Surgical Anatomy of the Thyroid, Parathyroid, and Adrenal Glands
Clive S. Grant
Success in the surgical management of a patient can be conveniently divided into three phases: preoperative, intraoperative, and postoperative. Vitally important is the preoperative decision making and planning; an expertly performed operation for a wrong reason is still a bad operation. However, if the preoperative process is correctly conceived, at least in an elective procedure, a perfectly executed operation guarantees a smooth postoperative course in a high percentage of patients. The foundation for this operative success is a thorough knowledge of surgical anatomy. Anatomy to anatomists or pathologists is different from surgical anatomy. Because surgeons operate through limited incisions and must preserve function wherever possible, as well as control or prevent bleeding, the “anatomist’s anatomy” must be applied from the surgeon’s perspective. An attempt has been made to
amalgamate the two forms of anatomy in the following sections to give a broad perspective (the anatomist’s view as well as the perspective of the surgeon).
amalgamate the two forms of anatomy in the following sections to give a broad perspective (the anatomist’s view as well as the perspective of the surgeon).
The surgical anatomy of the thyroid and parathyroid glands is so closely interrelated that much of what is important to one proves equally important to the other. Because of this overlap, the overall anatomic relationships of the region are covered in the Thyroid section, and the differences or additions as they relate specifically to parathyroid disease are noted in the Parathyroid section.
Thyroid
Embryology
From a median entodermal diverticulum on the ventral wall of the pharyngeal gut, in approximately the fourth week of embryologic development, the thyroid descends from the posterior tongue (foramen cecum) in front of the pharynx as a bilobed diverticulum. It initially remains attached to the pharynx by a hollow tube, the thyroglossal duct, which attaches to the foramen cecum. At the end of the second month, the thyroid reaches its final position in front of the trachea; and the thyroglossal duct tissue, which has become solid, usually breaks up and disappears. Distal persistence of the solid duct is represented by the pyramidal lobe of the thyroid. If parts of the ductal epithelium persist, the secretion of the epithelium expands the remnant tube, which is closed at both ends, into a cystic mass filled with colloid-like material—a thyroglossal duct cyst. It rarely has a connection either to the skin or the tongue unless it has been infected and drained or previously operated on. Cysts can develop anywhere along the course of the thyroglossal duct but are most typically found overlying the hyoid bone in the midline just above the thyroid cartilage. Adjacent to the primary persistent thyroglossal duct remnants, other smaller duct and mucus-secreting gland remnants are often found.
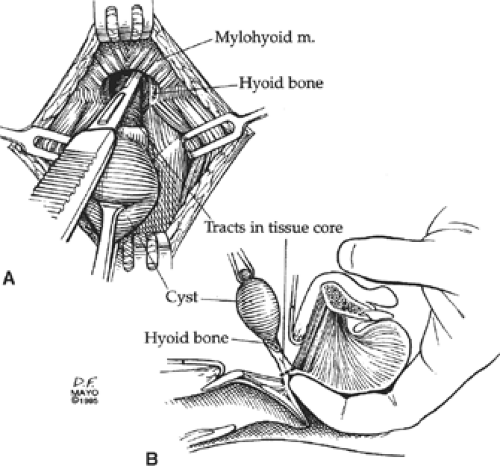
To prevent cyst recurrence, the duct and remnants can be encompassed in a core of tissues that should be excised from the cyst through the mylohyoid muscle to the base of the tongue, the site of the foramen cecum (Fig. 1). In addition, because the hyoid bone fuses in the midline in close proximity to the thyroglossal duct, the duct can pass either anterior or posterior, or even course through the bone. The central portion of the hyoid bone should, therefore, be excised as part of the operation for a thyroglossal duct cyst. Ectopic normal thyroid tissue or papillary thyroid carcinoma can develop in a thyroglossal duct cyst or anywhere along the tract of the thyroglossal duct. Lingual thyroid represents a total failure of thyroid descent, in which the entire thyroid is located at the foramen cecum of the tongue, under the mucosa.
Contributing perhaps less than 1% of the eventual thyroid mass, yet critically important in considering thyroid malignancy, are the lateral thyroid anlagen. Originating from the fourth pharyngeal pouches, corresponding to the ultimobranchial bodies, they are responsible for production of calcitonin from the parafollicular or C cells. They fuse with the posterior and medial aspect of each thyroid lobe. Medullary thyroid carcinomas evolve from these small parts of the thyroid.
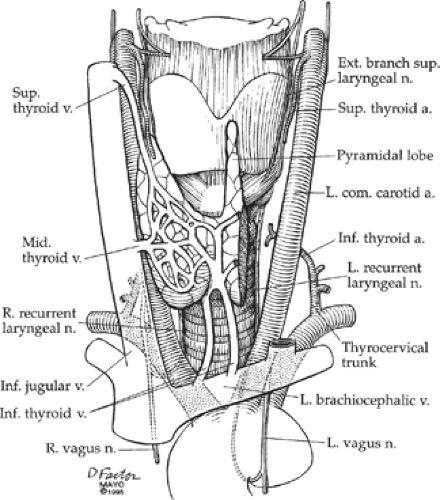
An overall view of the anatomy relevant to thyroid and parathyroid operations is shown in Figure 2. For optimal surgical exposure, the patient is positioned with a small pillow placed between the scapulae, and the neck is hyperextended, bringing the thyroid gland as far anterior as possible. The skin incision follows Langer lines transversely, optimally in a skin crease.
Dissection of Muscles
Beneath the skin and subcutaneous tissue is the thin platysma muscle, under which is a relatively avascular plane. In this plane, the superior and inferior flaps can be raised with minimal blood loss. Once the flaps have been developed, the strap muscles—the sternohyoid and sternothyroid muscles—are exposed. The more anterior sternohyoid muscles lie close together, but the midline between them can be identified as a thin line of fat and avascular fascia. Dissection along this line to separate these muscles is facilitated by lifting the muscles anteriorly so as to avoid the inferior thyroid veins, which course just below, running longitudinally over the trachea. Often bordering the midline along these muscles are the anterior jugular veins. These veins can be avoided but can be ligated as the need arises.
As the sternohyoid muscle is elevated, the underlying sternothyroid muscles are exposed. The fascia between these two muscles can be dissected for improved exposure. With the sternohyoid muscles retracted, as the sternothyroid muscle is dissected from the underlying thyroid lobes, care is taken to avoid the widely interconnecting venous network in the thyroid capsule. This caution is of particular importance in a larger goiter because the strap muscles can be thinned and splayed out across the bulging thyroid lobes and the large veins are in jeopardy. The insertion of the sternothyroid muscle into the thyroid cartilage can obscure the superior pole of the thyroid gland and can be partially transected for better exposure. Both the sternohyoid and sternothyroid muscles (as
well as the omohyoid muscle) are innervated by the ansa cervicalis, derived from the hypoglossal nerve and C1 through C3. These muscles can be partially or completely removed as necessary for cancer operations without any significant disability. The cricothyroid muscles run obliquely from the cricoid cartilage to the thyroid cartilage and are innervated by the external branch of the superior laryngeal nerve. This muscle and nerve should be carefully preserved because they serve the important function of fine-tuning the voice.
well as the omohyoid muscle) are innervated by the ansa cervicalis, derived from the hypoglossal nerve and C1 through C3. These muscles can be partially or completely removed as necessary for cancer operations without any significant disability. The cricothyroid muscles run obliquely from the cricoid cartilage to the thyroid cartilage and are innervated by the external branch of the superior laryngeal nerve. This muscle and nerve should be carefully preserved because they serve the important function of fine-tuning the voice.
The principal arterial blood supply of the thyroid gland comes from the paired superior and inferior thyroid arteries, and, to a much lesser degree, the thyroidea ima (Fig. 2). Even when all these arteries are ligated, remnants of thyroid often survive from other small branches derived from laryngeal and tracheoesophageal arteries. The superior thyroid artery is the first branch of the external carotid artery and courses inferiorly to reach the superior pole of the thyroid gland. It often branches at this point, with the main branch running over the anterior surface of the superior pole of the thyroid and the other smaller branches entering more posteriorly. The inferior thyroid artery usually arises from the thyrocervical trunk, runs superiorly behind the carotid artery, and then arches medially to the thyroid gland, coursing either perpendicular to or in a recurrent path to the thyroid gland. The thyroidea ima artery is encountered in less than 10% of patients and is almost never a relevant vessel except to ligate.
Dissection of Thyroid Lobe
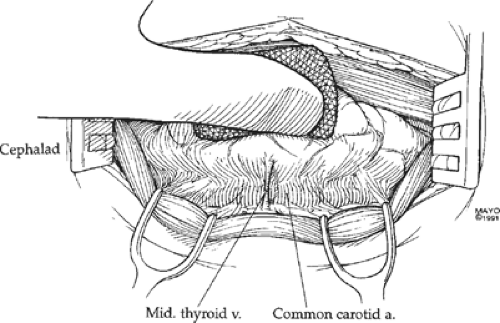
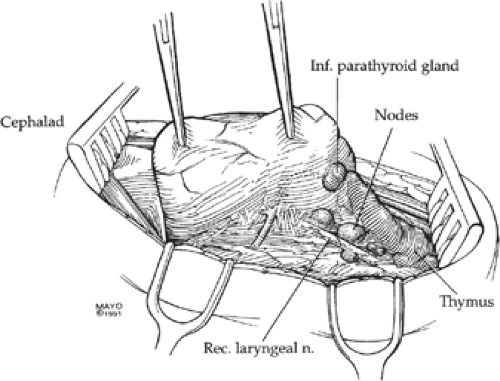
Once the strap muscles have been dissected laterally, the thyroid gland is elevated anteriorly and medially, opening an areolar plane overlying the carotid artery and traversed by one or more small middle thyroid veins (Fig. 3). These veins are ligated and transected, and the space anterior to the carotid from the thyroid cartilage inferiorly to the base of the neck can be dissected safely. This step exposes the transversely directed inferior thyroid artery and the obliquely coursing recurrent laryngeal nerve, a branch of the vagus nerve, which, on the right, wraps around the subclavian artery and passes behind the carotid artery to ascend in the tracheoesophageal groove (Fig. 4). On the left, the recurrent laryngeal nerve crosses the arch of the aorta, loops under it, adjacent and lateral to the ligamentum arteriosum, and ascends in the tracheoesophageal groove. Adjacent and mostly anterior to the recurrent laryngeal nerve are the tracheoesophageal lymph nodes, which are a common site of metastasis in papillary and medullary thyroid carcinoma. Removal of these nodes requires care to protect the recurrent laryngeal nerve; it should preserve not only the inferior parathyroid gland but also its blood supply, which usually crosses anterior to the recurrent laryngeal nerve. Damage to the recurrent laryngeal nerve on one side causes vocal cord paralysis and hoarseness and prevents complete closure of the vocal cords to protect the trachea. This incomplete closure results in choking, especially when the patient consumes fluids. Bilateral nerve injury jeopardizes the airway and usually requires at least a temporary tracheostomy. When the right subclavian artery anomalously originates directly from the aortic arch as its fourth branch, it
passes behind the trachea and esophagus. The right recurrent nerve, therefore, does not recur around this artery and takes a direct course from the vagus nerve to the larynx (Fig. 5). In this instance, although it emerges posterior to the carotid artery, its perpendicular course mimics the usual course of the inferior thyroid artery and must be distinguished from it.
passes behind the trachea and esophagus. The right recurrent nerve, therefore, does not recur around this artery and takes a direct course from the vagus nerve to the larynx (Fig. 5). In this instance, although it emerges posterior to the carotid artery, its perpendicular course mimics the usual course of the inferior thyroid artery and must be distinguished from it.
 Fig. 4. A non-recurrent, recurrent laryngeal nerve (on the patient’s right side) courses directly from the vagus to its insertion at the cricothyroid membrane. |
The inferior thyroid artery is usually the principal blood supply to both the superior and inferior parathyroid glands. These feeding vessels are small and fragile, often traveling in a course parallel, if not slightly anterior, to the parathyroid glands before reaching the vascular hila (Fig. 6). As the inferior thyroid artery intersects with the recurrent laryngeal nerve, it usually branches into superior and
inferior trunks. The superior trunk typically divides again with one branch anterior and another posterior to the recurrent laryngeal nerve. The inferior thyroid veins run vertically, anterior to the trachea, and are easily identified and controlled during the course of thyroidectomy. Accompanying these veins are the pretracheal lymph nodes, both infra- and supraisthmic (Delphian), which often contain metastatic thyroid cancer.
inferior trunks. The superior trunk typically divides again with one branch anterior and another posterior to the recurrent laryngeal nerve. The inferior thyroid veins run vertically, anterior to the trachea, and are easily identified and controlled during the course of thyroidectomy. Accompanying these veins are the pretracheal lymph nodes, both infra- and supraisthmic (Delphian), which often contain metastatic thyroid cancer.
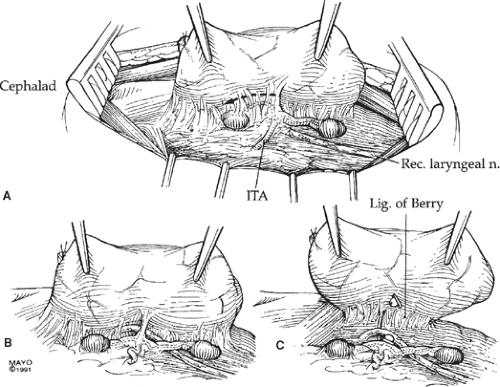
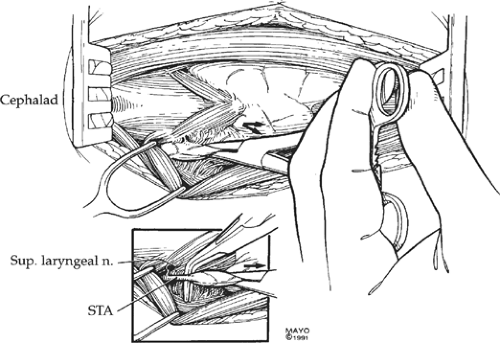
The superior thyroid artery and vein, which are sacrificed during thyroidectomy, must be separated from the external branch of the superior laryngeal nerve. Placing inferior and lateral traction on the superior pole of the thyroid gland usually distracts the artery away from the nerve, and the artery can be cleanly isolated and individually ligated (Fig. 7).
Once the vascular branches to the thyroid lobe have been transected and the nodes cleared, the posterior capsule of the thyroid is all that remains before the lobe is completely removed. To re-emphasize, a small vessel regularly courses in this dense posterior capsule (Berry ligament), and the recurrent laryngeal nerve is also commonly tethered anteriorly. Gentle dissection will expose the vessel for ligation and push the recurrent laryngeal nerve down and out of danger before the ligament is transected.
In addition to the pretracheal and tracheoesophageal lymph nodes already mentioned, thyroid cancer often metastasizes to lateral nodes. The routes of spread roughly follow the venous drainage. Cancers of the upper lobe, in addition to the primary drainage to the supraisthmic nodes, can involve the midjugular nodes, both anterior and lateral to the internal jugular vein, and occasionally extend superiorly along the vein to the base of the skull. Cancers of the mid- and lower thyroid lobes drain initially into the pretracheal and tracheoesophageal nodes, then to the mid- and lower jugular nodes and anterior mediastinal nodes.
Table 1 Compartments of Neck and Levels of Cervical Lymph Nodes | ||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
|
Modified Radical Neck Dissection
Important in the surgical management of papillary, medullary, and in some Hürthle cell carcinomas, lymph node metastases to the lateral internal jugular lymph nodes will necessitate a lymphadenectomy. Depending upon the extent of the dissection, various descriptive terms have been applied including regional, functional, selective, and modified radical neck dissection. Perhaps more important is the thorough, en bloc approach, and the neck compartments dissected. The anatomic boundaries of Compartments I to VI are summarized in Table 1, and graphically illustrated in Figure 8. Rarely used in thyroid cancer surgery is the classic radical neck dissection that implies sacrifice of the sternocleidomastoid muscle (SCM), internal jugular vein (IJ), and the spinal accessory nerve. Additionally, the submandibular triangle is virtually never dissected for thyroid cancer. Whereas in medullary thyroid carcinoma and node-positive Hürthle cell carcinoma, thorough dissection of Compartment VI is advised, controversy exists as to the extent and indications for this compartment dissection in papillary cancer.
Whether a standard collar incision is extended vertically along the anterior border of the SCM, or a separate transverse incision is made higher in the neck, extensive subplatysmal flaps are developed.
Compartments Iii, Iv, and the Anterior Aspect of Compartment V
The dissection proceeds with dissecting the plane between the SCM and the strap muscles exposing the omohyoid muscle that is conveniently sacrificed (Figs. 9 and 10). This uncovers the lower aspect of the IJ and adjacent carotid sheath structures (carotid artery medially, IJ laterally, and
vagus nerve posteriorly between the other two). The lymph nodes to be removed extend from the base of the neck inferiorly, behind the clavicle and slightly behind the IJ anteriorly, and laterally behind the SCM. Retracting the IJ anteriorly and medially (protecting the adjacent vagus nerve), areolar tissue is easily dissected laterally down to the floor of the neck onto the prevertebral fascia extending laterally as the fascia overlying the anterior scalene muscle (Figs. 11 and 12). Running vertically on the anterior scalene muscle is the phrenic nerve that is crossed low in the neck by the transverse cervical artery (Fig. 13A,B), a branch of the thyrocervical trunk. This artery may be sacrificed, but care must be taken to preserve the phrenic nerve. The lateral border of the IJ may be used as a guide to dissect inferiorly, but it will join the subclavian vein, and on the left side, the thoracic duct. This duct runs adjacent to the esophagus in the chest, coursing up behind the carotid sheath structures, and loops up a short distance from medial to lateral behind the IJ, and then enters the subclavian vein near its junction with the IJ. Nodes near the clear-fluid-containing duct are commonly involved in thyroid cancer, and the duct is very vulnerable to injury. In adults, if injured, the thoracic duct may be ligated without harm. The dissection across the base of Compartment IV at the level of the clavicle is usually safe with only relatively small veins requiring control. After releasing the inferior attachments, and with dissection superiorly along the lateral border of the IJ, and safely elevating the packet of lymph nodes from the anterior scalene muscle, the packet of nodes and soft tissue can be retracted anteriorly, putting tension on the posterior attachments behind the SCM. Dissecting from inferior to superior, the cutaneous cervical plexus nerves (C 2 to 4) will be encountered as substantial nerves coursing obliquely down behind the SCM (Fig. 14A,B). With care, these nerves can be preserved without jeopardizing a good nodal dissection. Deeply situated at the inferior and lateral aspect of the dissection, coursing from behind the anterior scalene and in front of the middle scalene muscles are the brachial plexus trunks. The superior border of Compartment III is defined as the level of the hyoid bone or carotid bifurcation. Not infrequently, lymph nodes, located anterior to the carotid artery at the level of the bifurcation, are metastatically involved and may be overlooked if not intentionally sought.
vagus nerve posteriorly between the other two). The lymph nodes to be removed extend from the base of the neck inferiorly, behind the clavicle and slightly behind the IJ anteriorly, and laterally behind the SCM. Retracting the IJ anteriorly and medially (protecting the adjacent vagus nerve), areolar tissue is easily dissected laterally down to the floor of the neck onto the prevertebral fascia extending laterally as the fascia overlying the anterior scalene muscle (Figs. 11 and 12). Running vertically on the anterior scalene muscle is the phrenic nerve that is crossed low in the neck by the transverse cervical artery (Fig. 13A,B), a branch of the thyrocervical trunk. This artery may be sacrificed, but care must be taken to preserve the phrenic nerve. The lateral border of the IJ may be used as a guide to dissect inferiorly, but it will join the subclavian vein, and on the left side, the thoracic duct. This duct runs adjacent to the esophagus in the chest, coursing up behind the carotid sheath structures, and loops up a short distance from medial to lateral behind the IJ, and then enters the subclavian vein near its junction with the IJ. Nodes near the clear-fluid-containing duct are commonly involved in thyroid cancer, and the duct is very vulnerable to injury. In adults, if injured, the thoracic duct may be ligated without harm. The dissection across the base of Compartment IV at the level of the clavicle is usually safe with only relatively small veins requiring control. After releasing the inferior attachments, and with dissection superiorly along the lateral border of the IJ, and safely elevating the packet of lymph nodes from the anterior scalene muscle, the packet of nodes and soft tissue can be retracted anteriorly, putting tension on the posterior attachments behind the SCM. Dissecting from inferior to superior, the cutaneous cervical plexus nerves (C 2 to 4) will be encountered as substantial nerves coursing obliquely down behind the SCM (Fig. 14A,B). With care, these nerves can be preserved without jeopardizing a good nodal dissection. Deeply situated at the inferior and lateral aspect of the dissection, coursing from behind the anterior scalene and in front of the middle scalene muscles are the brachial plexus trunks. The superior border of Compartment III is defined as the level of the hyoid bone or carotid bifurcation. Not infrequently, lymph nodes, located anterior to the carotid artery at the level of the bifurcation, are metastatically involved and may be overlooked if not intentionally sought.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree