Patient Story
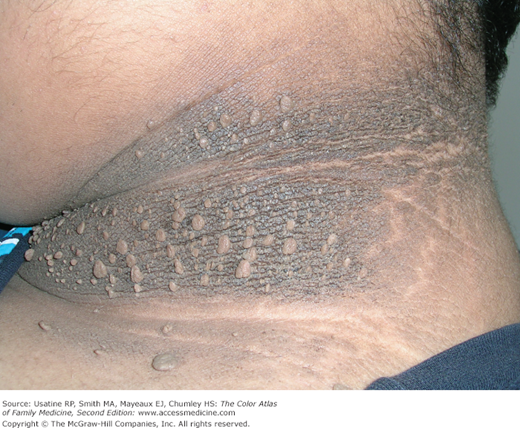
Diane is a 35-year-old woman who has struggled with obesity for most of her life. Her current body mass index (BMI) is 36. She has tried “every kind of diet you can imagine” but has always gotten stuck after losing the first 10 pounds and gets discouraged. She is not currently exercising regularly. She is concerned about all the skin tags on her neck and wants them removed if possible. She and her husband are talking about having another baby and she would like to be in better shape before she attempts pregnancy. She wants to discuss risks of pregnancy considering her weight and asks for any advice that you can give her on how to successfully lose weight. You obtain a random blood sugar because of the acanthosis and obesity (Figure 224-1). The result is 150 mg/dL and you order a fasting blood sugar (FBS) before her next visit, at which time you will remove her skin tags. After discussing diet and exercise, you encourage her to pursue Weight Watchers or a similar program.
Introduction
Obesity is defined as a BMI greater than or equal to 30. BMI is calculated as weight in kilograms divided by height in meters squared, rounded to 1 decimal place.1 Obesity in children is defined as a BMI greater than or equal to the age- and sex-specific 95th percentiles of the 2000 Centers for Disease Control and Prevention (CDC) growth charts. Adults with a BMI greater than 40 have substantially more serious health consequences, including heart disease and diabetes, and a reduced life expectancy.
Epidemiology
- Based on the National Health and Nutrition Examination Surveys, more than one-third of U.S. adults (35.7%) and 16.9% of children and adolescents are obese (2010).1 Slightly more women than men are obese (35.8% vs. 35.5%), although obesity is more prevalent in boys than girls at ages 2 to 19 years (18.6% vs. 15%). The prevalence of obesity has dramatically increased over the past 20 years.
- At the 6-year follow-up of the Nurses’ Health Study (NHS; a prospective cohort study of 50,277 women), 3757 (7.5%) women who had a BMI of less than 30 in 1992 became obese (BMI ≥30).2
- The medical care costs of obesity in the United States (2008 dollars) are approximately $147 billion.3
Etiology and Pathophysiology
Obesity is a complex problem involving genetics, health behaviors, environment, and sometimes medical diseases (see “Differential Diagnosis” below) or drugs (e.g., steroids, antidepressants). The simplest explanation of obesity is an imbalance between intake (calories eaten) and output (physical activity).
The genetic contribution to interindividual variation in common obesity has been estimated at 40% to 70%.4 Despite this relatively high heritability, the search for obesity susceptibility genes has been difficult. At least five variants in four candidate genes are associated with obesity-related traits. Although genome-wide linkage studies have been unable to pinpoint genetic loci for common obesity, high-density genome-wide association studies have discovered at least 15 previously unanticipated genetic loci associated with BMI and extreme obesity risk.4 Genetic influences, however, cannot explain the recent increased prevalence in the rate of weight gain by age; rather significant changes in lifestyle factors are likely responsible.5
- Two GI “hormones” that appear to integrate into the brain may regulate appetite; these hormones—ghrelin (increases appetite) and obestatin (slows gastric emptying, blocking ghrelin action)—may also play a role in obesity. A metaanalysis concluded that obestatin and total and active ghrelin were significantly higher in normal weight subjects than those of obese groups.6 It is not clear why this occurs but lower levels of ghrelin in obese subjects may be a response to hyperinsulinemia.
Lifestyle factors associated with obesity include physical activity level (low levels and associated behaviors such as television viewing), diet, and sleep.
