Patient Story
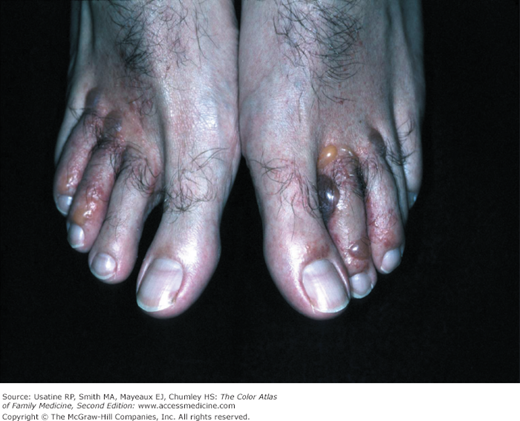
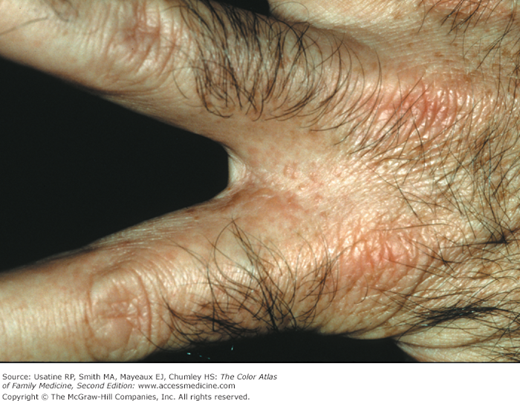
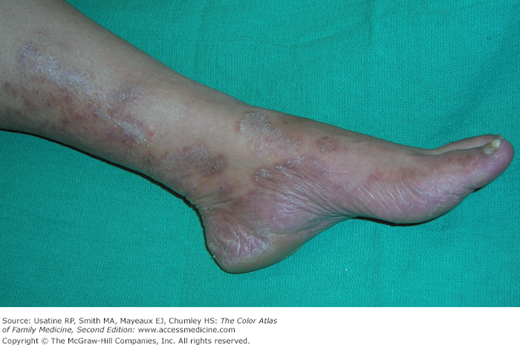
A 38-year-old man presents with an itchy rash on his hands and blisters on his feet for 1 week duration (Figure 140-1). Vesicular tinea pedis with bullae were present. The papules and vesicles between the fingers were typical of an autoeczematization reaction (Id reaction) (Figure 140-2). The patient was treated with an oral antifungal medication and a short burst of oral prednisone for the autosensitization reaction.
Introduction
Epidemiology
Etiology and Pathophysiology
- A cutaneous fungal infection most commonly caused by Trichophyton rubrum.1
- Trichophyton mentagrophytes and Epidermophyton floccosum follow in that order.
- T. rubrum causes most tinea pedis and onychomycosis.
Risk Factors
Diagnosis
Three types of tinea pedis
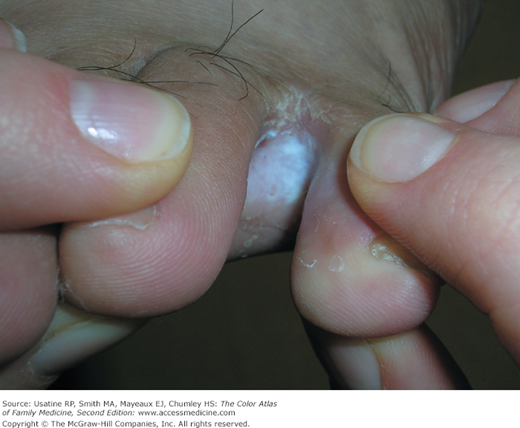
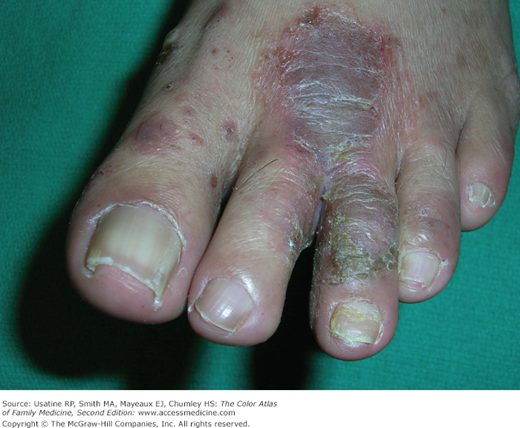
- Interdigital type—most common (Figure 140-3).
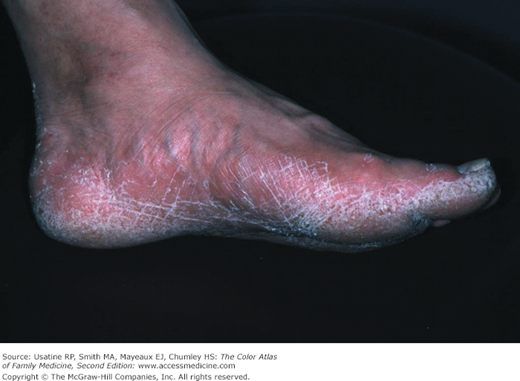
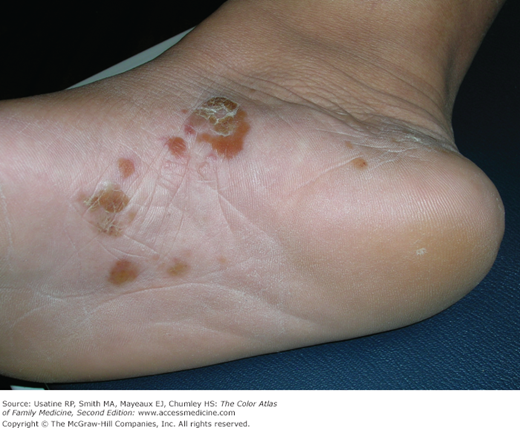
- Moccasin type (Figure 140-4 and 140-5).
- Inflammatory/vesicular type—least common (Figure 140-1).
Some authors describe an ulcerative type (Figure 140-6).
- Interdigital—white or green fungal growth between toes with erythema, maceration, cracks, and fissures—especially between fourth and fifth digits (Figure 140-3). The dry type has more scale and the moist type becomes macerated.
- Moccasin—scale on sides and soles of feet (Figure 140-4 and 140-5).
- Vesicular—vesicles and bullae on feet (Figure 140-6).
- Ulcerative tinea pedis is characterized by rapidly spreading vesiculopustular lesions, ulcers, and erosions, typically in the web spaces (Figure 140-7). It is accompanied by a secondary bacterial infection. This can lead to cellulitis or lymphangitis.
- Autosensitization (dermatophytid reaction; ID reaction) is a hypersensitivity response to the fungal infection causing papules on the hands (Figure 140-2).
- Examine nails for evidence of onychomycosis—fungal infections of nails may include subungual keratosis, yellow or white discolorations, dysmorphic nails (Chapter 193, Onychomycosis).
- Examine to exclude cellulitis that may show erythema, swelling, tenderness with red streaks tracking up the foot and lower leg (Chapter 120, Cellulitis).