men, especially older Causcasian men, are more likely to commit suicide successfully than are depressed women. Antidepressants can mask suicidal ideation.
The three types of depression are (1) reactive, (2) major, and (3) bipolar disorder, previously referred to as manic depression. Reactive depression usually has a sudden onset after a precipitating event (e.g., depression resulting from a loss, such as death of a loved one). The patient knows why he or she is depressed and may call this “the blues.” Usually, this type of depression lasts for months, and a benzodiazepine agent may be prescribed. Major depression is characterized by loss of interest in work and home, inability to concentrate and complete tasks, difficulty sleeping or excessive sleeping, feelings of fatigue and worthlessness, and deep depression, also known as dysphoria. Major depression can be either primary, unrelated to other health problems, or secondary to a health problem such as a physical or psychiatric disorder or drug use. Antidepressants have been effective in treating major depression. Bipolar disorder involves swings between two moods, the manic (euphoric) and the depressive (dysphoric); lithium was originally the drug of choice for treating this type of disorder. Other mood stabilizers such as carbamazepine; valproic acid, or divalproex; and lamotrigine are also currently first-line drugs of choice for bipolar disorder.
Pathophysiology
Many theories exist as to the cause of major depression. A common one suggests an insufficient amount of brain monoamine neurotransmitters (norepinephrine, serotonin, perhaps dopamine). It is thought that decreased levels of serotonin permit depression to occur, and decreased levels of norepinephrine cause depression. However, there can be other physiologic causes of depression, and social and environmental factors play a role.
Complementary and Alternative Therapy for Depression
St. John’s wort and Gingko biloba have been suggested for the management of mild depression, but these should not be taken along with prescription antidepression medications. St. John’s wort can decrease reuptake of the neurotransmitters serotonin, norepinephrine, and dopamine. The use of these and many complementary and alternative products should be discontinued 1 to 2 weeks before surgery. The patient should check with a health care provider regarding complementary and alternative therapies (Complementary and Alternative Therapies 23.1).
Antidepressant Agents
Antidepressants are divided into five groups: (1) tricyclic antidepressants (TCAs), or tricyclics; (2) selective serotonin reuptake inhibitors (SSRIs); (3) serotonin norepinephrine reuptake inhibitors (SNRIs); (4) atypical antidepressants that affect various neurotransmitters; and (5) monoamine oxidase inhibitors (MAOIs). TCAs and MAOIs were marketed in the late 1950s, and many of the SSRIs and atypical antidepressants were available in the 1980s. The SSRIs and SNRIs are popular antidepressants because they do not cause sedation, hypotension, anticholinergic effects, or cardiotoxicity as do many of the TCAs. However, users of SSRIs can experience sexual dysfunction, but this can be managed. With unpleasant side effects or lack of improvement, the patient is usually changed to another category of drug.
Tricyclic Antidepressants
Tricyclic antidepressants (TCAs) are used to treat major depression because they are effective and are less expensive than SSRIs and other drugs. Imipramine was the first TCA marketed in the 1950s.
The action of TCAs is to block the uptake of the neurotransmitters norepinephrine and serotonin in the brain. The clinical response of TCAs occurs after 2 to 4 weeks of drug therapy. If there is no improvement after 2 to 4 weeks, the antidepressant is slowly withdrawn and another antidepressant is prescribed. Polydrug therapy, the practice of giving several antidepressants or antipsychotics together, should be avoided if possible because of potential serious side effects.
The effectiveness of TCAs in treating major depression is well documented. This group of drugs elevates mood, increases interest in daily living and activity, and decreases insomnia. For agitated depressed persons, amitriptyline, doxepin, or trimipramine may be prescribed because of their highly sedative effect. TCAs are often given at night to minimize problems caused by their sedative action. When discontinuing TCAs, the drugs should be gradually decreased to avoid withdrawal symptoms such as nausea, vomiting, anxiety, and akathisia. Imipramine hydrochloride is used for the treatment of enuresis (involuntary discharge of urine during sleep in children).
The TCA drugs include amitriptyline, imipramine, trimipramine, doxepin, desipramine, nortriptyline, and protriptyline. The TCA drugs desipramine and nortriptyline are major metabolites of imipramine and amitriptyline.
Pharmacokinetics
Amitriptyline is strongly protein bound. The half-life is 10 to 50 hours, and a cumulative drug effect may result. Amitriptyline is primarily excreted in urine.
Pharmacodynamics
Amitriptyline is well absorbed, but antidepressant effects develop slowly over several weeks. The onset of the antidepressant effect of amitriptyline is 1 to 3 weeks, and the peak concentration is 2 to 5 hours. Drug doses are decreased for older patients to reduce side effects.
Side Effects and Adverse Reactions
The TCAs have many side effects: orthostatic hypotension, sedation, anticholinergic effects, cardiotoxicity, and seizures. Rising from a sitting position too rapidly can cause dizziness and lightheadedness (orthostatic hypotension), so the patient should be instructed to rise slowly to an upright position. The TCAs block the histamine receptors, thus sedation is likely to occur initially but decreases with continuous use of the drug. Because TCAs block the cholinergic receptors, they can cause anticholinergic effects such as tachycardia, urinary retention, constipation, dry mouth, and blurred vision. Other side effects of TCAs include allergic reactions (skin rash, pruritus, and petechiae) and sexual dysfunction (erectile dysfunction and amenorrhea). Most TCAs can cause blood dyscrasias (leukopenia, thrombocytopenia, and agranulocytosis) that require close monitoring of blood cell counts. Amitriptyline may lead to symptoms of extrapyramidal syndrome (EPS). Clomipramine can cause neuroleptic malignant syndrome (NMS). Because the seizure threshold is decreased by TCAs, patients with seizure disorders may need TCA dose adjustment. The most serious adverse reaction to TCAs is cardiotoxicity, such as dysrhythmias that may result from high doses of the drug. The therapeutic serum range of TCAs should be monitored.
Drug Interactions
Alcohol, hypnotics, sedatives, and barbiturates potentiate central nervous system (CNS) depression when taken with TCAs. Concurrent use of MAOIs with amitriptyline may lead to cardiovascular instability and toxic psychosis. Antithyroid medications taken with amitriptyline may increase the risk of dysrhythmias.
Selective Serotonin Reuptake Inhibitors
Selective serotonin reuptake inhibitors (SSRIs) block the reuptake of serotonin into the nerve terminal of the CNS, thereby enhancing its transmission at the serotonergic synapse. These drugs do not block the uptake of dopamine or norepinephrine, and they do not block cholinergic and alpha1-adrenergic receptors. SSRIs are more commonly used to treat depression than are TCAs, and they have fewer side effects than TCAs.
The primary use of SSRIs is for major depressive disorders. They are also effective for treating anxiety disorders such as obsessive-compulsive disorder (OCD), panic disorders, phobias, posttraumatic stress disorder (PTSD), and other forms of anxiety. Fluvoxamine is useful for treating OCD in children and adults. SSRIs have also been used to treat eating disorders and selected drug abuses. Miscellaneous uses for SSRIs include decreasing premenstrual tension syndrome, preventing migraine headaches, and preventing or minimizing aggressive behavior in patients with borderline personality disorder.
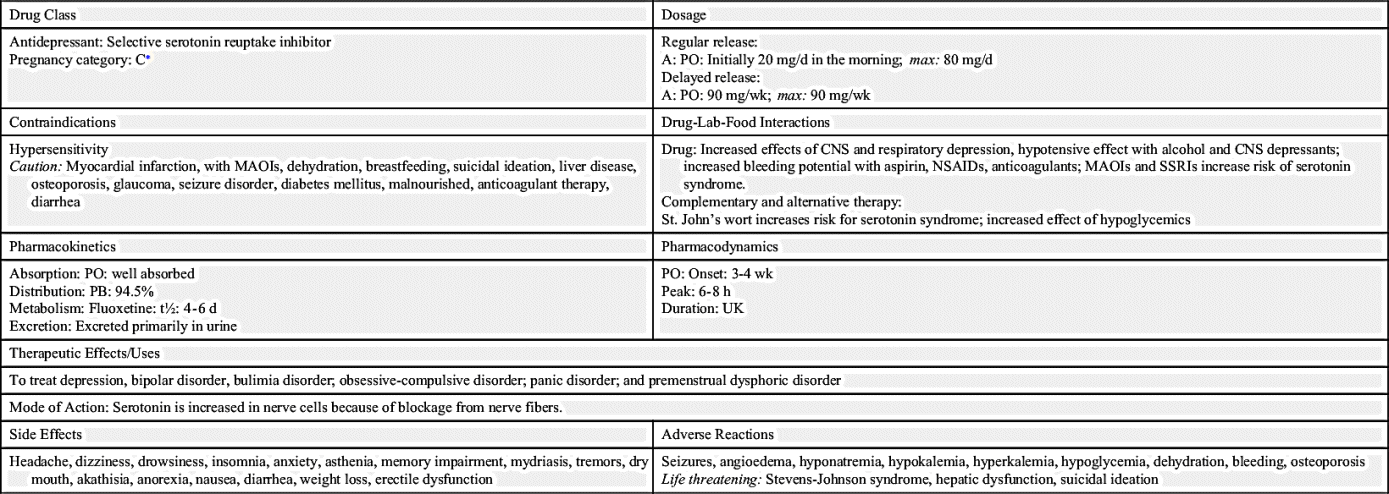
The SSRIs include fluoxetine, fluvoxamine, sertraline, paroxetine, citalopram, and escitalopram. Fluoxetine has been effective in 50% to 60% of patients who fail to respond to TCA therapy (TCA-refractory depression). The U.S. Food and Drug Administration (FDA) approved a weekly delayed-release fluoxetine dose of 90 mg. However, before taking the weekly dose, the patient should respond to a daily maintenance dose of 20 mg/day without serious effects.
Many SSRIs have an interaction with grapefruit juice that can lead to possible toxicity. It is recommended that daily intake be limited to 8 ounces of grapefruit juice or one half of a grapefruit.
Prototype Drug Chart 23.1 describes the drug characteristics of the SSRI fluoxetine.
Pharmacokinetics
Fluoxetine is strongly protein bound, and the half-life is 4 to 6 days; therefore a cumulative drug effect may result from long-term use. Fluoxetine is metabolized and excreted by the kidneys.
Pharmacodynamics
Fluoxetine is well absorbed; however, its antidepressant effect develops slowly over several weeks. The onset of fluoxetine’s antidepressant effect is between 1 and 12 weeks, and peak concentration with consistent therapy is at 6 to 8 hours after ingestion. The drug dose for older adults should be decreased to reduce side effects.
Side Effects and Adverse Reactions
Fluoxetine produces common side effects such as dry mouth, blurred vision, insomnia, headache, nervousness, anorexia, nausea, diarrhea, and suicidal ideation. Fluoxetine has fewer side effects than amitriptyline.
Some patients may experience sexual dysfunction when taking SSRIs. Men have discontinued taking fluoxetine after experiencing a decrease in sexual arousal. Some women have become anorgasmic while males reported erectile dysfunction and delayed ejaculation when taking paroxetine HCl. The side effects often decrease or cease over the 1- to 4-week period of waiting for the therapeutic effect to emerge.
Serotonin Norepinephrine Reuptake Inhibitors
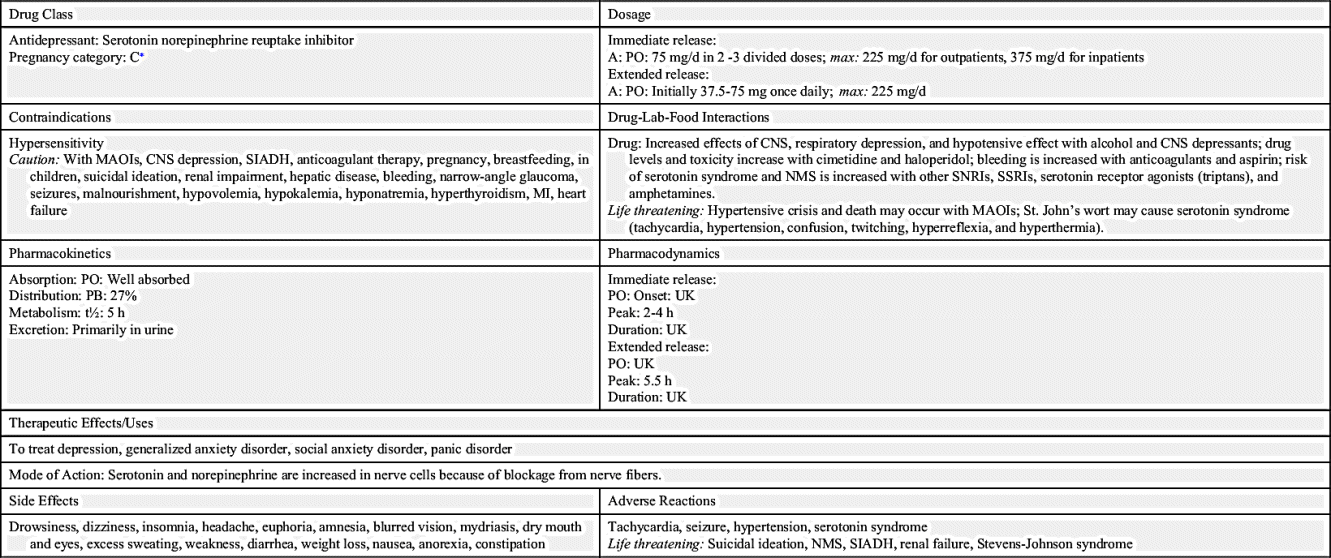
Venlafaxine was the first of the serotonin norepinephrine reuptake inhibitors (SNRIs) approved for major depression in 1993. SNRIs inhibit the reuptake of serotonin and norepinephrine, increasing availability in the synapse. SNRIs are used for major depression. Other approved uses are for generalized anxiety disorder and social anxiety disorder. Other SNRIs include duloxetine and desvenlafaxine. The concurrent interaction of venlafaxine and St. John’s wort may increase the risk of serotonin syndrome and NMS. Prototype Drug Chart 23.2 describes the drug characteristics of venlafaxine.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree