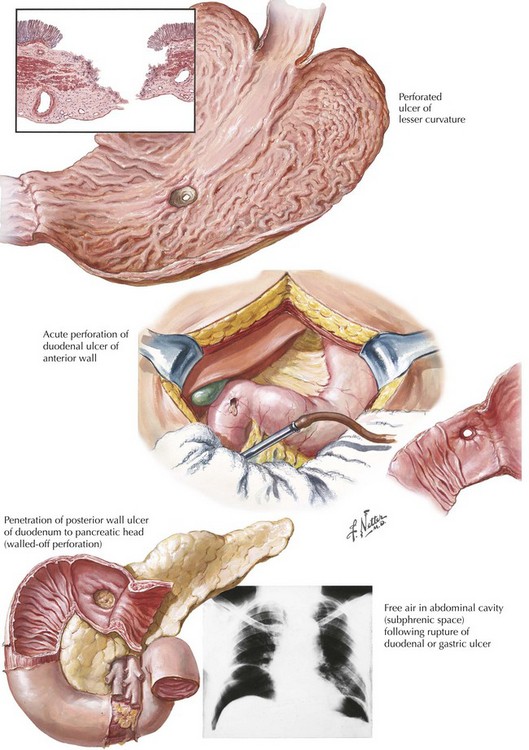
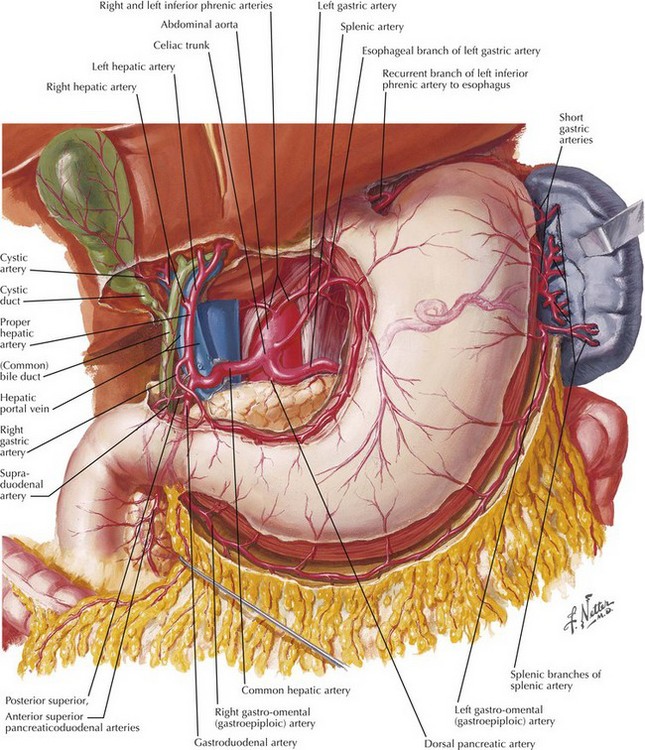
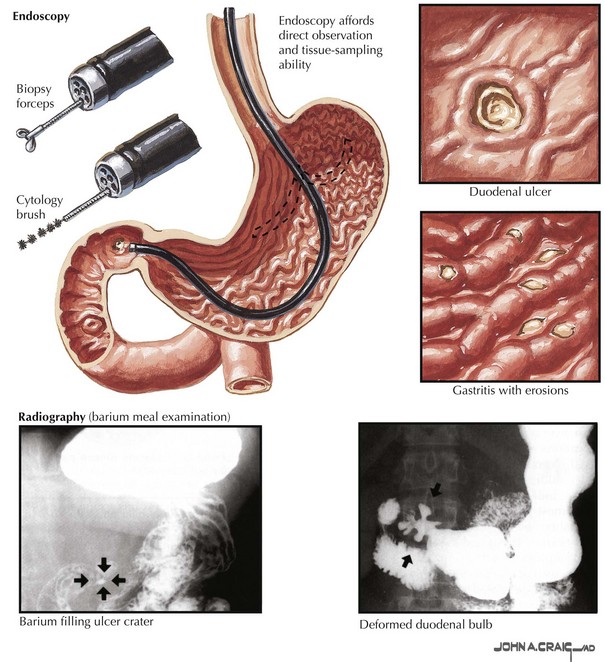
Chapter 7 Acute ulcer disease presents as acute gastrointestinal hemorrhage or perforation (Fig. 7-1). Knowledge of the anatomy of the stomach and its surrounding arterial supply can help predict the complication of ulceration (Fig. 7-2). Erosion of the ulcer posteriorly into the gastroduodenal artery can lead to life-threatening hemorrhage, presenting as tachycardia, hypotension, and hematemesis. Anterior erosion can lead to perforation of the duodenal wall with an acute abdomen, including tachycardia, abdominal tenderness with guarding and rigidity, and pneumoperitoneum on upright chest radiograph. In a more chronic scenario, recurrent episodes may lead to gastric outlet obstruction from repeated scarring. Less severe presentations of peptic ulcer disease often include complaints of burning epigastric abdominal pain. Definitive diagnosis and elimination of other conditions can be made by upper gastrointestinal endoscopy or upper gastrointestinal series (Fig. 7-3). Any gastric ulcerations seen on endoscopy should be biopsied at multiple sites around the border to determine if the lesion harbors a malignancy. Patients should be evaluated for the presence of H. pylori and treated if positive. They should also undergo medical treatment with acid suppression medication before surgery is considered. Patients with persistent severe disease, especially after maximal medical therapy and treatment for H. pylori, should be considered for a definitive acid-reducing procedure.
Truncal and Highly Selective Vagotomy
Clinical Indications
![]()
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


Basicmedical Key
Fastest Basicmedical Insight Engine