- In the NHS, each 2-hour per day increment in TV watching was associated with a 23% (95% confidence interval [CI], 17% to 30%) and each 2-hour per day increment in sitting at work was associated with a 5% (95% CI, 0% to 10%) increase in obesity.2
- Based on second-wave interview data from the National Longitudinal Study of Adolescent Health (N = more than 14,000 adolescents), increasing levels of vigorous physical activities lowered the risk for obesity among all adolescents, while eating sufficient fruits and vegetables was inversely associated with adolescents’ obesity.5 As in the above study, sedentary lifestyle was associated with adolescents’ obesity. However, in models based on race, low family socioeconomic status, and being sedentary were associated with overweight and obesity among whites and increased nighttime sleep hours was associated with obesity among African Americans.
- In one study, belief that obesity was inherited was associated with lower reported levels of physical activity and fruit and vegetable consumption while the belief that obesity was caused by lifestyle behaviors was associated with greater reported physical activity but not diet.7
- In a study of Latino men and women, men who did not exercise, rarely trimmed fat from meat, and ate fried foods the previous day were 16 pounds heavier than men with healthier habits.8 Women who had limited exercise (<2.5 hours per week), watched television regularly, ate chips and snacks, and ate no fruit the previous day were 45 pounds heavier than women with healthier habits.
Factors that have been discussed include location of grocery stores versus fast-food restaurants and safe places to exercise in relation to home proximity. Research studies suggest that neighborhood residents who have better access to supermarkets and limited access to convenience stores tend to have healthier diets and lower levels of obesity.9 Poor neighborhoods are often characterized by just the opposite. In fact, in one study, having the opportunity to move from a poor neighborhood to one with a lower level of poverty through housing vouchers was associated with modest reductions (4.6%) in the prevalence of extreme obesity and diabetes.10
Risk Factors
Diagnosis
- Although elevated weight alone is a risk factor for the development of hypertension, diabetes mellitus (DM), and heart disease, increased waist circumference confers additional morbidity risk (Figure 224-2).13
- Neck circumference enlargement (Figure 224-1) along with increased BMI and waist circumference are significant risk factors for obstructive sleep apnea and metabolic syndrome.14,15
- There is a strong direct correlation between epicardial fat and abdominal visceral adiposity with evidence supporting a role for epicardial fat in the pathogenesis of coronary artery disease.16
- Nonalcoholic fatty liver disease (NAFLD) is present in 57% of overweight individuals attending outpatient clinics compared to 98% of nondiabetic obese patients and in contrast to 10% to 30% of adults in the general population (see Chapter 61, Liver Disease).17
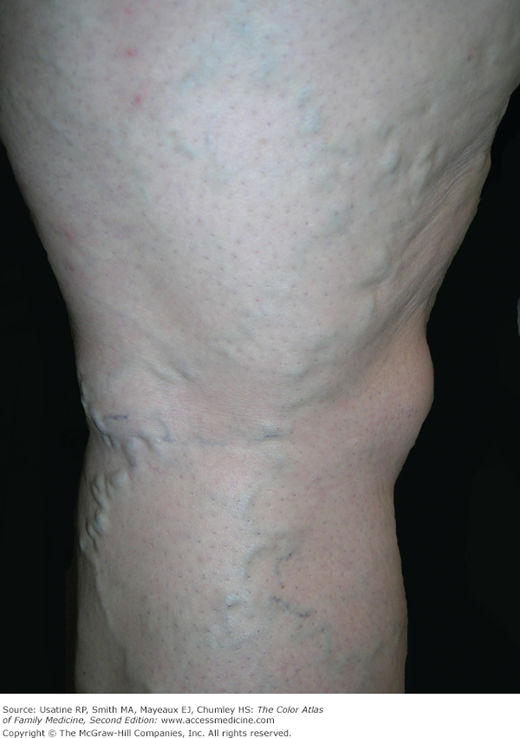
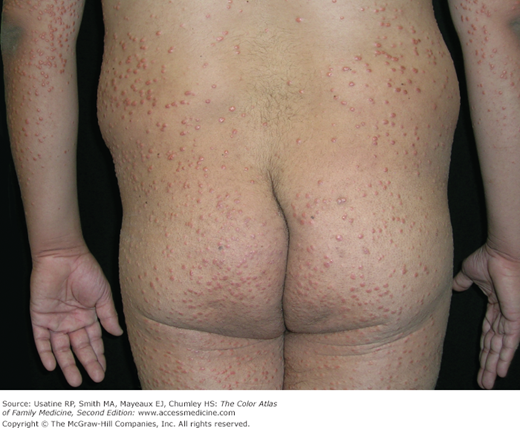
- Obesity is also associated with an increased risk of varicose veins (odds ratio [OR] 3.28; 95% CI 1.25 to 8.63) (see Chapter 52, Venous Insufficiency) (Figure 224-3).
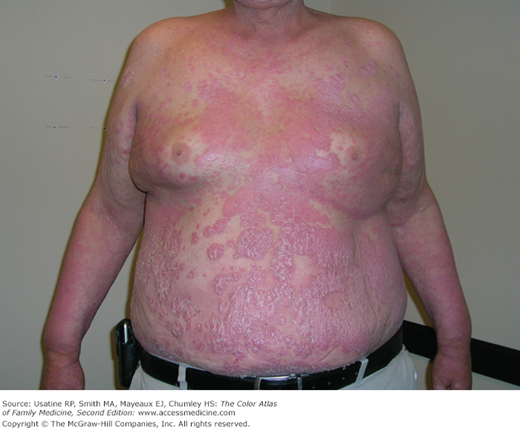
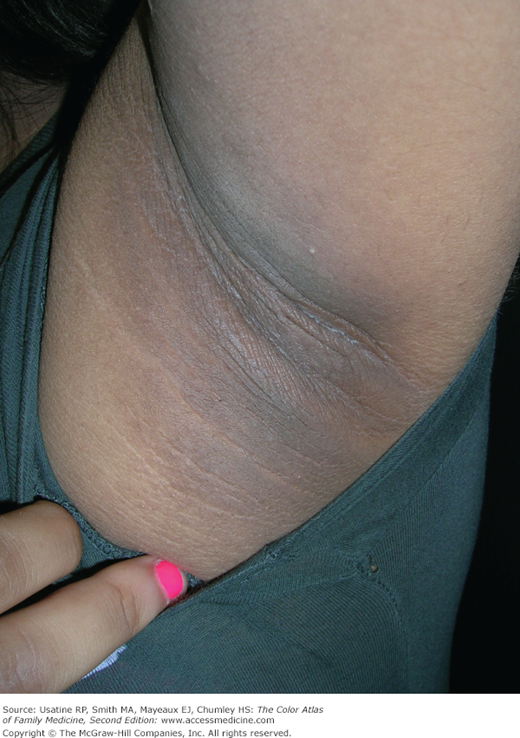
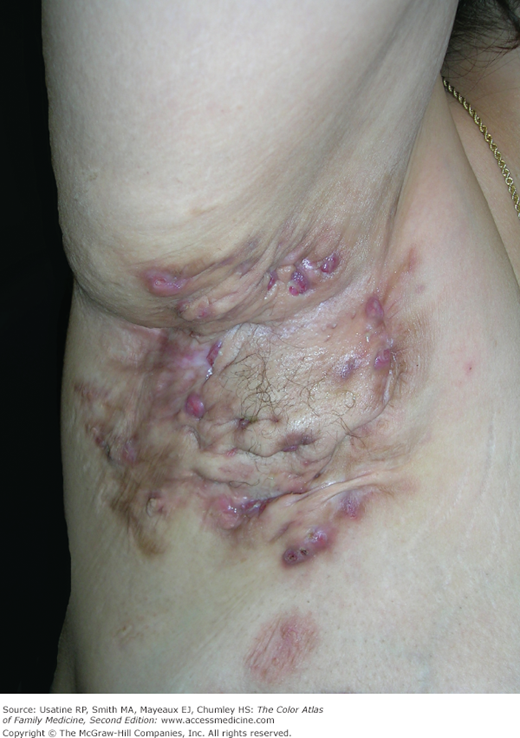
- Skin conditions associated with obesity include acanthosis nigricans (Figures 224-1 and 224-4), eruptive xanthomas (Figure 224-5), hidradenitis suppurativa (Figure 224-6), and psoriasis (Figure 224-2). (see Chapters 115, Hidradenitis Suppurativa, 152, Psoriasis, 220, Acanthosis Nigricans, and 223, Hyperlipidemia and Xanthomas).
Although no specific tests are suggested for patients with obesity, assessing a patient’s cardiovascular risk status in addition to BMI, waist circumference, and a patient’s motivation to lose weight may be helpful in planning treatment.13 Consider screening for DM and NAFLD.
Differential Diagnosis
- Cushing syndrome—Caused by prolonged exposure to endogenous or exogenous glucocorticoids; in addition to truncal obesity, clinical features include moon facies, supraclavicular fat pads, buffalo hump, purple striae, proximal muscle weakness, and hirsutism. Diagnosis is confirmed with inappropriately high serum or urine cortisol levels.
- Polycystic ovary syndrome—Criteria include two of three of oligoovulation or anovulation, hyperandrogenism, and polycystic ovaries.
- Obesity is also a finding in many single-gene disorders such as Prader-Willi syndrome (abnormality of proximal arm of chromosome 15 with associated characteristics of obesity, hypotonia, mental retardation, short stature, hypogonadotropic hypogonadism, strabismus, and small hands and feet) and Bardet-Biedl syndrome (associated with truncal obesity, childhood-onset visual loss preceded by night blindness, and polydactyly).
Management
The initial weight loss goal is to reduce body weight by approximately 10% from baseline over approximately 6 months.13 Additional weight loss can be attempted if this goal is achieved.
- Dietary changes may be useful. In a metaanalysis of long-term weight loss strategies in adults, however, dietary/lifestyle therapy provides less than 5 kg weight loss after 2 to 4 years.18 SOR A Commercial weight management services appear to be more effective and cheaper than primary care-based services led by specially trained staff (range: 4.4 kg [Weight Watchers] to 1.4 kg [general practice]).19 SOR A
- Exercise should be encouraged and can result in small weight losses and improvement in cardiovascular risk factors; greater intensity exercise results in additional small weight loss (weighted mean difference [WMD] approximately −1.5 kg).20,21 SOR A The addition of diet to exercise also increases weight loss (WMD −1 kg).
- Although data are limited, lifestyle interventions appear to reduce overweight in children.22 SOR B
- Behavioral and cognitive-behavioral strategies are also effective (WMD −2.5 kg and −2.3 kg, respectively), but are most effective when used in combination with diet and exercise (WMD [added cognitive-behavioral strategies] −4.9 kg).23 SOR A
- Behavioral strategies found to be effective include various forms of support, motivational interviewing, and reducing TV screen time.
- Both remote weight-loss support (study-specific website and e-mail) and in-person support during group and individual sessions along with remote support resulted in greater sustained weight loss at 24 months than the control group (−4.6 kg, −5.1 kg, and −0.8 kg, respectively).24
- A program entitled “High Five for Kids,” using motivational interviewing targeting television viewing, fast food, and sugar-sweetened beverage intake, was not effective in one randomized clinical trial (RCT) in reducing BMI at 1 year.25
- With respect to psychological interventions, of three interventions (usual care with quarterly primary care physician educational visits, brief lifestyle counseling, or enhanced brief lifestyle counseling including meal replacements) examined in adult patients with obesity, enhanced care was more effective than usual care for initial weight loss and sustained weight loss at 2 years (1.7 ± 0.7 and 4.6 ± 0.7 kg, respectively).26 SOR B
- In the 2005 systematic review by Douketis et al., pharmacologic therapy for obesity resulted in to 10-kg average weight loss after 1 to 2 years.18 SOR A An older Cochrane review of orlistat, sibutramine, and rimonabant found more modest but significant weight reduction (2.9 to 4.7 kg); conclusions were limited by high attrition rates.27
- The National Heart, Lung, and Blood Institute (NHLBI) Clinical Guideline recommends consideration of drug therapy approved by the FDA for long-term use as an adjunct to diet and physical activity for patients with a BMI of 30 with no concomitant obesity-related risk factors or diseases, and for patients with a BMI of 27 with concomitant obesity-related risk factors or diseases. SOR B

Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree