http://evolve.elsevier.com/Edmunds/NP/
 Top 100 drug;
Top 100 drug;  Key drug. The antihistamine diphenhydramine is the earliest antihistamine that is commonly used.
Key drug. The antihistamine diphenhydramine is the earliest antihistamine that is commonly used.
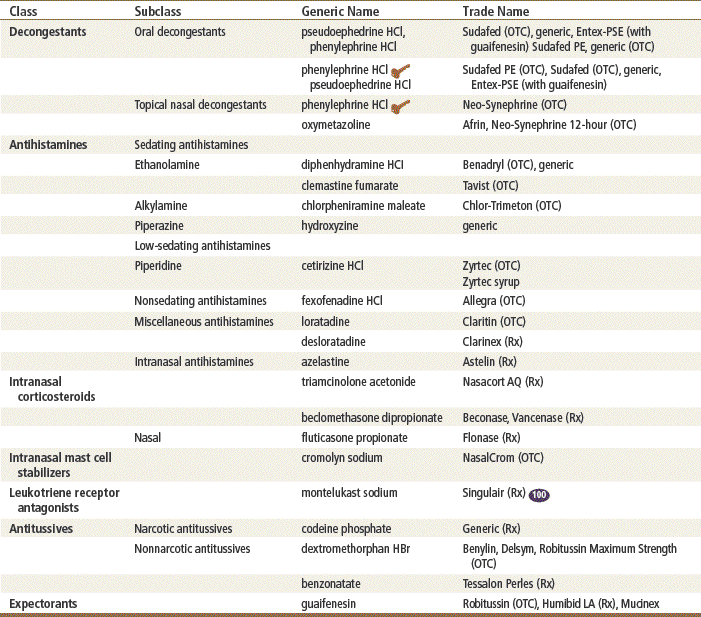
The seven classes of drugs discussed in this chapter are used to treat a variety of upper respiratory conditions. The two most common conditions in primary care practice that require these medications are upper respiratory viral infection (URI or viral rhinitis) and allergic rhinitis (hay fever). Bacterial infections are covered in the section on antibiotics.
Decongestants and antihistamines are commonly used both OTC and by prescription for treatment of a variety of conditions. Decongestants are used as first-line drugs for URIs. Antihistamines are first-line treatment for allergic rhinitis. Leukotriene receptor antagonists may be used as first-line treatment for allergic rhinitis but are typically prescribed when other treatments fail to relieve symptoms. The antihistamines most commonly seen in primary care practice are discussed here.
Intranasal steroids and cromolyn are generally considered second-line treatment for upper respiratory conditions. Oral formulations of these drugs are used for lower respiratory conditions. These drugs are discussed in detail in Chapter 14; only their intranasal use in upper respiratory conditions is discussed here.
Antitussives and expectorants are used as adjunct therapy in upper respiratory and lower respiratory conditions. Combination drugs that contain these different categories of medications are available both OTC and by prescription. These combination product ingredients change rapidly, and this may be very confusing to the consumer. Often, OTC combinations purchased by patients contain medications that are not indicated for the condition for which the combination is labeled, and use can be counterproductive to clearing up symptoms. Many nighttime formulations contain alcohol and acetaminophen, which should not be consumed together. Some consumers use products incorrectly, taking an antihistamine for congestion when actually a decongestant is needed. Products with analgesics are often used by patients even in the absence of pain or fever. Many consumers, particularly the elderly, use these products without considering the ingredients and possible drug interactions with medications they are already taking, or preexisting medical conditions that may be adversely affected by certain medications. An example would be patients with hypertension, glaucoma, or urinary retention who take pseudoephedrine for congestion. Many patients self-prescribe OTCs for respiratory problems, so query patients specifically about use of OTC products. (See Chapter 7 for information on OTC use.)
Despite these problems, commonly prescribed combination medications are important in the treatment of respiratory problems and include antihistamine/decongestant combinations (e.g., Allegra-D, Claritin-D, Zyrtec-D), decongestant/expectorant combinations (e.g., Guaifed PD), and antitussive/expectorant combinations (e.g., Robitussin AC, DM), which can be useful in the treatment of multisymptom upper and lower respiratory conditions, if used appropriately. A knowledgeable clinician may suggest special formulations that are available OTC for patients with hypertension (e.g., Coricidin HBP, Coricidin HBP Cough & Cold), and several products are sugar and alcohol free. Despite the multiple combination preparations that are available both OTC and by prescription, many authorities recommend prescribing single-ingredient medications to avoid drug errors and overmedicating.
Therapeutic Overview of Upper Respiratory Infection and Allergic Rhinitis
The respiratory system is composed of the upper air passage structure, including the nasal passages, paranasal sinuses, pharynx, and larynx, and the lower air passages, including the trachea, bronchi, and lungs. Air moves through the upper passages (the conducting portion) into the lung (respiratory portion), where gas exchange occurs through the alveoli of the lung. The respiratory airway is lined with epithelial tissue that contains mucous glands and surface goblet cells that synthesize and secrete thick mucus. Below the larynx to the ends of the bronchi, the airways are lined with columnar epithelial cells that contain hair-like projections or cilia, which continuously beat in an upward motion toward the pharynx. Inhaled irritants stick to the mucus and are moved upward by the cilia to the pharynx, where they are swallowed or expectorated.
Pathophysiology
URIs are often viral in origin, and allergic rhinitis results from an allergic reaction that may have nothing to do with infection. A secondary bacterial infection is common in both URIs and allergic rhinitis that are untreated. Acute sinusitis and otitis media are the most common complications of URIs, although pneumonia may develop in susceptible patients. Critical decisions revolve around determining whether the problem is viral or bacterial, and whether the process has an allergic component.
Disease Process
Disease insult to the respiratory tract disturbs the normal physiologic processes: Production of mucus is dramatically increased, but the mucus thickens with dehydration or fever; the mucociliary mechanism is inhibited, and the cilia become sticky and unable to move. Patients cough or swallow enormous amounts of mucus.
URIs are caused by rhinoviruses, adenoviruses, and other viruses. Nasal congestion, watery rhinorrhea, and sneezing are present in 50% to 70% of patients within the first 3 days. Sore throat is reported by 50% of patients in the first 2 days. Other nonspecific symptoms include headache and general malaise. Symptoms are self-limiting, lasting a few days to a few weeks. On physical examination, the nasal mucosa is reddened and edematous with a watery discharge. Diagnosis is based on clinical observation, after absence of signs of bacterial infection is noted—purulent nasal discharge, red tympanic membrane, change in color of discharge, or high fever. URIs should be evaluated by a clinician, particularly if there is any risk of serious disease, including severe acute respiratory syndrome, which is a possible but unlikely differential in the United States.
Allergic Rhinitis
Seasonal allergic rhinitis is caused by a variety of irritations, most commonly allergy to pollen: trees in the spring, grasses in the summer, and ragweed in the fall. Perennial allergic rhinitis usually is caused by allergy to dust, molds, or mites. The symptoms may be similar to URI symptoms, except that they may be more persistent, may fluctuate, and often are related to exposure to allergens. Sneezing, injected conjunctiva, watery itchy eyes, red edematous eyelids, and watery rhinorrhea are often prominent. On physical examination, the turbinates may be pale or violaceous because of venous engorgement rather than red and erythematous as in URI.
Mechanism of Action
Decongestants are sympathomimetic amines that act to stimulate β-adrenergic receptors of vascular smooth muscle and cause vasoconstriction. This results in nasal decongestion, contraction of gastrointestinal and urinary sphincters, pupil dilation, and decreased pancreatic β-cell secretion. Pseudoephedrine also has β-adrenergic properties that cause relaxation of the bronchi.
In the sympathetic nervous system, adrenergic effector cells contain two distinct receptors, the α- and β-receptors. Sympathomimetic drugs mimic the action of norepinephrine on sympathetic effector organs, thereby affecting the adrenergic receptors. Important α-adrenergic activities include (1) vasoconstriction of arterioles, leading to increased blood pressure; (2) dilation of the pupils; (3) intestinal relaxation; and (4) bladder sphincter contraction. β-Receptors are divided into β1– and β2-receptors because some drugs affect some, but not all, β-receptors. β1-adrenergic activity includes (1) cardioacceleration and (2) increased myocardial contractility, whereas β1 stimulation leads to (1) vasodilation of skeletal muscle, (2) bronchodilation, (3) uterine relaxation, and (4) bladder relaxation.
Pseudoephedrine HCl/phenylephrine is an α-adrenergic receptor agonist (sympathomimetic) that produces vasoconstriction by stimulating α-receptors in the mucosa of the respiratory tract. It also reduces tissue edema and nasal congestion, increases nasal airway patency, promotes drainage of sinus secretions, and opens obstructed eustachian ostia. Pseudoephedrine also is used in the illegal manufacturing of methamphetamine. State and federal regulations now restrict the sale of pseudoephedrine, and it is stored behind the pharmacy counter. In some states, it is available only by prescription. Several manufacturers are using formulations that contain phenylephrine in nonprescription preparations.
Phenylephrine acts directly on α-adrenergic receptors and can be administered orally or topically to relieve nasal congestion in URI, sinusitis, and allergic rhinitis. The efficacy of oral phenylephrine has not been studied extensively.
Nasal sprays or inhaled (topical application of) decongestants to the nasal mucous membranes cause vasoconstriction, resulting in shrinkage, which helps to promote drainage and improve breathing through the nasal passages. These inhaled agents produce reduced systemic effects compared with oral preparations, achieving decongestion without causing sudden or wide changes in blood pressure, cardiac stimulation, or vascular redistribution.
Oxymetazoline is a topical direct-acting sympathomimetic amine that acts on the α-adrenergic receptors of the nasal mucosa, causing vasoconstriction and resulting in decreased blood flow and decreased nasal congestion.
Antihistamines
Antihistamines compete for histamine at the H1-receptor sites and are used to treat immunoglobulin (Ig)E-mediated allergy. Antihistamine therapy is helpful in treating allergic rhinitis and urticaria in most, but not all, patients. Antihistamines antagonize the pharmacologic effects of histamine. They do not inactivate histamine or block histamine release, antibody production, or antigen–antibody interactions. They also have anticholinergic (drying), antipruritic, and sedative effects to varying degrees. These drugs are classified by the amount of sedation they cause. Azelastine is a topical antihistamine nasal spray with few adverse systemic side effects that is used to treat allergic and vasomotor rhinitis.
Intranasal Corticosteroids
The steroids used in intranasal products have potent glucocorticoid and weak mineralocorticoid activity. Glucocorticoids inhibit cells, including mast cells, eosinophils, neutrophils, macrophages, lymphocytes, and mediators such as histamine, leukotrienes, and cytokines. They exert direct local antiinflammatory effects with minimal systemic effects. Intranasal corticosteroids effectively control the four major symptoms of allergic rhinitis: rhinorrhea, congestion, sneezing, and nasal itch. They are helpful in managing moderate to severe disease and are used in treating both seasonal and perennial allergic rhinitis. These medications must be used consistently on a daily basis for effectiveness, and maximum effects may not be noted for several days to weeks. For details on the immune system, see Chapter 68.
Intranasal Mast Cell Stabilizers
Cromolyn sodium is an OTC intranasal mast cell stabilizer that is used as a preventative agent that is taken in advance of allergen exposure. It is an antiinflammatory agent that has no intrinsic bronchodilator, antihistaminic, vasoconstrictor, or glucocorticoid activity. Cromolyn inhibits sensitized and mast cell degranulation that occurs after exposure to specific antigens. The drug inhibits the release of mediators, histamine, and slow-reacting substance of anaphylaxis (SRS-A) from the mast cell. It inhibits calcium from entering the mast cell, resulting in the prevention of mediator release. It is effective in reducing rhinorrhea, sneezing, and nasal itch, but it has minimal effect on nasal congestion. Cromolyn acts locally on tissue, inhibiting the release of chemical mediators by preventing mast cell degranulation. It has an excellent safety profile and minimal adverse effects consisting of nasal irritation, stinging, and sneezing. Cromolyn must be taken properly as a nebulized aerosol, inhaled through the mouth, or swallowed orally four to six times a day, and its effect may not be seen for 4 to 6 weeks to months. For details, see Chapter 14.
Leukotriene Receptor Antagonists
Montelukast sodium, a leukotriene receptor antagonist, causes inhibition of airway cysteinyl leukotriene receptors (CysTLs), which are products of arachidonic acid metabolism that are released from mast cells and eosinophils. The CysTL type 1 receptor is found in airway smooth muscle cells, airway macrophages, and proinflammatory cells such as eosinophils and myeloid stem cells. CysTLs are released from the nasal mucosa after allergen exposure and are associated with symptoms of allergic rhinitis.
Antitussives
Codeine and dextromethorphan both act centrally by acting on the cough center of the medulla to suppress cough. Dextromethorphan is the d-isomer of codeine that lacks the analgesic and addictive properties of codeine. However, it is not as effective as codeine in depressing the cough reflex. Benzonatate (dextromethorphan) anesthetizes stretch receptors in the respiratory passages, reducing the cough reflex at its source.
Expectorants
Guaifenesin increases respiratory tract fluid secretions and helps to loosen bronchial secretions by reducing adhesiveness and tissue surface tension. By reducing the viscosity of secretions, guaifenesin increases the efficacy of the mucociliary mechanism in removing accumulated secretions from the upper and lower airways. As a result, nonproductive coughs become more productive, less frequent, and less irritating to the airways. Guaifenesin products that are marketed as sustained or timed release have come under FDA scrutiny. Timed-release OTC drugs require FDA approval because the FDA must ensure that the product releases its active ingredients safely and effectively, sustaining the intended effect over the entire time in which the product is intended to work. Many sustained-release products had been on the market without receiving this approval. Guaifenesin is classed as questionably effective in some studies.
Treatment Principles
Evidence-Based Recommendations
Cardinal Points of Treatment
Allergic Rhinitis
Cough
Nonpharmacologic Treatment
 See Table 15-1 for a list of potential herbal-drug interactions.
See Table 15-1 for a list of potential herbal-drug interactions.
Pharmacologic Treatment
Decongestants
Antihistamines
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree



 Do not use cold or cough medications for children younger than 6 years.
Do not use cold or cough medications for children younger than 6 years. Complementary and Alternative Medications Used for Respiratory Problems That May Have Drug Interactions
Complementary and Alternative Medications Used for Respiratory Problems That May Have Drug Interactions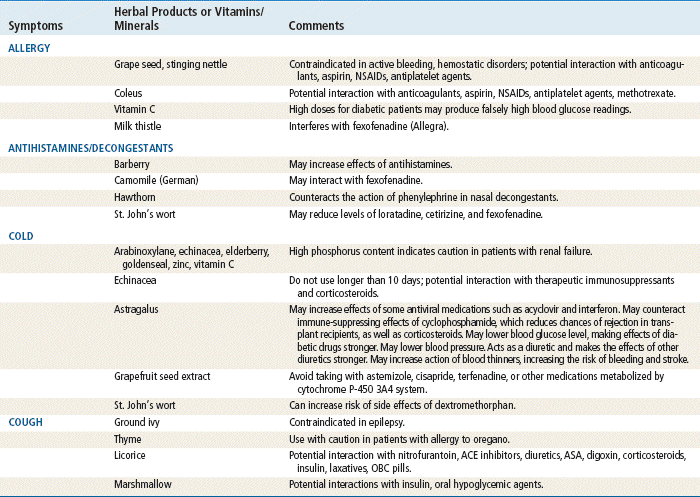
 Pseudoephedrine also is used in the illegal manufacturing of methamphetamine. State and federal regulations now restrict the sale of pseudoephedrine, and it is stored behind the pharmacy counter. In some states, it is available only by prescription.
Pseudoephedrine also is used in the illegal manufacturing of methamphetamine. State and federal regulations now restrict the sale of pseudoephedrine, and it is stored behind the pharmacy counter. In some states, it is available only by prescription.