Patient Story
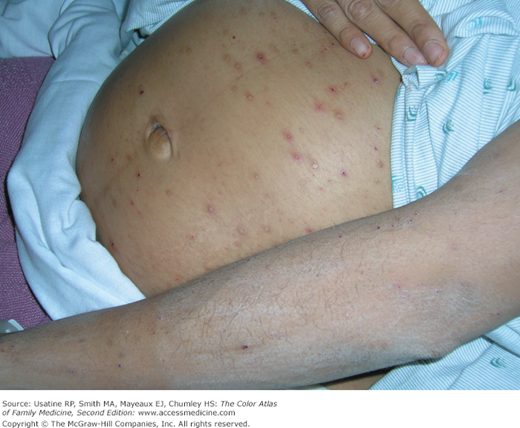
A 32-year-old G3P2 woman presents with persistent itching in her 31st week of pregnancy. The itching is constant and worse at night. Her pregnancy had been uncomplicated and she has no past history of medical problems. Many excoriations are noted and there are no blisters (Figure 74-1). She has no jaundice or scleral icterus. Her transaminases were greater than 300 and her total bilirubin was elevated at 2.1. Her bile salts were elevated and her hepatitis panel was negative. The ultrasound showed gallstones but no obstruction was seen. A diagnosis of “intrahepatic cholestasis of pregnancy” was made and the patient was treated with oral ursodiol (a bile salt binding agent) and topical 1% hydrocortisone cream. The bile salts and transaminases were decreased and the patient’s pruritus improved but did not resolve until after delivery.1
Introduction
Maternal skin and skin structures undergo numerous changes during pregnancy. There are two general categories of pregnancy-associated skin conditions: (a) benign skin conditions associated with normal hormonal changes of pregnancy (striae gravidarum, hyperpigmentation, hair and vascular changes), and (b) pregnancy-specific dermatoses (prurigo of pregnancy, intrahepatic cholestasis of pregnancy).
Synonyms
Epidemiology
- Almost all pregnant women develop some increase in skin pigmentation. This usually occurs in discrete areas, probably because of differences in melanocyte density.
- Striae gravidarum (stretch marks) occur in up to 90% of pregnant women by the third trimester.2
- Spider telangiectasias occur in approximately 66% of light-complected and 10% of dark-complected pregnant women, primarily appearing on the face, neck, and arms. The condition is most common during the first and second trimesters.3 Palmar erythema occurs in approximately two-thirds of light-complected and up to one-third of dark-complected pregnant women.2
- Hemorrhoidal, saphenous, and vulvar varicosities occur in approximately 40% of pregnant women.3
- Prurigo of pregnancy (now called atopic eruption of pregnancy) occurs with an incidence of approximately 1 in 300 to 1 in 450 pregnancies.4,5
- Intrahepatic cholestasis of pregnancy occurs in approximately 1 of 146 to 1293 pregnancies in the United States.3
Etiology and Pathophysiology
- The most common skin pigmentary change is darkening of the linea alba (Figure 74-2), which is then called the linea nigra.6 It may span from the pubic symphysis to the umbilicus or all the way to the xiphoid process.
- The skin around the areola may also darken and develop a reticular type pattern. Other anatomic areas that develop hyperpigmentation are the nipples, axillae, vulva, perineum, anus, inner thighs, and neck.7 Darkening may also occur in nevi during pregnancy.
- As pregnancy progresses, increased eccrine activity may result in hyperhidrosis (increased sweating) and/or miliaria (“prickly heat”).8 Apocrine activity decreases during pregnancy but increases postpartum, so hidradenitis suppurativa improves during pregnancy but may rebound later.8
- Hypertrophy of sebaceous glands produces small, brown papules on the areolae (Montgomery tubercles, Figure 74-3) in up to half of pregnant women. They usually regress postpartum.8
- Stretch marks (striae distensae, striae gravidarum) begin as pink/violaceous linear patches in the sixth to seventh month of gestation and are a common cosmetic concern among pregnant women (Figure 74-4). They evolve into hypopigmented linear depressions. They are most common on the abdomen, breasts, and thighs, but may also arise on the lower back, buttocks, and upper arms.8 The cause of striae is multifactorial and includes physical factors (e.g., actual stretching of the skin) and hormonal factors adrenocortical (e.g., steroids, estrogen, and relaxin). Although striae fade postpartum, they do not completely disappear.
- Spider angiomas, arterial spiders, or spider nevi may develop, especially in whites. They occur mostly on the neck, face, upper chest, arms, and hands.6 Almost all regress postpartum.
- Palmar erythema may develop and may be limited to the thenar or hypothenar eminence, or may be diffuse and mottled.8
- Acrochordons (skin tags) may develop, enlarge, or increase on the face, neck, axillae, chest, groin, and inframammary area during the second half of pregnancy. Some may regress postpartum.9
- Keloids, leiomyomas, dermatofibromas, and neurofibromas may enlarge during pregnancy.9
- Scalp hair appears thicker during pregnancy as a result of slowing of the normal progression of hairs to the telogen (“resting”) stage, thereby creating a relative increase in anagen hair. Hair loss (telogen effluvium) is common 1 to 5 months postpartum as the percentage of telogen hairs in the scalp normalizes or increases (Figure 74-5).9 Telogen effluvium resolves within 15 months postpartum, but the scalp hair may never return to prepregnancy thickness.9
- Hirsutism may occur on the face, arms, legs, back, and suprapubic region.9 Hirsutism appears to be a result of increased levels of ovarian and placental androgens. Frontoparietal hair loss (androgenic alopecia) may develop late in pregnancy but usually resolves postpartum.
- Saphenous, vulvar, and hemorrhoidal varicosities may increase in number and/or size (see Chapter 66, Hemorrhoids). This may be because of increased blood volume, increased venous pressure, or genetic predisposition. Jacquemier sign refers to venous distention in the vestibule and vagina and is associated with vulvar varicosities, which are particularly difficult to treat.8 Varicosities regress, at least partially, postpartum.
- Vascular type tumors may develop or enlarge during pregnancy. Pyogenic granulomas (Figure 74-6

Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree