Patient Story
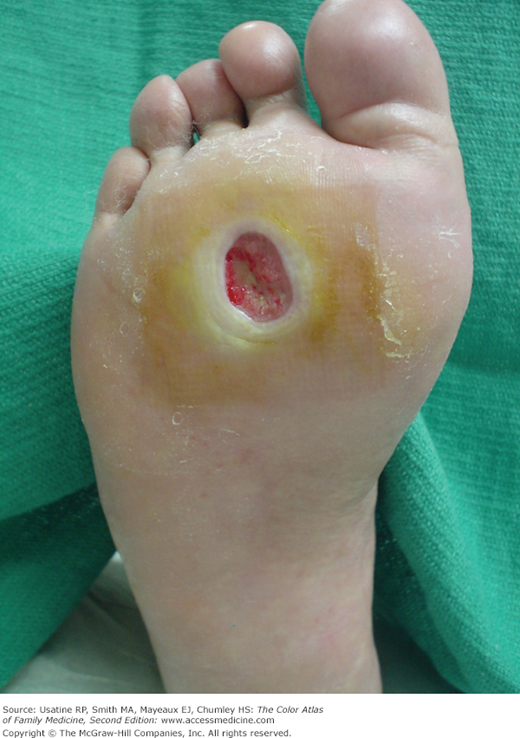
A 57-year-old man with type 2 diabetes presented with history of a neuropathic ulceration to the right foot for 2 weeks (Figure 211-1). The patient recalled having a callus for several months. He noticed blood on his sock 3 days ago. He denied fever or chills, but his glucose has been running higher than normal. The patient demonstrated loss of protective sensation, but vascular status was intact. He was referred to a podiatrist who immediately offloaded his foot with a total contact cast. His ulcer healed in 1 month, and he was subsequently fitted with orthopedic shoes.
Introduction
Foot complications in patients with diabetes mellitus are common, costly, and impact quality of life. Neuropathic ulcers can lead to the most devastating outcome, which is an amputation. Eighty-five percent of all amputations related to diabetes are preceded by an ulcer. Prevention, early recognition, and treatment of foot ulcers are critical in avoiding amputations.
Epidemiology
Etiology and Pathophysiology
- Peripheral neuropathy is an important factor in the development of a diabetic foot ulcer.
- Neuropathy causes autonomic denervation of precapillary arterioles, leading to persistent vasodilation and chronic edema.
- Moderate pressure with repetitive trauma occurs in a particular site, often from poorly fitting footwear, which then leads to ulceration.
Risk Factors
- Diabetic neuropathy increases the risk of developing a foot ulcer by 70%.3
- Patients with pedal deformity combined with diabetic neuropathy are 12 times more likely to develop a foot ulcer.3
- Limited joint mobility, high level of activity, and poorly fitting footwear also increase the risk of the repetitive trauma that leads to ulceration.
Diagnosis
- A red, granular base (Figures 211-1 and 211-2).
- Surrounding hyperkeratosis with white, macerated margins (Figures 211-1 and 211-2).