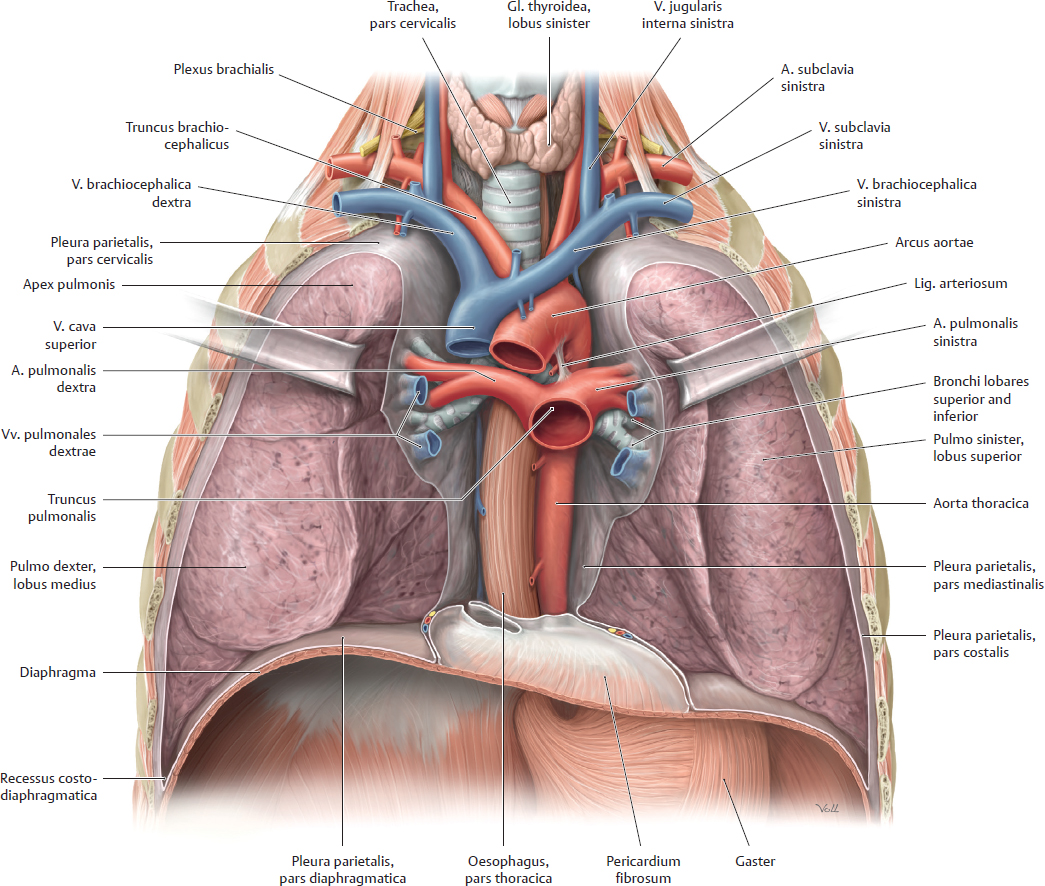
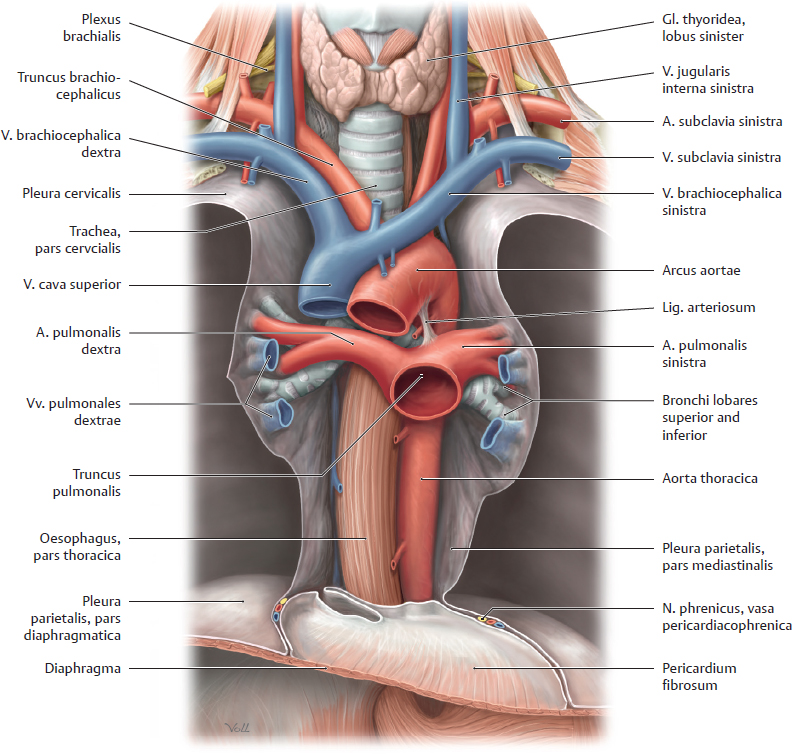
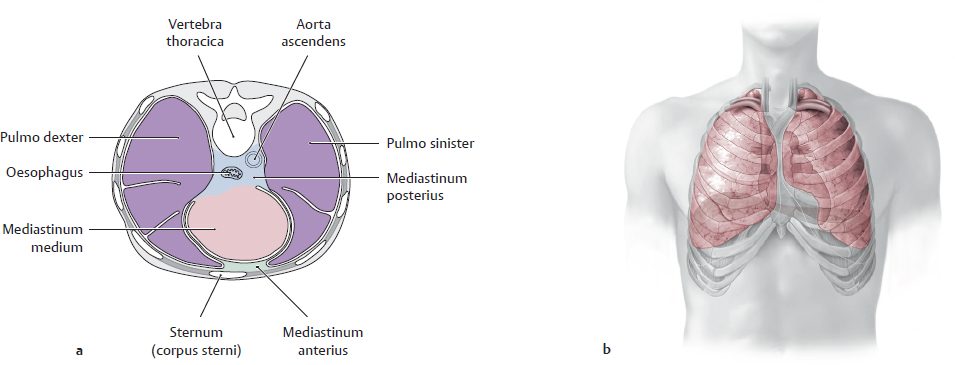
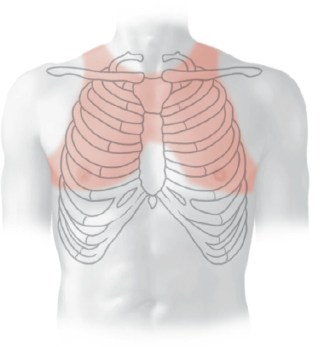
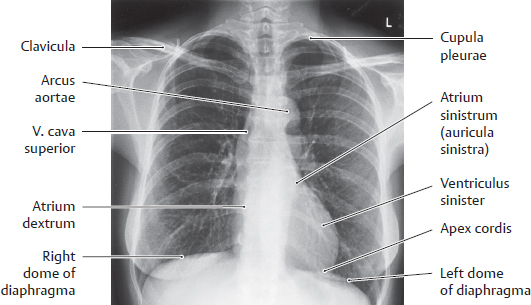
13 Organs of the Respiratory System and their Neurovasculature A Location of the lungs in the thorax: Topographical relations a Transverse section through the thorax, superior view. The lungs completely occupy the cavitates pleurales sinistra and dextra flanking the mediastinum. Anteriorly, they approach each other in front of the pericardium and posteriorly they are located close to the columna vertebralis. Due to the asymmetrical position of the cor, the left lung is slightly smaller than the right lung (see D). b Projections of the lungs onto the skeleton thoracis, anterior view. Superiorly, both lungs extend above the apertura thoracis superior; inferiorly, the undersurface of the lungs arches over the domes of the diaphragma. The distinct notch at the inferior medial border of the left lung is due to the heart, which is partially overlapped by the medial border of the lungs. B Percussion field of the lungs Anterior view. The air-filled lungs constitute a resonant cavity that produces a sonorous lung sound on percussion of the chest. The sonorous lung field extends cranially, with attenuation, to the apices of the lungs at the apertura thoracis superior. It also extends to the front of the chest, again with attenuation, and closely approaches the anterior midline (recessus costomediastinalis with margo anterior pulmonis on deep inspiration, see pp. 130 and 133). The fluid-filled cor dampens the lung sounds, producing an area of cardiac dullness (see p. 89). A sharp transition from lung sound to liver sound is clearly audible at the margo inferior of the right lung, since the hepar is a solid organ with less resonance (medium-pitched, nonsonorous percussion sound). Note: The lung percussion field does not precisely match the anatomical extent of the lungs because only well-aerated portions of the lung are sonorous to percussion. The anatomical extent of the lungs is greater than the percussion field. C Radiographic appearance of the normal lungs Anterior view. Different regions of the lungs show different degrees of lucency in the chest radiograph. The perihilar region of the lung (where the bronchi principales enter the lung and vessels enter and leave the lung) is less radiolucent than the peripheral region, which contains small-caliber vascular branches and bronchi segmentales. Additionally, the perihilar lung region is partly covered by the cor. These “shadows” appear as white or bright areas on the radiograph. The same effect is observed in diseased lung areas, which appear more opaque as a result of fluid infiltration (inflammation) or tissue proliferation (neoplasia). These opacities are easier to detect in the peripheral part of the lung, which is inherently more radiolucent than the perihilar lung. D The lungs in situ Anterior view of the opened thorax (depiction simplified). The cor and pericardium have been removed. The vessels surrounding the cor have been transected, and all mediastinal connective tissues have been removed. The lungs have been retracted laterally to stretch and expose the bronchi principales. The cavitas abdominis has been opened and eviscerated, leaving only the gaster in place. The pars cervicalis of the trachea is still visible below the cartilago cricoidea. Shortly below its entry into the chest through the apertura thoracis superior, the trachea is almost completely obscured by the great vessels (see p. 88). The pars thoracica of the oesophagus can be seen below the bifurcatio tracheae, which lies directly behind the pars ascendens aortae. The lungs in the cavitates pleurales closely approach the columna vertebralis posteriorly, while anteriorly they extend in front of the pericardium and narrow the mediastinum anterius. Percussion of the chest yields a “sonorous” lung sound (see B) which is dulled by the cor and pericardium. The extent of the lungs depends on the phase of respiration (see p. 151), but the apices pulmonum always extend into the apertura thoracis superior, which is closed by a condensation of loose connective tissue—the membrana suprapleuralis. The apical lung tissue is pictured here as soft and pliant, corresponding to its natural consistency. It should be noted that when the cavitates pleurales are opened at operation, the lungs tend to collapse toward the hilum owing to their elastic recoil; they do not completely fill the cavitates pleurales as shown here. (For clarity, the lungs are portrayed in an expanded state.) A Pleura and cavitates pleurales: Structure and topography a Transverse section through the thorax, inferior view; b Anterior view of the right cavitas pleuralis, which has been opened. The cavitates pleurales are paired like the lungs they enclose, which is one reason they have a greater extent than the lungs: • anteriorly, they extend past the pericardium to just behind the sternum, and in the dorsomedial direction up to the columna vertebralis (a); • due to the arching of the dome of the diaphragma, the inferior margin of the cavitates pleurales extends downward and overlaps with the cavitas abdominis (b); • due to the asymmetrical position of the cor in the mediastinum, the left cavitas pleuralis is slightly smaller than the right cavitas pleuralis (a); • because the cavitates pleurales have a greater extent than the lungs, recesses develop in them (see also p. 133). Completely analogous to the cavitates peritonealis and pericardialis, each cavitas pleuralis is composed of two serous layers: the pleura visceralis (pleura pulmonalis attached to the surface of the lung) and the pleura parietalis (attached to the fascia endothoracica). As a result of the attachment to the thorax, the pleura and thus the lungs (which adhere to the walls of the cavitates pleurales through capillary forces) automatically follow the movements of the chest wall. The line of junction between the tunicae serosae pleurae visceralis and parietalis occurs along at the medial surface of the lungs (see p. 26). The capillary fissure-like space between the pleurae visceralis and parietalis contains a small amount of clear serous fluid. This fluid layer allows both layers of the pleura to glide past each other and at the same time serves to hold the pleural layers together by capillary forces. For more about the topographical parts of the pleural layers see C. B Pars mediastinalis of the pleura and the mediastinum The mediastinum is bounded on either side by the cavitates pleurales from which it is separated by the pars mediastinalis of the pleura parietalis. The pars mediastinalis pleurae is in direct contact with the mediastinal connective tissue. All neurovascular structures running between mediastinum and lungs (e.g., bronchi, aa. pulmonales, vv. pulmonales) are wrapped in pars mediastinalis pleurae, which fuses with the outer layer of the connective tissues of these neurovascular structures. The nn. phrenici and aa./vv. pericardiophrenicae, which are only just visible at the bottom of the diagram, pass between the pars mediastinalis pleurae and pericardium. C Portions of the pleura parietalis
13.1 Lungs: Location in the Thorax
13.2 Cavitates Pleurales
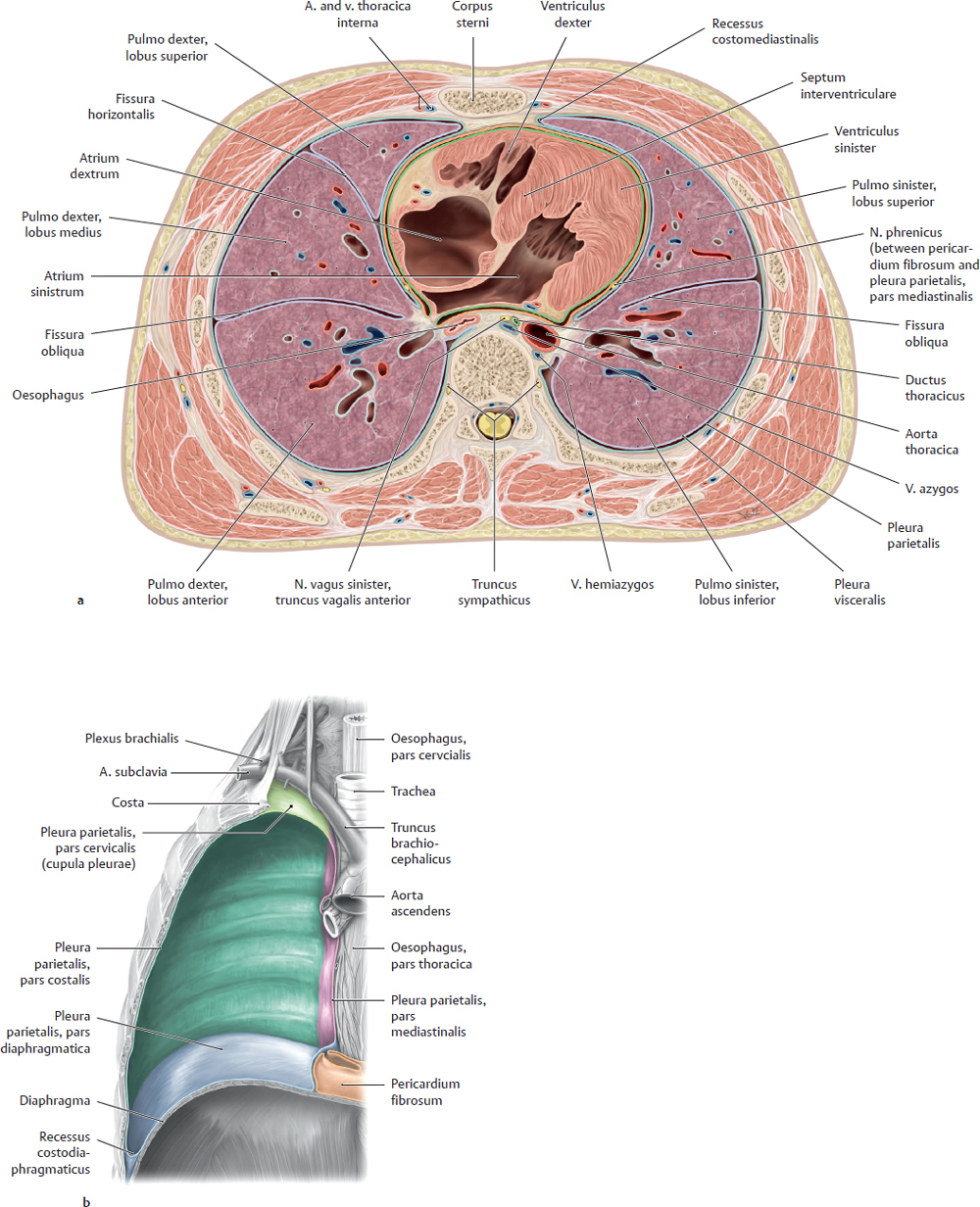
Portion | Location | Adjacent layer of connective tissue |
Pars costalis | Inner chest wall | Fascia endothoracica |
Pars diaphragmatica | Surface of the diaphragma | Fascia phrenicopleuralis |
Pars mediastinalis | Lateral to mediastinum | Unnamed, direct transition to the connective tissue of the mediastinum |
Cupula pleurae | Apical, above the apertura thoracis superior | Membrana suprapleuralis (Sibson’s fascia) |
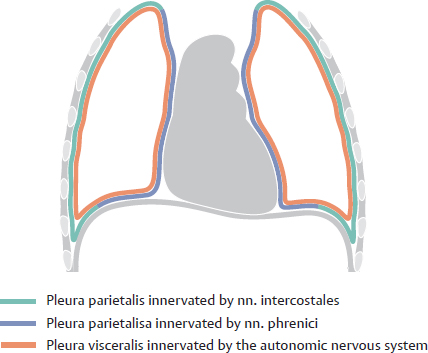
D Innervation of the pleura
The pleura parietalis, as part of the trunk wall, is innervated by somatic sensory nerves: The pars mediastinalis and the largest part of the pars diaphragmatica are supplied by the nn. phrenici. A small part of the pars diaphragmatica located close to the ribs is also supplied by nn. intercostales. The pars costalis is innervated by nn. intercostales. The pleura visceralis is the organ-related layer and as such receives a sparse innervation by visceral sensory fibers, probably from the pars sympathica of the nervous system. The corresponding neuronal perikarya are located in ganglia sensoria nervorum spinalium—their branching axons pass through the ganglion sympathicum without terminating.
13.3 Boundaries of the Lungs and Pleura Parietalis
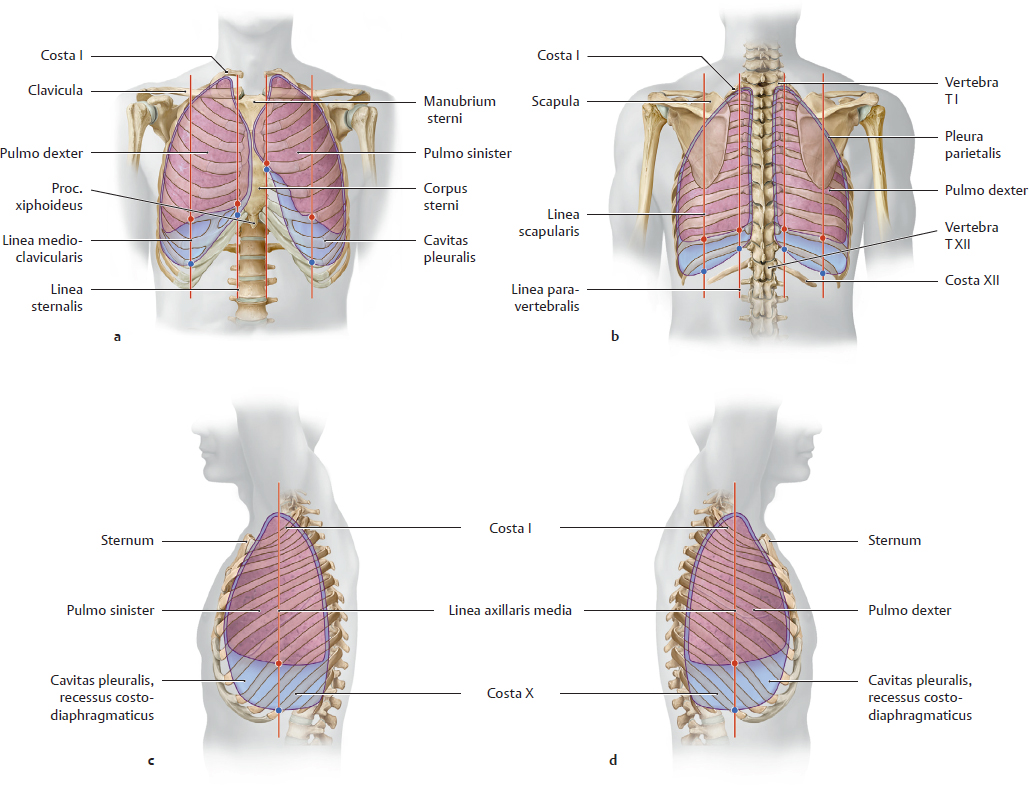
A Projections of the boundaries of the lungs and pleura parietalis onto the skeleton thoracis
Anterior view (a), posterior view (b), view from the left and right sides (c and d). The diagrams show the boundaries of the pleura parietalis and lungs. The table (see B) summarizes some of the projection sites of the pleura and lungs onto the anterior, posterior, and lateral thoracic wall. The pleura parietalis lines the inner surface of the skeleton thoracis and projects itself onto palpable or visible bony landmarks.
The connection between these landmarks forms the boundaries of the pleura parietalis (important in cases of pleural inflammations with effusion – visible on radiographs).
Note: The asymmetrical position of the cor makes the cavitas pleuralis slightly smaller on the left side than on the right side. This causes the boundaries of the pleura parietalis on the left side at the level of the cor to shift more laterally than on the right side.
B Relations of the lungs and pleural boundaries to landmarks on the skeleton thoracis

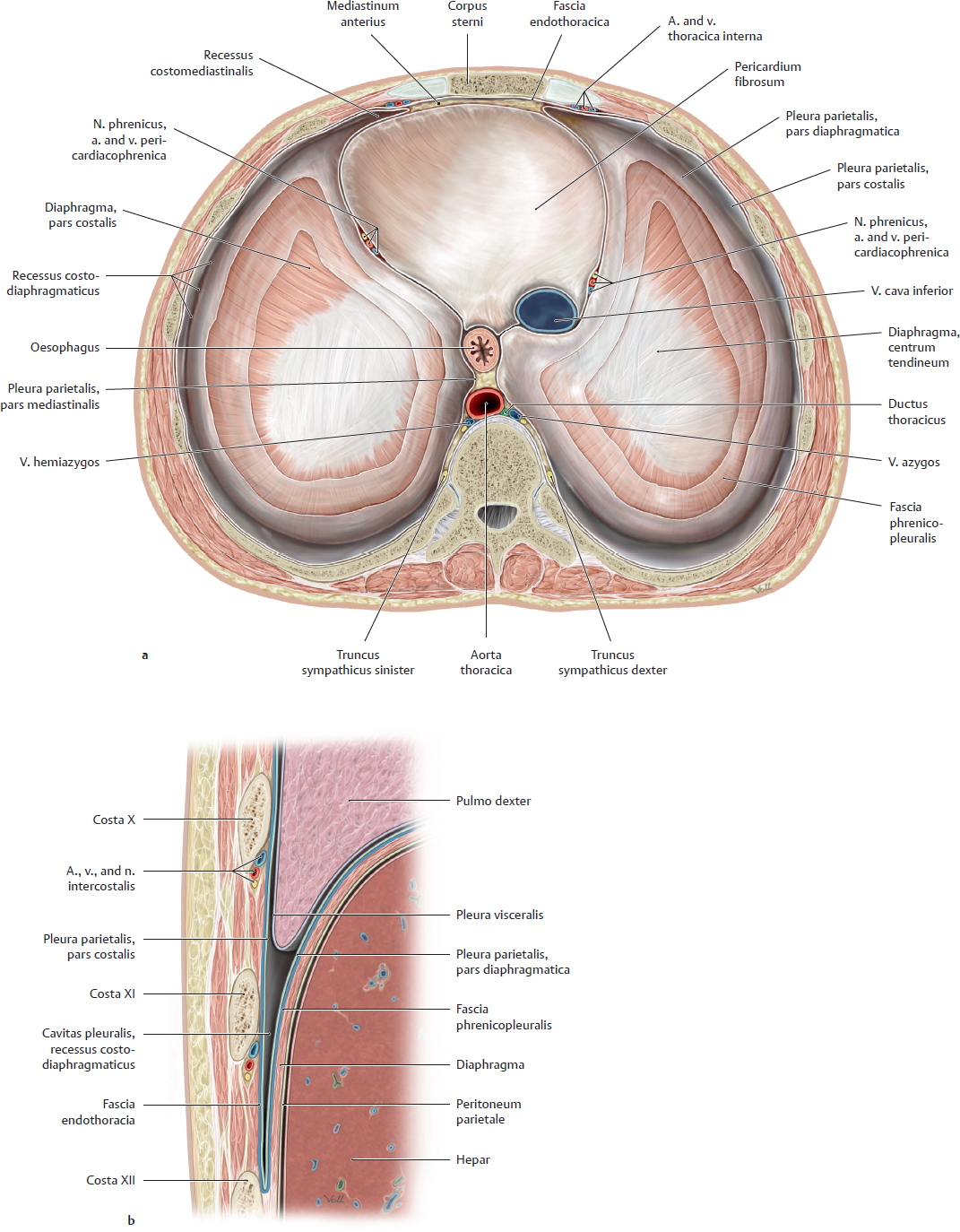
C Recesses of the pleura parietalis
a Superior view, the cor and lungs have been removed, the pleura parietalis has been removed over a large area of the diaphragma; b Detail from a parasagittal section through the right side of the thorax and abdomen, viewed from the lateral side.
The extent of the pleura visceralis, which directly invests the lung, is identical to that of the lung. However, the pleura parietalis, which completely lines the inner surface of the chest wall, has a greater extent than the lungs. This arrangement creates two major recesses within the cavitas pleuralis:
• The recessus costodiaphragmaticus, located on each side of the domes of the diaphragma, facing the ribs (b), which is lined by the partes costalis and diaphragmatica of the pleura parietalis, and
• The recessus costomediastinalis, located anterior to the pericardium, on the left and right sides of the mediastinum anterius (a), which is lined by the partes costalis and mediastinalis of the pleura parietalis.
For more about the function of the recessus pleurales, see p. 151.
13.4 Trachea
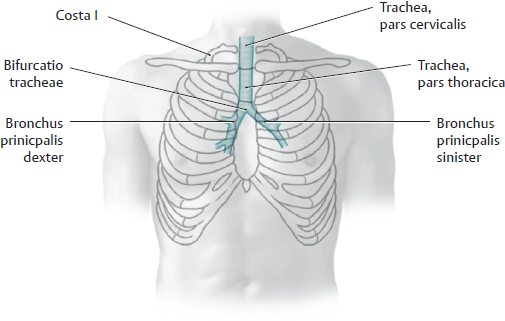
A The trachea projected onto the neck and thorax
The trachea is located in the mediastinum and lies precisely in the median plane. The initial part (pars cervicalis) of the trachea begins just below the larynx, and its pars thoracica ends at the bifurcatio tracheae. The trachea expands during inspiration and contracts during expiration. The projection in the figure shows the appearance of the trachea at functional residual capacity (relaxed end-expiration).
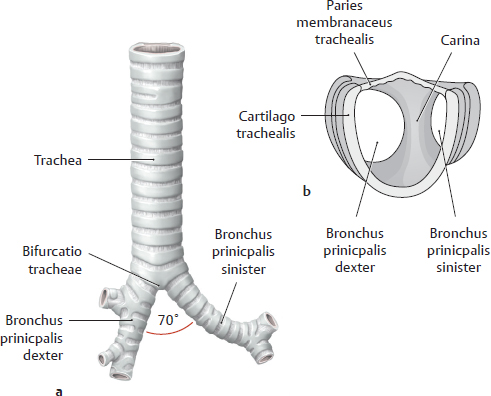
B Shape of the trachea
a Anterior view; b Superior view of the bifurcatio tracheae.
The trachea is a flexible airconducting tube 10 to 12 cm long. At the approximate level of the corpora vertebrae T3–T4, it bifurcates into the bronchi principales sinister and dexter, which form an angle of approximately 55–70°. Viewed from the anterior side, the bifurcatio tracheae lies just below the junction of the manubrium and corpus sterni.
Note: The bronchus principalis dexter is more vertical than the bronchus principalis sinister, and therefore it is more common for aspirated foreign bodies to enter the bronchus principalis dexter than the sinister. This also makes it easier to view the interior of the bronchus principalis dexter with an endoscope. Owing to the asymmetry of the cor and the associated asymmetrical position of the lungs, the bronchus principalis sinister is slightly longer than the dexter.
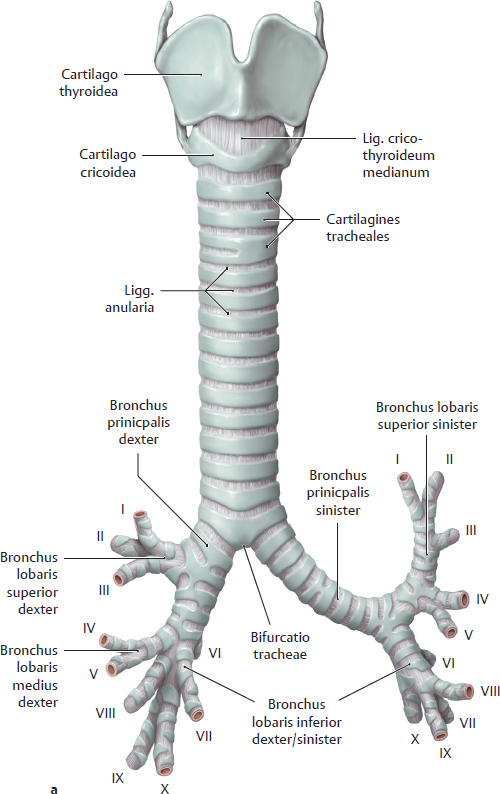
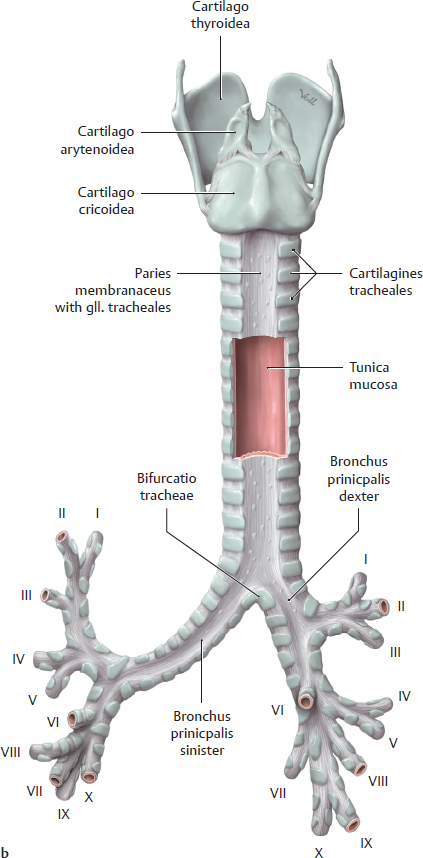
C Structure of the trachea and arbor bronchialis
a Anterior view; b Posterior view with opened posterior wall. The trachea consists of 16–20 horseshoe-shaped rings composed of hyaline cartilage (the cartilagines tracheales) and a posterior paries membranaceus composed of connective tissue and m. trachealis (not shown here). The cartilagines tracheales are interconnected longitudinally by collagenous connective tissue (ligg. anularia). The two parts of the trachea are clearly distinguishable:
• Pars cervicalis: extends from the first cartilago trachealis below the cartilago cricoidea of the larynx at the level of the C 6/C 7 vertebrae to the apertura thoracis superior (see A);
• Pars thoracica: extends from the apertura thoracis superior to the bifurcatio tracheae, where the trachea divides into the bronchi principales dexter and sinister at the level of the T4 vertebra. A cartilaginous spur (carina, see Bb) at the bifurcatio tracheae projects upward into the tracheal lumen.
The bronchi principales sinister and dexter divide into two or three bronchi lobares, respectively, which subsequently branch into bronchi segmentales (see D).
D Divisions of the trachea and arbor bronchialis
Bronchus principalis dexter | Bronchus principalis sinister |
Bronchus lobaris superior dexter Bronchus segmentalis apicalis (I) Bronchus segmentalis posterior (II) Bronchus segmentalis anterior (III) | Bronchus lobaris superior sinister Bronchus segmentalis apicoposterior (I, II) Bronchus segmentalis anterior (III) |
Bronchus lobaris medius Bronchus segmentalis lateralis (IV) Bronchus segmentalis medialis (V) | Bronchus lingularis superior (IV) Bronchus lingularis inferior (V) |
Bronchus lobaris inferior dexter Bronchus segmentalis superior (VI) Bronchus segmentalis basalis medialis (VII) Bronchus segmentalis basalis anterior (VIII) Bronchus segmentalis basalis lateralis (IX) Bronchus segmentalis basalis posterior (X) | Bronchus lobaris inferior sinister Bronchus segmentalis superior (VI) Bronchus segmentalis basalis medialis (VII) Bronchus segmentalis basalis anterior (VIII) Bronchus segmentalis basalis lateralis (IX) Bronchus segmentalis basalis posterior (X) |
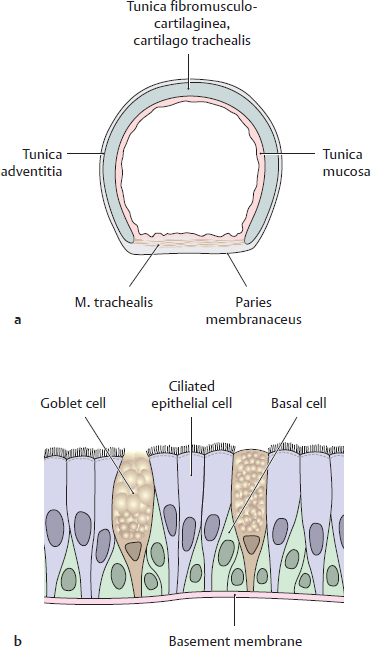
E Wall structure of the trachea and bronchi principales
a Histological organization of the wall of the trachea: The trachea is a fibroelastic tube supported by spaced C-shaped rings of hyaline cartilage. The open end of each ring is closed by a posterior paries membranaceus. The entire tube is lined by a tunica mucosa, consisting of an epithelial layer (b), with an underlying lamina propria of loose connective tissue containing a fibroelastic band at its base. Below the mucosa is a submucosa containing seromucous glandulae that secrete a protective mucous film. The paries membranaceus that closes the open end of the cartilago trachealis contains circularly-oriented smooth muscle (m. trachealis) with additional longitudinal bands. The outermost component is an adventitial layer of connective tissue. Microscopic structure changes substantially at different levels of the arbor bronchialis (see pp. 140–141, 146–147).
b The tracheal epithelium: Facing the tracheal lumen is a pseudostratified respiratory epithelium with three prominent cell types: columnar ciliated cells, which drive mucus and particles along the tracheal surface toward the pharynx, goblet cells, which secrete mucus, and basal cells, which do not span the full height of the epithelium. Basal cells are mitotic precursors for other cell types in the epithelium. A thick basement membrane underlies this epithelium. The tracheal epithelium contains several other intrinsic cell types, not depicted, as well as lymphocytes and mast cells that have migrated from underlying connective tissue. Prolonged exposure to irritants such as tobacco smoke increases the number of goblet cells and decreases the flow of secretions, compromising airway clearance.
Note: The epithelium of the carina, unlike that of the rest of the trachea, consists of nonkeratinized squamous cells
13.5 Lungs: Shape and Structure
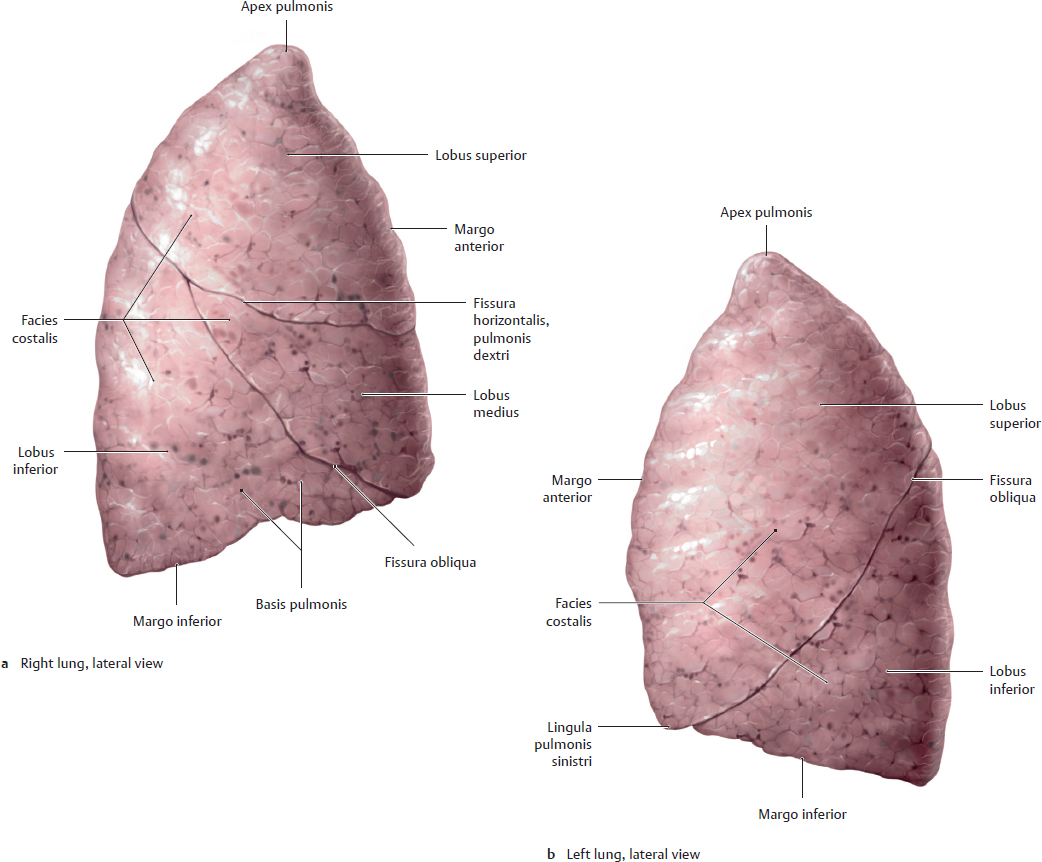
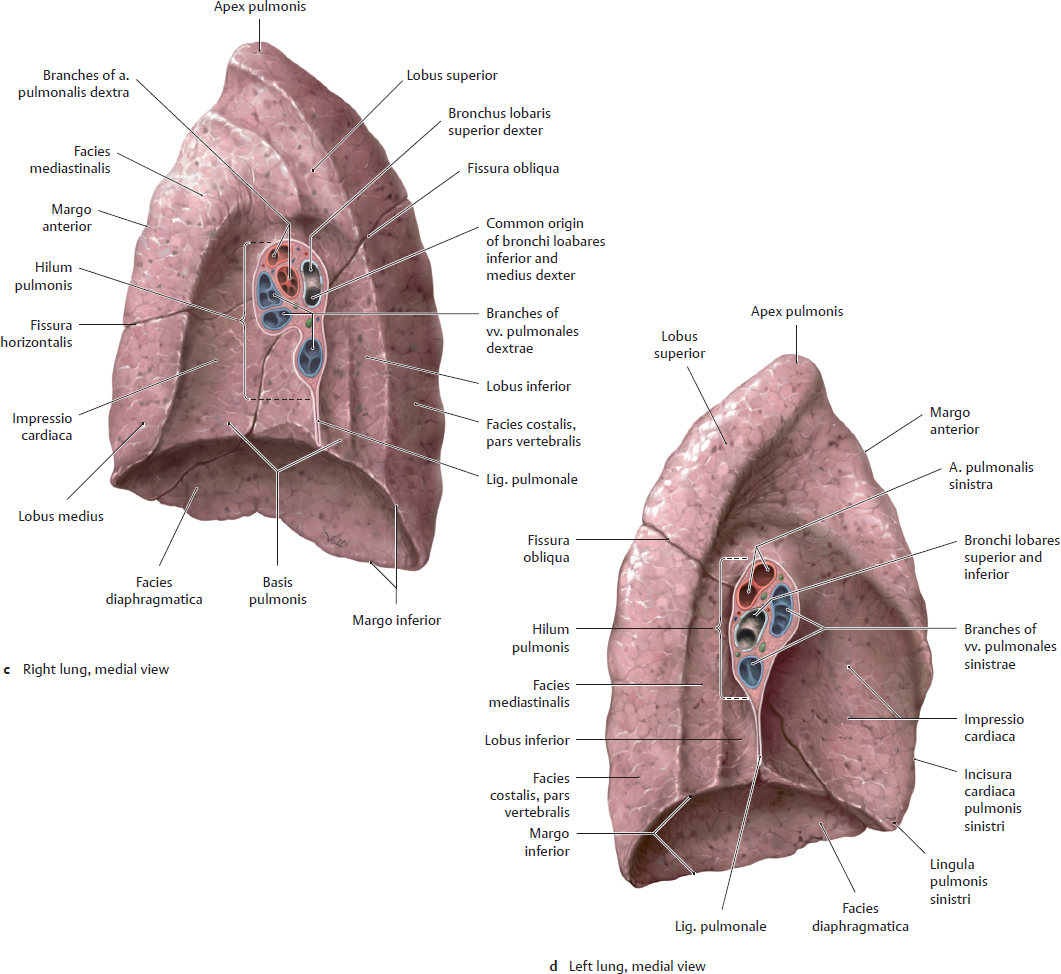
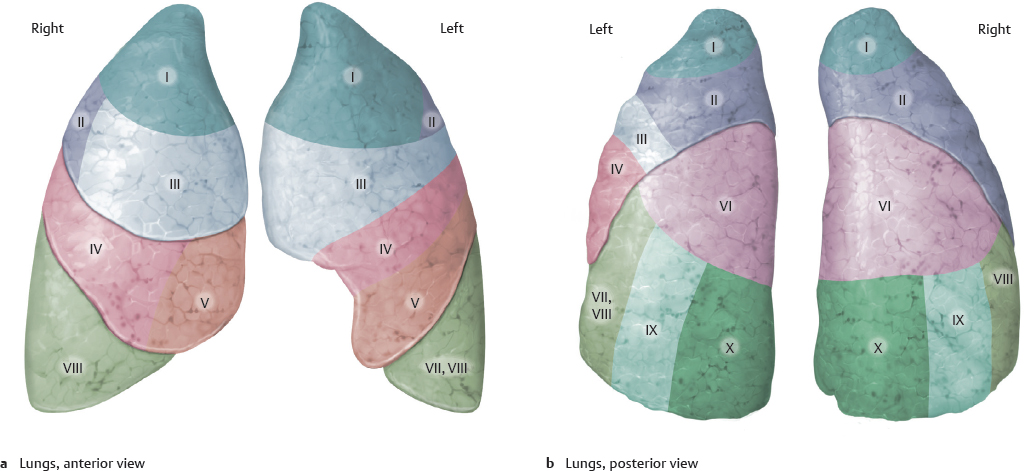
A Gross anatomy of the left and right lung
a, b Lateral view. c, d Medial view.
The color of the healthy lung ranges from gray to bluish-pink. Grayishblack particles are often visible beneath the pleural surface (as shown here) and are found even in nonsmokers. They do not necessarily have pathological significance, consisting of dust or carbonaceous particles that have been inhaled and deposited in the lung. A lung that has not been chemically fixed has a soft, spongy texture and collapses when taken from the chest. The shape shown above is the in vivo shape of the dynamically expanded lung (see p. 151). The right lung, with a volume of approximately 1500 cm, is slightly larger than the left lung, which has a volume of approximately 1400 cm (due to the inclination of the cor to the left side). Each of the lungs is divided into lobi by one or more interlobar fissures:
• The left lung is divided into two lobes (lobi superior and inferior) by one fissura obliqua.
• The right lung consists of three lobes (lobi superior, medius, and inferior) separated by one fissura obliqua and one fissura horizontalis. The pulmonary fissures are completely lined by pleura visceralis.
Note: Owing to the steep angle of the fissura obliqua in the left lung, the lingula of the lobus superior forms part of the basis pulmonis sinistri. The smallest morphologically distinct and autonomous structural unit of the lung is the lobulus, which is aerated by a bronchiolus. The pulmonary lobuli are separated from one another by (often incomplete) fibrous interlobular septa, demarcating numerous polyhedral areas that may be visible on the lung surface.
Aside from the differences noted above, both lungs have the same basic parts:
• The apex pulmonis, which extends into the apertura thoracis superior
• The basis pulmonis, which rests on the diaphragma
• Surfaces of the lung:
– Facies costalis: relates laterally and posteriorly to the ribs. The pars vertebralis of the facies costalis faces the columna vertebralis (see c, d);
– Facies mediastinalis: relates medially to the mediastinum.
– Facies diaphragmatica (see c, d): relates inferiorly to the diaphragma.
– Facies interlobares. In the chemically fixed specimen, impressions from the ribs are visible on the facies costalis, an impressio cardiaca on the facies mediastinalis, and an impression from the diaphragma leaflet on the facies diaphragmatica. The left lung additionally has a distinct incisura cardiaca in its margo anterior.
• Borders of the lung:
– Margo anterior: sharp, thin border located at the junction of the facies costalis and mediastinalis (inserts into the recessus costomediastinalis).
– Margo inferior: located at the junction of the facies diaphragmatica and facies costalis or mediastinalis, sharp at the facies costalis (inserts into the recessus costodiaphragmaticus) and blunt at the facies mediastinalis.
• Hilum: area where bronchi and neurovascular structures enter and leave the facies mediastinalis. The radix pulmonis comprises all of the blood vessels, lymphatics, bronchi, and nerves that enter and emerge at the hilum. Elements of the arbor bronchialis are generally located in the posterior part of the hilum. Pulmonary venous branches are anterior and inferior, and pulmonary arterial branches are found mainly in the upper part of the hilum.
Both lungs are invested by a serous membrane, the pleura visceralis (pulmonary pleura), which is reflected at the mediastinal surface to continue as the pleura parietalis. This pleural fold is ruptured when the lung is removed, appearing as the lig. pulmonale.