Chapter 16 The Male Genital System
DEVELOPMENTAL DISORDERS
4 What are the complications of cryptorchidism?
Cryptorchidism is associated with an increased incidence of:
 Infertility: The testis retained in the abdominal cavity or the inguinal canal undergoes atrophy, and the seminal epithelium degenerates.
Infertility: The testis retained in the abdominal cavity or the inguinal canal undergoes atrophy, and the seminal epithelium degenerates.5 What is the difference between hypospadias and epispadias?
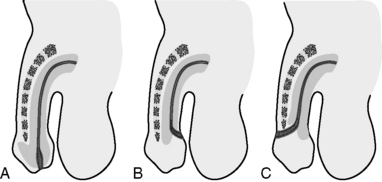
The urethral meatus is normally located at the tip of the penis. The anomaly in which the opening of the urethra is found on the ventral surface of the penile shaft is called hypospadias. Opening of the penile urethra on the dorsal surface of the penis is called epispadias. Hypospadias is more common (1:1000 newborn males) than epispadias (1:30,000 newborn males). Hypospadias is a less severe anomaly, and it usually occurs in an isolated form. Epispadias often involves a longer segment of the penis and is often combined with extrophy of the urinary bladder. See Fig. 16-1.
10 What are the other scrotal disorders that may be confused with hydrocele?
 Epididymal cysts: These cysts represent developmental recesses attached to the epididymis. If filled with sperm, they are called spermatocele.
Epididymal cysts: These cysts represent developmental recesses attached to the epididymis. If filled with sperm, they are called spermatocele. Varicocele: This term is used for the varicous dilatation of the scrotal veins (“bag of worms” noticed on palpation).
Varicocele: This term is used for the varicous dilatation of the scrotal veins (“bag of worms” noticed on palpation).INFECTIONS
11 What is epididymoorchitis?
 Sexually transmitted pathogens, such as Neisseria gonorrhoeae, Ureaplasma urealyticum, and Chlamydia trachomatis, are typically found in young adults.
Sexually transmitted pathogens, such as Neisseria gonorrhoeae, Ureaplasma urealyticum, and Chlamydia trachomatis, are typically found in young adults. Uropathogens, such as Escherichia coli, Pseudomonas aeruginosa, and Klebsiella, cause epididymoorchitis in the elderly suffering from prostatic hyperplasia and urinary tract infections.
Uropathogens, such as Escherichia coli, Pseudomonas aeruginosa, and Klebsiella, cause epididymoorchitis in the elderly suffering from prostatic hyperplasia and urinary tract infections.13 What are the common causes of ulceration on the glans penis?
 Genital herpes: Herpes simplex virus 2 (HSV-2) infection presents with vesicles that ulcerate and heal by formation of crusts.
Genital herpes: Herpes simplex virus 2 (HSV-2) infection presents with vesicles that ulcerate and heal by formation of crusts. Syphilis: Treponema pallidum infection may result in the formation of an ulceration (syphilitic chancre).
Syphilis: Treponema pallidum infection may result in the formation of an ulceration (syphilitic chancre).NEOPLASMS AND RELATED CONDITIONS
17 List the most important facts about testicular tumors
 Peak incidence in the 30- to 40-year-old age group. They are rare in prepubertal children and the elderly.
Peak incidence in the 30- to 40-year-old age group. They are rare in prepubertal children and the elderly. Serum tumor markers found in approximately 50% patients. These markers include alpha-fetoprotein (AFP) and human chorionic gonadotropin (hCG).
Serum tumor markers found in approximately 50% patients. These markers include alpha-fetoprotein (AFP) and human chorionic gonadotropin (hCG).18 What are the risk factors for testicular cancer?
 Sex chromosome abnormalities: Germ cell tumors occur at a rate of 25% in dysgenetic gonads, intersexes, hermaphrodites, and pseudohermaphrodites. Fortunately, these conditions are rare.
Sex chromosome abnormalities: Germ cell tumors occur at a rate of 25% in dysgenetic gonads, intersexes, hermaphrodites, and pseudohermaphrodites. Fortunately, these conditions are rare.