Osteochondroma
G. Petur Nielsen, MD
Andrew E. Rosenberg, MD
Key Facts
Terminology
Benign cartilage-capped tumor that originates in metaphysis or near apophysis
Accounts for 36-50% of benign tumors and 8.5-15% of all primary bone neoplasms that are surgically treated
Etiology/Pathogenesis
Neoplastic process
Associated with mutations involving EXT genes
Majority occur sporadically
Clinical Issues
Most patients in 2nd decade of life at time of diagnosis
Typically arise in metaphysis of bones derived from endochondral ossification
Treated by observation or simple excision
Image Findings
Surface lesion with continuity of cortices and medullary cavity of bone and lesion
Macroscopic Features
Cartilage cap of variable thickness; ranges from < 1 to > 2 inches in depth
Overall size ranges from 3-6 cm
Direct continuity between cortices and medullary cavity of lesion and underlying bone
Microscopic Pathology
Outer fibrous layer is perichondrium
Cartilage cap mimics growth plate
Cartilage cap undergoes enchondral ossification
TERMINOLOGY
Abbreviations
Osteochondroma (OCE)
Synonyms
Exostosis
Osteocartilaginous exostosis
Definitions
Benign cartilage-capped tumor that originates in metaphysis or region of apophysis
Arises on surface of bones and enlarges through process of endochondral ossification
Osteochondroma occurs in 2 clinical settings
As solitary lesion
Multiple lesions (multiple hereditary osteochondromatosis)
ETIOLOGY/PATHOGENESIS
Neoplastic Process
May occur sporadically, but when a manifestation of hereditary multiple osteochondromas (HMO), an autosomal dominant genetic disorder, they tend to be polyostotic and bilaterally symmetrical
Previously, osteochondromas were believed to develop from lateral displacement or redirection of growth plate or defects in surrounding periosteal cuff of bone
Based on the observation that osteochondromas never arise on surface of existing cortex and were induced experimentally in animals by manipulating the growth plate
Recent studies have shown that chondrocytes in cartilage cap have inactivating mutations involving genes EXT1 and EXT2 on chromosomes 8q24 and 11p11-12
Indicates that chondrocytes are derived from monoclonal cellular proliferation and strongly suggests that neoplastic component of osteochondromas resides in cartilage cap
Involvement of EXT3 on chromosome 19p also seen in some cases
Genetic abnormalities of osteochondroma have not been identified in dysplasia epiphysealis hemimelica or metachondromatosis
Small minority of osteochondromas are associated with previous radiation
Most patients are young
25% of patients ≤ 5 years who receive total body radiation develop osteochondroma
Patients with metachondromatosis have both osteochondromas and enchondromas
CLINICAL ISSUES
Epidemiology
Incidence
Most common primary bone tumor
Accounts for 36-50% of benign bone tumors and 8.5-15% of all primary neoplasms of bone
Approximately 80-85% of osteochondromas are solitary
Age
Most patients are in their 2nd decade of life at time of diagnosis
Incidence is 35/1,000,000 individuals 0-18 years of age
Age range is 8-77 years with average of 21 years
Gender
Male preponderance; M:F = 1.5-2:1
Site
Typically arise in appendicular skeleton
In metaphysis of bones derived from endochondral ossification
Distal femur, proximal tibia, proximal humerus
Rarely arise in epiphysis
Known as Trevor disease or dysplasia epiphysealis hemimelica in this location
Can involve flat bones, such as ilium and scapula
Rare in small bones of hands and feet and vertebrae, and never arise in craniofacial skeleton
Presentation
Many are asymptomatic
Incidental finding on imaging studies
Some are 1st detected as slowly enlarging firm mass present for many years
May be painful
Impingement upon adjacent neurovascular structures
Inflamed overlying bursa: Inflammatory bursitis
Fracture of stalk
Interferes with range of motion
Natural History
Slow growth that usually ceases at puberty
Osteochondromas exhibit greatest amount of growth while physeal plates are open
Malignant transformation should be considered if osteochondroma grows rapidly
Treatment
Small and asymptomatic osteochondromas do not require intervention
May sustain various complications that cause them to become symptomatic and justify removal
Excision usually adequate therapy
Cortex is transected near base of lesion, which is well defined in pedunculated lesions
Overlying bursa should also be removed with cartilage cap
If portion of perichondrium or cartilage cap is left behind, then lesion may recur locally
Prognosis
Malignant degeneration of solitary osteochondroma is very uncommon (0.4-2%)
Development of dedifferentiated component, such as high-grade osteosarcoma or pleomorphic spindle cell sarcoma, is exceedingly rare
IMAGE FINDINGS
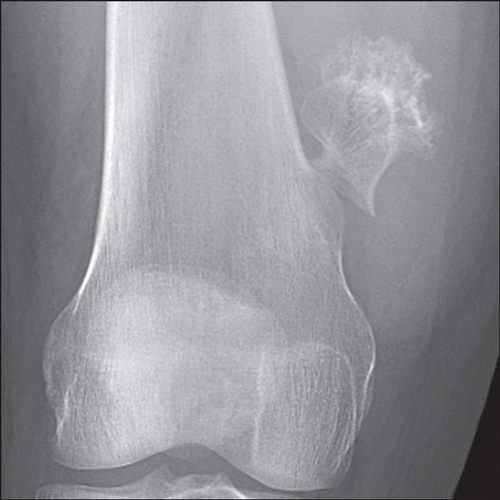
Radiographic Findings
Arises from surface of bone
Cortices of lesion and underlying bone and their marrow cavities are in direct continuity
In long tubular bones, lesion typically points away from nearest joint in reaction to forces exerted by muscles and tendons
Direction of osteochondroma is not diagnostic feature
Cartilaginous surface is lobulated and may contain calcifications
Base can be narrow or broad (sessile lesion)
Lesion can sometimes be heavily mineralized
MR Findings
T1-weighted image shows similar signal intensity of medullary cavity of lesion and underlying bone
T2-weighted image shows high signal intensity cartilaginous cap
Low signal intensity surrounding cap represents perichondrium
Helpful in evaluating thickness of cartilaginous cap
CT Findings
Nicely shows continuity of cortices and medullary cavity of osteochondroma and underlying bone
Useful in demonstrating thickness of cartilaginous cap
Helpful in showing bursa formation
Bone Scan
Hot in growing individuals
In adults, osteochondromas are often not hot on bone scan
Exceptions: Fracture, bursitis, malignant transformation
MACROSCOPIC FEATURES
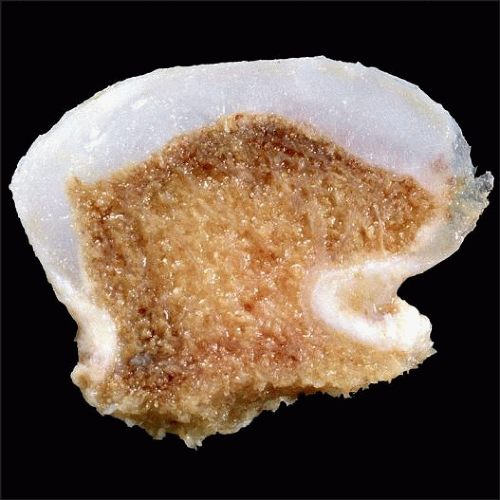
General Features
Mushroom shaped
Outer layer consists of thin sheath of fibrous tissue that overlies pearly gray-white cartilaginous cap
In older individuals, cartilaginous cap may be very attenuated or gone
May contain gritty areas of calcification or cystification
Cartilage cap of variable thickness; ranges from < 1 inch to several inches in depth
Surface of cap is smooth and lobulated
Base has sharp but undulating margin with underlying cancellous bone
Cartilage cap may demonstrate variable degrees of mineralization
In form of irregular stipples or ring-like calcifications
Due to partial or complete “framing” of cartilage lobules by ossification or amorphous mineralization
Base of cartilage cap undergoes enchondral ossification and merges with areas that have appearance of cancellous bone
Size
1 cm to > 20 cm in greatest dimension
Average: 3-6 cm
MICROSCOPIC PATHOLOGY
Histologic Features
Outer layer is perichondrium
Composed of dense fibrous tissue that overlies hyaline cartilage cap
Overall architecture recapitulates that of disorganized growth plate
Peripheral portion of cap is least cellular with individual chondrocytes surrounded by abundant hyaline cartilage matrix
Cellularity of cartilage increases in deeper layers
Chondrocytes become arranged in vague columns
In deeper layers, chondrocytes enlarge with more abundant cytoplasm
Chondrocytes exhibit minimal cytologic atypia and no mitotic activity
Scattered binucleate cells may be present
Matrix calcifies at base of cap
Chondrocytes undergo necrosis
Portions of mineralized cartilage are resorbed by osteoclasts at base of cap
Residual struts of cartilage matrix that are left behind act as scaffolding for bone deposition
Newly formed trabeculae mimic primary spongiosa at base of normal growth plate
DIFFERENTIAL DIAGNOSIS
Bizarre Parosteal Osteochondromatous Proliferation (BPOP)
Contains reactive fibrous tissue that overlies cellular cap of cartilage, which undergoes enchondral ossification
Underlying cortex is intact
Periosteal Myositis Ossificans
Radiographically arises on surface of bone with intact underlying cortex
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree