http://evolve.elsevier.com/McCuistion/pharmacology
This chapter describes drugs used for hormonal replacement and for inhibition of hormonal secretion from the pituitary, thyroid, parathyroid, and adrenal glands. Before reading this chapter, review the introduction to Unit XV, which describes the locations of the endocrine glands and the hormones they secrete. Knowledge of the various endocrine glands and their respective hormones and functions facilitates an understanding of the drugs that act on the endocrine glands.
Pituitary Gland
Anterior Lobe
The pituitary gland, or hypophysis, has an anterior and a posterior lobe. The anterior pituitary gland, called the adenohypophysis, secretes hormones that target glands and tissues, including:
• Growth hormone (GH), which stimulates growth in tissue and bone
• Thyroid-stimulating hormone (TSH), which acts on the thyroid gland
• Adrenocorticotropic hormone (ACTH), which stimulates the adrenal gland
• Gonadotropins (follicle-stimulating hormone [FSH] and luteinizing hormone [LH]), which affect the ovaries and testes
• Prolactin (PRL), which primarily affects the breast tissues
Drugs with adenohypophyseal properties used to stimulate or inhibit glandular activity for GH, TSH, ACTH, and PRL are discussed according to their therapeutic use. The negative feedback system that controls the amount of hormonal secretion from the pituitary gland and the target gland is discussed in the introduction to Unit XV.
Growth Hormone
Two hypothalamic hormones regulate growth hormone: (1) GH-releasing hormone (GH-RH; somatropin) and (2) GH-inhibiting hormone (GH-IH; somatostatin). GH does not have a specific target gland. It affects body tissues and bone; GH replacement stimulates linear growth when there are GH deficiencies. Growth hormone drugs cannot be given orally because they are inactivated by gastrointestinal (GI) enzymes. Subcutaneous (subcut) or intramuscular (IM) administration of GH is necessary.
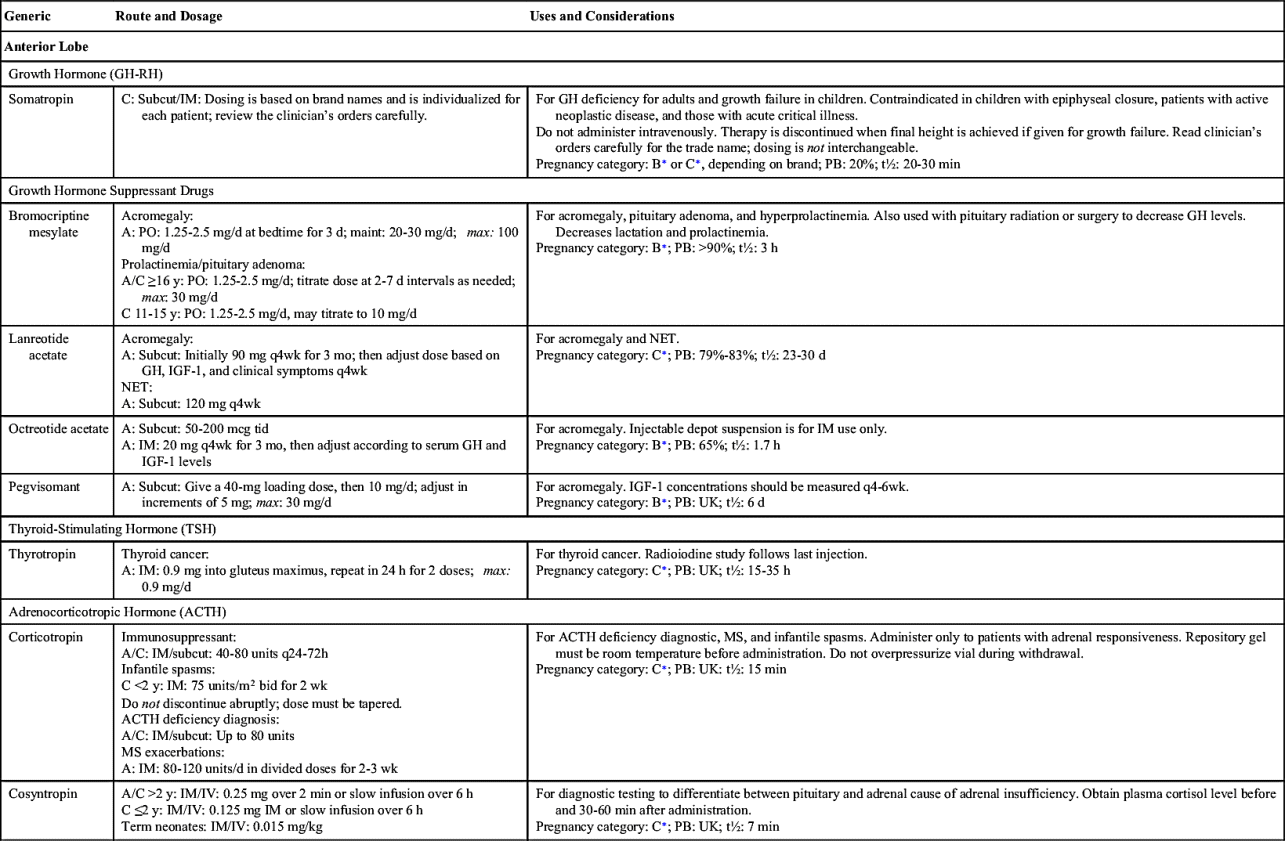
If a child’s height is well below the standard for a specified age, GH deficiency may be the cause, and dwarfism can result. Because of the cost, tests are performed to determine whether GH replacement therapy is essential. Since GH acts on newly forming bone, it must be administered before the epiphyses are fused. Administration of GH over several years can increase height by a foot. However, prolonged GH therapy can antagonize insulin secretion, eventually causing diabetes mellitus. Athletes should be advised not to take GH to build muscle and physique because of its effects on blood glucose along with other serious side effects. Table 46.1 lists the drugs used to replace or inhibit GH and gives their dosages, uses, and considerations.
Drug Therapy: Growth Hormone Deficiency
Somatropin is a growth hormone used to treat growth failure in children because of GH deficiency. Somatropin is a product that has the identical amino acid sequence as human growth hormone (HGH); it is contraindicated in pediatric patients who have growth deficiency due to Prader-Willi syndrome and in those who are severely obese or who have severe respiratory impairment because fatalities associated with these risk factors can occur. Corticosteroids can inhibit the effects of somatropin, therefore they should not be taken concurrently. Somatropin can enhance the effects of antidiabetics and can cause hypoglycemia.
Side effects and adverse effects
Somatropin can cause paresthesia, arthralgia, myalgia, peripheral edema, weakness, and cephalgia. Metabolic complications include glucose fluctuations, hypothyroidism, and hematuria. Flulike symptoms and hyperpigmentation of the skin can also occur. Adverse reactions include seizures, intracranial hypertension, and secondary malignancy (e.g., leukemia).
Drug Therapy: Growth Hormone Excess
Gigantism, excessive growth during childhood, and acromegaly, excessive growth after puberty, can occur with GH hypersecretion; these are frequently caused by a pituitary tumor. If the tumor cannot be destroyed by radiation, GH receptor antagonists (e.g., pegvisomant), somatostatin analogues (e.g., lanreotide, octreotide), and dopamine agonists (e.g., bromocriptine) act by either blocking GH receptor sites or by inhibiting secretion of GH.
Pegvisomant blocks GH receptor sites, preventing abnormal growth by normalizing insulin-like growth factor 1 (IGF-1) level, and it is given by injection. Common side effects include hyperhidrosis, cephalgia, and fatigue. Adverse effects include chest pain, hypertension, and elevated hepatic transaminases.
Lanreotide is an analogue of somatostatin that has actions similar to those of endogenous somatostatin. The effects of reduced GH are dose related and have a duration of at least 28 days after a single injection, therefore injections are given every 4 weeks. Lanreotide is available in depot formulation and is administered deep in the subcutaneous layer. Common side effects include mild GI symptoms: diarrhea, abdominal pain, nausea, vomiting, constipation, weight loss, and flatulence.
Octreotide is a synthetic somatostatin-inhibiting secretion of GH. It is available in immediate-release and depot formulations. Immediate-release formulations are given by thrice-daily subcutaneous injection, and depot injection is administered once monthly. Common side effects include GI upsets such as nausea, bloating, and flatus. Adverse effects include cardiac toxicity, such as bradycardia and arrhythmia.
Bromocriptine, a dopamine agonist, inhibits the secretion of GH caused by pituitary adenomas. It is available in oral form and has fewer side effects than other treatments for hyperpituitarism, which include GI symptoms (e.g., nausea, anorexia, dyspepsia, and xerostomia). Adverse effects include cardiac toxicity (e.g., hypertension, myocardial infarction [MI], and angina) and cerebrovascular toxicity (e.g., stroke and seizure). Bromocriptine should be discontinued if hypertension occurs due to pregnancy (e.g., preeclampsia, eclampsia, or pregnancy-induced hypertension).
Thyroid-Stimulating Hormone
The adenohypophysis secretes thyroid-stimulating hormone (TSH) in response to thyroid-releasing hormone (TRH) from the hypothalamus. TSH stimulates the thyroid gland to release thyroxine (T4) and triiodothyronine (T3, or liothyronine). Excess TSH secretion can cause hyperthyroidism, and a TSH deficit can cause hypothyroidism. Hypothyroidism may be caused by a thyroid gland disorder (primary cause) or a decrease in TSH secretion (secondary cause). Thyrotropin, a purified extract of TSH for thyroid cancer, is used as a diagnostic agent to differentiate between primary and secondary hypothyroidism. Side effects caused by thyrotropin include symptoms of hyperthyroidism. Other side effects include urticaria, rash, pruritus, and flushing.
Table 46.1 lists the drug used to replace TSH and its dosages, uses, and considerations.
Adrenocorticotropic Hormone
The hypothalamus releases corticotropin-releasing factor (CRF), which stimulates the pituitary corticotrophs to secrete adrenocorticotropic hormone (ACTH), which stimulates the release of glucocorticoids (cortisol), mineralocorticoids (aldosterone), and androgen from the adrenal cortex and catecholamines (epinephrine and norepinephrine) from the adrenal medulla. Usually, ACTH and cortisol secretions follow a diurnal rhythm, in which the ACTH and cortisol secretion is higher in the early morning and then decreases throughout the day. Stresses such as surgery, sepsis, and trauma override the diurnal rhythm, causing an increase in secretions of ACTH and cortisol. Hypocortisolism, or adrenal insufficiency, can occur and may be due to inadequate secretion of ACTH or dysfunction of the adrenal glands. Cosyntropin (synthetic ACTH) or corticotropin (exogenous ACTH) is administered to establish the endocrine gland responsible for the inadequate serum cortisol. Table 46.1 lists the drugs used to replace ACTH and their dosages, uses, and considerations.
Cosyntropin, a synthetic ACTH, is only approved for diagnostic purposes and is less potent and less allergenic than corticotropin. Cosyntropin stimulates the production and release of cortisol, corticosterone, and androgens from the adrenal cortex. It is administered via IM or intravenous (IV) routes. Plasma cortisol concentrations should be measured just before (basal) and 30 to 60 minutes after administration; normal response is the doubling of the basal cortisol level. Caution is advised when administering cosyntropin in patients receiving diuretics; cosyntropin can increase electrolyte loss. Patients taking estrogens can have an abnormal decreased response to the ACTH stimulation test. Side effects and adverse effects include bradycardia, hypertension, sinus tachycardia, and peripheral edema.
The ACTH drug corticotropin is primarily used to diagnose adrenal gland disorders, treat multiple sclerosis (MS), and treat infantile spasms; it is rarely used for corticosteroid-responsive disorders. Corticotropin is available as repository corticotropin injection (RCI), which is administered via IM or subcut routes. RCI controls the synthesis of ACTH from cholesterol, which stimulates adrenal glands in releasing its hormones. The effects of RCI are primarily due to the glucocorticoid from the adrenal cortex. RCI decreases the symptoms of MS during its exacerbation phase.  The drug should be tapered over a 2-week period for infantile spasms to avoid adrenal insufficiency. Corticotropin has numerous drug interactions. Diuretics and anti-Pseudomonas penicillins, such as piperacillin, can decrease the serum potassium level (hypokalemia). If the patient is taking a digitalis preparation and hypokalemia is present, digitalis toxicity can result. Phenytoin, rifampin, and barbiturates increase the metabolic rate, which can decrease the effect of the ACTH drug. Persons with diabetes may need increased insulin and oral antidiabetic (hypoglycemic) drugs because ACTH stimulates cortisol secretion, which increases the blood glucose level.
The drug should be tapered over a 2-week period for infantile spasms to avoid adrenal insufficiency. Corticotropin has numerous drug interactions. Diuretics and anti-Pseudomonas penicillins, such as piperacillin, can decrease the serum potassium level (hypokalemia). If the patient is taking a digitalis preparation and hypokalemia is present, digitalis toxicity can result. Phenytoin, rifampin, and barbiturates increase the metabolic rate, which can decrease the effect of the ACTH drug. Persons with diabetes may need increased insulin and oral antidiabetic (hypoglycemic) drugs because ACTH stimulates cortisol secretion, which increases the blood glucose level.
 The drug should be tapered over a 2-week period for infantile spasms to avoid adrenal insufficiency. Corticotropin has numerous drug interactions. Diuretics and anti-Pseudomonas penicillins, such as piperacillin, can decrease the serum potassium level (hypokalemia). If the patient is taking a digitalis preparation and hypokalemia is present, digitalis toxicity can result. Phenytoin, rifampin, and barbiturates increase the metabolic rate, which can decrease the effect of the ACTH drug. Persons with diabetes may need increased insulin and oral antidiabetic (hypoglycemic) drugs because ACTH stimulates cortisol secretion, which increases the blood glucose level.
The drug should be tapered over a 2-week period for infantile spasms to avoid adrenal insufficiency. Corticotropin has numerous drug interactions. Diuretics and anti-Pseudomonas penicillins, such as piperacillin, can decrease the serum potassium level (hypokalemia). If the patient is taking a digitalis preparation and hypokalemia is present, digitalis toxicity can result. Phenytoin, rifampin, and barbiturates increase the metabolic rate, which can decrease the effect of the ACTH drug. Persons with diabetes may need increased insulin and oral antidiabetic (hypoglycemic) drugs because ACTH stimulates cortisol secretion, which increases the blood glucose level.TABLE 46.2
Physiologic Data: Adrenal Hyposecretion and Hypersecretion
| Body System | Adrenal Hyposecretion (Addison Disease) | Adrenal Hypersecretion (Cushing Syndrome) |
Metabolism: Glucose Protein Fat | Hypoglycemia, muscle weakness, weight loss | Hyperglycemia, muscle wasting; thinning of skin; poor wound healing; osteoporosis; fat accumulation in face (moon face), back of neck (buffalo hump), and trunk (protruding abdomen); hyperlipidemia; high cholesterol, weight gain |
| Central nervous system | Apathy, depression, fatigue, irritability | Increased neural activity, mood elevation, irritability, seizures, weakness, fatigue |
| Integument | Hyperpigmentation | Easy bruising, striae, plethora, and excess hair growth to face (hirsutism), neck, chest, abdomen, and thighs |
| Eyes | None | Cataract formation |
| Cardiovascular | Tachycardia, hypotension, orthostatic hypotension, cardiovascular collapse, syncope, dizziness | Hypertension, edema, heart failure |
| Gastrointestinal | Nausea, vomiting, diarrhea, abdominal pain, anorexia | Peptic ulcers |
| Hematology | Anemia | Increased red blood cell count and neutrophils, impaired clotting |
| Reproductive | Irregular menses or amenorrhea | Amenorrhea, decreased fertility and libido |
| Fluids and electrolytes | Hypovolemia, hyponatremia, hyperkalemia | Hypervolemia, hypernatremia, hypokalemia |
Side effects and adverse effects
Side effects and adverse reactions are due to the activity of the adrenal glands and their hormones. See Table 46.2 for the physiologic data for hypoadrenalism and hyperadrenalism.
Prolactin
The primary function of prolactin (PRL) is stimulation of breast tissue for milk production. PRL deficiency (hypoprolactinemia) is generally without symptoms except during breastfeeding, when it can cause lactation disruption. Excess PRL (hyperprolactinemia) produces symptoms in both males and females. Males may develop excess breast tissue (gynecomastia) and may lactate (galactorrhea), and excess PRL decreases sperm production. Females with excess PRL can experience lactation that is not pregnancy related, or they can develop amenorrhea. Excess PRL can be treated with dopamine agonists (e.g., bromocriptine, cabergoline). Cabergoline is better tolerated, has a longer half-life, and offers more convenient dosing than bromocriptine. Dopamine agonists are discussed in Chapter 20.
Posterior Lobe
The posterior pituitary gland, known as the neurohypophysis, secretes antidiuretic hormone (ADH) and oxytocin. ADH and oxytocin are produced by the hypothalamus and travel by way of the hypophysial portal system into the posterior pituitary gland for storage and secretion. (Oxytocin is discussed in Unit XVII.) Table 46.1 lists the drugs used to replace or inhibit ADH and their dosages, uses, and considerations.
ADH promotes water reabsorption from the renal tubules to maintain water balance in the body fluids. When there is a deficiency of ADH, large amounts of water are excreted by the kidneys. This condition, called diabetes insipidus (DI), can lead to severe fluid volume deficit and electrolyte imbalances. Head injury and brain tumors resulting in trauma to the hypothalamus and pituitary gland can also cause DI. Fluid and electrolyte balance must be closely monitored in these patients, and ADH replacement may be needed. The ADH preparations, vasopressin and desmopressin acetate, can be administered intranasally or by injection. Desmopressin is also used in managing patients with bleeding disorders due to hemophilia A or von Willebrand disease type 1. Unlike vasopressin, desmopressin does not induce the release of ACTH, nor does it increase serum cortisol level. It is available as a nasal spray, oral tablet, and in parenteral formulations. ADH is contraindicated in patients with moderate to severe renal disease and in patients with hyponatremia or a history of such. Side effects and adverse reactions include hyponatremia, cephalgia, dyspepsia, diarrhea, nausea, and vomiting. Seizures may occur due to hyponatremia. Hypotension and tachycardia can occur due to hypovolemia.
When secretion of ADH from the posterior pituitary gland is excessive, the most common cause is small cell carcinoma of the lung. Medications, other malignancies, and stressors (e.g., pain, infection, anxiety, trauma) may also be causative factors. These conditions lead to an excessive amount of water retention expanding the intracellular and intravascular volume known as syndrome of inappropriate antidiuretic hormone (SIADH). This increased fluid volume causes enhanced glomerular filtration and decreased tubular sodium reabsorption. Natriuresis, excretion of urinary sodium, can occur and can cause hyponatremia. SIADH can be treated by fluid restrictions, by hypertonic saline, or by drugs such as demeclocycline, conivaptan, and tolvaptan.
Demeclocycline is a tetracycline antibiotic that can induce nephrogenic DI within 5 days of starting treatment that is reversed in 2 to 6 days following cessation of treatment. The most common complaint with demeclocycline is photosensitivity. As with other tetracyclines, dental discoloration and enamel hypoplasia can occur. Fluid and electrolytes must be monitored closely.
Vaptans (e.g., conivaptan and tolvaptan) are vasopressin receptor antagonists and are indicated for the treatment of euvolemic hyponatremia in SIADH. Its effects increase serum sodium and free water clearance.  Conivaptan is contraindicated in patients with corn allergy. Common complications with conivaptan therapy are injection site reactions such as phlebitis, pain, edema, and pruritus; therefore the drug must be administered only in large veins, and infusion sites should be rotated every 24 hours. Other common side effects and adverse reactions include orthostatic hypotension, syncope, hypertension, atrial fibrillation, and electrolyte imbalances.
Conivaptan is contraindicated in patients with corn allergy. Common complications with conivaptan therapy are injection site reactions such as phlebitis, pain, edema, and pruritus; therefore the drug must be administered only in large veins, and infusion sites should be rotated every 24 hours. Other common side effects and adverse reactions include orthostatic hypotension, syncope, hypertension, atrial fibrillation, and electrolyte imbalances.
 Conivaptan is contraindicated in patients with corn allergy. Common complications with conivaptan therapy are injection site reactions such as phlebitis, pain, edema, and pruritus; therefore the drug must be administered only in large veins, and infusion sites should be rotated every 24 hours. Other common side effects and adverse reactions include orthostatic hypotension, syncope, hypertension, atrial fibrillation, and electrolyte imbalances.
Conivaptan is contraindicated in patients with corn allergy. Common complications with conivaptan therapy are injection site reactions such as phlebitis, pain, edema, and pruritus; therefore the drug must be administered only in large veins, and infusion sites should be rotated every 24 hours. Other common side effects and adverse reactions include orthostatic hypotension, syncope, hypertension, atrial fibrillation, and electrolyte imbalances.Tolvaptan is given orally. It has black-box warnings for patients with alcoholism, hepatic disease, and malnutrition; tolvaptan should be avoided in these patients. Common side effects and adverse reactions are related to loss of fluids (e.g., thirst, dry mouth, constipation, hyperglycemia, dizziness, and weakness). Fluid and serum electrolytes must be closely monitored.
Vaptans are contraindicated in patients with hypovolemia. Fluid restrictions should be avoided during therapy to prevent too rapid an increase in serum sodium.
Table 46.1 lists the drugs used for pituitary disorders and their dosages, uses, and considerations.
Thyroid Gland
The thyroid gland is an important regulator for many of the bodily functions. The three hormones produced and secreted by the thyroid gland are triiodothyronine (T3), thyroxine (T4) that helps with metabolism, and to a lesser extent calcitonin for regulating serum calcium. A majority of thyroid hormone is synthesized as T4, which is then converted to T3 to act on target cells. Iodide, an inorganic form of iodine, is needed for the synthesis of T3 and T4. These are carried in the blood by thyroxine-binding globulin (TBG) and albumin, which protect the hormones from being degraded. T3 is more potent than T4, and only unbound (free) T3 and T4 have biologic actions and produce a hormonal response.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree