http://evolve.elsevier.com/McCuistion/pharmacology/
Three groups of drugs—cardiac glycosides, antianginals, and antidysrhythmics—are discussed in this chapter. Drugs in these groups regulate heart contraction, heart rate and rhythm, and blood flow to the myocardium (heart muscle).
Cardiac Glycosides
Digitalis use began as early as CE 1200, making it one of the oldest drugs. It is still used in a purified form. Digitalis is obtained from the purple and white foxglove plant, and it can be poisonous. Digitalis preparations have come to be known for their effectiveness in treating heart failure (HF), also known as cardiac failure (CF), and previously referred to as congestive heart failure (CHF). When the heart muscle (myocardium) weakens and enlarges, it loses its ability to pump blood through the heart and into the systemic circulation. This is called heart failure, pump failure, or chronic heart failure. When compensatory mechanisms fail and the peripheral and lung tissues are congested, the condition is called acute heart failure. The causes of HF include chronic hypertension, myocardial infarction (MI), coronary artery disease (CAD), valvular heart disease, congenital heart disease, and arteriosclerosis.
Heart failure can be left-sided or right-sided. The patient has left-sided HF when the left ventricle does not contract sufficiently to pump the blood returned from the lungs and left atrium out through the aorta into the peripheral circulation; this causes excessive amounts of blood to back up into the lung tissue. Usually the patient has shortness of breath (SOB) and dyspnea. Right-sided HF occurs when the heart does not sufficiently pump the blood returned into the right atrium from the systemic circulation. As a result, the blood and its constituents are backed up into peripheral tissues, causing peripheral edema. Left-sided HF may lead to right-sided HF and vice versa. Myocardial hypertrophy resulting in cardiomegaly, increased heart size, can be a major problem associated with chronic HF.
In the cardiac physiology of HF, an increase in preload and afterload occurs. The increased preload results from an excess of blood volume in the ventricle at the end of diastole. This occurs because of a pathologic increase in the stretching and thickening of the ventricular walls, which allows a greater filling pressure associated with a weakened heart. Increased afterload is an additional pressure or force in the ventricular wall caused by excess resistance in the aorta. This resistance must be overcome to open the aortic valve so blood can be ejected into the circulation. The American College of Cardiology Foundation (ACCF) and the American Heart Association (AHA) have classified HF in stages according to its severity. Table 37.1 lists the stages of HF according to the ACCF/AHA. In the early stage of HF, there are no symptoms, and no structural heart damage occurs. Detailed information related to the staging process of HF can be found at http://www.heart.org/HEARTORG/Conditions/HeartFailure/Heart-Failure_UCM_002019_SubHomePage.jsp.
Naturally occurring cardiac glycosides are found in a number of plants, including Digitalis. Also called Digitalis glycosides, this group of drugs inhibits the sodium-potassium pump, which results in an increase in intracellular sodium. This increase leads to an influx of calcium, which causes the cardiac muscle fibers to contract more efficiently. Digitalis preparations have three effects on heart muscle: (1) a positive inotropic action increases myocardial contraction stroke volume, (2) a negative chronotropic action decreases heart rate, and (3) a negative dromotropic action decreases conduction of heart cells. The increase in myocardial contractility strengthens cardiac, peripheral, and kidney function by enhancing cardiac output, decreasing preload, improving blood flow to the periphery and kidneys, decreasing edema, and promoting fluid excretion. As a result, fluid retention in the lungs and extremities is decreased. Digoxin does not prolong life, rather it acts by increasing the force and velocity of myocardial systolic contraction.
Digoxin is a secondary drug for HF. First-line drugs used to treat acute HF include intravenous (IV) inotropic agents (dopamine and dobutamine) and phosphodiesterase inhibitors, such as milrinone. Other drugs prescribed for HF include oral diuretics, beta blockers, angiotensin-converting enzyme (ACE) inhibitors, angiotensin-receptor blockers (ARBs), calcium channel blockers, and vasodilators, all of which are more convenient to self-administer. Oral administration allows the patient to go home on these medications.
Cardiac glycosides are also used to correct atrial fibrillation, cardiac dysrhythmia with rapid uncoordinated contractions of atrial myocardium, and atrial flutter, cardiac dysrhythmia with rapid contractions of 200 to 300 beats/min. This is accomplished by the negative chronotropic effects (decreased heart rate) and negative dromotropic effects (decreased conduction through the atrioventricular [AV] node).
When digoxin cannot convert atrial fibrillation to normal heart rhythm, the goal is to slow the heart rate by decreasing electrical impulses through the AV node. For management of atrial fibrillation, a calcium channel blocker such as verapamil may be prescribed. To prevent thromboemboli resulting from atrial fibrillation, warfarin is prescribed concurrently with other drug therapy. Warfarin is discussed in Chapter 40.
Nonpharmacologic Measures to Treat Heart Failure
Nondrug therapy is an integral part of the regimen for controlling HF. The nondrug component of the regimen should be tailored to meet the needs of each patient, but the following are some general recommendations. The patient should limit salt intake to 2 g/day, approximately 1 teaspoon. Alcohol intake should be either decreased to 1 drink per day or completely avoided because excessive alcohol use can lead to cardiomyopathy. Fluid intake may be restricted. Smoking should be avoided because it deprives the heart of oxygen (O2). Obesity may increase cardiovascular problems if it is associated with unhealthy behaviors, thus obese patients should modify their behaviors as needed. Saturated fat intake should be decreased. Mild exercise, such as walking or bicycling, is recommended.
TABLE 37.1
The American College of Cardiology Foundation/American Heart Association Stages of Heart Failure
| Stage | Characteristics According to Stage |
| A | High risk for heart failure without symptoms of structural heart disease |
| B | Some cardiac changes, such as decreased ejection fraction without symptoms of heart failure |
| C | Structural heart disease with symptoms of heart failure, such as fatigue, shortness of breath, edema, and decrease in physical activity |
| D | Severe structural heart disease and marked symptoms of heart failure at rest |
Laboratory Tests
Atrial Natriuretic Hormone or Peptide
Reference values: 20 to 77 pg/mL; 20 to 77 ng/L (SI units). An elevated atrial natriuretic hormone (ANH) or atrial natriuretic peptide (ANP) may confirm HF. ANH is secreted from the atria of the heart and acts as an antagonist to renin and aldosterone. Released during expansion of the atrium, it produces vasodilation and increases glomerular filtration rate (GFR). Results of ANH secretion include a large volume of urine that decreases blood volume and blood pressure.
Brain Natriuretic Peptide
Reference values: Desired value is less than 100 pg/mL; positive value is greater than 100 pg/mL. The brain natriuretic peptide (BNP) is primarily secreted from atrial cardiac cells and, when tested, aids in the diagnosis of HF. Diagnosing HF is difficult in persons with lung disease who are experiencing dyspnea and in those who are obese or older. An elevated BNP helps differentiate that dyspnea is due to HF rather than to lung dysfunction. Frequently the BNP is higher than 100 pg/mL in women who are 65 years of age or older. An 80-year-old woman may have a BNP of 160 pg/mL; however, the BNP is markedly higher (i.e., 400 pg/mL) in HF. BNP is considered a more sensitive test than ANP for diagnosing HF. Today, a bedside/emergency department machine can be used to measure BNP.
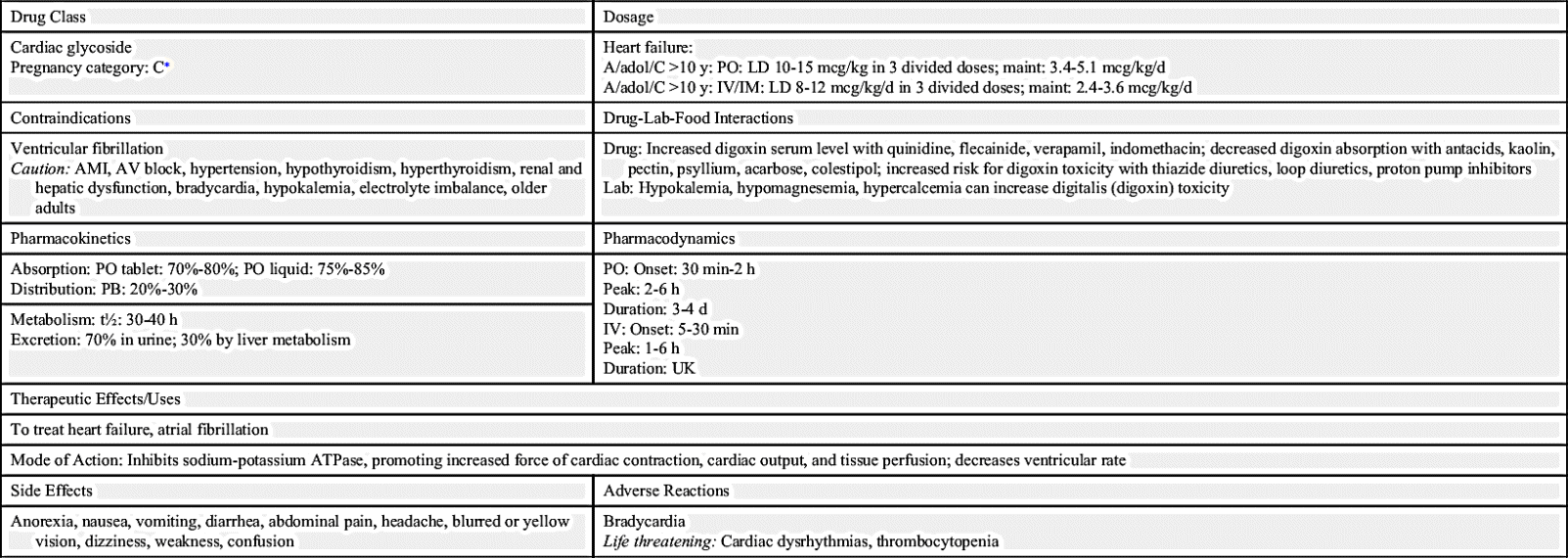
Digoxin
Prototype Drug Chart 37.1 gives the pharmacologic data for digoxin, a cardiac glycoside.
Pharmacokinetics
The absorption rate of digoxin in oral tablet form is 70% to 80%. The rate is 75% to 85% in liquid form. The protein-binding power for digoxin is 20% to 30%. The half-life is 30 to 40 hours. Because of its long half-life, drug accumulation can occur. Side effects should be closely monitored to detect digitalis toxicity. Patients should be made aware of side effects that need to be reported to the health care provider. Serum digoxin levels are most commonly drawn when actual digitoxicity is suspected. This allows the health care provider to ascertain the extent of such toxicity and to confirm elimination of the drug after it is stopped or decreased in dosage (see the Digitalis [Digoxin] Toxicity section later in this chapter).
Thirty percent of digoxin is metabolized by the liver, and 70% is excreted by the kidneys mostly unchanged. Kidney dysfunction can affect the excretion of digoxin. Thyroid dysfunction can alter the metabolism of cardiac glycosides. For patients with hypothyroidism, the dose of digoxin should be decreased; in hyperthyroidism, the dose may need to be increased.
Pharmacodynamics
In patients with a failing heart, cardiac glycosides increase myocardial contraction, which increases cardiac output and improves circulation and tissue perfusion. Because these drugs decrease conduction through the AV node, the heart rate decreases. The onset and peak actions of oral and IV digoxin vary. The digoxin therapeutic serum level for dysrhythmias is 0.8 to 2.0 ng/mL. The target therapeutic serum level for heart failure is 0.5 to 1.0 ng/mL.
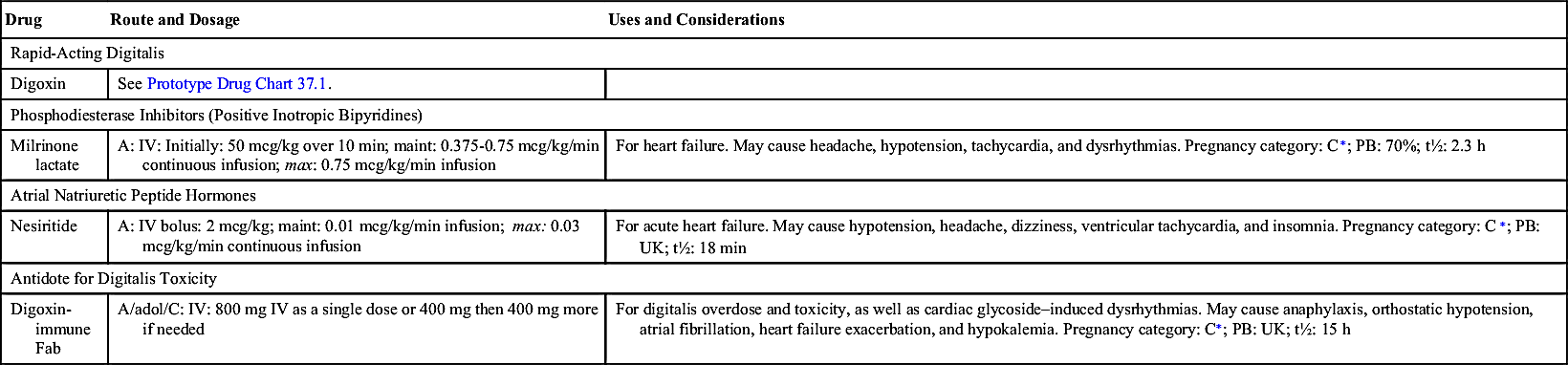
Digoxin can be administered orally or by the IV route. Table 37.2 lists the digitalis preparations and their dosages, uses, and considerations.
Digitalis (Digoxin) Toxicity
Overdose or accumulation of digoxin causes digitalis toxicity. Signs and symptoms include anorexia, diarrhea, nausea and vomiting, bradycardia (pulse rate below 60 beats/min), premature ventricular contractions, cardiac dysrhythmias, headaches, malaise, blurred vision, visual illusions (white, green, or yellow halos around objects), confusion, and delirium. Older adults are more prone to toxicity.
Cardiotoxicity is a serious adverse reaction to digoxin, and ventricular dysrhythmias result. Three cardiac-altered functions can contribute to digoxin-induced ventricular dysrhythmias: (1) suppression of AV conduction, (2) increased automaticity, and (3) a decreased refractory period in ventricular muscle. The antidysrhythmics phenytoin and lidocaine are effective in treating digoxin-induced ventricular dysrhythmias. Lidocaine should be limited to short-term treatment.
Antidote for Cardiac/Digitalis Glycosides
Digoxin-immune Fab may be given to treat severe digitalis toxicity. This agent binds with digoxin to form complex molecules that can be excreted in the urine, thus digoxin is unable to bind at the cellular site of action. Serum digoxin levels should be closely monitored, and signs and symptoms of digoxin toxicity should be reported promptly to the health care provider. Digitalis toxicity may result in first-degree, second-degree, or complete heart block.
Drug Interactions
Drug interaction with digitalis preparations can cause digitalis toxicity. Many of the potent diuretics, such as furosemide and hydrochlorothiazide, promote the loss of potassium from the body. The resultant hypokalemia, low serum potassium level, increases the effect of digoxin at its myocardial cell site of action, resulting in digitalis toxicity. Cortisone preparations taken systemically promote sodium retention and potassium excretion or loss and can also cause hypokalemia. Patients who take digoxin along with a potassium-wasting diuretic or a cortisone drug should consume foods rich in potassium or take potassium supplements to avoid hypokalemia and digitalis toxicity. Antacids can decrease digitalis absorption if taken at the same time. To prevent this problem, doses should be staggered.
 Phosphodiesterase Inhibitors
Phosphodiesterase Inhibitors
Phosphodiesterase inhibitors are another positive inotropic group of drugs given to treat acute HF. This drug group inhibits the enzyme phosphodiesterase (PDE), which promotes a positive inotropic response and vasodilation. A drug in this group is milrinone lactate. This drug increases stroke volume and cardiac output and promotes vasodilation. It is administered intravenously for no longer than 48 to 72 hours. Severe cardiac dysrhythmias might result from the use of PDE inhibitors, so the patient’s electrocardiogram (ECG) and cardiac status should be closely monitored. Milrinone is a high-alert medication that may cause significant harm to a patient when given inappropriately.
Other Agents Used to Treat Heart Failure
Vasodilators, ACE inhibitors, angiotensin II–receptor antagonists (blockers), diuretics (thiazides, furosemide), spironolactone, and some beta blockers are other drug groups prescribed to treat HF.
Vasodilators can be used to treat HF. The vasodilators decrease venous blood return to the heart and result in a decrease in cardiac filling, ventricular stretching (preload), and oxygen demand on the heart. Arteriolar dilators act in three ways: they (1) reduce cardiac afterload, which increases cardiac output; (2) dilate the arterioles of the kidneys, which improves renal perfusion and increases fluid loss; and (3) improve circulation to the skeletal muscles.
ACE inhibitors are usually prescribed for HF. ACE inhibitors dilate venules and arterioles, which improves renal blood flow and decreases blood fluid volume. ACE inhibitors also moderately decrease the release of aldosterone, which in turn reduces sodium and fluid retention.
ACE inhibitors can increase potassium levels, so serum potassium levels should be monitored, especially if potassium-sparing diuretics such as spironolactone are being taken concurrently. Angiotensin II–receptor blockers (ARBs) such as valsartan and candesartan have been approved for HF in patients who cannot tolerate ACE inhibitors. Refer to Chapter 39 for a complete discussion of ACE inhibitors and ARBs.
Diuretics are the first-line drug treatment for reducing fluid volume. They are frequently prescribed with digoxin or other agents.
Spironolactone, a potassium-sparing diuretic, is used in treating moderate to severe HF. Aldosterone secretions are increased in HF. This promotes body loss of potassium and magnesium needed by the heart and increases sodium and water retention. Spironolactone blocks the production of aldosterone. This drug improves heart rate variability and decreases myocardial fibrosis by its cardioprotective effect of blocking aldosterone in the heart and blood vessels to promote cardiac remodeling. The recommended dose for HF is 12.5 to 25 mg/day. Occurrence of hyperkalemia (excess serum potassium) is rare unless the patient is receiving 50 mg/day and has renal insufficiency. However, the serum potassium level should be closely monitored.
In the past, all beta blockers were contraindicated for patients with HF because this drug class reduces cardiac contractility. With dosage control, beta blockers (carvedilol, metoprolol, and bisoprolol) have been shown to improve cardiac performance. Doses should be low initially and gradually increased. It may take 1 to 3 months for a beneficial effect to develop. Refer to Chapters 15 and 39 for more information on beta blockers.
Nesiritide is an atrial natriuretic peptide hormone that inhibits antidiuretic hormone (ADH) by increasing urine sodium loss. Its effect in correcting HF is achieved by promoting vasodilation, natriuresis, and diuresis. It is useful for treating patients who have acute decompensated HF with dyspnea at rest or who have dyspnea with little physical exertion.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree