Patient Story
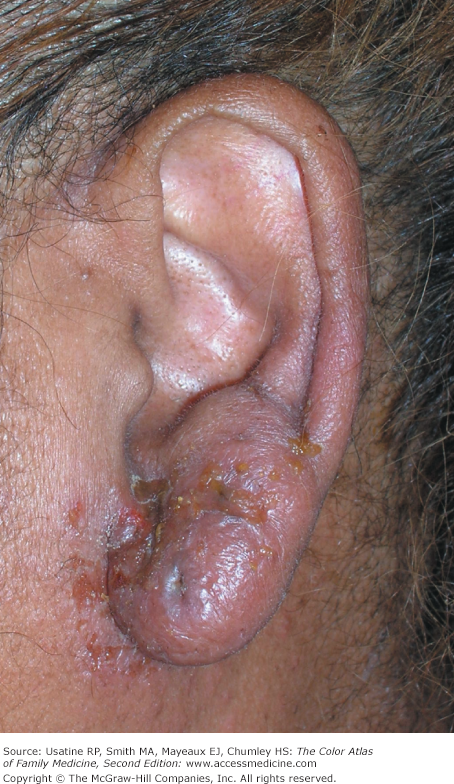
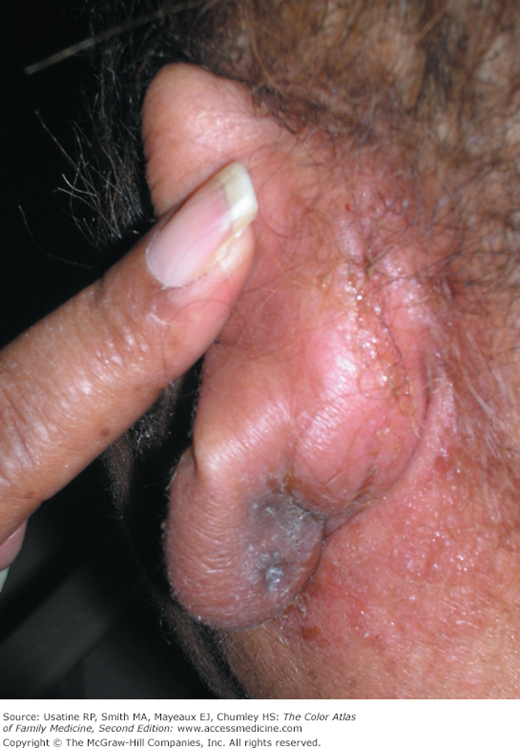
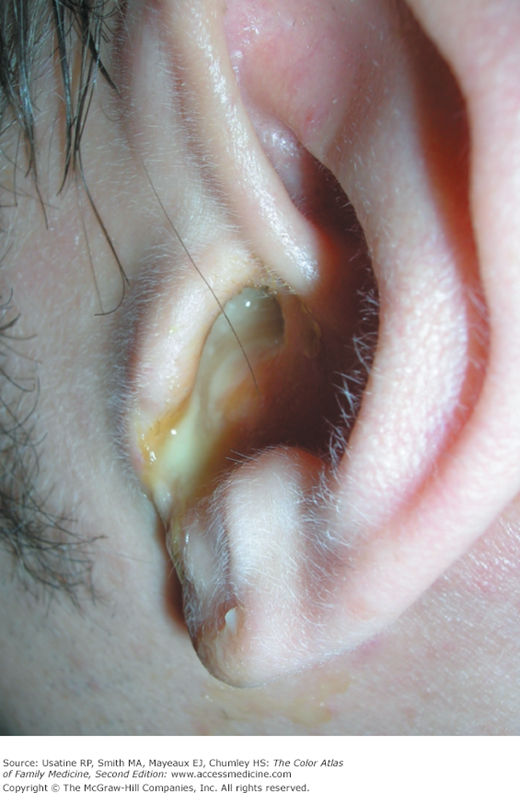
A 40-year-old woman with type 2 diabetes presents to her family physician with a 2-day history of bilateral otalgia, otorrhea, and hearing loss. Symptoms started in the right ear and then rapidly spread to the left ear. She had a low-grade fever and was systemically ill. The external ear was swollen with honey-crusts (Figures 27-1 and 27-2). The external auditory canal (EAC) was narrowed and contained purulent discharge (Figure 27-3). Ear, nose, and throat (ENT) was consulted and she was admitted to the hospital for the presumptive diagnosis of malignant otitis externa. The MRI showed some destruction of the temporal bone. She was started on IV ciprofloxacin and the ear culture grew out Pseudomonas aeruginosa sensitive to ciprofloxacin. The patient responded well to treatment and was able to go home on oral ciprofloxacin 5 days later.
Introduction
Otitis externa (OE) is common in all parts of the world. OE is defined as inflammation, often with infection, of the EAC.1
Epidemiology
- Incidence of OE is not known precisely; its lifetime incidence was estimated at 10% in one study.2
- Occurs more in adults than in children.
Etiology and Pathophysiology
- Common pathogens, which are part of normal EAC flora, include aerobic organisms predominantly (P. aeruginosa and Staphylococcus aureus) and, to a lesser extent, anaerobes (Bacteroides and Peptostreptococcus). Up to a third of infections are polymicrobial. A small proportion (2% to 10%) of OE is caused by fungal overgrowth (e.g., Aspergillus niger usually occurs with prolonged antibiotic use).1
- Pathogenesis of OE includes the following:
- Trauma, the usual inciting event, leads to breech in the integrity of EAC skin.
- Skin inflammation and edema ensue, which, in turn, leads to pruritus and obstruction of adnexal structures (e.g., cerumen glands, sebaceous glands, and hair follicles).
- Pruritus leads to scratching, which results in further skin injury.
- Consequently, the milieu of the EAC is altered (i.e., change in quality and quantity of cerumen, increase in pH of EAC, and dysfunctional epithelial migration).
- Finally, the EAC becomes a warm, alkaline, and moist environment—ideal for growth of different pathogens.
- Trauma, the usual inciting event, leads to breech in the integrity of EAC skin.
Risk Factors
- Environmental factors:
- Moisture—Macerates skin of EAC, elevates pH, and removes protective cerumen layer (from swimming, perspiration, high humidity).
- Trauma—Leads to injury of EAC skin (from cotton buds, fingernails, hearing aids, ear plugs, paper clips, match sticks, mechanical removal of cerumen).
- High environmental temperatures.
- Moisture—Macerates skin of EAC, elevates pH, and removes protective cerumen layer (from swimming, perspiration, high humidity).
- Host factors:
- Anatomical—Wax and debris accumulate and lead to moisture retention (e.g., a narrow ear canal, hairy ear canal).
- Cerumen—Absence or overproduction of cerumen (leads to loss of the protective layer and moisture retention, respectively).
- Chronic dermatologic disease (e.g., atopic dermatitis, psoriasis, seborrheic dermatitis).
- Immunocompromise (e.g., chemotherapy, HIV, AIDS).
- Anatomical—Wax and debris accumulate and lead to moisture retention (e.g., a narrow ear canal, hairy ear canal).
Diagnosis
- OE can either be localized, like a furuncle, or generalized (Figure 27-4). The latter is known as “diffuse OE,” or simply OE. Seborrheic dermatitis of the external ear and EAC can be diffuse or generalized (see Figure 27-4).
- Forms of (diffuse) OE:1