Fig. 8.1 Example of a patient with severe chronic blepharospasm; a disabling spasm of the periocular muscles is observed.
Pathophysiology
Neurophysiological recordings of the blink reflex have given important insights into the pathophysiology of blepharospasm. In patients with blepharospasm, the recovery cycle of the R2 component of the blink reflex is enhanced, presumably owing to a lack of brainstem interneuronal inhibition (Berardelli et al., 1985, 1998). Blepharospasm is also associated with an abnormal responsiveness of the blink reflex to sensory stimuli. Studies using magnetic brain stimulation also suggest a loss of inhibition and increased plasticity in the central nervous system of patients with blepharospasm (Defazio et al., 2007; Quartarone et al., 2008).
Anatomy of the periocular muscles
Knowledge of the anatomy of the upper facial muscles is essential for treating patients with blepharospasm. The muscle most commonly involved in blepharospasm is the orbicularis oculi. The orbicularis oculi, a sphincter muscle around the eye, comprises orbital, preseptal and pretarsal parts (Fig. 8.2). The orbital part originates in the medial part of the orbit and runs around the eye via the upper eye cover fold and lid and returns in the lower eyelid to the palpebral ligament. The preseptal or palpebral part originates in the palpebral ligament and runs above and below the eye to the lateral angle of the eye. The orbital and the preseptal muscles form concentric circles around the eye. The pretarsal part lies just around the palpebral margin.
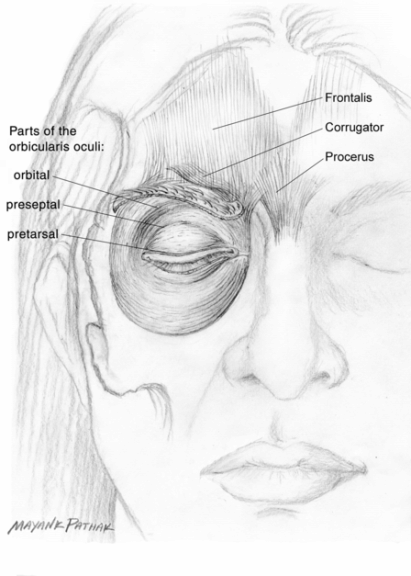
Fig. 8.2 Normal anatomy of the orbicularis oculi muscle. The orbital, preseptal and pretarsal parts are shown.
Blepharospasm can also involve the levator palpebrae superioris. This muscle arises from the inferior surface of the sphenoid bone. From this point, it diverges anteriorly to insert into the skin of the upper eyelid and the superior tarsal plate. The levator palpebrae elevates and retracts the upper eyelid. Other muscles that may also be affected in patients with blepharospasm are the corrugator, the procerus and the frontalis. The corrugator muscle originates at the inner orbit near the root of the nose and inserts into the skin of the forehead above the center of each eyebrow and pulls the eyebrows and skin from the center of each eyebrow to its inner corner medially and down. The procerus muscle originates in the fascia of the nasal bone and upper nasal cartilage, runs through the area of the root of the nose and fans upward to insert in the skin in the center of the forehead between the eyebrows. It acts to pull the skin of the center of the forehead down, forming transverse wrinkles in the glabella region and bridge of the nose. It usually acts together with corrugator or orbicularis oculi, or both. The frontalis muscle is a thin and quadrilateral muscle adherent to the superficial fascia. The frontalis muscle passes through and inserts into the bundles of the orbicularis oculi muscle on the superior border of the eyebrow at the middle and medial side of the upper eyelid. The frontalis muscle intermixes with the bundle of the orbicularis oculi muscle.
Botulinum neurotoxin treatment: techniques and results
In 1989 the US Food and Drug Administration approved botulinum neurotoxin serotype A (BoNT-A; formulation onabotulinumtoxinA [Botox, Allergan, Irvine, CA, USA]) as a therapeutic agent in patients with blepharospasm, and the European approval followed in 1994. Other formats of BoNT-A (abobotulinumtoxinA [Dysport, Ipsen, Paris, France] or incobotulinumtoxinA [Xeomin, Merz, Frankfurt, Germany]) were also shown to be effective and were subsequently approved worldwide (Truong et al., 2008). Treatment of blepharospasm with BoNT-A is usually straightforward and easy. Four injections are usually given in the orbital or preseptal portion of the orbicularis oculi muscle, but the number of injections in the orbicularis oculi can be increased to include the lateral canthus. The BoNT-A can also be injected into the pretarsal portion of the orbicularis oculi (Fig. 8.3) (Albanese et al., 1996; Cakmur et al., 2002). In most patients, pretarsal BoNT-A treatment achieves a significantly higher response rate and longer-lasting maximum response. Injection into the pretarsal part is more painful but produces fewer side effects. Injected into the pretarsal portion of the orbicularis oculi muscle is now considered by several authors the best method for treating involuntary eyelid closure caused by contractions of this muscle and for treating apraxia of eyelid opening (Ward et al., 2006). Different formulations of BoNT-A, such as abobotulinumtoxinA, incobotulinumtoxinA, have similar results, provided that approximate dose ratios of 1:4 (onabotulinumtoxinA: abobotulinumtoxinA) and 1:1 (onabotulinumtoxinA:incobotulinumtoxinA) are utilized. (The use of formal ratios is discouraged.) The total dose of BoNT-A injected per session ranges from 25 to 50 U onabotulinumtoxinA/incobotulinumtoxinA or 100 to 240 U abobotulinumtoxinA. In rare and selected patients with severe blepharospasm refractory to standard treatment regimens, increasing the dose of BoNT-A up to 100 U onabotulinumtoxinA (or equivalent doses) per session may be helpful. The mean treatment interval is around 3–4 months and appears strikingly stable in most patients. In individuals with severe blepharospasm involving other nearby facial muscles, the corrugator, procerus and frontalis can also be injected in addition to orbicularis oculi. The recommended doses are 2.5–5.0 U onabotulinumtoxinA/incobotulinumtoxinA or 10–15 U abobotulinumtoxinA for corrugators; 2.5–5 U onabotulinumtoxinA/incobotulinumtoxinA or 5–7.5 U abobotulinumtoxinA for the procerus muscle; and 15 U onabotulinumtoxinA/incobotulinumtoxinA or 40 U abobotulinumtoxinA for the frontalis muscle.
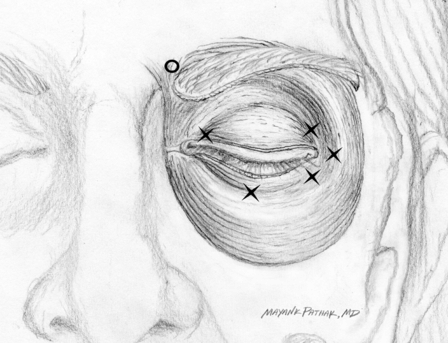
Fig. 8.3 Injection points in patient with blepharospasm. X, onabotulinumtoxinA 5 U/abobotulinumtoxinA 20 U; 0, onabotulinumtoxinA 2.5 U/abobotulinumtoxinA 10 U.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


