The Frozen Section: Historical Background, Technique, and Quality Assurance
Anthony G. Montag
History of the Frozen Section
The history of the frozen section as intraoperative consultation is intertwined with the development of pathology as a clinical specialty. Prior to the late 19th century, pathology or pathologic anatomy was an exercise in the gross correlation of premortem symptoms and physical examination with postmortem findings. As pathology developed into a distinct specialty in the late 19th century, its focus was largely research oriented; the correlation of pathologic findings to clinical disease continued to be carried out by practicing clinicians, frequently surgeons, well into the 20th century. The frozen section served a pivotal role in bringing microscopy into the clinical practice of medicine and the pathologist into the clinical management of patients.
Although autopsies were performed by ancient Egyptian and Greek physicians, the father of pathologic anatomy is generally regarded to be the Giovanni Morgagni (1682–1771) (Fig. 1.1), who held the chair of anatomy at the University of Padua from 1712 to 1771. Morgagni had served as student, prosector, editor, and biographer to the great surgeon and anatomist Antonio Valsalva, from whom he learned clinical–pathologic correlation. Morgagni’s 1761 treatise, The Seats and Causes of Disease, correlated the clinical and gross pathologic findings of 700 autopsies (1) and recognized the association of clinical symptoms with a specific organ, such as jaundice with abnormalities of the liver. He rejected Galen’s humoral theory of disease, dominant in Western medicine for 1,500 years, favoring diagnosis and treatment based on an understanding of underlying morbid anatomy.
The French anatomist Marie Francois Xavier Bichat (Fig. 1.2) published his Treatise on Membranes in General and on Various Membranes in Particular in 1800, followed by Physiological Researches on Life and Death in 1801 (1). Bichat realized that organs were themselves complex structures composed of tissues or membranes, and described 21 separate types including cartilage, fibrous tissue, serous membrane, glands, and hair. This reductionist approach to anatomy, breaking an
organ into tissue components, led Bichat to be considered as the father of histology. Ironically, his observations were made using only a hand lens; the microscopes available in the late 18th century had poor resolution and were regarded as unreliable novelties by most anatomists.
organ into tissue components, led Bichat to be considered as the father of histology. Ironically, his observations were made using only a hand lens; the microscopes available in the late 18th century had poor resolution and were regarded as unreliable novelties by most anatomists.
 Figure 1.2 Marie Francois Xavier Bichat (1771–1802), regarded as the father of histology for his description of 21 tissue types that comprise organs. (Courtesy of the National Library of Medicine.) |
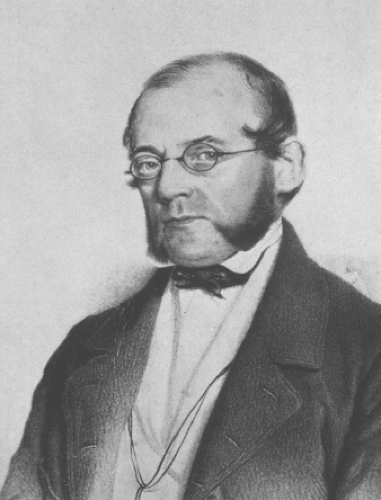 Figure 1.3 Carl von Rokitansky (1804–1878), father of gross pathology. (Courtesy of the National Library of Medicine.) |
Pathology as an independent specialty of medicine has its origins in Vienna with Carl Rokitansky (Fig. 1.3), who founded the first institute for pathology and is said to have personally performed 30,000 autopsies (2). Rokitansky’s treatise, General Pathologic Anatomy, put forth a general classification of diseases including blood dyscrasias, new growths, and congenital abnormalities (3). Regarded as the father of gross pathology, Rokitansky made little use of the microscope, although he did publish one treatise that included microscopy: On Connective Tissue Tumors of the Nervous System.
Rudolf Virchow (Fig. 1.4), Rokitansky’s pupil, spent much of his career at the Charity Hospital in Berlin, popularized microscopy in the study of pathology, and is regarded as the father of modern pathology (4). Virchow realized that at a more fundamental level, cells, rather than Bichat’s tissues, were the probable root of disease. In 1858, he published Cellular Pathology as Based Upon Physiological and Pathological Histology, which was widely accepted and established microscopic anatomy as integral to the understanding of pathology and medicine. His other major contribution was to refute the tenet of spontaneous generation of cells from inanimate
material, which still lingered in the cell theory published in 1839 by Theodor Schwann and Matthias Schleiden. Virchow asserted “Omnis cellula e cellula,” or that all cells come from cells. Ironically, in spite of the rise of cellular pathology as a concept, Virchow was primarily an experimental and autopsy pathologist, and the diagnosis of disease on living patients continued to be based on clinical impression and gross features, often as judged by the surgeon (5). Only rare attempts at diagnosis from a tumor fragment or biopsy had been attempted, and Virchow had his own reasons to be reluctant about the reliability of biopsy as a diagnostic technique. One of Virchow’s first attempts at biopsy diagnosis occurred in 1887 on specimens from the German Emperor Frederick III, who had developed a laryngeal mass. Virchow rendered a benign diagnosis; however, Frederick died the following year from laryngeal carcinoma (6). Although the lesion was probably inoperable at the time of biopsy, Frederick’s death led to the ascension of the more militaristic Wilhelm II, and may have contributed to the development of World War I. More directly, there was a lingering distrust of the technique of microscopic evaluation of biopsy specimens, which resulted in reluctance and disinterest in using microscopic pathology to direct the care of living patients.
material, which still lingered in the cell theory published in 1839 by Theodor Schwann and Matthias Schleiden. Virchow asserted “Omnis cellula e cellula,” or that all cells come from cells. Ironically, in spite of the rise of cellular pathology as a concept, Virchow was primarily an experimental and autopsy pathologist, and the diagnosis of disease on living patients continued to be based on clinical impression and gross features, often as judged by the surgeon (5). Only rare attempts at diagnosis from a tumor fragment or biopsy had been attempted, and Virchow had his own reasons to be reluctant about the reliability of biopsy as a diagnostic technique. One of Virchow’s first attempts at biopsy diagnosis occurred in 1887 on specimens from the German Emperor Frederick III, who had developed a laryngeal mass. Virchow rendered a benign diagnosis; however, Frederick died the following year from laryngeal carcinoma (6). Although the lesion was probably inoperable at the time of biopsy, Frederick’s death led to the ascension of the more militaristic Wilhelm II, and may have contributed to the development of World War I. More directly, there was a lingering distrust of the technique of microscopic evaluation of biopsy specimens, which resulted in reluctance and disinterest in using microscopic pathology to direct the care of living patients.
Several technical developments in the field of microscopy in the latter half of the 19th century led to its adoption as a reliable technique (2). The microscope itself was improved with the introduction of achromatic and apochromatic lenses to correct distortion and by the invention of the
substage condenser and oil immersion lens by Ernst Abbe. Consequently, German microscope manufacturers became the leaders in microscopy, and high-quality instruments were readily available. Histochemical stains from natural dyes were introduced in the mid-1800s, but the development of the aniline dye industry in Germany led to the introduction of many new stains between 1870 and 1900, including methylene blue, Gram, Congo red, and Mallory trichrome stains (7). Microtomes, including freezing microtomes, were introduced by the 1870s, and the introduction of formalin fixation and wax embedding led to more uniform histology.
substage condenser and oil immersion lens by Ernst Abbe. Consequently, German microscope manufacturers became the leaders in microscopy, and high-quality instruments were readily available. Histochemical stains from natural dyes were introduced in the mid-1800s, but the development of the aniline dye industry in Germany led to the introduction of many new stains between 1870 and 1900, including methylene blue, Gram, Congo red, and Mallory trichrome stains (7). Microtomes, including freezing microtomes, were introduced by the 1870s, and the introduction of formalin fixation and wax embedding led to more uniform histology.
Surgical practice also underwent a revolution in the late 19th century. In 1846, the first public demonstration of anesthesia using ether was carried out at the Massachusetts General Hospital. Oliver Wendell Holmes published his treatise on puerperal fever in 1847, establishing that it was frequently carried by the obstetrician from patient to patient, and called for more sanitation in hospitals and in the operating room. In 1867, Joseph Lister published on antisepsis, and proposed hand washing, gloves, and the use of carbolic acid. The result was that surgery became less painful, and the patient was more likely to survive. It also gave the surgeon the luxury of time, to better define the disease, and to tailor an operation that would not have been possible with a writhing patient.
By the end of the 19th century, all the elements were in place for surgical pathology to emerge as a clinical specialty, yet the use of biopsy to make a definitive diagnosis before surgery was seldom done. Pathology emerged as an academic pursuit, using microscopy to correlate gross and microscopic findings with clinical history and to classify disease; however, in most cases only on autopsy or material from definitive surgeries. For many surgical cases, clinical–pathologic evaluation was performed by the surgeon, often by gross examination only. This practice was reinforced by the tradition of academic surgeons spending a year or two in pathology departments in Europe, virtually none of which were handling biopsy material and most of which were grounded in autopsy pathology and experimental pathology. This dichotomy continued in academic centers well past the middle of the 20th century with the tradition of having a separate group of research faculty involved in autopsy pathology. As a consequence, many of the advances in the application of pathology to living patients took place in departments of surgery or gynecology, or in clinically oriented private hospitals and clinics.
William Halsted, Chief of Surgery of the new Johns Hopkins Hospital, requested the first intraoperative frozen section be done by the pathologist William Welch in 1891 (8). Welch had studied pathology extensively in Europe and had established the first hospital pathology laboratory in Bellevue Hospital Center, New York, prior to being recruited to Johns Hopkins. Halsted scheduled the frozen section on a suspected breast cancer case, and Welch prepared a slide using a carbon dioxide freezing microtome, but not before Halsted had concluded the case. Subsequently, Thomas Cullen, who had studied in Germany and learned a technique for
freezing formalin-fixed tissue, published a frozen section method in the Johns Hopkins Bulletin in 1895. The fixation step required before freezing the tissue block meant the procedure still took nearly an hour to complete.
freezing formalin-fixed tissue, published a frozen section method in the Johns Hopkins Bulletin in 1895. The fixation step required before freezing the tissue block meant the procedure still took nearly an hour to complete.
Although several other rapid frozen section methods were subsequently published in Europe, it is generally accepted that the standard cryostat method used today was first published in JAMA in 1905 by Louis Wilson of the Mayo Clinic (9). Wilson used a dextrin solution to embed the tissue and a carbon dioxide freezing microtome to produce the sections. By using methylene blue and reading the slides without permanent mounting, the technique could be performed in a few minutes as opposed to an hour for Cullen’s method. This method rapidly became a routine at the Mayo Clinic, and was adopted by other clinical centers. Most centers today include a brief fixation step before staining in hematoxylin and eosin, followed by permanent mounting, but the essential technique is largely unchanged (10).
Unfortunately, standard textbooks of pathology in the early 20th century continued to feel that the rapid frozen section technique was unreliable, and the technique was not widely adopted until after the late 1920s. In many academic centers, pathologists continued to regard diagnostic pathology as outside the interest of the pathology department. The American Society of Clinical Pathology was formed in 1922 to elevate the status of the pathologist as a physician who provided clinical services for live patients, and the frozen section consultation was one of the first services promoted by the organization (11,12).
A strong proponent of the frozen section was Dr. Joseph Bloodgood, a surgeon at Johns Hopkins. Prior to the 1920s, he had been skeptical of the frozen section technique, believing that an experienced surgeon could recognize the nature of a tumor with the naked eye (13). Beginning in 1927, Bloodgood began a campaign to promote the frozen section as a medical standard (14). He submitted editorials to major regional medical journals and, in an editorial in JAMA




Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree




