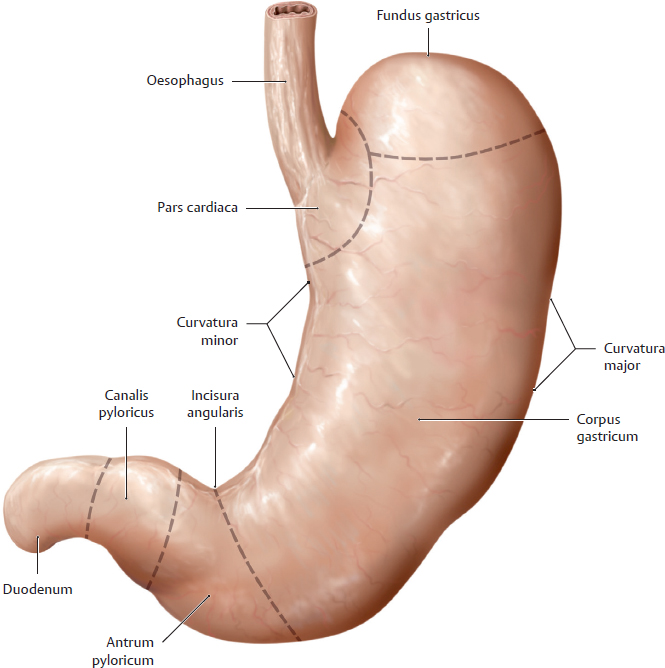
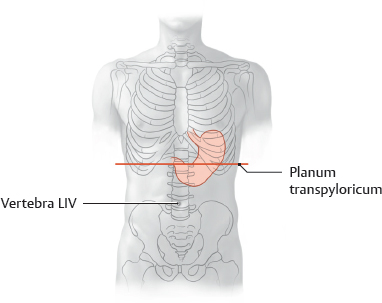
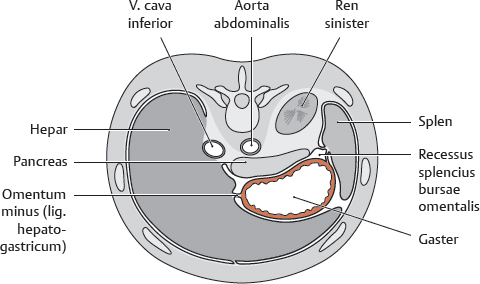
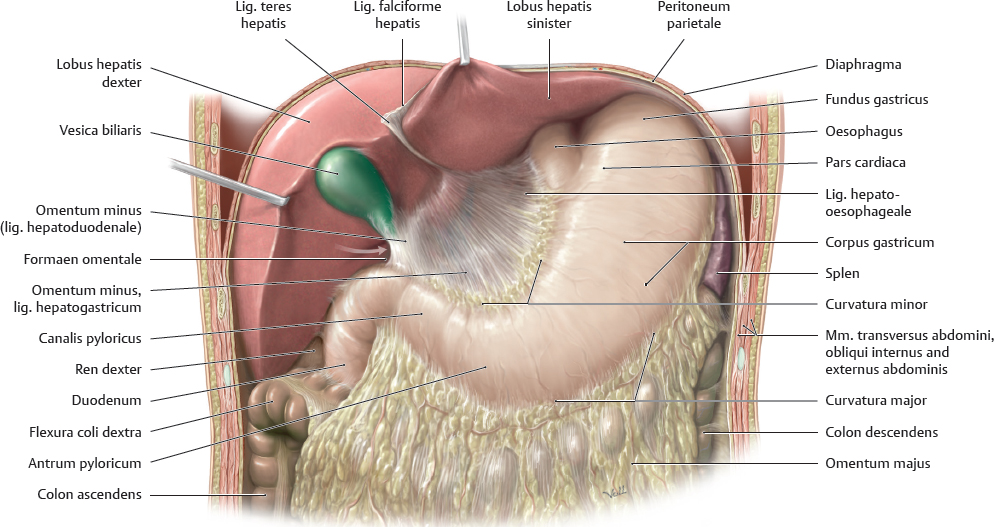
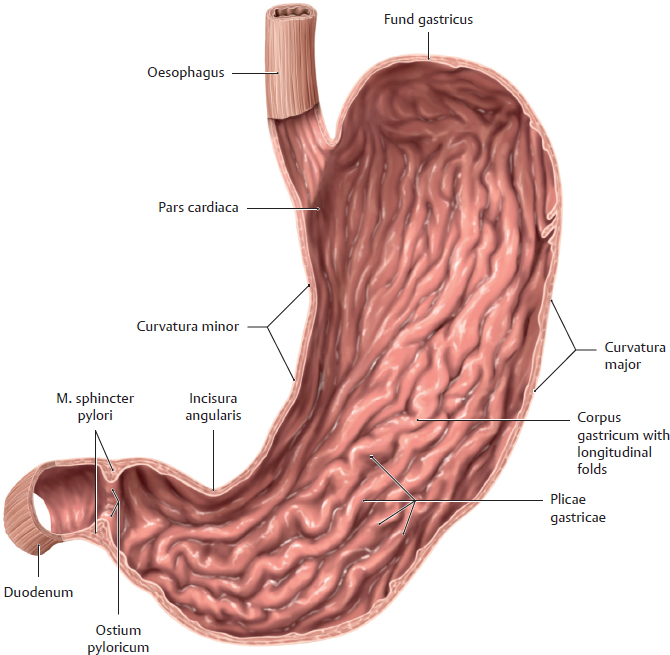
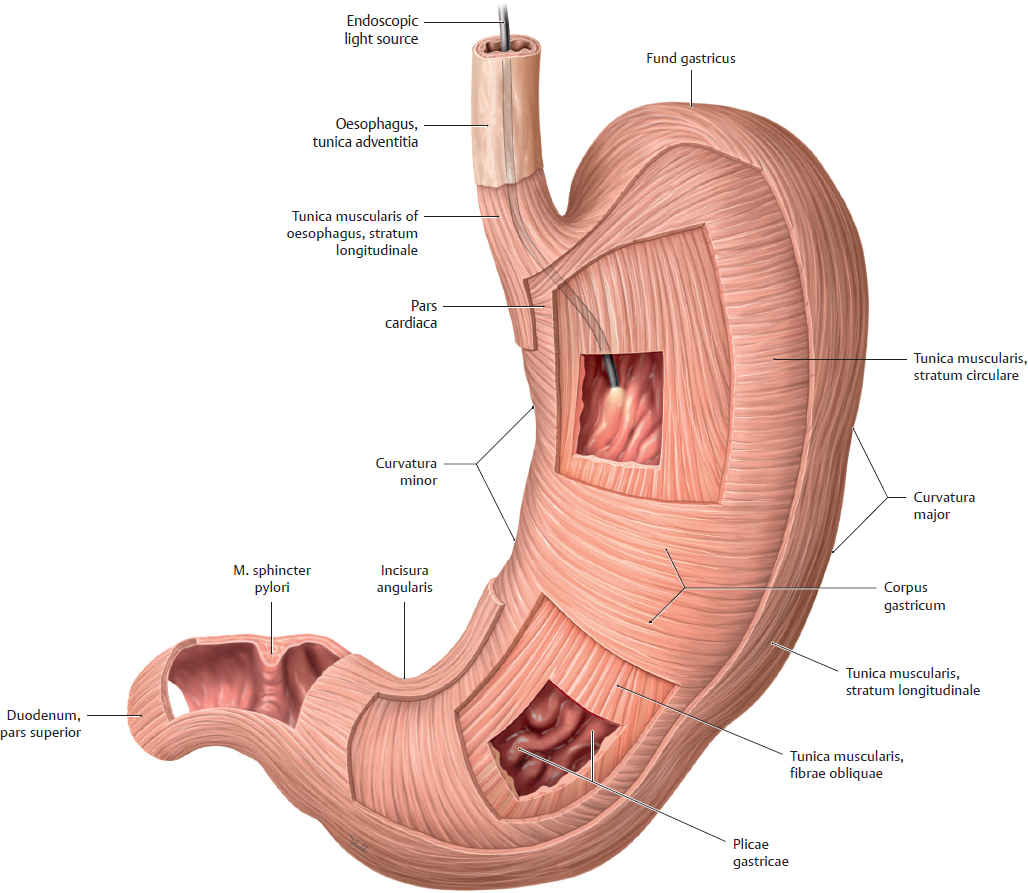
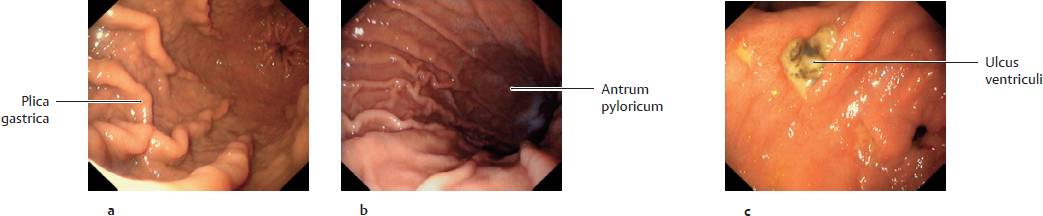
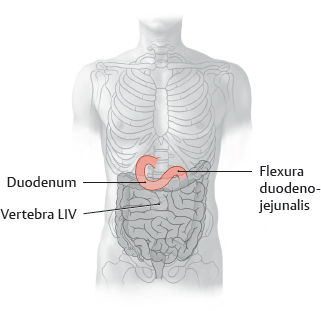
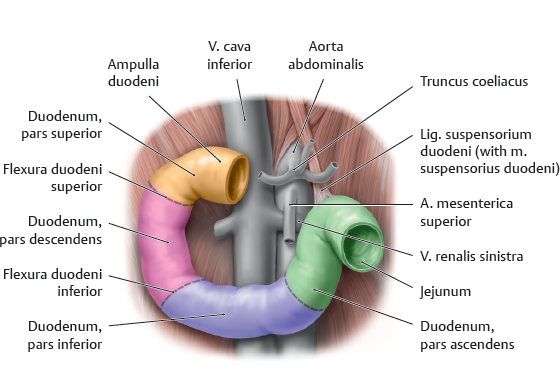
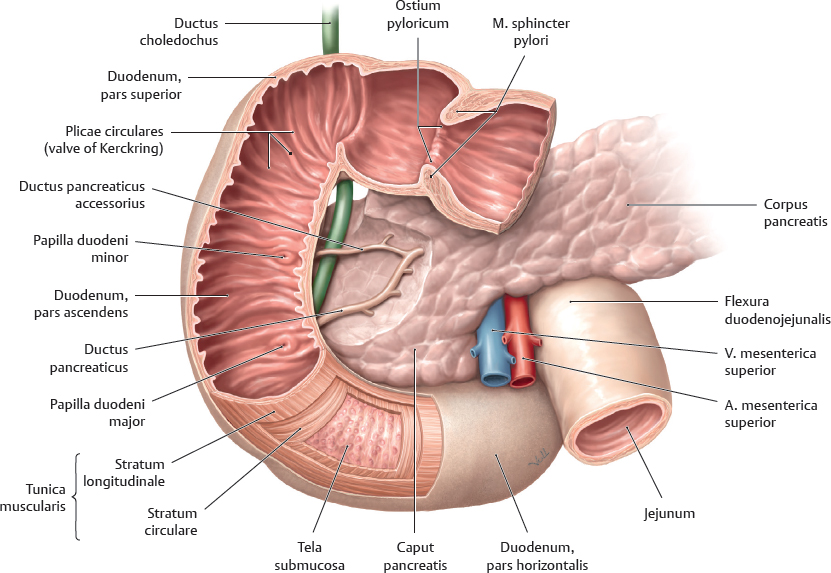
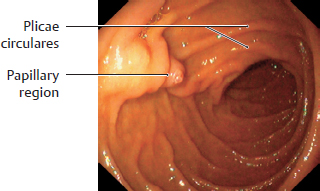
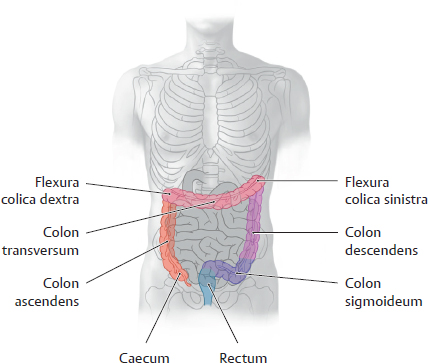
18. Organs of the Digestive System and their Neurovasculature A Projection onto the trunk Anterior view. The gaster is intraperitoneal and located in the left upper quadrant (epigastrium). Note the planum transpyloricum (halfway between the superior border of the symphysis pubica and superior border of the manubrium sterni, see p. 352). It serves as an important anatomical landmark: the pylorus is located at or slightly below the planum transpyloricum. Unlike other parts of the gaster, the pylorus hardly moves at all since it is connected to the duodenum, which is retroperitoneal (and thus relatively immobile). B Topographical relationships Transverse section at approximately the T 12/L 1 level. Viewed from above. Note the relationship of the gaster to the splen, pancreas, hepar, and bursa omentalis: The curvatura major extends to the splen; the lobus hepatis sinister extends in front of the gaster and into the left upper quadrant. When the abdomen is opened, very little of the gaster is visible as most of it is obscured by the hepar. Posterior to the gaster lies a narrow peritoneal space called the bursa omentalis. Its posterior wall is largely formed by the pancreas. Due to its peritoneal covering, the gaster is very mobile relative to the neighboring organs. This is important for facilitating the gaster’s peristaltic movements. Due to its embryonic placement in the mesogastrium ventrale and dorsale (see p. 32), the gaster has direct peritoneal attachments to the splen and hepar. C The gaster in situ Anterior view of the opened upper abdomen. The hepar has been retracted superolaterally, and the oesophagus has been pulled slightly downward for better exposure. The arrow points to the foramen omentale, the opening in the bursa omentalis behind the omentum minus. Peritoneal adhesions are visible between the hepar and the pars descendens duodeni. The omentum minus is visibly subdivided into a relatively thick lig. hepatoduodenale (transmitting neurovascular structures to the porta hepatis) and a thinner lig. hepatogastricum, which is attached to the curvatura minor of the gaster. A lig. hepatooesophageale can also be identified. The curvatura major of the gaster is closely related to the splen in the left upper quadrant (LUQ). The omentum majus is a duplication of peritoneum that covers the colon transversum and drapes over the loops of intestinum tenue (not visible here). D Shape and anatomical divisions Anterior view of the paries anterior. The body (corpus) of the gaster is the largest part of the gaster. It terminates blindly at the fundus gastricus, which in the standing patient is the highest part of the gaster and is usually filled with air (visible on radiographs as the “gastric bubble”). Note: The cardia is the area of the gastric inlet where the oesophagus opens into the gaster (at the ostium cardiacum). While the oesophagus is invested by adventitial connective tissue (tunica adventitia), the gaster has a visceral peritoneal covering or tunica serosa. The transition from tunica adventitia to tunica serosa is sharply defined, and occasionally the tunica serosa continues a short distance onto the lower end of the oesophagus. The part of the gaster that opens into the duodenum, the pars pylorica, consists of a broad antrum pyloricum, a narrow canalis pyloricus, and the pylorus itself (ostium pyloricum). The stratum circulare of the tunica muscularis of the gaster is markedly thickened at the end of the canalis pyloricus to form the m. sphincter pyloricus (not visible here), which produces a visible external constriction of the canalis pyloricus. E Interior of the gaster Anterior view of the gaster with the paries anterior removed. For clarity, small portions of the oesophagus and duodenum are also shown. The gastric tunica mucosa forms prominent folds (plicae gastricae) that serve to increase its surface area. These folds are directed longitudinally toward the pylorus, forming “canales gastrici”. The plicae gastricae are most prominent in the corpus gastricum and along the curvatura major and diminish in size toward the pyloric end. The tunica mucosa imparts a glossy sheen to the stomach lining. Note: The ostium pyloricum is quite large in this dissection. Normally, the orifice usually opens to a luminal diameter of only 2–3 mm. A Muscular layers Anterior view of the paries anterior gastricus with the tunica serosa and tela subserosa removed. The tunica muscularis of the gaster has been windowed at several sites. The entire stomach wall ranges from 3 mm to approximately 10 mm in thickness (see B for individual layers). Most of its tunica muscularis consists not of two layers (as in other hollow organs of the gastrointestinal tract) but of three muscular layers: • An outer stratum longitudinale, which is most pronounced along the curvatura major (greatest longitudinal expansion) • A middle stratum circulare, which is well developed in the corpus gastricum and most strongly developed in the canalis pyloricus (anular m. sphincter pyloricus, see p. 221) • An innermost layer of fibrae obliquae, which is derived from the stratum circulare and is clearly visible in the corpus gastricum. The three-layered structure of its muscular wall enables the gaster to undergo powerful churning movements. The muscles can forcefully propel solid food components against the gastric wall in the acidic gastric juice, breaking the material up into particles approximately 1 mm in size that can pass easily through the pylorus. The longitudinally- oriented plicae gastricae (reserve folds that disappear when the gaster is distended) form channels, called canales gastrici, that rapidly convey liquids from the gastric inlet to the pylorus. B Structure of the gaster wall and gll. gastricae a The structure of the gaster wall illustrates the layered wall structure that is typical of the hollow organs throughout the gastrointestinal tract. The gaster is unique, however, in that its tunica muscularis consists of three rather than two layers (see A). Note: The tunica serosa (visceral layer of the peritoneum) and tela subserosa (connective-tissue layer giving attachment to the tunica serosa and transmitting neurovascular structures for the tunica muscularis) are present only in areas where the organ in question is covered by peritoneum viscerale. In wall areas that lack a peritoneal covering (e.g., large portions of the duodenum and colon), the tunica serosa and tela subserosa are replaced by a fibrous tunica adventitia, which connects the wall of the organ to the connective tissue of surrounding structures. The tunica mucosa contains specialized cells that are aggregated into glandulae (visible microscopically). The glandular orifices open at the base of the foveolae gastricae (see b). In the corpus and pylorus of the gaster these glands extend down to the muscular layer of the mucosa, the lamina muscularis mucosae (deeper glands = more cells = higher secretory output). The tela submucosa (layer of connective tissue transmitting neurovascular structures for the tunica muscularis) contains the plexus submucosus for visceromotor and viscerosensory control of the hollow organs in the gastrointestinal tract. This plexus, like the plexus myentericus (located in the tunica mucosa for visceromotor control of the visceral muscle, not shown here), is part of the enteric nervous system (plexus entericus), which contains, in total, millions of scattered ganglion cells. b Structure of the gll. gastricae (after Lüllmann-Rauch) (simplified schematic of a gland from the corpus gastricum). Several types of cells are distinguished in the fundus and corpus gastricum: • Surface epithelial cells: cover the surface of the tunica mucosa and secrete a mucous film. • Neck cells: produce mucin to strengthen the mucous film (make it more anionic). • Parietal cells: produce HCl and intrinsic factor, which is necessary for vitamin B12 absorption in the ileum. • Chief cells: produce pepsinogen, which is converted to pepsin (for protein breakdown) in the stomach. • Enteroendocrine cells: different subtypes producing gastrin (G cells), somatostatin (D cells), or other factors controlling motility and secretion • Stem cells: reservoir for replenishing the surface epithelial cells and gland cells C Endoscopic appearance of the gastric tunica mucosa a, b Healthy gastric tunica mucosa with a glistening surface; c Gastric ulcer. a View into the corpus gastricum, which has been moderately distended by air insufflation. The tunica mucosa is raised into prominent, tortuous plicae gastricae that form the canales gastrici. b Inspection of the antrum pyloricum shows less prominent folds than in the corpus gastricum. c Fibrin-covered gastric ulcer with hematin spots. A gastric ulcer is defined as a tissue defect that extends at least into the lamina muscularis mucosae, but many ulcers extend much deeper into the stomach wall. Most gastric ulcers are caused by infection with Helicobacter pylori, a bacterium that is resistant to stomach acid (from Block, Schachschal and Schmidt: The Gastroscopy Trainer. Stuttgart: Thieme, 2004). A Projected onto the columna vertebralis The duodenum is a C-shaped loop of intestinum tenue lying predominantly on the right side of the columna vertebralis in the right upper quadrant (RUQ) and encompassing the L 1 through L 3 vertebrae and occasionally extending to L 4. The concavity of the duodenum normally encloses the caput pancreatis at the L 2 level (see D). B Parts of the duodenum Anterior view. The anatomical parts of the duodenum (partes superior, descendens, horizontalis, and ascendens with intervening flexures) have a total length of approximately 12 fingerwidths (L. duodeni = “twelve at a time”). Note the lig. suspensorium duodeni (called also the ligament of Treitz), which often contains smooth-muscle fibers. Mobile loops of intestinum tenue may wrap around this ligament and become entrapped between the ligament and the vessels behind it (most notably the pars abdominalis aortae). This “Treitz hernia” may cause mechanical obstruction of the affected bowel loop and strangulate its blood supply. C Wall structure and duct orifices Anterior view. Most of the duodenum has been opened. The ostium pyloricum (here greatly dilated) opens to a luminal diameter of only about 2–3 mm for the passage of chyme. The duodenum has basically the same wall structure as the other hollow organs of the gastrointestinal tract (see B, p. 223). The structure of the tunica mucosa is shown in F. The pars descendens of the duodenum has two small elevations along its inner curve: the papilla duodeni minor, which bears the orifice of the ductus pancreaticus accessorius, and the papilla duodeni major (called also the papilla of Vater), which has a common orifice for the ductus pancreaticus and ductus choledochus. Thus, the release of bile and pancreatic juice to aid digestion takes place in the upper part of the duodenum. D The duodenum in situ Anterior view. The gaster, hepar, intestinum tenue, and large portions of the colon transversum have been removed. The retroperitoneal fat and connective tissue, including the capsula adiposa, have been substantially thinned. The caput pancreatis lies in the concavity of the C-shaped loop of the duodenum. The first 2 cm of the pars superior of the duodenum is still intraperitoneal (attached to the hepar by the lig. hepatoduodenale), but most of the duodenum is retroperitoneal. Owing largely to the proximity of the duodenum and the caput pancreatis, lesions of the pancreas (tumors) or malformations (anular pancreas) may cause duodenal obstruction. The peritoneum at the duodeno-jejunal junction forms the recessus duodenales superior and inferior. Mobile loops of intestinum tenue may enter these peritoneal recesses and become entrapped there (internal hernia), causing a potentially life-threatening bowel obstruction. E Endoscopic view The endoscope is pointing down into the pars descendens of the duodenum. The papillary region where the ductus biliaris and ductus pancreaticus open into the duodenum is visible on the left side of the image at approximately the 10 o’clock position. The plicae circulares (valves of Kerckring) are typical of those found in the intestinum tenue, diminishing in size in the proximal to distal direction (from Block, Schachschal and Schmidt: Endoscopy of the Upper G I Tract. Stuttgart: Thieme, 2004). F Histological structure Longitudinal section through the duodenal wall. The duodenum has basically the same histological structure as the other hollow organs of the gastrointestinal tract (see B, p. 223), with some notable differences such as the presence of gll. duodenales (Brunner) (secrete mucins and bicarbonate to neutralize the acidic gastric juice) and valves of Kerckring (specialized plicae circulares). Other features that distinguish the duodenum from the jejunum and ileum are its more prominent mucosal folds, which diminish in size toward the end of the intestinum tenue. Note: The tunica muscularis externa of all portions of the intestinum, unlike that of the gaster, consists of only two layers: an inner stratum circulare and an outer stratum longitudinale. A Parts of the intestinum tenue: overview (a) and anatomical constrictions (b) Anterior view. The intestinum crassum surrounds the loops of intestinum tenue like a frame. Because the intestinum tenue loops are intraperitoneal and therefore very mobile, it is not possible to define their location by reference to skeletal landmarks. If the intestinal loop rotates normally during embryonic development (see p. 36), the duodenum lies behind the colon transversum. If the intestinal loop rotates in the wrong direction, the duodenum will come to lie in front of the colon transversum. Note the following normal anatomical constrictions: • Junction of the pylorus and duodenum (luminal diameter of the ostium pyloricum is only about 2–3 mm) • Flexura duodenojejunalis • Ostum ileale Swallowed foreign bodies may become lodged at these sites, obstructing intestinal transit and causing mechanical intestinal paralysis (mechanical ileus, a life-threatening condition that is an absolute indication for surgical treatment). B Wall structure of the jejunum and ileum The wall layers of the intestinum tenue are displayed in a “telescoped” cross-section. The tunica mucosa has been incised longitudinally and opened. The jejunum and ileum have basically the same wall structure as the other hollow organs of the gastrointestinal tract (see B, p. 223), but local differences are observed in the plicae circulares (see C) and vascular supply (see p. 260). C Differences in the wall structure of the jejunum and ileum Macroscopic views of the jejunum (a) and ileum (b), which have been opened longitudinally to display their mucosal surface anatomy. Note: The transversely oriented plicae circulares in the jejunum are spaced much closer together than in the ileum. Lymphatic follicles are particularly abundant in the wall of the ileum (from the lamina propria to the tela submucosa) for mounting an immune response to antigens in the intestinal contents (noduli lymphoidei aggregati, Peyer’s patches). D The jejunum and ileum in situ Anterior view. The abdominal wall has been opened and the colon transversum has been reflected upward. Coils of jejunum and ileum completely fill the four quadrants of the cavitas peritonealis below the mesocolon transversum and are framed by the colon segments. In this dissection the loops of intestinum tenue have been displaced slightly to the left in front of the colon descendens, hiding it from view. The colon ascendens and caecum are visible along the right flank of the abdomen. A Projection of the intestinum crassum onto the skeleton Because of the embryonic rotation of the primary intestinal (midgut) loop, the intestinum crassum typically forms a frame encompassing the intestinum tenue. The position and length of the colon segments may vary, however, depending on the course of intestinal rotation. For example, when the intestinal loop rotates normally, the colon ascendens acquires a “normal” length (as shown here). If intestinal rotation is incomplete, the colon ascendens is shortened. The colon transversum is particularly mobile owing to its mesocolon, while the cola ascendens and descendens are less mobile because they are fixed to the posterior wall of the cavitas peritonealis. The flexura coli sinistra usually occupies a somewhat higher level than the flexura coli dextra due to the space occupied by the large lobus hepatis dexter. Also, the colon descendens is usually more posterior than the colon ascendens. B Distinctive morphological features of the intestinum crassum There are four morphological features—three visible externally and one internally—that distinguish the intestinum crassum from the intestinum tenue. It should be noted that these features do not occur equally in all parts of the intestinum crassum and are absent in the caecum, appendix vermiformis, and rectum.
18.1 Gaster: Location, Shape, Divisions, and Interior View
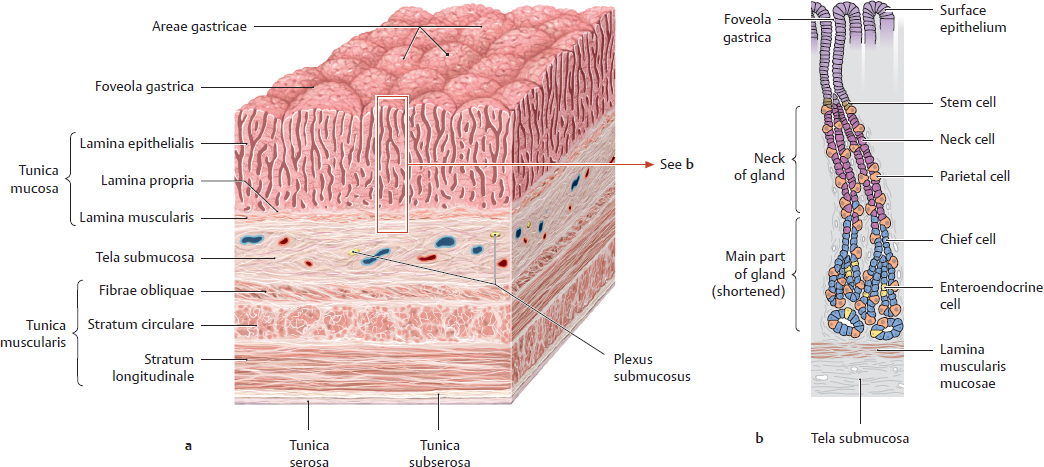
18.2 Gaster: Wall Structure and Histology
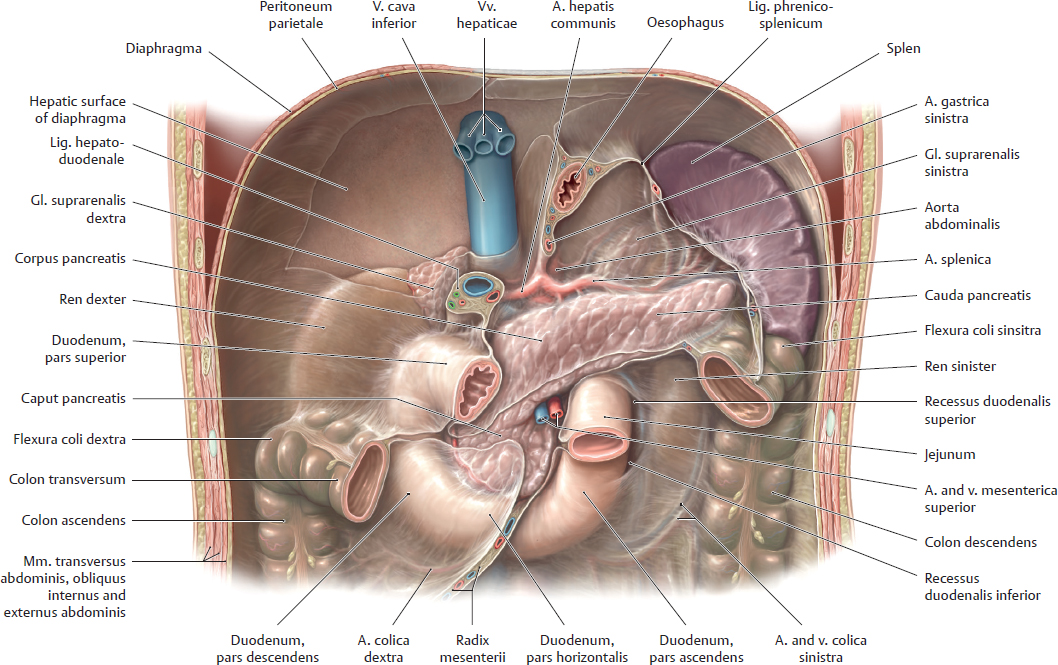
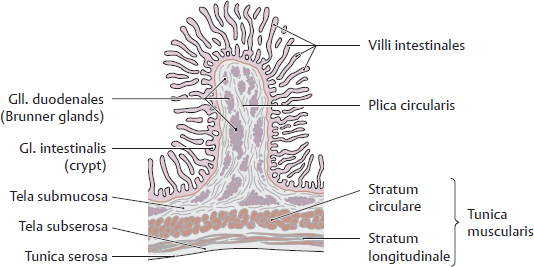
18.3 Intestinum Tenue: Duodenum
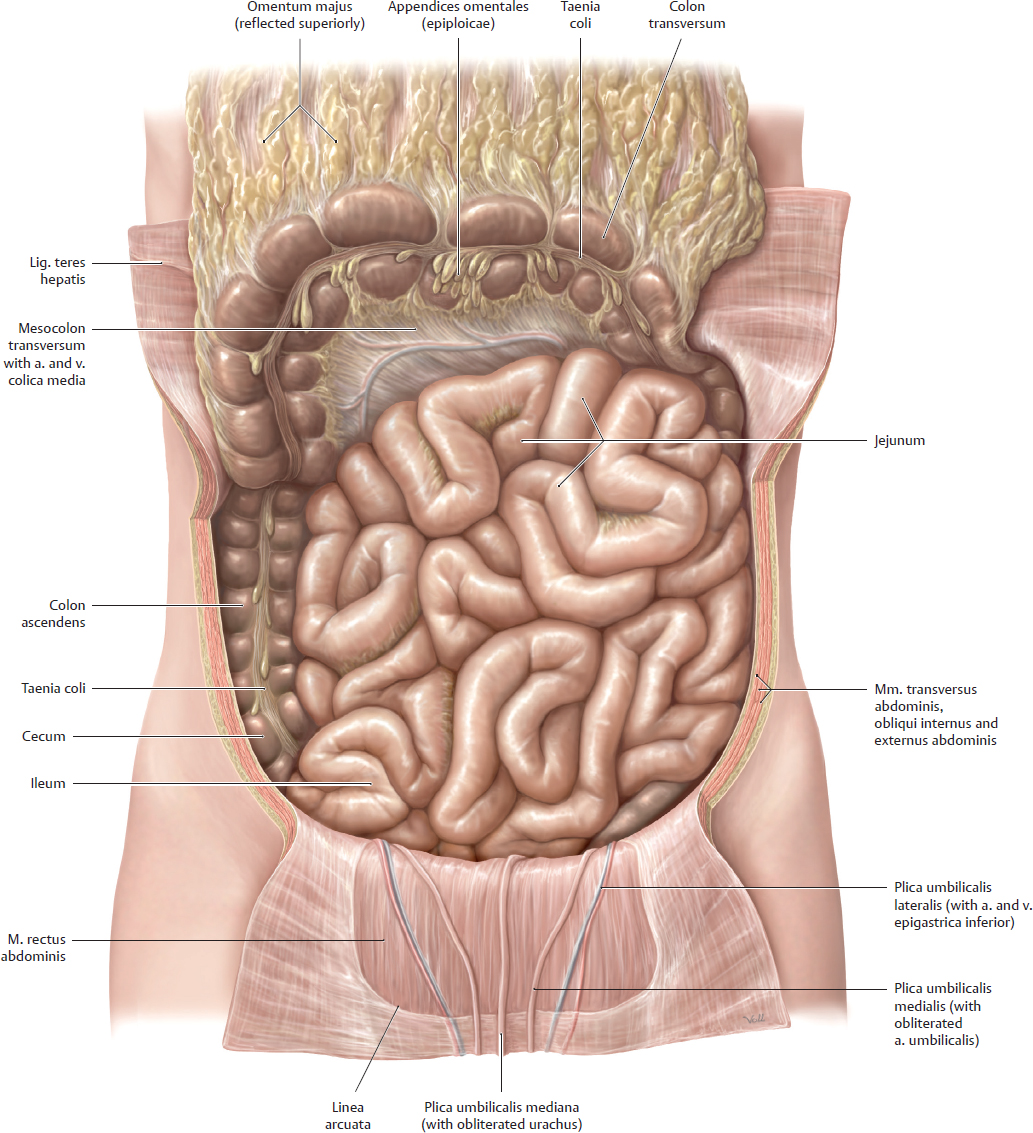
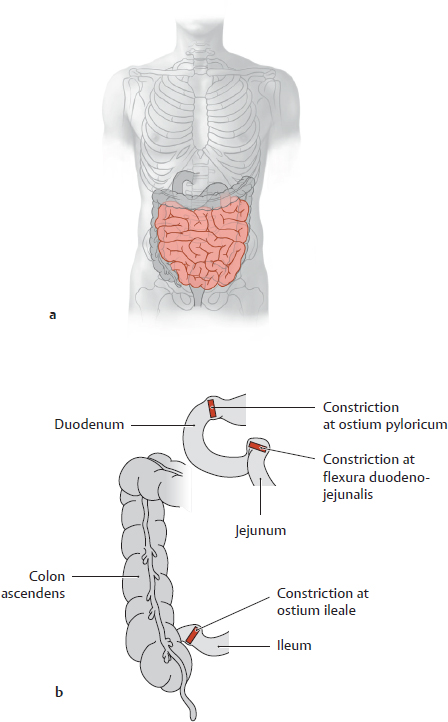
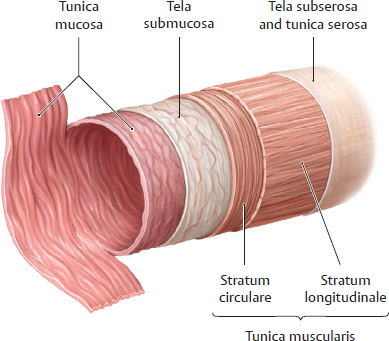
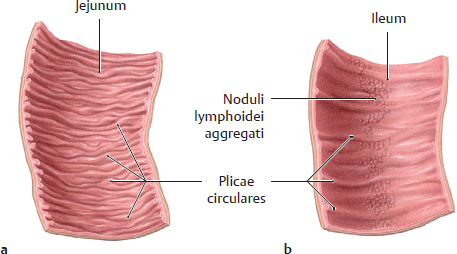
18.4 Intestinum Tenue: Jejunum and Ileum
18.5 Intestinum Crassum: Colon Segments
Taeniae coli | In most portions of the intestinum crassum, the longitudinal muscle fibers do not form a continuous layer around the intestinal wall but are concentrated to form three longitudinal bands, the taeniae (see C). Taeniae are not present in the rectum or appendix vermiformis. The three taeniae converge to form the muscularis externa of the appendix. |
Appendices epiploicae | Fat-filled protrusions of the tunica serosa, scattered over the surface of the intestinum crassum except on the caecum (absent or sparse) and rectum (absent). |
Haustra (haustrations) | Saccular wall protrusions between the transverse folds of the intestinum crassum (see p. 230), absent in the rectum. |
Plicae semilunares coli | Visible only internally, in contrast to the external features above. They are functional features caused by contraction of the tunica muscularis. The internal plicae correspond to external constrictions that separate the haustra. |
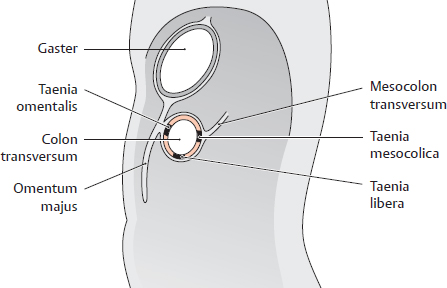
C The three taeniae of the colon
Sagittal section, viewed from the left side. The three taeniae are named for their position on the colon:
• Taenia libera (free taenia)
• Taenia omentalis (the taenia at the attachment of the omentum majus)
• Taenia mesocolica (the taenia at the attachment of the mesocolon)
D Anatomical divisions of the intestinum crassum
The intestinum crassum consists of the following divisions in the proximal-to-distal direction:
• Caecum with the appendix vermiformis
• Colon, consisting of four parts:
– Colon ascendens
– Colon transversum
– Colon descendens
– Colon sigmoideum
• Rectum
Note: For various reasons, some authors consider the rectum to be a separate section of the intestine, and not a part of the intestinum crassum. However, according to the Terminologia Anatomica, which serves as the international standard on human anatomic terminology, the rectum is a segment of the intestinum crassum.
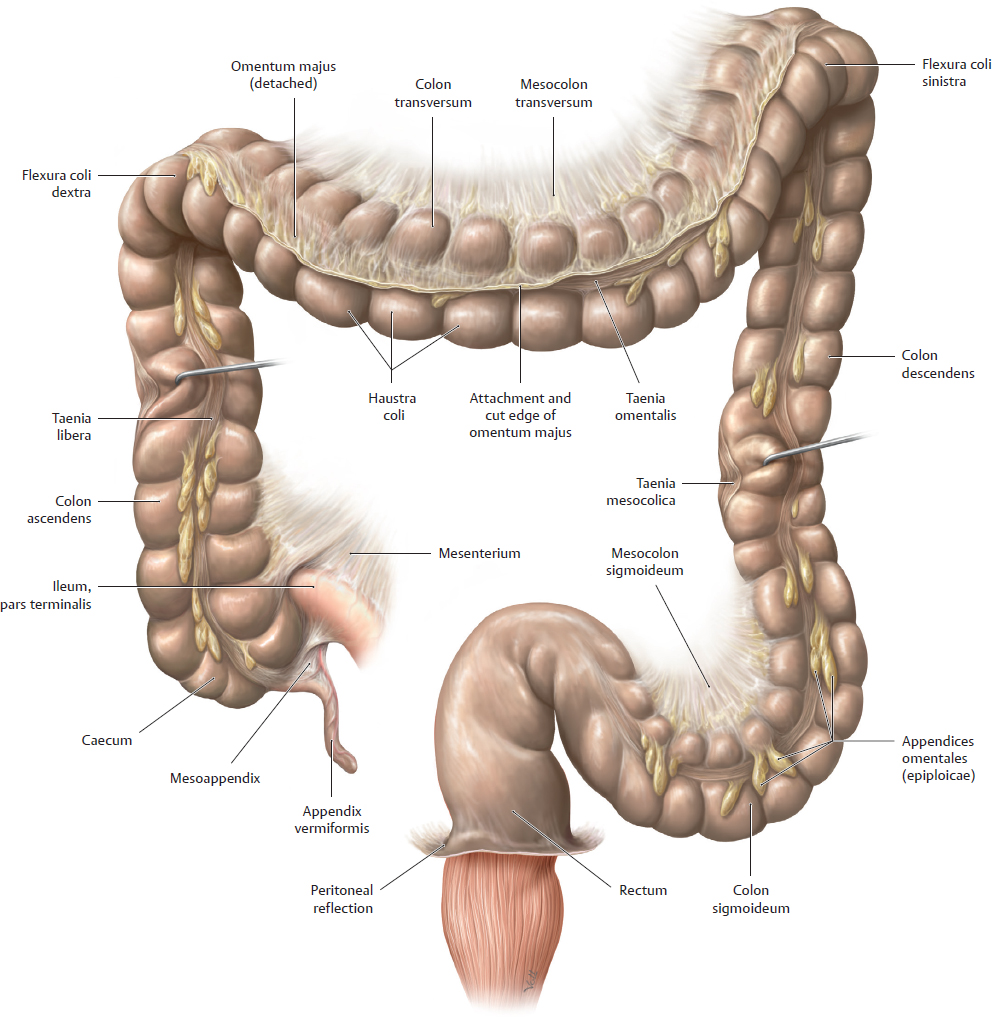
E Intestinum crassum: Segments, shape, and distinctive features
Anterior view, intestinum crassum. The pars terminalis of the ileum and portions of the mesocola transversum and sigmoideum are shown. The cola ascendens and transversum have been rotated to display their taeniae.
Note: Colorectal cancer, which has become one of the most common cancers in industrialized countries, has a special predilection for the rectosigmoid junction and the rectum itself (i.e., sites distal to the flexura coli sinistra).
The various colon segments possess all the morphological characteristics of the intestinum crassum (haustra, taeniae, appendices epiploicae, see B). Typically these features disappear past the rectosigmoid junction. As the taeniae disappear, they are replaced on the rectum by a continuous stratum longitudinale. Instead of haustra, the rectum has three permanent constrictions that are produced by internal plicae transversae (see p. 233). The peritoneal reflection on the anterior rectal wall represents the site where the peritoneum is reflected onto the posterior wall of the uterus (in the female) or onto the upper surface of the vesica urinaria (in the male).
Note: The cola ascendens and descendens are (secondarily) retroperitoneal and therefore, unlike the cola sigmoideum and transversum, they do not have a mesocolon and are covered only anteriorly by peritoneum. The rectum is extraperitoneal in the pelvis minor, lacks a “suspensory ligament,” and bears other unique features.
18.6 Intestinum Crassum: Wall Structure, Caecum, and Appendix Vermiformis
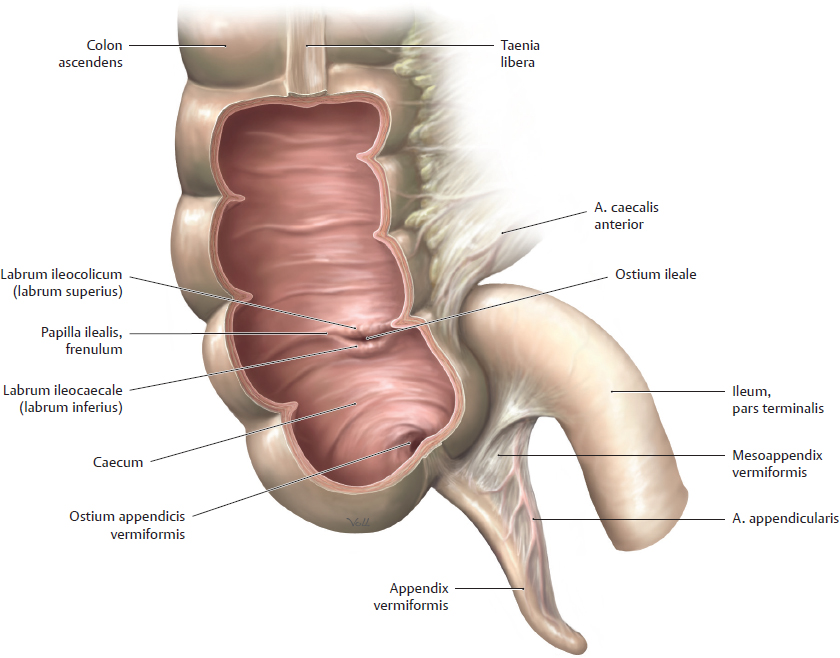
A Caecum and pars terminalis ilei
Anterior view. The caecum is unique in its end-to-side connection with the pars terminalis of the intestinum tenue (ileum) and the presence of the appendix vermiformis. As a result, there are two openings in the wall of the caecum: the ostium ileale on a small papilla (papilla ilealis) and, below that, the ostium appendicis vermiformis. The ostium ileale is approximately round in the living individual but is often slit-like in the postmortem condition. It is bounded by superior and inferior flaps or “lips,” the labrum ileocolicum (labrum superius) and the labrum ileocaecale (labrum inferius). Both are continued as a narrow ridge of mucosa, the frenulum ostii ilealis.
Note: Inflammation of the appendix vermiformis (appendicitis) is one of the most common surgically treated diseases of the gastrointestinal tract. If acute appendicitis goes untreated, the inflammation may perforate into the free cavitas peritonealis (a “ruptured appendix” in popular jargon). This creates a route by which bacteria in the bowel lumen can enter the cavitas peritonealis and gain access to the large peritoneal surface, quickly inciting a life-threatening inflammation of the peritoneum (peritonitis).
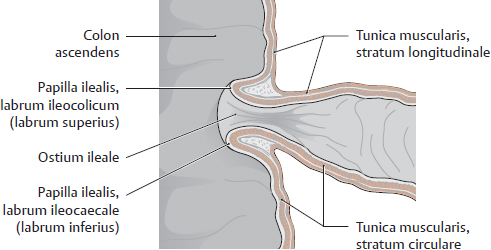
B Ostium ilealis
Anterior view of a longitudinal coronal section of the cecum and ileum. The ostium ilealis hermetically seals the pars terminalis ilei from the caecum and prevents the reflux of contents from the intestinum crassum (structural constriction, see A, p. 226). At the ostium ilealis, the end of the ileum evaginates the stratum circulare of the tunica muscularis of the intestinum crassum into the cecal lumen. All layers of the ileal wall except the stratum longitudinale of the tunica muscularis and peritoneum contribute to the structure of the ileocecal orifice. The strata circulares tunicarum muscularium of the ileum and caecum function as a sphincter, which periodically opens the ostium. This allows the contents of the intestinum tenue to enter the intestinum crassum while effectively preventing reflux. The function of the sphincter is similar to that of the pylorus.
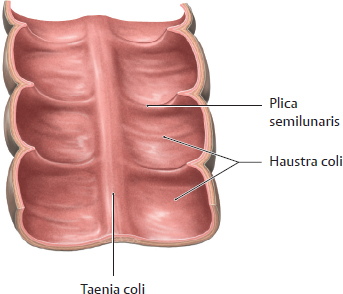
C Interior of the colon
The interior of the colon is marked by transversely oriented folds called plicae semilunares. They are formed by the shortness of the muscular taenia of the colon wall and are visible externally as anular constrictions. The sacculations between the folds are the haustra coli. The plicae semilunares are inconstant features that depend on the muscular tension in the taenia. The plicae and haustra move slowly down the colon with waves of peristaltic activity.
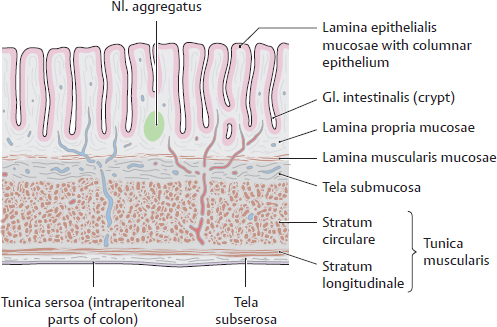
D Wall structure of the colon and caecum
Longitudinal section through the bowel wall. All the typical wall layers of the gastrointestinal canal are present: the tunica mucosa, tela submucosa, tunica muscularis externa, and tunica serosa (or adventitia in the retroperitoneal parts of the colon, see B, p. 223). There are several features, however, that distinguish the wall structure of the colon and caecum from that of the gaster and intestinum tenue:
• The tunica mucosa is devoid of villi (i.e., the total surface area is not enlarged as much as in the intestinum tenue). Instead of villi, there are large numbers of deep crypts (Lieberkühn crypts, glandulae intestinales), more numerous than in the intestinum tenue.
• The epithelial layer of the tunica mucosa contains large numbers of goblet cells (for clarity, not shown here).
• The colonic mucosal surface undulates in large-scale, crescent-shaped, plicae semilunares (see C).
• The tunica muscularis externa consists of an inner stratum circulare and an outer stratum longitudinale, which is concentrated in three longitudinal bands, the taeniae coli (see p.228).
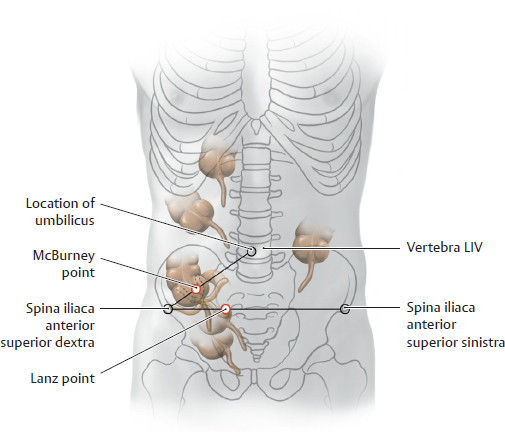
E Variants in the position of the appendix vermiformis
Disturbances in the rotation of the embryonic gut can result in numerous positional variants of the caecum and appendix vermiformis. The appendix may even come to lie in the left side of the abdomen. The inflammation of an appendix in the typical position is characterized by tenderness at two points:
• McBurney point: Position on a line connecting the umbilicus and the right spina iliaca anterior superior. The McBurney point is one-third of the distance along this line from the spina iliaca.
• Lanz point: Position on a line connecting the the spinae iliacae anteriores superiores. The Lanz point is one third of the distance along this line from the right spina.
Although very useful, these are not definitive clinical signs. Tenderness may be felt at other abdominal sites, especially if the appendix is in an atypical position.
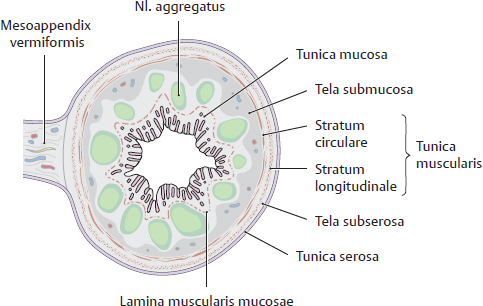
F Wall structure of the appendix vermiformis
The appendix vermiformis has the typical wall structure of an intraperitoneal intestinal tube. One striking feature is the abundance of lymphatic follicles (noduli lymphoidei aggregati) in the tela submucosa (also present in the colon and caecum, but in much smaller numbers). With its high degree of immunological activity, the appendix has been characterized as the “intestinal tonsil.” The mucosa has numerous deep crypts that are in intimate contact with the noduli lymphoidei aggregati in the lamina propria and the tela submucosa (crypts and noduli lymphoidei aggregati are not visible here). Since the appendix vermiformis is intraperitoneal, it possesses a small mesenterium, the mesoappendix, which transmits neurovascular structures.
18.7 Intestinum Crassum: Location, Shape, and Interior View of Rectum
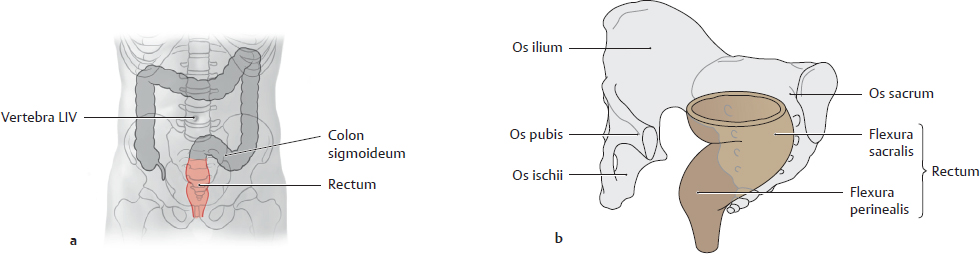
A Location and curves of the rectum
Anterior view (a) and left anterior view (b). The rectum is 15–16 cm long and extends approximately from the superior border of the third sacral vertebra to the perineum. It is “straight” only in the frontal projection (as shown in a); it presents two flexures in the sagittal projection (see b): the flexura sacralis (retroperitoneal) and the flexura perinealis (extraperitoneal), which represents the start of the canalis analis and is already extraperitoneal. The flexura sacralis—conforming to the shape of the os sacrum—is concave anteriorly. The flexura perinealis is an important functional component of rectal continence (see p. 234f).
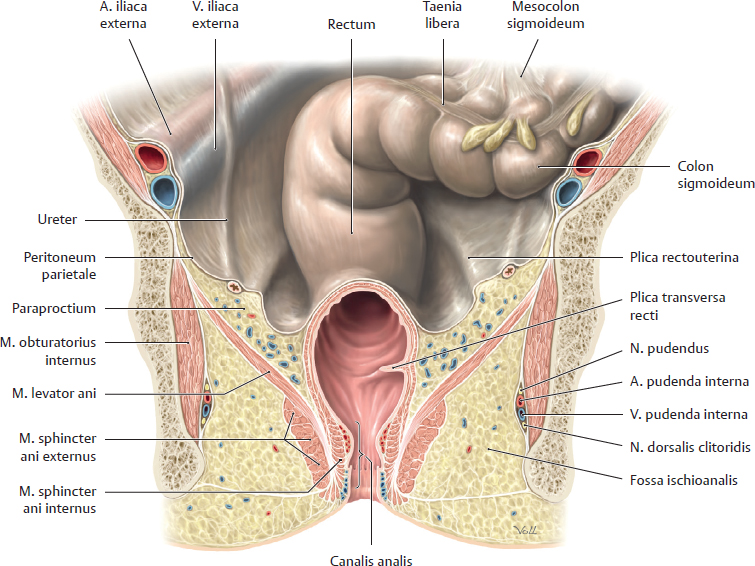
B The rectum in situ
Coronal section of the female pelvis, anterior view, with the rectum opened from about the level of the middle plica transversa recti. The taeniae of the colon sigmoideum are not continued onto the rectum. The constrictions in the outer wall of the rectum correspond to the plicae transversae on the inner wall. The rectum (which would appear in this form only if the ampulla were full) is shown in a slightly raised position. Below the m. levator ani is the powerful m. sphincter ani externa, the muscular component of the rectal continence organ. The pararectal connective tissue below the cavitas peritonealis contains numerous vessels that supply the rectum.
This drawing was made from the dissection of a female cadaver. Thus, the peritoneum would be reflected from the anterior wall of the rectum onto the posterior wall of the uterus. Although both the anterior rectal wall and uterus are not visible here (anterior to this plane of section), parts of the plicae rectouterinae are still visible.
C Distinct morphological features of the rectum
The mucosa and wall structure of the rectum does not differ from the intestinum crassum, including the colon and caecum. Nevertheless, it lacks several colonic characteristics:
• no taeniae, the rectum has a continuous stratum longitudinale tunicae muscularis;
• no appendices epiploicae;
• no haustra;
• no plicae semilunares, the rectum has plicae transversae recti
• the wall of rectum is devoid of ganglion cells;
• embryonic development: the part above the anorectal line, like the colon, is derived from endoderma, the canalis analis is derived from ectoderm (which is why some authors don’t consider it part of the rectum).
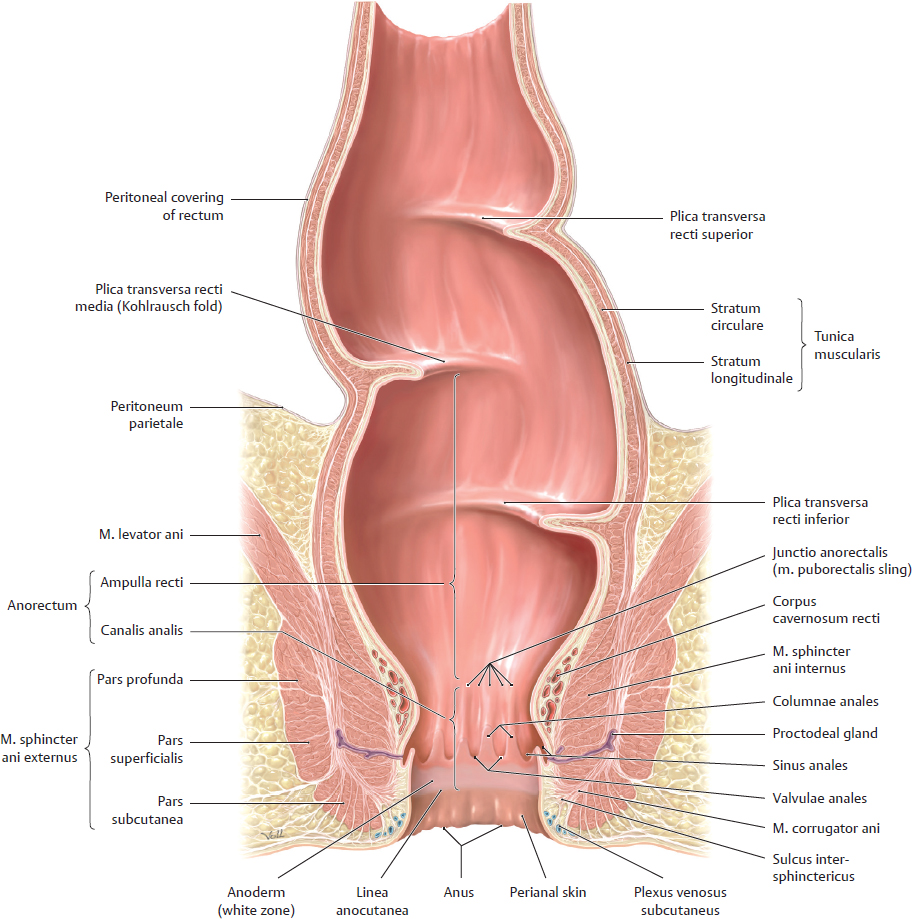
D Rectum and canalis analis: Divisions, internal surface and wall structure
Anterior view of the rectum in coronal section with the anterior wall removed. Instead of plicae semilunares, the rectum contains three permanent plicae transversae. The distal portion of the rectum, also known as the anorectum, is recognizable by a palpable protrusion (m. puborectalis sling or junctio anorectalis) which is visible on the mucosal surface. The anorectum is divided into two segments, the ampulla recti and the canalis analis.
• Ampulla recti: the lowest portion of the rectum between the middle plica transversa recti (Kohlrausch fold, flexura intermediosinistra lateralis) and the junctio anorectalis. The ampulla recti is the most distensible part of the rectum and, contrary to popular opinion, does not serve as a reservoir for holding stool but is usually empty (see mechanism of defecation, p. 237). The middle plica transversa, which projects into the rectum from its right posterior wall, is approximately 6–7 cm from the anus and can just be reached with the palpating finger. Rectal tumors located below the Kohlrausch fold may therefore be palpable.
• Canalis analis: located below the junctio anorectalis at the distal flexura perinealis (see A). It is approximately 4 cm long and normally kept closed by the mm. sphincteres ani. The clinically important “surgical anal canal” begins at the level of the junctio anorectalis and extends to the linea anocutanea, which is also palpable. It is a groove located between the margins of the mm. sphincteres ani internus and externus (sulcus intersphinctericus) at the junction of the anoderm (zona alba), a region with very dense somatic innervation, and the pigmented perianal skin (see p. 234 B). Above the anoderm are located 8–10 longitudinal mucosal folds (columnae anales), produced by the arterial corpus cavernosum recti (hemorrhoidal plexus), located in the submucosa (see p. 234). The distal ends of the columnae anales are connected by valve-like transverse folds (valvulae anales). All valvulae anales together form the linea pectinata, which is an important landmark because it is visible. Behind the valvulae anales are pocket-like depressions (sinus anales or pouches of Morgagni), into which empty 6–8 outflow ducts of the rudimentary mucus-secreting anal glands (proctodeal glands). The most common site of these glands is the commissura laborium posterior (approximately at 6 o’clock in the lithotomy position), either in the tela submucosa or intersphincteric (between the mm. sphincteres ani interni and externi) space, so that the outflow ducts partially transverse the m. sphincter ani internus.
Note: Bacterial infections of the glands may cause perianal abscesses and anal fistulas, which are difficult to treat (see p. 239).
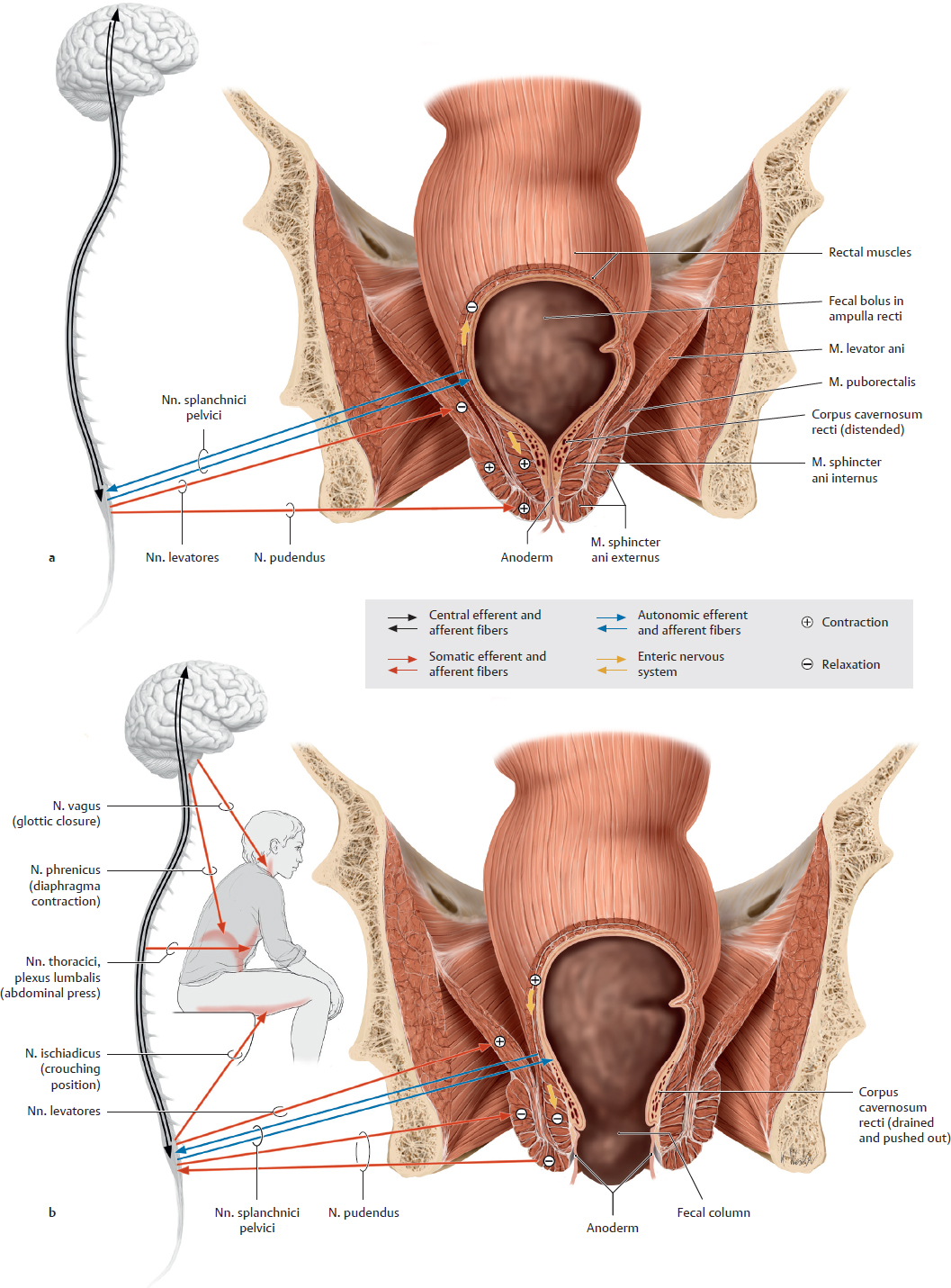
18.8 Continence Organ: Structure and Components
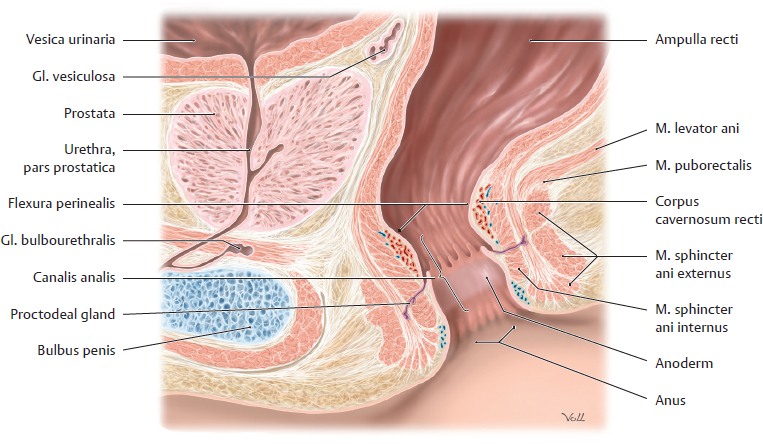
A Components of the continence apparatus
Midsagittal section at the level of the canalis analis in the male, viewed from the left side.
The continence apparatus, or continence organ, controls the closing (continence) and opening (defecation) of the rectum and provides a tight closure before and after evacuation of solid, liquid and gas bowel contents.
It consists of a distensible hollow organ as well as vascular and muscular continence mechanisms, including their neural control. These angiomuscular continence mechanisms are integrated into a structurally narrow segment, which begins at the level of the flexura perinealis and continues along the canalis analis:
• Distensible hollow organ:
– rectum with stretch receptors, mainly in the ampulla recti (viscerosensory innervation)
– anus with distensible skin in the canalis analis (somatosensory innervation);
• Muscular continence:
– m. sphincter ani internus (visceromotor innervation)
– m. sphincter ani externi (somatomotor innervation)
– m. levator ani, especially the m. puborectalis (somatomotor innervation);
• Vascular continence:
– hemorrhoidal plexus (permanently distended cavernous tissue that subsides only during defecation);
• Neural control:
– visceral and somatic nervous system (mainly from S2–S4) with the nn. splanchnici pelvici, n. pudendus and plexus rectales.
Functionally, both continence and defecation are the result of a finetuned feedback loop between receptors and effectors of the continence apparatus with involvement of the central nervous system (see p. 236 f).
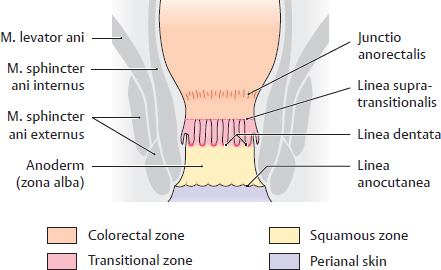
B Epithelial regions of the canalis analis (after Lüllmann-Rauch)
In the canalis analis, the unilayered columnar epithelium of the colorectal tunica mucosa at the level of the zona transitionalis analis is continuous with the stratified squamous epithelium of the anoderm and perianal skin. The transition occurs near characteristic landmarks. The canalis analis can be divided into the following epithelial regions:
• colorectal zone between junctio anorectalis and supratransitional line; homogeneous colorectal mucosa with crypts;
• zona transitionalis at the level of the columnae anales (between supratransitional line and linea pectinata) mosaic patterns of colorectal mucosa, unilayered columnar epithelium and stratified squamous epithelium;
• squamous zone between linea pectinata and linea anocutanea: evenly covered by stratified, nonkeratinized squamous epithelium, which is intimately attached to the underlying m. sphincter ani internus, hence its whitish appearance (white zone). Deep sensory innervation with touch, pressure, temperature and mainly pain receptors (clinically: anoderm);
• perianal skin below the linea anocutanea: start of the stratified squamous epithelium of the outer layer of the skin (heavy pigmentation, eccrine and apocrine sweat glands and hair follicles).
Note: Knowledge about the epithelial regions of the canalis analis is important mainly for the differentiation between rectal (usually adenocarcinoma) and anal carcinoma (of keratinizing or non-keratinizing squamous epithelium).
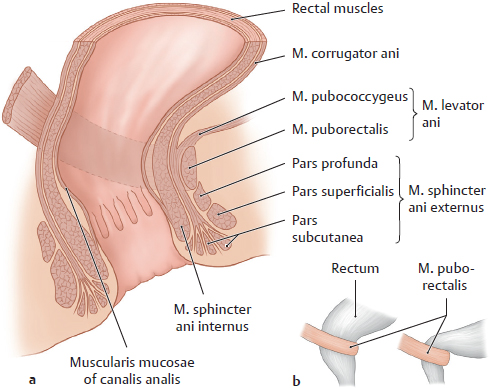
C Structure of the muscular continence mechanism
a Midsagittal section, viewed from the left side; b M. puborectalis sling and anorectal angle: relaxed muscle (left) and contracted muscle (right).
The complex system of anal sphincters involves both smooth and striated muscles. Whereas the smooth muscles represent the direct continuation of the muscles of the rectal wall, the striated muscles are formed by specialized areas of the pelvic floor muscles. Thus, these muscular continence mechanisms are maintained under both somatic-voluntary and visceral-involuntary control.
Involuntarily innervated smooth muscles:
• M. sphincter ani internus: most significant smooth muscle; as the continuation of the stratum circulare tunicae muscularis of the rectum, it forms a strong circular ring. Sympathetic nerve fibers and the absence of enteric ganglion cells (aganglionosis) allow it to maintain constant tonic activity to help constrict the canalis analis (the internal sphincter is responsible for 70% of fecal continence);
• Lamina muscularis mucosae of the canalis analis: as the continuation of the lamina muscularis mucosae, it extends beyond the hemorrhoidal plexus and ends at the linea pectinata; stabilizes the hemorrhoidal plexus and holds it in place;
• Corrugator ani: as the continuation of the stratum longitudinale of the tunica muscularis of the rectum, the muscle fibers extend beyond the canalis analis, permeate through the subcutaneous part of the m. sphincter ani externus and insert into the perianal skin. M. corrugator ani owes its name to the fact that muscle contraction produces radial wrinkles on the perianal skin.
Voluntarily innervated striated muscles:
• M. sphincter ani externus: cylindrical muscle that encircles the outside wall of the canalis analis, made up of three recognizable parts: partes profunda, superficialis, and subcutanea. Whereas the partes profunda and subcutanea are arranged in circular layers, the pars superficialis extends between the anteriorly located corpus perineale and the posterior lig. anococcygeum and surrounds the canalis analis and serves as a clamp. It is largely composed of type I fibers, which are slow, durable, and fatigue resistant.
• M. puborectalis: as the innermost portion of the m. levator ani, it forms a strong sling of muscle, which loops around the rectum at the level of the junctio anorectalis and is closely aligned to the pars profunda of the m. sphincter ani externus. It arises from the fixed end of the os pubis, so when the m. puborectalis contracts it creates a “kink” between canalis analis and rectum at the anorectal angle.
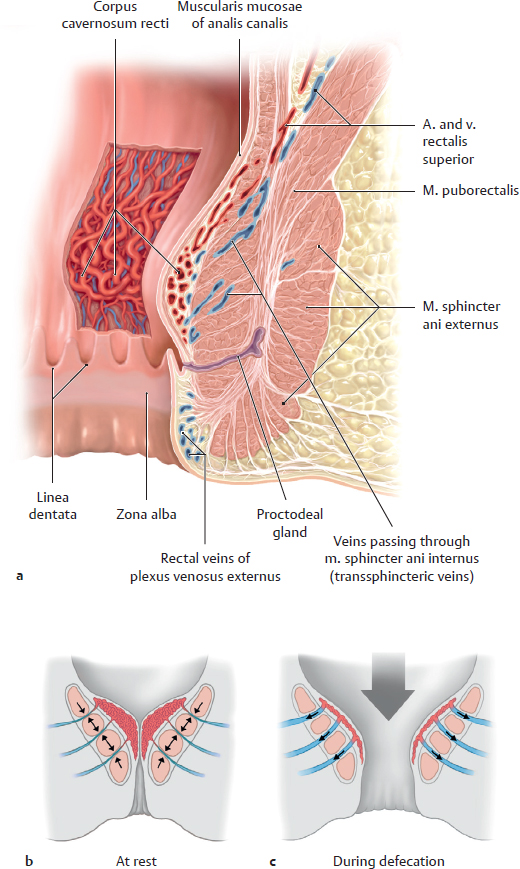
D Structure of the vascular continence mechanism
a Longitudinal section of the canalis analis with the hemorrhoidal plexus windowed; b and c Hemorrhoidal plexus at rest and during defecation. Above the linea pectinata at the level of the columnae anales in the submucosa lies a cavernous body, the hemorrhoidal plexus. Its elasticity largely ensures liquid- and gas-tight closure of the rectum. The circular configuration of the hemorrhoidal plexus is similar in structure to the corpus cavernosum penis but differs in that it is permanently distended. The hemorrhoidal plexus is a network of cavernous tissue and is almost exclusively supplied by three branches of the a. rectalis superior (at 3, 7 and 11 o’clock in the lithotomy position), which further divide near the columnae anales (see p. 265). Blood reaches the venous drainage system via arteriovenous anastomoses through transsphincteric veins—largely along the m. sphincter ani internus—and reaches the drainage area of the v. mesenterica inferior (and is carried to the v. portae hepatis) but also partially through the vv. rectales mediae and inferiores to the perianal veins of the external venous plexus. When the sphincter apparatus relaxes during defecation, it allows blood to drain from the hemorrhoidal plexus.
Note: Abnormal dilation (hyperplasia) of the hemorrhoidal plexus beyond the physiological range leads to hemorrhoidal disease, one of the most common proctological disorders (see p. 238 f).
18.9 Continence Organ: Function
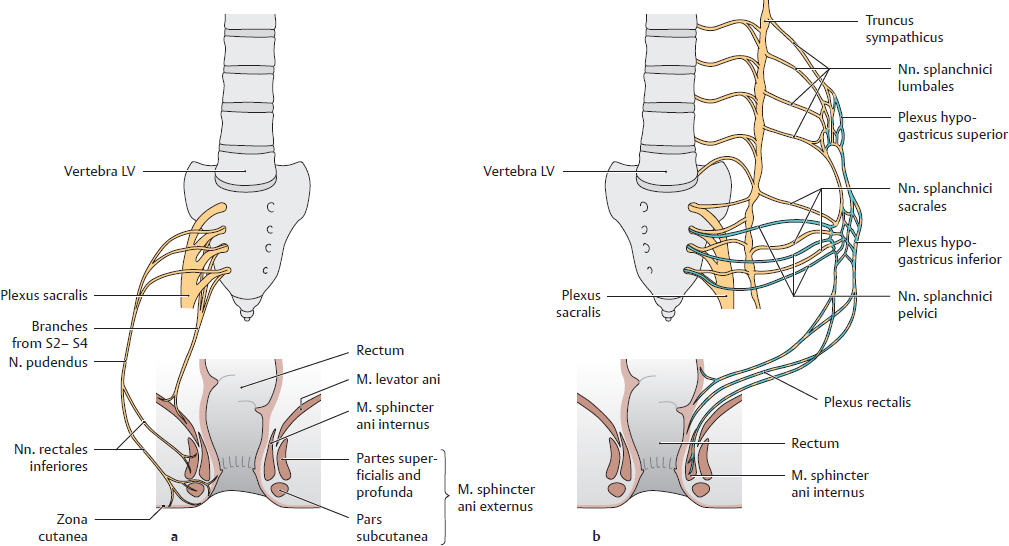
A Innervation (after Stelzner)
a Somatomotor and somatosensory innervation; b Visceromotor and viscerosensory innervation.
• Somatomotor: n. pudendus for the m. sphincter ani externus, levator nerves for the m. levator ani (especially the m. puborectalis). They provide active, partially voluntary innervation of the m. sphincter ani externus and m. levator ani.
• Somatosensory: nn. rectales inferiores for the anus and perianal skin. Arising from the n. pudendus, they transmit touch and especially pain sensation. The skin of the anus is extremely sensitive to pain. Even small tears in the anal skin, which often show inflammatory changes, tend to be extremely painful.
• Visceromotor: nn. splanchnici pelvici (S2–S4) for the m. sphincter ani internus. The resting tone of the internal sphincter helps to maintain closure of the canalis analis and inhibits venous drainage from the hemorrhoidal plexus; the corpus cavernosum remains distended, contributing to fecal continence and flatus control. Topographically, the nn. splanchnici pelvici are closely related to the plexus rectales.
• Viscerosensory: nn. splanchnici pelvici (S2–S4) supply the wall of the rectum, particularly the stretch receptors in the ampulla recti. Stretching of the ampulla by the fecal column triggers a subjective awareness of the need to defecate.
B Mechanism of defecation (after Wedel; see right page)
a Filling of the ampulla recti; b Relaxation of the voluntarily controlled sphincters and propulsion of fecal column.
Both defecation and continence are under central nervous system control involving different anatomical structures ranging from the cortex cerebri to the perianal skin, with the anorectum being one of multiple effectors. Directly involved are the diaphragma pelvis, muscles used during squatting, the abdominal press as well as autonomic and sensory nerves along with their higher nerve centers.
Filling of the ampulla recti and stimulation of local stretch receptors in the ampullary wall: When the fecal bolus is propelled into the ampulla recti by anterogradely propagating waves, mechanoreceptors detect distension and transmit the information via visceral afferents in the funiculus posterior medullae spinalis to the sensory cortex, which perceives the urge to defecate. Olfactory, visual, or acoustic stimuli can either accelerate or decelerate the perception and subsequent voluntary action, which results in defecation.
Rectoanal inhibitory reflex and relaxation of the voluntarily innervated sphincters: When the ampulla fills with feces, the intrarectal pressure increases and the m. sphincter ani internus relaxes, followed by voluntary relaxation of the m. puborectalis sling and the m. sphincter ani externus. As a result, the anorectal angle straightens and the canalis analis widens.
Propulsion of fecal column: Rectal evacuation is assisted by a direct involuntary increase in pressure in the rectal area and by simultaneous increase in pressure by the contraction of voluntarily innervated muscles: abdominal (abdominal press), perineal (pelvic floor lift), diaphragmatic (diaphragma contraction) and glottic (glottis closure) muscles. The squatting position further increases abdominal pressure (flexor reflex). With the propulsion of the fecal column, the hemorrhoidal cushions are drained and pushed out.
Completion of defecation: After the sphincter apparatus allows the fecal column to pass through, it comes in contact with the highly sensitive anoderm, which perceives the volume, consistency, and location of the stool. This perception initiates the voluntary process of completing defecation. Defecation is completed once the sphincter apparatus contracts and the hemorrhoidal plexus fills up.
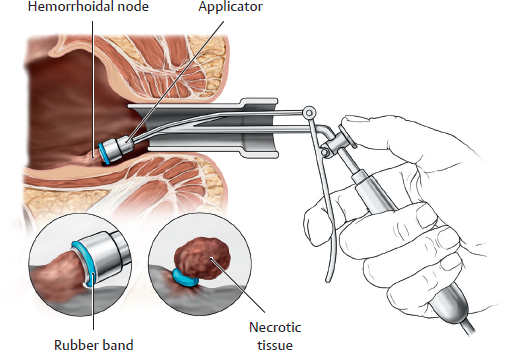
18.10 Disorders of the Canalis Analis: Hemorrhoidal Disease, Anal Abscesses, and Anal Fistulas
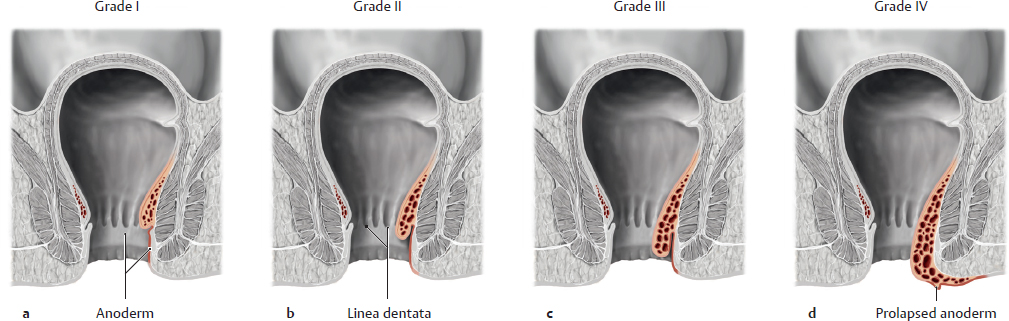
A Hemorrhoidal disease
Hemorrhoidal disease is one of the most common proctological disorders. The site of origin is the circular hemorrhoidal plexus of the cavernous body of the rectum located above the linea pectinata. It is largely responsible for the fine adjustment of anal continence. Hemorrhoid is a general term used to describe hyperplasia (enlargement) of a corpus cavernosum with arterial blood supply, a condition which initially does not cause any symptoms. Hemorrhoids become pathological once they become symptomatic (bleeding is bright red from arterial blood, mucus discharge, itching, burning, fecal soiling, etc.) and when they require treatment (hemorrhoidal disease). Most commonly, hemorrhoids result from increased pressure on the anus during defecation, often caused by chronic constipation as a result of a lack of fiber and fluids in the diet. Another cause is impaired venous return due to increased m. sphincter ani tone as this may lead to the hemorrhoidal plexus taking on a gnarled appearance. Diagnosis and classification of hemorrhoids are based on examination, palpation, and proctoscopy of the canalis analis. Depending on the severity of the hemorrhoids and their symptoms, they are divided into four grades:
• Grade I (a): swollen, elastic cushions of tissue that are visible only on proctoscopy (located above the linea pectinata) and may cause painless bright red bleeding (painless because the swollen cushions are located above the anoderm);
• Grade II (b): visibly hyperplastic vascular cushions, which can prolapse inside or outside of the canalis analis during defecation or while pressing but retract immediately after emptying the bowels. Dripping blood and mucus discharge may cause oozing or itching, a condition also known as perianal eczema;
• Grade III (c): during defecation or while the intra-abdominal pressure is increased, hemorrhoids prolapse spontaneously and require manual repositioning. Possible thrombosis or incarceration of the prolapsed knot may cause significant pain;
• Grade IV (d): at this stage, the nodular enlargements and large parts of the canalis analis, including the highly pain-sensitive anoderm, are permanently prolapsed (irreducible) and attached to the anal margin (also known as an anal prolapse).
Note: Unlike in the German medical terminology, the Anglo-American and Swiss terminology distinguish between internal and external hemorrhoids. Internal hemorrhoids originate from the internal plexus venosus rectalis, external hemorrhoids are subcutaneous clots at the margin of the anus (e.g., perianal thromboses). In our assessment, however, external hemorrhoids are simply hyperplastic vascular cushions of the plexus venosus rectalis with their arterial blood supply that have prolapsed to the outside.
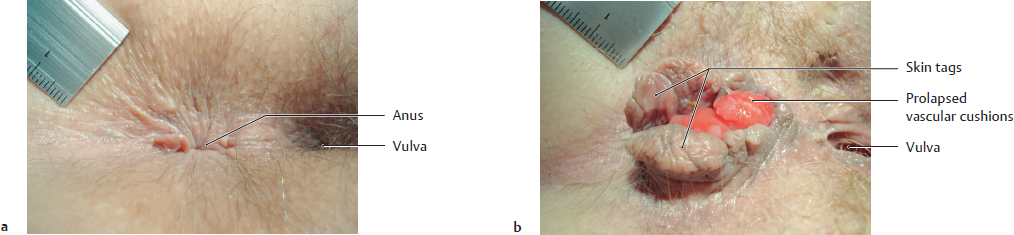
B Conditions of the perianal skin with and without hemorrhoidal disease
a Normal anatomy of the perianal area in a 38 year old female patient;
b Grade IV hemorrhoids in a 54 year old female patient: mucosal prolapse at the commissura laborium anterior combined with right- and left-lateral anal skin tags (harmless, generally asymptomatic perianal skin folds) (from Rohde, H,: Lehratlas der Proktologie. Thieme, Stuttgart 2006).