Patient Story
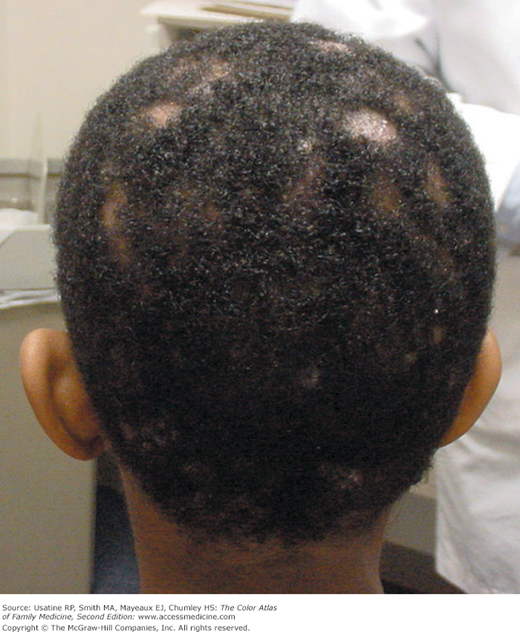
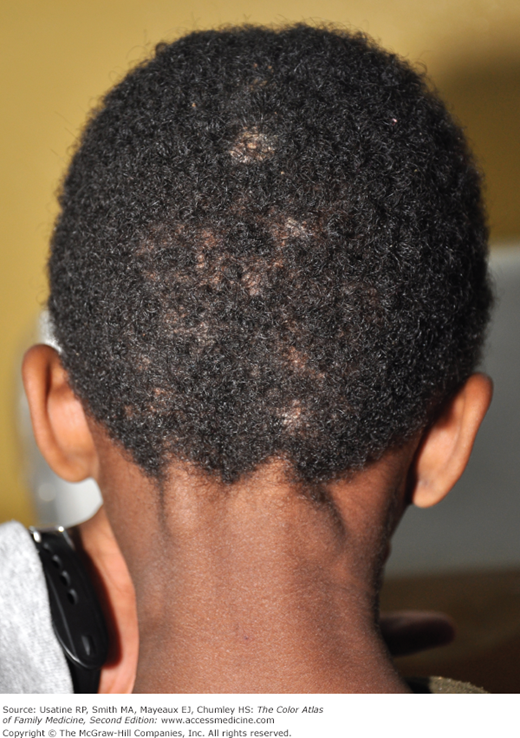
An 11-year-old boy has a history of 2 months of progressive patchy hair loss (Figure 137-1). He has some itching of the scalp but his mother is worried about his hair loss. Physical examination reveals alopecia with scaling of the scalp and broken hairs looking like black dots in the areas of hair loss. A KOH preparation is created by scraping an area of alopecia onto a slide. A few loose hairs are added to the slide before the KOH and cover slip are placed. Fungal elements are seen under the microscope. After 6 weeks of griseofulvin, the tinea capitis is fully resolved.
Introduction
Epidemiology
- Tinea capitis is more common in young, black boys.
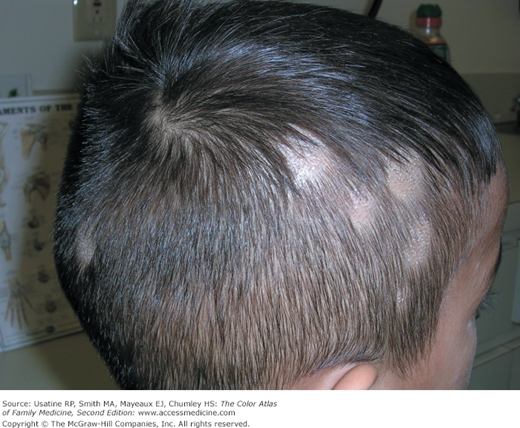
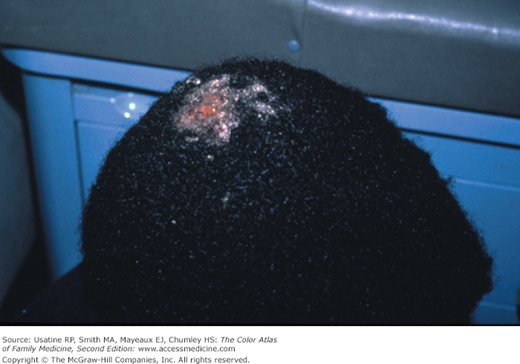
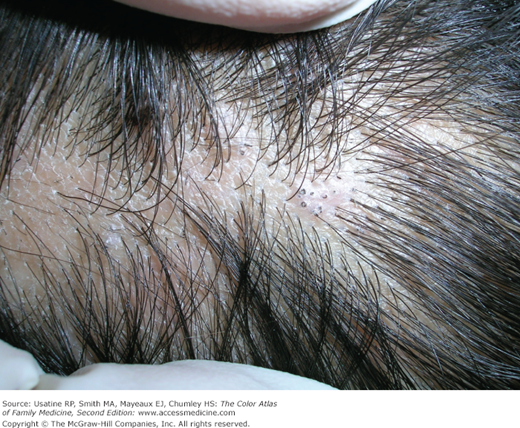
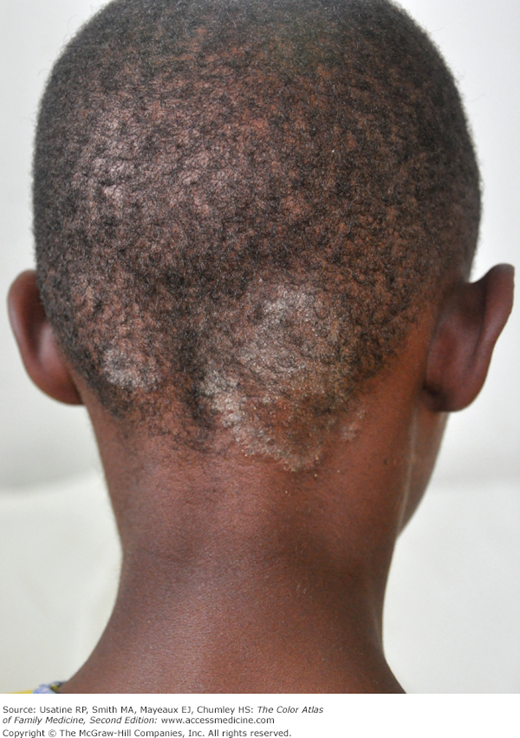
- Tinea capitis is the most common type of dermatophytoses in children younger than 10 years (Figures 137-1, 137-2, 137-3, 137-4, 137-5). It rarely occurs after puberty or in adults.1 The infection has a worldwide distribution.
- Combs, brushes, couches, and sheets may harbor the live dermatophyte for a long period of time.
- Spread from person to person with direct contact or through fomites.
- Occasionally spread from cats and dogs to humans.
Etiology and Pathophysiology
- Tinea capitis is a superficial fungal infection affecting hair shafts and follicles on the scalp but could involve the eyebrows and eyelashes.
- Caused by Trichophyton and Microsporum dermatophytes. The most common organism in the United States is Trichophyton tonsurans, which is associated with black dot alopecia. Microsporum canis is less common now than decades ago. M. canis is still highly prevalent in developing countries. The natural reservoir of M. canis is dogs and cats.
Risk Factors
Diagnosis
- The clinical appearance is often adequate to make the diagnosis.
- Confirm the diagnosis by scraping the scaling areas on the scalp and placing a few loose hairs on a microscope slide with KOH. (DMSO and a fungal stain will help.) Look for hyphae and spores (Figure 137-6). Look for endoectothrix invasion of the hair shaft with fungus.