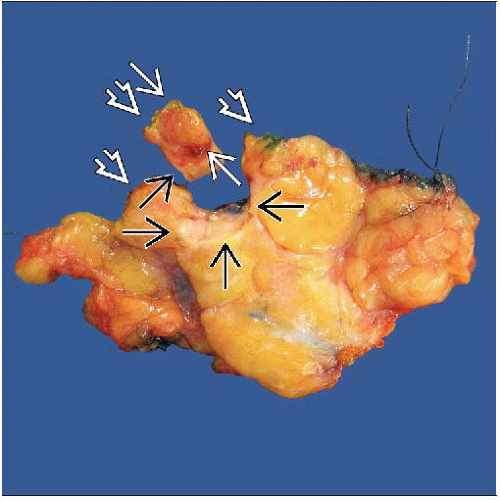
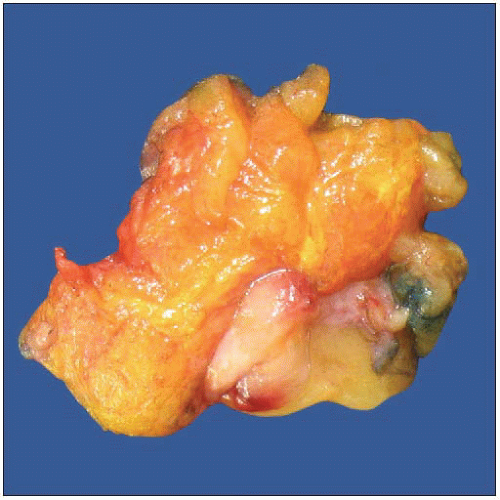
Margins and Reexcisions
INTRODUCTION
Margins and Local Recurrence Rates
Carcinoma present at inked margin (“positive” margin) correlates with higher likelihood of residual disease in the breast
Carcinoma close to margins also increases likelihood of residual disease, but magnitude of risk is dependent on type of cancer (invasive or in situ), distance from margin, and extent
Residual carcinoma in the breast is associated with increased risk of local recurrence
Minimizing risk of local recurrence is important goal
Can improve survival for patients whose initial carcinoma is likely curable (carcinoma in situ and small node-negative invasive carcinomas)
Reduces need for additional surgery and treatment
Reduces possibility of uncontrolled local disease in skin and chest wall (“carcinoma en cuirasse”)
Recurrence is often very psychologically difficult for patients
Often mastectomy is required for treatment as radiation cannot be delivered to chest 2nd time
Margins for palpable invasive carcinomas are generally negative
Surgeon palpates the cancer and excises rim of grossly normal tissue
Apparently positive margin on microscopic examination may be due to ink leakage or inadvertent incision into carcinoma
Generally several mm of cauterized tissue within biopsy cavity
Residual carcinoma at edge of biopsy site will not be viable
Therefore, focally positive margin for invasive cancer usually does not correlate with residual invasive carcinoma in the patient
Margins for nonpalpable invasive carcinomas (due to small size or diffusely invasive pattern) may be positive
Surgeon cannot palpate the cancer and, therefore, must make educated guess as to how much tissue to remove
If carcinoma is transected, it will be present at margin over broad front
Cautery artifact on carcinoma supports that margin is a true surgical margin
Extensive residual carcinoma may be present in breast
Margins are often positive or close for DCIS
DCIS is rarely grossly evident
Extent of DCIS cannot be determined with certainty by clinical examination or imaging
Surgeon cannot definitively know how much tissue to remove
Margins can only be evaluated with certainty microscopically on permanent sections
Prediction of Residual Carcinoma
Even under best conditions, likelihood of residual carcinoma in breast can only be estimated
Presence of cancer at margins does not predict residual cancer with certainty
There may not be breast tissue beyond edge of specimen
Particularly relevant for margins adjacent to skin and pectoralis muscle
Often several mm of cauterized tissue in biopsy cavity in patient
Cautery may destroy small amounts of residual invasive carcinoma
Margins may be falsely positive due to ink leakage into cracks or specimen fragmentation
Can be gaps between areas of involvement by DCIS
Duct at margin can appear free of DCIS, but DCIS can be present further along in duct
Margins can be falsely negative if areas of involvement are not sampled or if areas are too small to be present within the width of the section
Risk Factors for Local Recurrence
Approximately 10% of patients will have local recurrence at 10 years
Risk factors for recurrence include
Young patient age
Poorly differentiated carcinomas
Positive margins
Extensive intraductal component (EIC) with DCIS located away from invasive carcinoma
Extensive lymph-vascular invasion
Subtypes of breast cancer have different local recurrence rates at 5 years
Luminal A (ER or PR positive, HER2 negative): 0.8%
Luminal B (ER or PR positive, HER2 positive): 1.5%
HER2 (ER and PR negative, HER2 positive): 8.4%
Triple negative (basal-like) (ER, PR, and HER2 negative): 7.1%
Growth rate of hormone-positive carcinomas can be inhibited by hormonal therapy over many years
Patients with HER2-positive carcinomas are now being treated with HER2-targeted therapy over many years
Treatment reduces likelihood of local recurrence
Targeted therapy for triple negative carcinomas is not yet available
TYPES OF MARGINS
En Face (Shave)
Thin (2-4 mm) slice of tissue is taken from surface of specimen; similar to removing section of orange peel
Any cancer seen in tissue section on glass slide is, by definition, at margin
Actual distance from margin cannot be determined
Larger area can be examined than is seen in perpendicular sections
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree