http://evolve.elsevier.com/McCuistion/pharmacology/
Diuretics are used for two main purposes: to decrease hypertension (lower blood pressure) and to decrease edema, typically peripheral and pulmonary, in heart failure (HF) and renal or liver disorders. Hypertension is a blood pressure greater than 140/90 mm Hg. Diuretics discussed in this chapter are used either alone or in combination to decrease blood pressure and edema.
Diuretics produce increased urine flow, or diuresis, by inhibiting sodium and water reabsorption from the kidney tubules. Most sodium and water reabsorption occurs throughout the renal tubular segments (proximal, loop of Henle [descending loop and ascending loop], and collecting tubule). Diuretics can affect one or more segments of the renal tubules. Fig. 38.1 illustrates the renal tubule along with the normal process of water and electrolyte reabsorption and diuretic effects on the tubules.
Every 1.5 hours, the total volume of the body’s extracellular fluid (ECF) goes through the kidneys (glomeruli) for cleansing; this is the first process for urine formation. Small particles such as electrolytes, drugs, glucose, and waste products from protein metabolism are filtered in the glomeruli. Larger products such as protein and blood cells are not filtered with normal renal function, and they remain in the circulation. Sodium and water are the largest filtrate substances.
Normally, 99% of the filtered sodium that passes through the glomeruli is reabsorbed; 50% to 55% of sodium reabsorption occurs in the proximal tubules, 35% to 40% occurs in the loop of Henle, 5% to 10% occurs in the distal tubules, and less than 3% occurs in the collecting tubules. Diuretics that act on the tubules closest to the glomeruli have the greatest effect in causing natriuresis, sodium loss in the urine. A classic example is the osmotic diuretic mannitol. The diuretic effect depends on the drug reaching the kidneys and its concentration in the renal tubules.
Diuretics have an antihypertensive effect because they promote sodium and water loss by blocking sodium and chloride reabsorption. This causes a decrease in fluid volume, which lowers blood pressure. With fluid loss, edema—fluid retention in body tissues—should decrease, but if sodium is retained, water is also retained, and blood pressure increases.
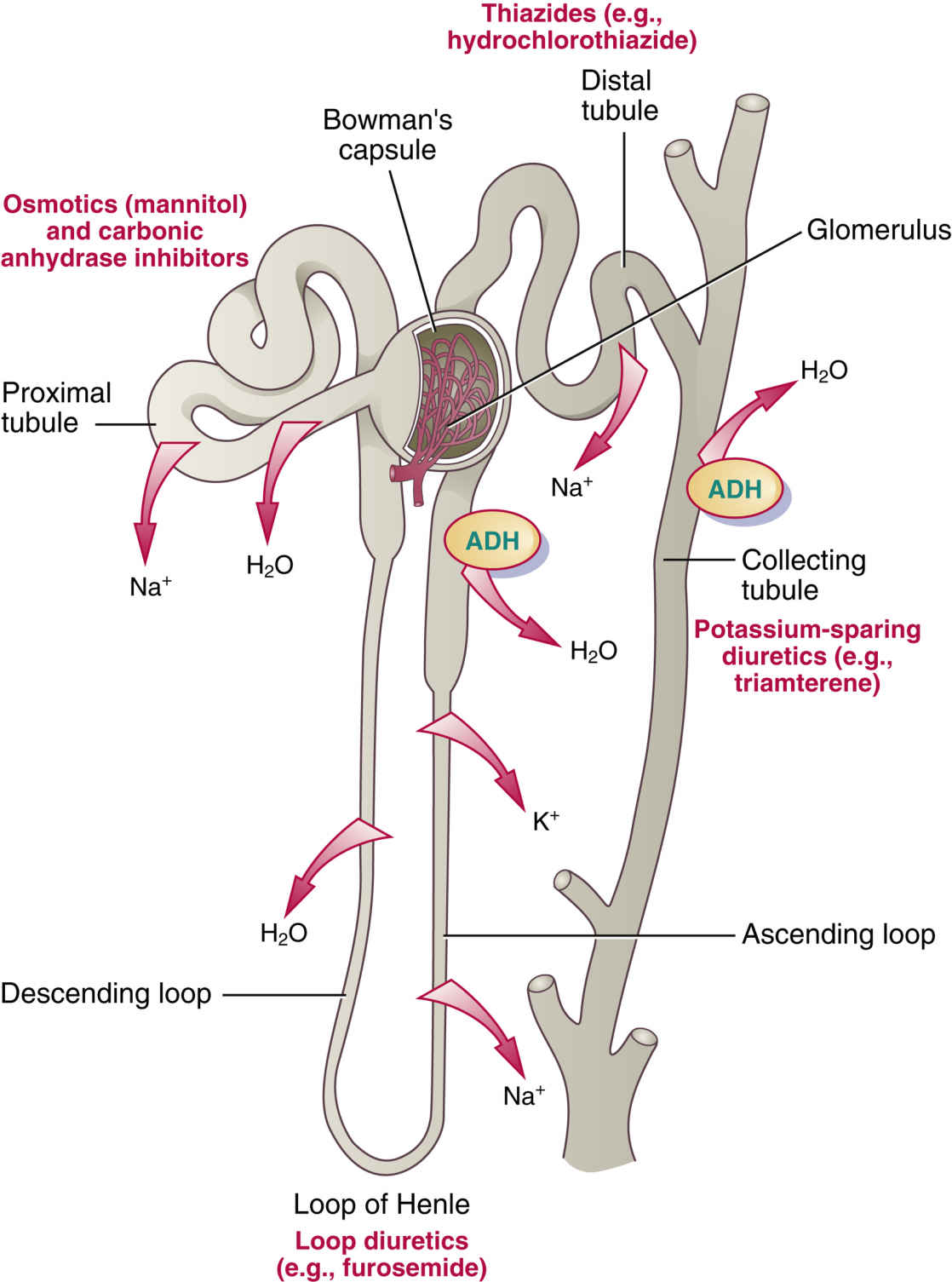
FIG. 38.1 Diuretics act on different segments of the renal tubule. Osmotic, mercurial, and carbonic anhydrase inhibitor diuretics affect the proximal tubule; loop diuretics affect the loop of Henle; thiazides affect the distal tubule; and potassium-sparing diuretics act primarily on the collecting tubules. ADH, Antidiuretic hormone; H2O, water; K+, potassium; Na+, sodium.
Many diuretics cause the loss of other electrolytes, including potassium, magnesium, chloride, and bicarbonate. The diuretics that promote potassium excretion are classified as potassium-wasting diuretics, and those that promote potassium retention are called potassium-sparing diuretics.
The following five categories of diuretics are effective in removing water and sodium:
• Thiazide and thiazide-like diuretics
• Loop or high-ceiling diuretics
• Osmotic diuretics
• Carbonic anhydrase inhibitors
• Potassium-sparing diuretics
Thiazide, loop, and potassium-sparing diuretics are most frequently prescribed for hypertension and for edema associated with HF. Except for those in the potassium-sparing group, all diuretics are potassium wasting.
Combination diuretics that contain both potassium-wasting and potassium-sparing drugs have been marketed primarily for the treatment of hypertension. Combinations have an additive effect in reducing blood pressure and are discussed in more detail in the Potassium-Sparing Diuretics section later in this chapter. Chapter 39 takes a closer look at the combinations of antihypertensive agents with hydrochlorothiazide.
Thiazides and Thiazide-Like Diuretics
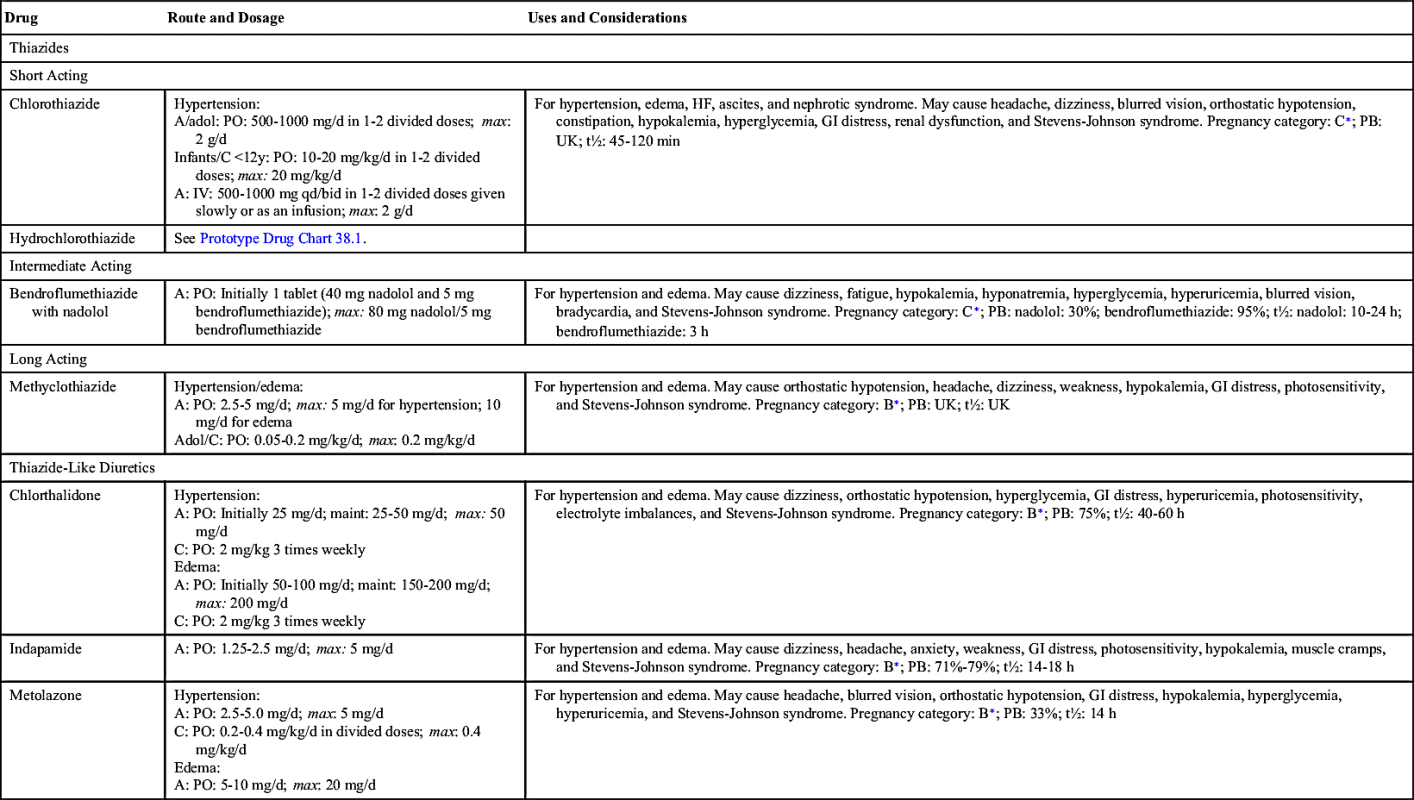
The first thiazide, chlorothiazide, was marketed in 1957 and was followed a year later by hydrochlorothiazide. There are numerous thiazide and thiazide-like preparations. Thiazides act on the distal convoluted renal tubule, beyond the loop of Henle, to promote sodium, chloride, and water excretion. Thiazides are used to treat hypertension and peripheral edema. They are not effective for immediate diuresis and should not be used to promote fluid loss in patients with severe renal dysfunction. Table 38.1 lists thiazide and thiazide-like diuretics and their dosages, uses, and considerations. Drug dosages for hypertension and edema are similar.
Thiazide diuretics are used primarily for patients with normal renal function. If the patient has a renal disorder and creatinine clearance is less than 30 mL/min, the effectiveness of the thiazide diuretic is greatly decreased. Thiazides cause a loss of sodium, potassium, and magnesium, but they promote calcium reabsorption. Hypercalcemia (calcium excess) may result, and the condition can be hazardous to the patient who is digitalized or has cancer that causes hypercalcemia. Thiazides affect glucose tolerance, so hyperglycemia can also occur. Thiazides should be used cautiously in patients with diabetes mellitus. Laboratory test results, such as electrolytes and glucose, need to be monitored.
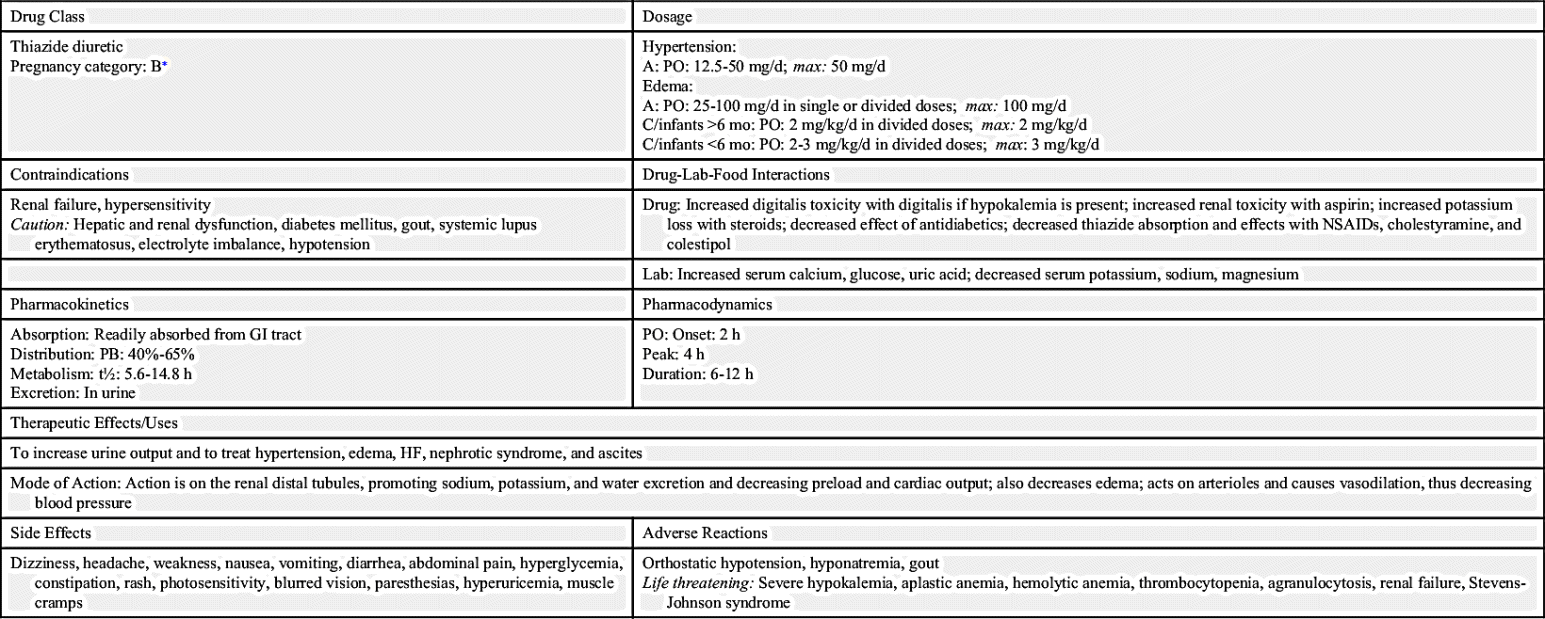
Hydrochlorothiazide has been combined with selected angiotensin-converting enzyme (ACE) inhibitors, beta blockers, alpha blockers, angiotensin II blockers, and centrally acting sympatholytics to control hypertension. Prototype Drug Chart 38.1 outlines the pharmacologic data for hydrochlorothiazide.
Pharmacokinetics
Thiazides are well absorbed from the gastrontestinal (GI) tract. Hydrochlorothiazide has moderate protein-binding power. The half-life of the thiazide drugs is longer than that of the loop diuretics. For this reason, thiazides should be administered in the morning to avoid nocturia (nighttime urination) and sleep interruption.
Pharmacodynamics
Thiazides act directly on arterioles to cause vasodilation, which can lower blood pressure. Other action includes the promotion of sodium chloride and water excretion, resulting in a decrease in vascular fluid volume and a concomitant decrease in cardiac output and blood pressure. The onset of action of hydrochlorothiazide occurs within 2 hours. Peak concentration times are long (4 hours). Thiazides are divided into three groups according to their duration of action: (1) short acting (duration <12 hours), (2) intermediate acting (duration 12–24 hours), and (3) long acting (duration >24 hours).
Side Effects and Adverse Reactions
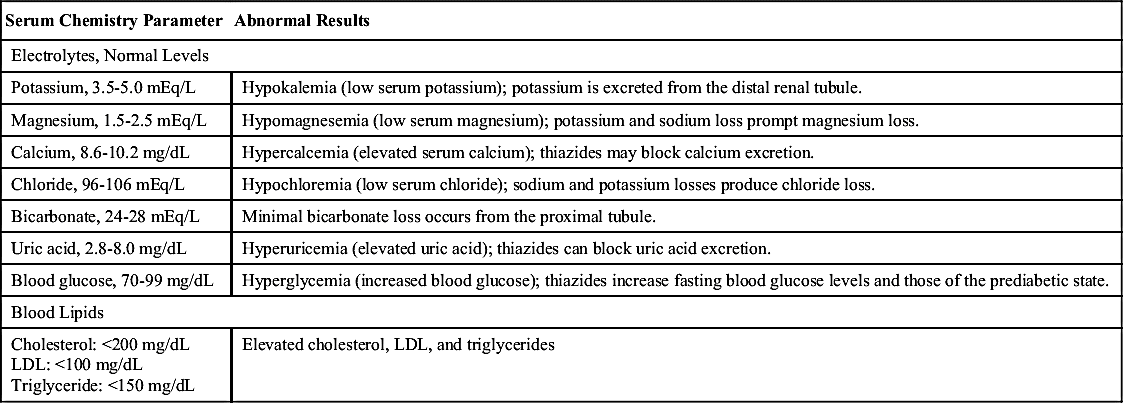
Side effects and adverse reactions of thiazides include electrolyte imbalances (hypokalemia, hypercalcemia, hypomagnesemia, and bicarbonate loss), hyperglycemia (elevated blood glucose), hyperuricemia (elevated serum uric acid level), and hyperlipidemia (elevated blood lipid level). Signs and symptoms of hypokalemia should be assessed, and serum potassium levels must be closely monitored. Potassium supplements are frequently needed. Serum calcium and uric acid levels should be checked because thiazides block calcium and uric acid excretion. Thiazides affect the metabolism of carbohydrates, and hyperglycemia can result, especially in patients with high to high-normal blood glucose levels. Thiazides can increase serum cholesterol, low-density lipoprotein, and triglyceride levels. A drug may be ordered to lower blood lipids. Other side effects include dizziness, headache, nausea, vomiting, constipation, urticaria, or hives (rare) and blood dyscrasias (rare). Table 38.2 summarizes the serum chemistry abnormalities that can occur with thiazide use.
Contraindications
Thiazides are contraindicated for use in renal failure. Symptoms of severe kidney impairment or shutdown include oliguria, a marked decrease in urine output; elevated blood urea nitrogen (BUN); and elevated serum creatinine.
Drug Interactions
Of the numerous thiazide drug interactions, the most serious occurs with digoxin. Thiazides can cause hypokalemia, which enhances the action of digoxin, and digitalis toxicity can occur. Potassium supplements are frequently prescribed, and serum potassium levels are monitored. Thiazides also induce hypercalcemia, which enhances the action of digoxin, resulting in possible digitalis toxicity. Signs and symptoms of digitalis toxicity—bradycardia, nausea, vomiting, and visual changes—should be reported. Thiazides enhance the action of lithium, and lithium toxicity can occur. Thiazides potentiate the action of other antihypertensive drugs, which may be used to advantage in combination drug therapy for hypertension.