Perforated Duodenal Ulcer
James W. Maher
Silas M. Chikunguwo
Introduction
Brief Historical Perspective
Muralto first described duodenal ulcers at autopsy in 1688. Crisp published a landmark paper in which he described symptomatology of perforated peptic ulcers in 1843. Therapy of perforated ulcer has been a hallmark of General Surgical practice for well over 100 years. Virtually, every American Board of Surgery candidate can rely on seeing a question in their oral examination regarding management of this entity; however, our understanding of the problem has changed drastically over the last 20 years. The last 10 years of the 20th century witnessed a scientific revolution in our
recognition of the role that infection with Helicobacter pylori plays in producing the gastric acid hypersecretion that characterizes peptic ulcer. This hypersecretion, and attempts to control it, had in fact been the subject of a previous scientific revolution during the 1950s and 1960s that had shepherded a transition from surgical therapy that focused on resection of acid-secreting mucosa via subtotal gastrectomy to eliminating the hypersecretion by section of the vagus nerves. This revolution was best summarized by the Nobel Prize-nominated vagotomy pioneer, Lester Reynolds Dragstedt, whose philosophy regarding the controversy between the choice of resection versus vagotomy was best summarized in his remark that “the stomach is a mighty handy organ to take to the dinner table”. This is a reminder that is even more valid today. This concept of duodenal ulcer as an infectious disease, not to mention the wide “over the counter” availability of H2 blockers and proton pump inhibitors, has led to a marked decrease in the incidence of complications such as: intractability and/or gastric outlet obstruction that formerly might have led to surgery. Unfortunately, our new understanding has not yet led to any detectable changes in incidence of ulcer perforation. Thus, ulcer perforation continues to be an important, even if somewhat diminished, staple of surgical practice. Opportunities for prevention must necessarily focus on the two etiologies most responsible for perforations: treatment of H. pylori infection and use of nonsteroidal anti-inflammatory drugs (NSAID). However, this is a formidable undertaking when one considers that ∼50% of the population of the United States harbors H. pylori infection and that there is a ubiquitous availability of NSAIDs as over-the-counter remedies. Any prospects for improvement in prognosis probably lie with general advances in acute surgery. The decrease in the incidence of uncomplicated duodenal ulcers over the past three to four decades has been somewhat attributable to our increased understanding of the multiple etiologies, risk factors, and epidemiology of duodenal ulcer disease, however, honest observers will note that the decrease in duodenal ulcer disease predated our understanding of its infectious nature as well as the remarkable therapeutic medications that are now so widely available.
recognition of the role that infection with Helicobacter pylori plays in producing the gastric acid hypersecretion that characterizes peptic ulcer. This hypersecretion, and attempts to control it, had in fact been the subject of a previous scientific revolution during the 1950s and 1960s that had shepherded a transition from surgical therapy that focused on resection of acid-secreting mucosa via subtotal gastrectomy to eliminating the hypersecretion by section of the vagus nerves. This revolution was best summarized by the Nobel Prize-nominated vagotomy pioneer, Lester Reynolds Dragstedt, whose philosophy regarding the controversy between the choice of resection versus vagotomy was best summarized in his remark that “the stomach is a mighty handy organ to take to the dinner table”. This is a reminder that is even more valid today. This concept of duodenal ulcer as an infectious disease, not to mention the wide “over the counter” availability of H2 blockers and proton pump inhibitors, has led to a marked decrease in the incidence of complications such as: intractability and/or gastric outlet obstruction that formerly might have led to surgery. Unfortunately, our new understanding has not yet led to any detectable changes in incidence of ulcer perforation. Thus, ulcer perforation continues to be an important, even if somewhat diminished, staple of surgical practice. Opportunities for prevention must necessarily focus on the two etiologies most responsible for perforations: treatment of H. pylori infection and use of nonsteroidal anti-inflammatory drugs (NSAID). However, this is a formidable undertaking when one considers that ∼50% of the population of the United States harbors H. pylori infection and that there is a ubiquitous availability of NSAIDs as over-the-counter remedies. Any prospects for improvement in prognosis probably lie with general advances in acute surgery. The decrease in the incidence of uncomplicated duodenal ulcers over the past three to four decades has been somewhat attributable to our increased understanding of the multiple etiologies, risk factors, and epidemiology of duodenal ulcer disease, however, honest observers will note that the decrease in duodenal ulcer disease predated our understanding of its infectious nature as well as the remarkable therapeutic medications that are now so widely available.
Epidemiology
Duodenal ulcers are one manifestation of what has been referred to as peptic ulcer disease (PUD) and account for two-thirds of all peptic ulcers. Population studies have shown that peptic ulceration remains a major public health problem worldwide. The lifetime frequency of PUD in the United States has been shown to be ∼10%. Studies by Logan and associates indicated that, in the United States alone, some 300,000 new cases of peptic ulcer are diagnosed each year. The frequency rates of duodenal ulcers in other countries are variable and have been shown to be primarily associated with H. pylori and use of NSAIDs. Although, as noted above, the surgical treatment of PUD has been fundamentally transformed, mortality and morbidity resulting from duodenal ulceration with perforation remain substantial. For example, the rate of peptic ulcer complication in patients of all age groups is approximately 1% to 2%. Lifetime risk of duodenal perforation in patients with duodenal ulceration who do not receive therapy has been reported to be 10%. In patients who require surgical interventions for complications, such as perforation, the mortality rate is significantly higher in the elderly than in other age groups. Recent studies have indicated that the life prevalence of duodenal ulcers to be 11% to 14% for males and approximately 8% to 11% for women. The epidemiology of perforated duodenal ulceration has changed significantly. The male to female ratio has decreased from 10:1 to 1.5:1, and the median age has increased to >60. As the proportion of patients with associated disease increases, the mortality and morbidity have remained fairly constant in the last three decades despite improvements in general medical care.
Pathophysiology
Duodenal ulcers have been characterized by the presence of a well-demarcated break in the mucosa that may extend into the muscularis propria of the duodenum. It has been shown that >95% of duodenal ulcers are located within the first portion of the duodenum; most are <1 cm in diameter. Unlike gastric ulcers, which may be malignant in about 5% of cases, duodenal ulcers are benign. Duodenal perforation is the second most common complication of PUD (Schwartz) and occurs in as many as 10% of patients with PUD. Most perforations arise from ulcers in the anterior aspect of the duodenal cap. Studies have shown that 92% of perforated duodenal ulcers perforated through the anterior duodenal wall; 10% of these are also associated with a concurrent, bleeding ulcer along the posterior wall, the so-called kissing ulcer. H. pylori is a gram-negative spiral flagellated bacterium. The organism is uniquely designed for survival in the hostile acidic stomach environment. The urease produced by this organism breaks down urea to alkaline ammonia and CO2, which protects the bacterium from acid injury. The flagella and spiral structure allow penetration of the mucus and attachment of the bacteria to the gastric epithelial cell.
More than half the world population is infected with H. pylori. It appears to spread by fecal-oral transmission and rates of infection are inversely proportional to socioeconomic status. Gastric inflammation is present in virtually all infected patients. There is no state of colonization without pathology. Infection is enduring and is never cured spontaneously. Eradication with antibiotic therapy results in resolution of gastritis. In the United States, ∼80% of duodenal ulcer patient are infected and this contrasts with infection in ∼60% of gastric ulcers. Nevertheless, only 20% of infected individuals develop a peptic ulcer, thus the exact mechanisms producing ulceration are incompletely understood. Eradication of H. pylori infection in ulcer patients reduces the ulcer recurrence rate to well below 10%.
Under normal physiological conditions, the duodenal mucosa resists damage from the effects of gastric acid and pepsin, with the help of protective factors such as the mucous layer, bicarbonate secretion, and prostaglandins, which exert a protective effect. A duodenal ulcer occurs when an imbalance occurs between the protective factors above and the aggressive factors: acid and pepsin. Any process that increases gastric acidity (e.g., individuals with increased maximal and basal acid output), decreases prostaglandin production (e.g., NSAIDs), or interferes with the mucosa layer (e.g., H. pylori infection) can lead to PUD with its attendant increased risk of duodenal perforation. Full understanding of the pathophysiology and pathogenesis of duodenal ulcer perforation requires clear comprehension of the major etiologies and risk factors of PUD.
Etiologies and Risk Factors
The pathogenesis of PUD is multifactorial as previously noted. Nevertheless, there are several environmental and/or host factors, which contribute to duodenal ulcer formation by increasing gastric acid secretion or weakening the mucosal barrier. Full understanding of the pathophysiology and pathogenesis of duodenal ulcers and their perforation complications require a brief discussion of the two major etiologies: NSAIDs and H. pylori infection.
Environmental Factors
These have been said to include NSAID use, cigarette smoking, excessive alcohol intake, and extreme emotional or physical stress. In the Western countries, it is estimated that up to 30% of regular NSAIDs users have one or more ulcers. Both NSAIDs and aspirin interfere with the protective mucus layer by inhibiting mucosal cyclooxygenase activity and reducing levels of mucosal prostaglandins. Gastric acid also exacerbates NSAID injury and conversely, gastric acid suppression has been shown to partially protect against NSAID injury. However, the exact mechanism by which NSAIDs cause duodenal perforation has not been clearly defined.
NSAID use has been reported to increase the risk of ulcer perforation by five to eight times that of nonusers (Svanes) and NSAID is a factor in between one-fifth to one-third of perforations, the proportion increasing with increasing age.
Cigarette smoking is a risk factor for PUD and its complications. Furthermore, cigarette smoking may adversely affect the healing of peptic ulcerations and, in the absence of treatment for H. pylori, may predispose to relapses. Cigarette smoking does not appear to influence the relapse rate for peptic ulceration if H. pylori in patients has been eradicated. Nevertheless, at least one study has disputed the association between smoking and PUD. Smoking probably promotes peptic ulceration by increasing gastric acidity and maximal acid output and enhancing H. pylori proliferation. Smokers have been found to have decreased prostaglandin concentrations in their gastric and duodenal mucosa and smoking has been shown to inhibit acid-stimulated duodenal mucosal bicarbonate secretion. It is not clear which, if any, of these proposed mechanisms contributes to peptic ulceration in cigarette smokers.
Alcohol has also been thought to be a strong risk factor for peptic ulcer although there is little hard data to support this. While the prevalence of ulcers is higher in alcoholic cirrhotics, no association has been demonstrated in drinkers without cirrhosis.
Ulcer patients commonly describe dyspepsia with ingestion of certain foods, but there is no evidence that such foods cause ulcers. Coffee (caffeinated and decaffeinated), tea, and colas are all potent acid secretagogues. It was once popular to prescribe a bland diet for ulcer patients; however, they are generally conceded to exert no benefit.
Ulcers have long been associated in the public’s mind with emotional stress; however, this association has been disparaged since the appreciation of the role of H. pylori infection and NSAID use. Emotional stress is apparently probably not sufficient to cause ulcers in most patients since eradication of H. pylori and elimination of NSAIDs generally prevent ulcer recurrence despite the patient’s emotional state.
There are some suggestions that genetic factors may predispose patient to peptic ulcer. The incidence among identical twins is higher than that for nonidentical twins and there is an increase in first-degree relatives of ulcer patients. The genes responsible are unknown. Some of this increased susceptibility may be due to a high rate of H. pylori infection among family members. It was initially thought that elevated serum levels of serum pepsinogen I might be a genetic marker, but this now appears to be a consequence of H. pylori infection, which disappears with eradication. Other proposed markers include O blood group, lack of secretion of blood group antigens in saliva, and the presence of certain HLA subtypes; however, it now appears that these associations relate more to susceptibility to H. pylori infection.
Clinical Presentation
Perforated PUD typically causes sudden and severe epigastric abdominal pain that may progress to involve the entire abdomen. The pain caused by the spillage of highly caustic gastric secretions into the peritoneum rapidly reaches peak intensity and remain constant. Many patients can state the exact time of onset of their symptoms. Radiation to the right scapula region is common because of right subphrenic collection of gastric contents. Occasionally, pain is sensed in the lower abdomen if gastric contents travel caudally through the paracolic gutter. Peritoneal irritation is usually intense, and most patients avoid movement to minimize discomfort. The degree of peritoneal findings, however, is strongly influenced by a number of factors:
Size of the perforation
Amount of bacterial and gastric contents contaminating the abdominal cavity
Time between perforation and presentation
Spontaneous sealing of the perforation.
Physical examination reveals low-grade fever, diminished bowel sounds, and rigidity of the abdominal wall musculature. The patient can also demonstrate signs and symptoms of:
Early shock
Tachycardia
Hypotension and
Diminished urine output
Other indicators of toxicity (such as peritoneal irritation, fever, and increased white blood cell count with left shift) may actually be absent in both elderly and immunocompromised patients. Furthermore, other acute conditions, such as myocardial infarction, dissecting aortic aneurysm, cholecystitis, pancreatitis, diverticulitis, appendicitis, and renal colic can mimic the symptomatology of perforated PUD.
Laboratory Studies
It has been argued that, in general, laboratory studies are of little value in evaluating a patient with suspected duodenal ulcer perforation, but such tests as complete blood cell count, amylase and lipase determinations, and liver functions tests may be useful in excluding other causes of upper abdominal pain.
Complete blood cell count (Leukocytosis with left shift is found in many cases.)
Serum gastrin levels: Gastrin levels greater than 1,000 pg/mL are suggestive of gastrinoma; however, use of acid-reducing agents may cause some elevation of gastrin. Gastrin levels in patients who are taking acid reducing agents are usually not more than 300 to 450 pg/mL. If there is any question, a secretin stimulation test will make the diagnosis; however, these measurements are not pertinent to the acute presentation.
H. pylori infection testing.
Serum H. pylori antibody detection: Antibodies (immunoglobulin G, IgG) to H. pylori can be measured in serum, plasma, or whole blood; however, they only indicate past infection and do not confirm current infection.
Pathologic identification of H. pylori on biopsy is diagnostic as is a positive Clo test on biopsy; this is not helpful in the acute presentation, but may be useful in postoperative therapy.
Urea breath tests: These are used to detect active H. pylori infection by testing for the enzymatic conversion of urea to CO2 and ammonia. Current use of PPI agents may result in false negative tests
Imaging Studies
Upright chest radiography or lateral abdominal decubitus radiography reveals evidence of free air (pneumoperitoneum) (60% to 85% of patients). Even though this finding is not specific for perforated peptic ulcer, free air is usually present in much smaller amounts with perforation of abdominal viscera other than the duodenum or stomach.
An upper gastrointestinal study with water-soluble contrast, such as gastrograffin, can demonstrate extravasations if the ulcer has not spontaneously sealed. The lethal effects of barium when mixed with stool in the setting of colon perforations are well known; the effect of barium in the peritoneal cavity in duodenal perforations is unstudied. Nevertheless, prudence would suggest that barium be avoided when there is a risk of duodenal perforation. A contrast study with gastrograffin may show leak from the duodenum or its sealing and it can be a useful test when one is considering nonoperative treatment or in the situation where the diagnosis is in doubt. Currently, upper endoscopy is not recommended if perforation is definitely present or strongly suspected precisely because it may disrupt spontaneous sealing of the perforation.
CT scanning of the abdomen may demonstrate free air in the presence of perforated duodenal ulcer. CT with contrast may also demonstrate extravasation of contrast in the presence of a perforated ulcer. If history and physical examination raise the possibility of perforation, upright chest radiography, and an upper GI contrast study with water-soluble contrast are the diagnostic studies of choice. CT scanning is usually not needed in this situation.
Risk Stratification
Mortality from perforated duodenal ulcer is dependent upon the presence or absence of several risk factors. Individual risk can also be assessed by use of APACHE II. Overall mortality is approximately 10% in most studies. It has been reported that in the developing world, the high morbidity and mortality experienced by patients with perforated duodenal ulcer is probably due to delayed presentation. Those in whom diagnosis is overlooked almost always die. Risk factors affecting prognosis are:
Delay in treatment (>24 h)
Preoperative shock (BP <100 mm Hg)
Concurrent serious medical illness
It is reported that when all three are present, the mortality rises to 100% (39).
Nonoperative Management
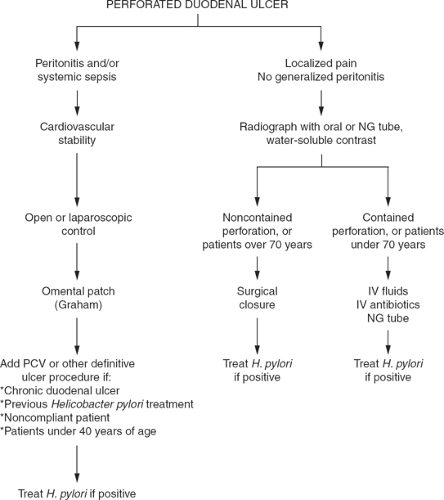
Current management of perforated duodenal ulcer in the United States usually includes operative approaches, but nonoperative management may be appropriate (Fig. 1).
Traditionally, perforated peptic ulcers were managed by urgent surgical repair, with or without an acid-reducing procedure. However, several studies have indicated that many patients can be successfully managed without an operation. In 1935, Wangensteen advocated a nonoperative approach in patients with perforation but without pneumoperitoneum. He believed that the absence of pneumoperitoneum indicated that the perforation had already sealed by the time of patient presentation; surgical exploration and repair was recommended for patients with demonstrable free air. More recently, Berne and Donovan have emphasized the use of the water-soluble upper gastrointestinal study, which demonstrates spontaneous sealing of the perforation. They note that as many as 40% of perforated PUD ulcers have sealed on an upper gastrointestinal study performed shortly after the patients present. Crofts et al. from Hong Kong, in 1989, showed that selective nonoperative treatment of perforated duodenal ulcer was accompanied by a low mortality rate and was not associated with a large number of complications when the gastroduodenogram demonstrated a sealed perforation. The mortality rate for patients treated operatively in their series was 6.2%, compared with mortality rate of 3% in those patients treated nonoperatively (retrospective review). Patients selected for nonoperative management should be treated as follows:
Nasogastric decompression
Fluid resuscitation with replacement of fluid and electrolytes
Proton pump inhibitors
Broad-spectrum antibiotics
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree