http://evolve.elsevier.com/McCuistion/pharmacology/
Cancer-related deaths rank second only to heart disease in the United States. Even though cancer-related mortality has decreased since the early 1990s, approximately 1 in 3 women and 1 in 2 men are projected to develop cancer over their lifetime. Excluding basal and squamous cell skin cancers, the highest incidence rates in men are prostate, lung, and colorectal cancer. In women, breast, lung, and colorectal cancers occur with the highest frequency. Lung cancer remains the leading cause of cancer-related death regardless of gender.
The incidences and mortality rates of cancer differ by ethnicity. Non-Hispanic blacks (henceforth “African Americans”) have higher incidences (except breast cancer) and higher death rates from cancer (except breast and lung) than any racial or ethnic group. African American women have lower incidences of breast cancer but higher mortality rates than Caucasian women do. Hispanics have the lowest incidences and mortality rates of lung cancer. Incidences and mortality rates for liver and stomach cancers due to hepatitis B virus (HBV) and Helicobacter pylori (H. pylori) are the highest among Asians and Pacific Islanders. Incidences of cancer increase among all immigrants as they adopt a more westernized lifestyle.
Cancer is a group of diseases in which abnormal cells grow out of control and can spread to other areas of the body. DNA is the genetic substance in the body cells that transfers information necessary for the production of enzymes and protein synthesis. In most cases, cancer is caused by damage to the DNA within the cell. Although some cancers are inherited, most develop when genes in a normal cell become damaged or lost. More than one mutation is required before a malignancy can develop, therefore the development of cancer is a multistep process that may take years to complete.
Pharmaceuticals are often used to destroy cancer cells and are called by different names, including anticancer drugs, cancer chemotherapeutic agents, antineoplastic drugs, or cytotoxic therapy. In the 1970s, combination chemotherapy—the use of two or more chemotherapy agents to treat cancer—was adopted and led to improved response rates and increased survival times. Chemotherapy may be used as the only treatment of cancer, or it may be used in conjunction with other modalities such as radiation, surgery, and biologic response modifiers. Combination chemotherapy increases the chance for months to years of cancer remission. If cancer can no longer be controlled, palliative treatment with chemotherapy may be used to relieve disease-related symptoms and improve quality of life.
Genetic, Inflammatory, Infective, Environmental, and Dietary Influences
Cancer can be influenced by genetic mutations, inflammation, infectious organisms, environment, and an unhealthy diet. Box 32.1 gives examples of environmental substances, viruses, and foods that have a carcinogenic effect in humans. Genes provide the instructions for the production and function of cellular proteins essential for normal cellular activities. Genetic defects may occur in a variety of ways, including deletion, translocation, duplication, inversion, or insertion of genetic material. When defects cannot be effectively repaired, cells exhibit abnormal characteristics and unregulated growth. More than 2000 genes have been causally implicated in the formation of cancer. Cancers with a proven genetic influence include breast, ovarian, prostate, endometrial, colon, pancreatic, and lung cancers; retinoblastoma; and malignant melanoma, to name a few. Many more genetic influences are expected to be found as cancer research continues.
Genes can cause cells to become cancerous in several ways. Proto-oncogenes are normal genes involved in cell differentiation and division, and they regulate cell death, also known as apoptosis. These processes are necessary for healthy tissues and organs. An oncogene is a mutation in a proto-oncogene that affects cellular growth-control proteins and triggers unregulated cell division. Some genes, called antioncogenes, protect others. One such gene is the tumor-suppressor (TS) genes that signal a cell to cease multiplying and stop the action of oncogenes. Uncontrollable cell growth can occur if TS genes become lost or dysfunctional. Other genes repair damage to DNA. If these DNA-repair genes are damaged, mutations are not corrected and are subsequently passed on to the next generation of daughter cells. These and other gene mutations can take place over a long time before cancer develops. As a result, cancers more commonly occur in older individuals.
Inflammation is a normal physiologic process to heal injured tissues. Chronic inflammation, such as chronic inflammatory bowel disease, is an ongoing inflammatory process. The continued inflammation can lead to DNA damage and can result in cancer.
A number of viruses are associated with the development of cancer. The human papillomavirus (HPV) has been found in most women with invasive cervical cancer. Individuals with human immunodeficiency virus (HIV) may develop lymphomas and rectal or genital cancers. The Epstein-Barr virus (EBV) is found in almost all people with Burkitt lymphoma in central Africa and has been implicated in the development of nasopharyngeal cancer. Hepatocellular carcinoma (liver cancer) is linked to hepatitis B and C viruses. Other viruses linked to cancer include human T-cell lymphotropic virus (HTLV) and Kaposi sarcoma–associated herpesvirus.
Bacteria can play a role in the development of cancer. The presence of H. pylori in the stomach is associated with an increased risk of gastric cancer. Some reports have indicated a link between certain bacteria and cancer of the gallbladder, colon, and lung. However, no clear evidence supports a link between bacterial infection and other cancers.
Environmental factors associated with the development of cancer include tobacco use, poor diet, decreased physical activity, chemicals, and excessive sun and radiation exposures. According to the Centers for Disease Control and Prevention (CDC), 90% of lung cancers in men and 80% in women occur due to smoking. Other cancer-causing environmental agents include alcohol consumption on a regular basis, which raises the risk of mouth, larynx, and throat cancers; being overweight or obese, which increases the risk of uterine, breast, prostate, and colorectal cancers; and excessive exposure to sun and other forms of ultraviolet (UV) rays, which promotes skin cancers. Many of these cancers can be prevented. According to the American Cancer Society (ACS), about 43,840 people were expected to succumb to cancer during the year 2015.
Cell Cycle–Nonspecific and Cell Cycle–Specific Anticancer Drugs
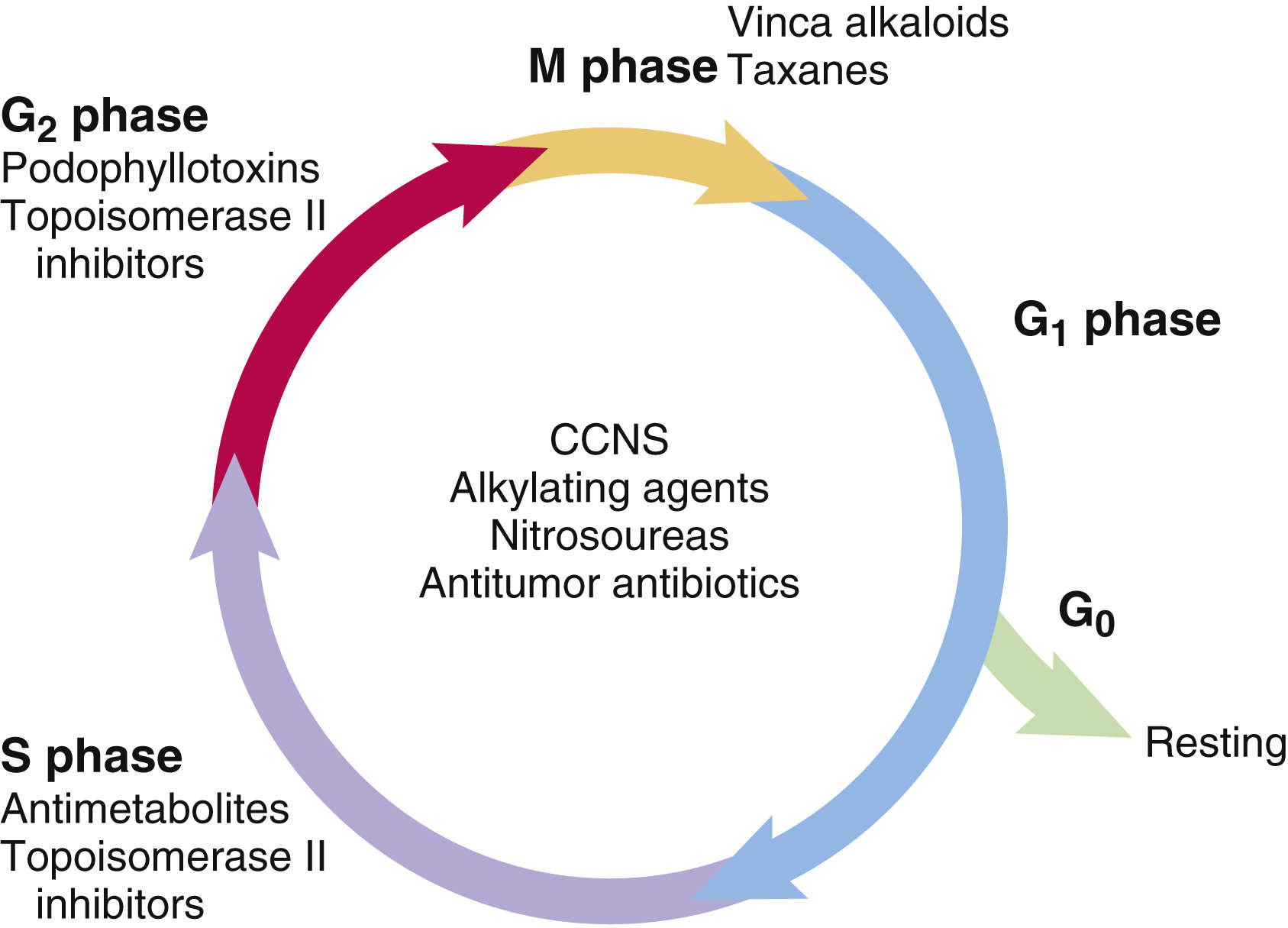
The cell cycle for normal and cancer cells and the growth fraction and doubling time are discussed in the opening pages for Unit X (see Fig. 32.1).
Anticancer drugs stop or slow the growth of cancer cells by interfering with cell replication and are classified according to their action. Cell cycle–nonspecific (CCNS) drugs act during any phase of the cell cycle, including the G0 phase. CCNS drugs include most alkylating drugs, antitumor antibiotics, and hormones. Cell cycle–specific (CCS) drugs exert their influence during a specific phase of the cell cycle and are most effective against rapidly growing cancer cells. The CCS drugs include antimetabolites, some alkylating agents, and vinca alkaloids. Fig. 32.1 shows selected categories of anticancer drugs and the phase of the cell cycle in which they are most effective.
Growth fraction and doubling time are two factors that play a major role in how the cancer cells respond to anticancer drugs. Anticancer drugs are more effective against neoplastic cells that have a high growth fraction. Leukemia and some lymphomas have high growth fractions and thus respond well to anticancer drug therapy.
Solid tumors have a large percentage of their cell mass in the G0 phase, thus they generally have a low growth fraction and are less sensitive to anticancer drugs. As the tumor grows, the blood supply decreases, thereby slowing the growth rate. High-dose chemotherapy results in better tumor-killing (tumoricidal) effects. Depending on the type of cancer, malignant cell growth is usually faster in the earlier stages of tumor development. Adequate vascularization is needed for the anticancer drugs to be effective. Anticancer drugs are more effective against small, fast-growing tumors with sufficient blood supply. The vascularization in solid tumors can be inconsistent. Some areas of tumor may have an adequate blood supply, whereas other areas are poorly perfused. This characteristic may make some large tumors resistant to anticancer drugs and therefore difficult to treat.
Cancer Chemotherapy
Anticancer drugs do not affect just cancer cells; instead, the drugs affect both cancer and normal cells. The side effects of chemotherapy are largely related to the toxic effects on normal cells. Normal cells are able to repair themselves and continue to grow, thus the side effects of chemotherapeutic agents are often temporary. Chemotherapy is usually administered systemically for cancer that has spread to other parts of the body, for cancers in multiple sites, or for cancers too large to be removed by other means (e.g., surgery). The most common route of chemotherapy administration is through intravenous (IV) infusion, although other routes may be used and include oral, intramuscular, subcutaneous, intraperitoneal, intraventricular (intrathecal), intrapleural, intravesicular, intraarterial, and topical routes.
Some types of cancer can be cured with chemotherapy (e.g., Hodgkin disease, Burkitt lymphoma, and testicular cancer). Other types of cancer (e.g., breast and colon cancer) may be treated with surgery first, followed by chemotherapy to eliminate any residual cancer cells (microscopic metastases) that may remain in the body. This is referred to as adjuvant therapy. Sometimes neoadjuvant chemotherapy may be given first to help shrink a large tumor, so that it can be surgically removed. Palliative chemotherapy, used to relieve symptoms associated with advanced disease (e.g., pain and shortness of breath), can improve quality of life.
Chemotherapy administration is guided by specific protocols based on the results of controlled research studies. The length of treatment is determined by the type and extent of the malignancy, the type of chemotherapy given, expected side effects of the drugs, and the amount of time that normal cells need to recover. Chemotherapy is usually given in cycles to improve the likelihood that cancer cells will be destroyed and that normal cells can recover. The duration, frequency, and number of chemotherapy cycles are based on the cancer type and size, the spread of the disease to other areas of the body (metastasis), and the condition of the patient. Chemotherapy treatment may consist of one drug or a combination of drugs. Combination chemotherapy may be administered in one day or may be spread out over several days. The duration of treatment is based on the protocol being followed; it can vary from minutes to days and may be repeated weekly, biweekly, or monthly. Selected anticancer drugs are listed in Box 32.2 according to classification.
Combination Chemotherapy
Single-agent drug therapy is not usually used to treat cancer because combination therapy with two or more anticancer drugs has demonstrated more effective tumoricidal activity. Combination therapy increases the likelihood of affecting cancer cells in all phases of the cell cycle.
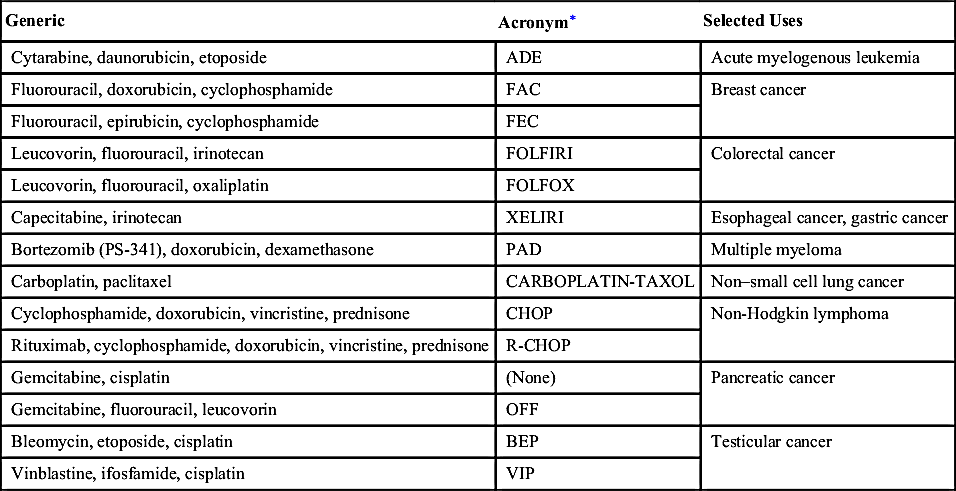
To maximize cell death, CCNS and CCS drugs are often combined to increase synergistic effects. Each individual drug used in combination therapy should have a proven tumoricidal activity, a different mode of action, and different dose-limiting toxicities. A combination of antineoplastic drugs has the advantage of decreasing drug resistance while increasing cancer cell destruction. Table 32.1 presents some of the combined anticancer drugs.
General Side Effects and Adverse Reactions
Anticancer drugs exert adverse effects on rapidly growing normal cells, such as skin and hair. These drugs can also affect cells in the gastrointestinal (GI) tract, mucous membranes, bone marrow, and reproductive system. Myelosuppression can occur when there is a significant decrease in the bone marrow activity that results in decreased white blood cells, platelets, and red blood cells. Following chemotherapy administration, the nadir—the time at which the blood count is at the lowest—typically occurs 7 to 10 days after treatment. Table 32.2 lists the general adverse effects anticancer drugs exert on the fast-growing cells of the body. Selected nursing measures and considerations are included. Because of the toxic effects of chemotherapy, care in handling of such drugs must be considered, and protective gear that includes gloves specific for handling chemotherapy drugs must be used.
Anticancer Therapy in Outpatient Settings
The administration of anticancer drugs in outpatient settings, such as in homes and oncology clinics, is both cost-effective and convenient. Although chemotherapy regimens have become increasingly aggressive, most patients are not hospitalized unless they require close monitoring or become very ill. Patients receiving highly potent drugs will need to be closely monitored for severe adverse effects. When a chemotherapy drug is given, a health care provider qualified to administer anticancer drugs follows the policies provided by the oncologist and the health care agency. To reduce the nurse’s exposure to hazardous chemotherapy drugs during administration, certain precautions should be followed to minimize occupational exposure:
• Use disposable powder-free gloves approved for handling chemotherapy, regardless of route of administration.
• Wear two pairs of gloves and change gloves every 30 minutes or when torn, punctured, or contaminated.
• Wear gowns with a front closure, long sleeves, and elastic or knit (closed) cuffs, and dispose of these after each use when administering IV chemotherapy.
• When there is a risk of aerosol exposure, follow the Occupational Safety and Health Administration (OSHA) respiratory protection standard. Surgical masks do not provide adequate respiratory protection.
• Use a face shield or a combination of a mask and face shield if there is a danger of splashing when administering chemotherapy or disposing of body fluids.
Cytotoxic drugs can be accidentally absorbed by inhalation, contact with skin or mucous membranes, or ingestion. For this reason, these guidelines should be followed:
1. Prepare chemotherapy in a separate work area. Use a plastic-backed absorbent pad to contain spills during preparation.
2. Wash hands before and after administration of chemotherapy.
3. Avoid hand-to-mouth or hand-to-eye contact while working with chemotherapy.
4. Refer to your agency’s policy for priming IV tubing and disconnecting tubing after administration.
5. Wear gloves when disposing of body fluids (e.g., urine, feces, and emesis) of patients who have received chemotherapy in the previous 48 hours.
6. Refer to agency policy for disposal of used equipment.
7. Refer to agency policy for handling chemotherapy spills or exposure.
Alkylating Drugs
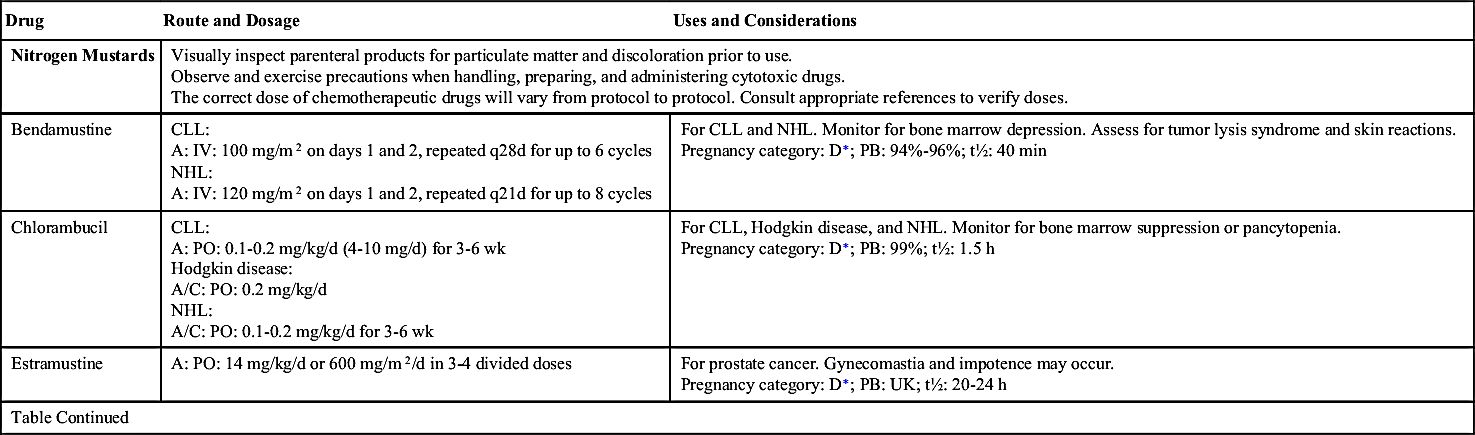
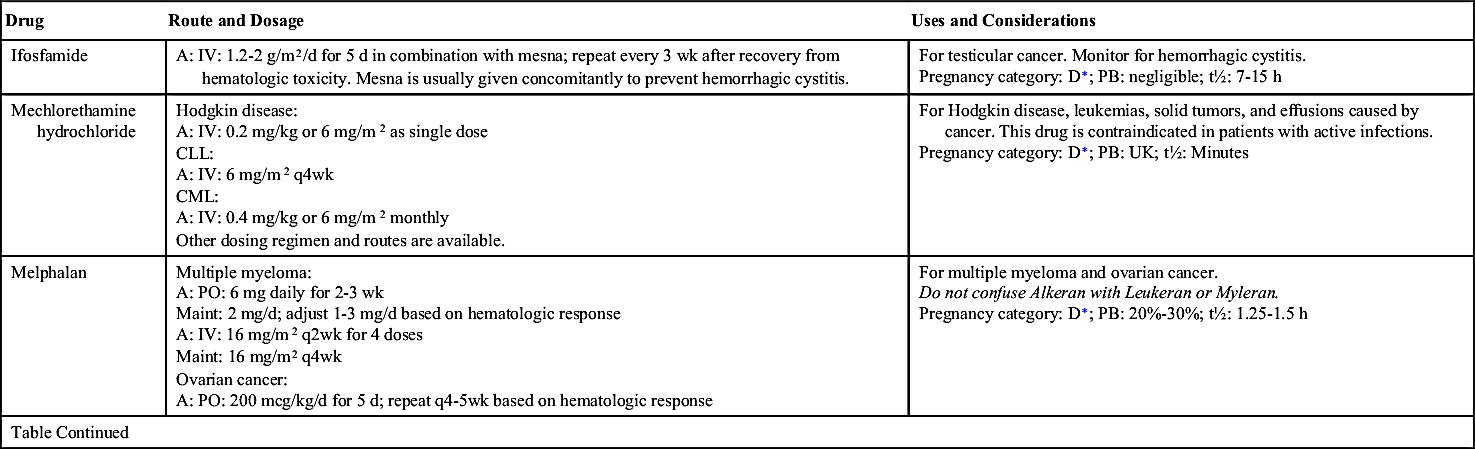
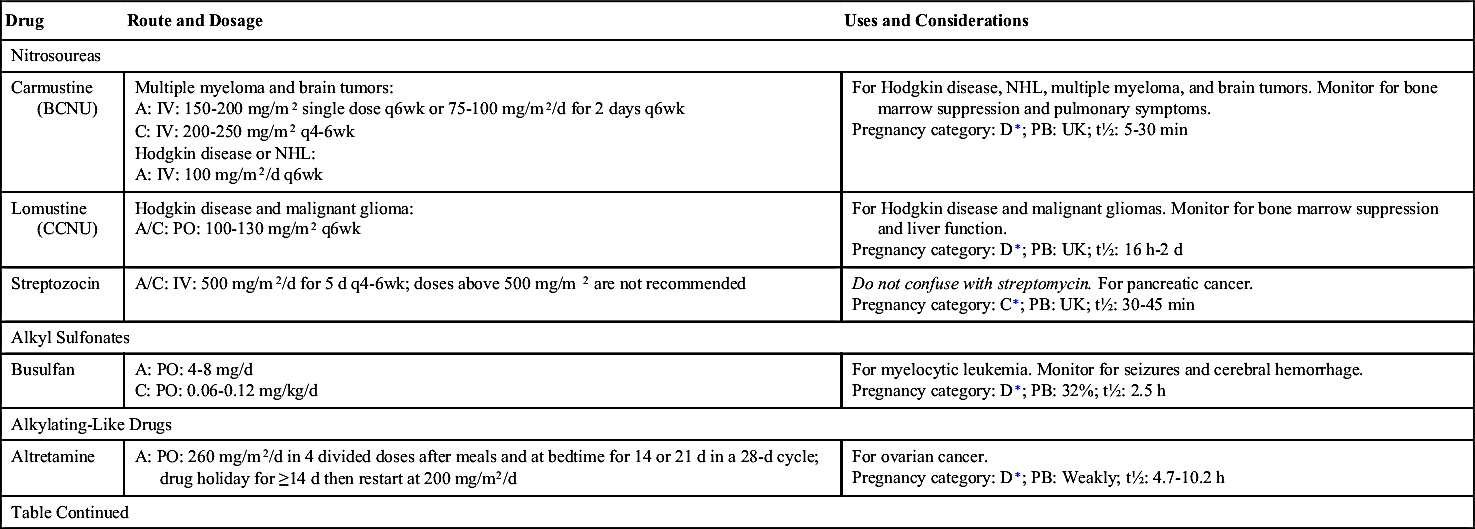
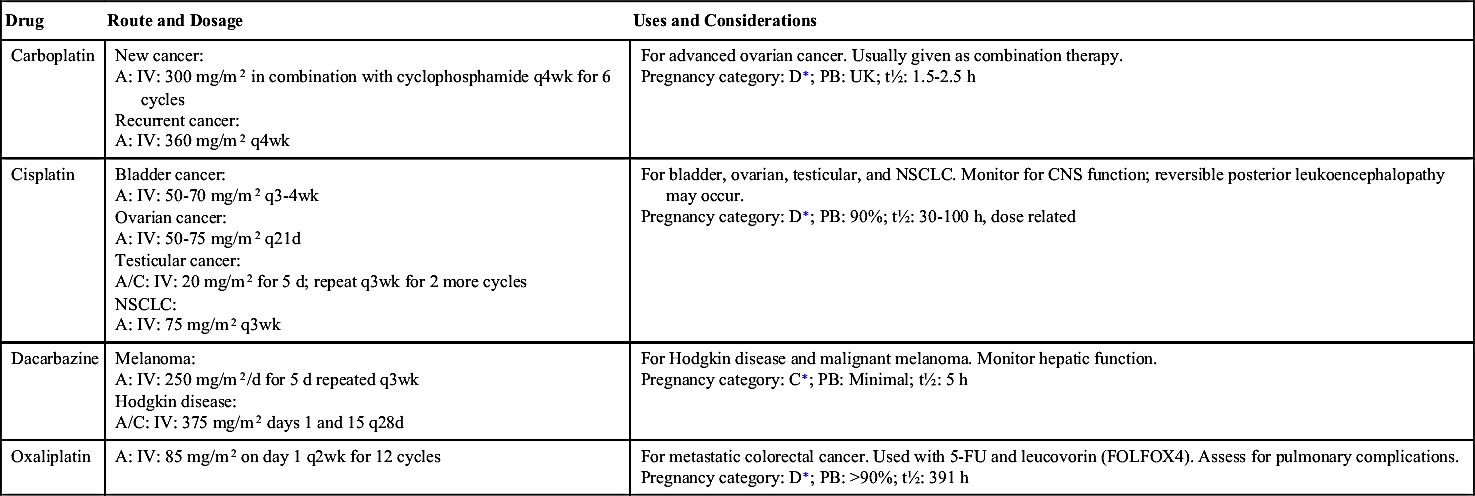
One of the largest groups of anticancer drugs is the alkylating compounds. Alkylating drugs damage the cell’s DNA by cross-linkage of DNA strands, abnormal base pairing, or DNA strand breaks, thus preventing the reproduction of cancer cells. Drugs in this group belong to the CCNS category and kill cells in all phases of the cell cycle. They are used to treat many different types of cancer, including leukemia, lymphoma, multiple myeloma, sarcoma, and solid tumors such as those of the breast, ovary, uterus, lung, bladder, and stomach. Even though alkylating agents are effective in all phases of the cell cycle, they are most effective in the G0 phase. Alkylating drugs are divided into five different classes: (1) nitrogen mustards, (2) nitrosoureas, (3) alkyl sulfonates, (4) triazines, and (5) ethylenimines. Table 32.3 lists some of the alkylating drugs, their uses, and considerations. Of the alkylating agents, nitrosoureas cross the blood-brain barrier, making them useful in the treatment of brain cancer. General adverse effects to anticancer drugs are discussed in Table 32.2. Additionally, alkylating agents given in high doses can cause long-term damage to the bone marrow, resulting in acute leukemia. The platinum (alkylating-like) drugs—cisplatin, carboplatin, and oxaliplatin—kill cells in a similar fashion but are less likely to cause leukemia later.
Cyclophosphamide
Cyclophosphamide, an alkylating agent, is an analogue of nitrogen mustard and has activity against many neoplastic diseases including Hodgkin and non-Hodgkin lymphoma (NHL), acute and chronic lymphocytic leukemia (CLL), multiple myeloma, breast and ovarian carcinoma, lung cancer, and retinoblastoma. The drug is also used for immunologic disorders such as lupus nephritis and has been shown to prevent progressive renal scarring, preserve renal function, induce renal remission, and decrease end-stage renal failure. This drug is a severe vesicant that causes tissue necrosis if it infiltrates into the tissues. Cyclophosphamide can be administered orally or intravenously. The patient should be well hydrated while taking cyclophosphamide to prevent hemorrhagic cystitis (bleeding due to severe bladder inflammation). Sodium 2-mercaptoethanesulfonate is a chemoprotectant drug often given with high-dose cyclophosphamide to inactivate urotoxic metabolites to reduce the incidence of hemorrhagic cystitis.
Pharmacokinetics
Oral cyclophosphamide is well absorbed in the GI system. Cyclophosphamide is a prodrug that is activated and extensively metabolized by the liver. About 5% to 25% of the drug is eliminated by the kidney as unchanged drug, and its elimination half-life is 3 to 12 hours. Approximately 20% is bound to plasma protein, and this is not dose dependent. Some cyclophosphamide metabolites are greater than 60% protein bound. Less than 10%, most in the form of metabolites, are excreted in feces.
Pharmacodynamics
Cyclophosphamide is an early antineoplastic drug used alone or with other drugs to treat a variety of cancers. Average time to peak plasma concentration (Tmax) is 1 hour. Several drug interactions can occur with cyclophosphamide. Patients should report all medications they are taking, including over-the-counter (OTC) medicines and herbal supplements. Anthracycline (e.g., doxorubicin) has been reported to induce cardiotoxicity when taken with cyclophosphamide, and it exacerbates hemorrhagic cystitis. Other serious drug interactions can occur when taking cyclophosphamide concomitantly with aspirin, allopurinol, phenobarbital, warfarin, thiazide diuretics, and some psychiatric medications. Complementary and Alternative Therapies 32.1 lists herbal supplements that may also interact with cyclophosphamide.
Side Effects and Adverse Reactions
The side effects of cyclophosphamide reflect those seen in the general class of antineoplastic drugs. (For the general side effects, see Table 32.2). Hemorrhagic cystitis is a serious problem that can arise when high doses of cyclophosphamide are given. Patients who receive a high dose should be assessed for cardiomyopathy and syndrome of inappropriate antidiuretic hormone (SIADH) during treatment with this drug. In addition, cyclophosphamide may increase pigmentation of the skin or nail beds. Prototype Drug Chart 32.1 details the pharmacologic behavior of cyclophosphamide.