70
Bone and Joint Infections
CHAPTER CONTENTS
INTRODUCTION
Bone and joint infections are serious infections because destruction of bone or cartilage can lead to significant disability. Osteomyelitis and infectious arthritis are caused primarily by bacteria or fungi. In these diseases, the organisms directly infect the bone and joint. In contrast, immune complex arthritis, reactive arthritis, and rheumatic fever are caused by immune reactions to either bacteria or viruses, and organisms are not found in the joints.
The clinical diagnosis of infectious arthritis often involves an analysis of joint fluid. Radiologic studies of joints and bone contribute important information. Microbiologic diagnosis of osteomyelitis and infectious arthritis is typically made by culturing either a bone specimen or joint fluid. Antimicrobial therapy is typically given for long periods (i.e., weeks to months).
OSTEOMYELITIS
Definition
Osteomyelitis is an infection of the bone. The term osteo refers to bone, and myelo refers to the bone marrow. Osteomyelitis is classified as either acute or chronic.
Pathophysiology
The most common mode by which organisms reach the bone is by hematogenous spread (i.e., either bacteremia or fungemia) from a distant site. Acute bacterial osteomyelitis often arises from a pyogenic skin infection such as a boil, but many sources are undetected. Mycobacterial and fungal osteomyelitis often arise from the initial site of infection in the lung.
In children, hematogenous spread tends to result in osteomyelitis located at the end of long bones (at the metaphyses) that are richly endowed with blood vessels. In adults, hematogenous spread results most commonly in vertebral osteomyelitis and discitis, not osteomyelitis of the long bones.
Osteomyelitis also occurs by direct extension from an infected contiguous site such as a skin or soft tissue infection. It also can occur following trauma that results in an open fracture and direct contamination of the bone.
Chronic osteomyelitis tends to occur in the lower extremity, especially in diabetics who often have vascular insufficiency. They are predisposed to skin and soft tissue infections that extend into the bone.
Clinical Manifestations
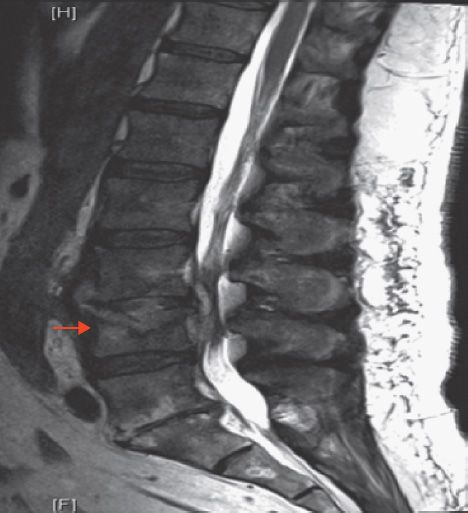
The most characteristic clinical manifestations are bone pain and localized tenderness at the site of infection. Most (but not all) patients also have constitutional symptoms such as fever, night sweats, and fatigue. Limited range of motion of an affected extremity is seen. In vertebral osteomyelitis, the lumbar region is affected more often than the cervical or thoracic regions (Figure 70–1).
FIGURE 70–1 Vertebral osteomyelitis. Arrow indicates site of vertebral lesion. (Reproduced with permission from McKean SC et al. Principles and Practice of Hospital Medicine. New York: McGraw-Hill, 2012. Copyright © 2012 by The McGraw-Hill Companies, Inc.)
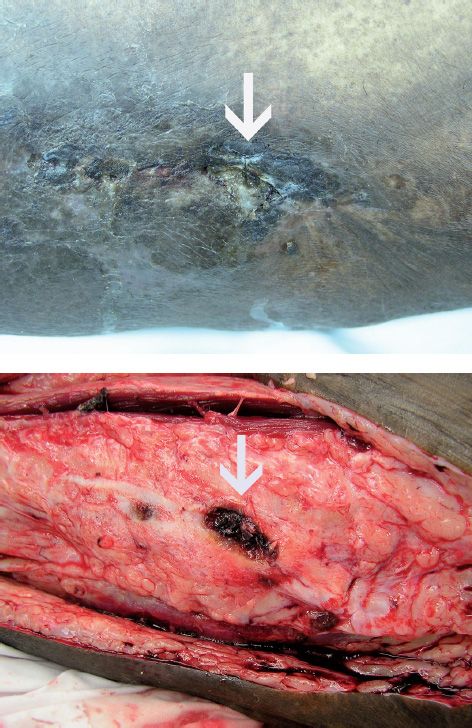
In acute osteomyelitis, the symptoms occur abruptly and progress rapidly, whereas in chronic osteomyelitis, the course is more indolent. In chronic osteomyelitis, necrosis of the bone occurs, and a sequestrum (an avascular piece of infected bone) can form at the site of the lesion (Figure 70–2). Relapses tend to occur in chronic osteomyelitis more than in acute osteomyelitis, and surgical debridement, especially to remove sequestra, is important to minimize the risk of relapse.
FIGURE 70–2 Chronic osteomyelitis. A. White arrow points to draining fistula at site of chronic osteomyelitis. B. White arrow points to necrotic bone caused by chronic osteomyelitis. (From Kemp WL, Burns DK, Brown TG: Pathology: The Big Picture. New York, McGraw-Hill, 2008. Copyright © 2008 by The McGraw-Hill Companies, Inc.)
Pathogens
The most common bacterial cause of acute osteomyelitis in both children and adults is Staphylococcus aureus (Table 70–1). However, vertebral osteomyelitis in adults may be caused by Mycobacterium tuberculosis (Pott’s disease). Osteomyelitis in patients with hip or knee prostheses is likely to be caused by Staphylococcus epidermidis or other skin flora. When osteomyelitis occurs in an intravenous drug user, it is most often caused by S. aureus; however, gram-negative rods, such as Pseudomonas
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree