http://evolve.elsevier.com/Edmunds/NP/
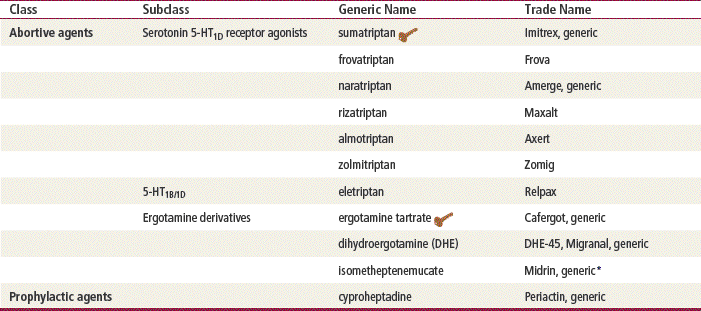
 Key drug. Key drugs chosen because they were first in their class and are still used. See Table 44-1 for discussions in other chapters of drugs commonly used for prophylaxis.
Key drug. Key drugs chosen because they were first in their class and are still used. See Table 44-1 for discussions in other chapters of drugs commonly used for prophylaxis.
∗Some products are off the market now, but available as combination products.
A wide variety of drugs are used for the treatment of migraines. They are divided into medications that are effective in acute treatment of migraine symptoms and medications used for chronic prophylaxis. The most commonly used migraine medications are the serotonin1 (5-HT1) receptor agonists, commonly known as the “triptans.” Migraine-specific products are discussed in detail in this chapter. Abortive medications include acetaminophen, aspirin, and NSAIDs, as well as triptans. Preventative medications approved by the FDA also include β-blockers, calcium channel blockers, TCAs, SSRIs, and anticonvulsants. Only their use in the treatment of migraines is discussed in this chapter.
Therapeutic Overview
Migraine is a primary disorder of the brain that still is poorly understood. Genetics is linked to the incidence of hemiplegic migraines, and because 70% to 80% of migraine sufferers have a family history of migraine, genetic components that have not been identified are probably involved. A single explanation that encompasses all of the phenomena that occur with migraine has eluded researchers to date. Many neural events can cause dilation of blood vessels, which causes pain and other nerve activation. The underlying physiologic problem appears to be the dysfunction of an ion channel in brainstem neurons that normally modulate sensory input and exert neural influence on cranial vessels. The brain neurotransmitters involved are primarily from the serotonergic system. Serotonin receptor subtypes, including 1B, 1D, and 1F, play a role in cerebral vasodilation and trigeminal nerve activation, which are believed to be the precursors of migraine pain.
Disease Process
Headaches represent a very common complaint in primary care. They have many causes, ranging in seriousness from stress to brain tumor; therefore, the cause must be determined whenever possible for effective therapy to be determined.
Tension headache (THA), the most common type of headache, usually is described as vise-like pressure associated with stress and/or fatigue. The pain of THA usually is generalized but may be worse in the area of the neck and the back of head. These patients are generally treated with analgesics for mild to moderate pain. (See Chapter 43 for more information on pain management.)
Approximately 23 million Americans are afflicted with migraine headaches. Migraine headaches usually begin in the teenage years, peaking between the ages of 25 and 34; they are three times more prevalent among women than men. These headaches represent a debilitating and costly medical problem. For a variety of reasons, a large group of persons do not seek medical care for their migraines.
Migraine symptoms vary. All migraines are paroxysmal in nature—clearly defined attacks separated by symptom-free intervals. Daily or continuous headaches usually are not migraines but are tension or vascular headaches. Migraines are classified as with aura or without aura and are graded as mild, moderate, or severe in intensity. The duration of migraine is an important variable because the clinician must choose medications whose duration of action is adequate. Classic migraines go through specific phases (Table 44-2).
Complicated migraines, which are less common, are characterized by attacks in which neurologic symptoms last for the entire headache or for several days or weeks or, in some cases, leave a permanent neurologic deficit. Complicated migraines are divided into three subtypes. An ophthalmoplegic migraine affects the third, fourth, or sixth cranial nerve; permanent damage to the third nerve has been reported. Hemiplegic migraine is characterized by both motor and sensory symptoms that are unilateral and may last longer than the headache itself; this type is very rare. Complete recovery from these symptoms may take weeks, and permanent weakness can occur following multiple attacks. Basilar-type migraine is characterized by any combination of vertigo, diplopia, dysarthria, tinnitus, decreased hearing, ataxia, simultaneous bilateral paresthesias, and altered consciousness. It may be difficult sometimes to distinguish between visual symptoms of a classic migraine and basilar artery migraine, although the latter is more likely to affect both visual fields.
A transformed migraine is a long-lasting headache that results from overuse of pain and/or migraine medications. Following a migraine episode, the patient has rebound headache daily or nearly daily. Medications that can cause this include caffeine, acetaminophen, NSAIDs, barbiturates, sedatives, narcotics, ergots, and triptans.
Treating headaches with narcotics and barbiturates increases the risk for development of chronic migraine headaches and should not be considered first choice to relieve pain.
Assessment
Diagnosed migraine must meet specific criteria established by the National Headache Foundation (Box 44-1). A diagnostic workup headache history includes age of onset of headaches; duration of complaint; frequency and duration of each headache; site, quality, and time of onset; associated phenomena; and aggravating and relieving factors. Physical examination, including neurologic examination, is typically normal. Some patients experience substantial burden from their migraines. The Migraine Disability Assessment Scale (MIDAS) is a five-item questionnaire that is used in practice (see Goadsby et al, 2002, for questionnaire uhs.berkeley.edu/home/healthtopics/pdf/assessment.pdf) to help the clinician measure how much intervention is required to improve the patient’s quality of life.
Migraine headache often is stimulated by visual, olfactory, or other environmental triggers that may be identified. (See Box 44-3.) The patient must be screened for concurrent illnesses, especially cardiovascular problems such as increased blood pressure and CAD. These concurrent illnesses may affect treatment options.
Recent research suggests that patients who suffer from migraine could be more prone to clinical depression. Participants who experienced migraines had an 80% higher relative risk of developing depression than those without headaches, while participants who were depressed were 40% more likely to suffer migraines, researchers said. Clinicians might be aware of this relationship in their assessment and patient monitoring.
Mechanism of Action
See Table 44-3 for drug effects on serotonin receptors.
TABLE 44-3
Drug Effects on Serotonin (5-HT) Receptors
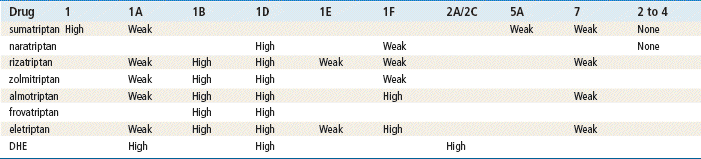
From Silberstein SD: Practice parameters: evidence-based guidelines for migraine headache, Neurology 55:754-762, 2000.
All 5-HT1 receptor agonists (triptans) have a similar chemical structure and a comparable mechanism of action. 5-HT1B and 5-HT1D receptors are located on the extracerebral, intracranial blood vessels that become dilated during a migraine attack and on nerve terminals in the trigeminal system. Therapeutic activity is caused by activation of these receptors, which results in cranial vessel constriction, inhibition of neuropeptide release, and reduced transmission in trigeminal pain pathways. Each product varies with regard to onset of action, duration of action, and incidence of recurrent headache.
Ergotamine derivatives demonstrate partial agonist and/or antagonist activity against dopaminergic, tryptaminergic, and α-adrenergic receptors, depending on their site. Ergotamine derivatives have three primary actions. They (1) depress central vasomotor centers, (2) constrict peripheral and cranial blood vessels, and (3) reduce extracranial blood flow and decrease hyperperfusion of the basilar artery area. In unrelated actions, these drugs also increase the force and frequency of uterine contractions.
Ergotamine tartrate is an α-adrenergic–blocking agent with direct stimulating effects on the smooth muscle of the peripheral and cranial vessels. Ergot drugs also produce an increase in central vasomotor center stimulation. Although dihydroergotamine (DHE) is an ergot, it is also a 5-HT1B/1D receptor agonist that is not as selective as the triptans. DHE binds to norepinephrine (noradrenaline) α1, α2A, and α2B and dopamine D2L and D3 receptors. It is a stronger venoconstrictor and a weaker arterial vasoconstrictor than ergotamine.
Combination Drugs
Isometheptenemucate is a sympathomimetic agent that acts as a vasoconstrictor of dilated cranial and cerebral arterioles. Midrin is a combination capsule that contains 65 mg of isometheptenemucate; 325 mg of acetaminophen, which exerts an analgesic effect; and 100 mg of dichloralphenazone, a mild sedative that acts centrally to allay anxiety. Caffeine, which is added to many migraine combinations, helps to promote constrictive properties and enhances absorption. ASA, acetaminophen, ibuprofen, and caffeine, all of which are commonly found in combination analgesic products used for the treatment of patients with mild to moderate migraine, have been shown through evidence-based studies to be effective in the prophylaxis and treatment of migraine.
Prophylactic Agents
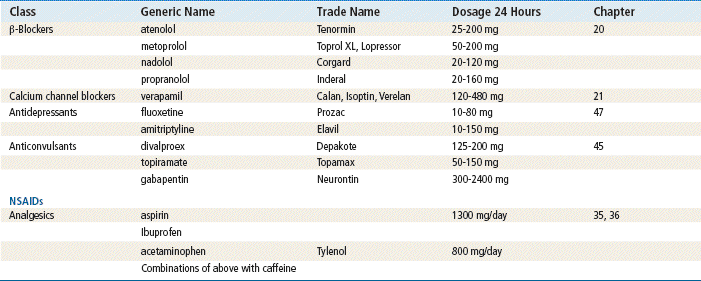
See Box 44-4 for a list of prophylactic medications.
The β-blockers are postulated to exert antimigraine effects through stabilization of vascular tone. Postulated mechanisms by which this stabilization may occur include (1) inhibition of norepinephrine release by blocking prejunctional β-receptors, (2) reduction in enzyme activity (tyrosine hydroxylase) that is the rate-limiting step in norepinephrine synthesis, and (3) delayed reduction of locus ceruleus neuron firing. Blocking of central β-receptors interferes with vigilance-enhancing adrenergic pathways that are important in headache prevention. Interaction with serotonin receptors by some β-adrenergic blockers may stabilize vascular tone.
Calcium channel blockers regulate cellular functions, including vascular smooth muscle contraction, neurotransmission, and hormone secretion enzyme activity. These products also block intracerebral vasoconstriction caused by vasoactive neurotransmitters such as 5-HT (serotonin) and norepinephrine. In addition, calcium channel blockers may impede neurovascular inflammation and prevent hypoxia of cerebral neurons.
Tricyclic antidepressants act to reduce migraine activity by increasing the availability of synaptic norepinephrine or serotonin “downregulation” of 5-HT receptors and β-receptor density. Thus, they enhance the opiate mechanism and provide inhibition of 5-HT and norepinephrine reuptake, while binding to receptors on platelets and neurons that are blocking 5-HT uptake. The net result is an increased threshold for precipitation of a migraine attack in selected individuals.
SSRIs are potent, specific 5-HT receptor reuptake inhibitors that reduce migraine frequency and intensity. They act to prevent the vasoconstrictive effects of decreased serotonin levels during headache. Such constriction sets up a cascade of neuron inflammatory changes that produce headache pain. Maintaining the serum level of 5-HT with SSRIs prevents initiation of this pathway, thereby preventing migraine.
Anticonvulsants are believed to exert antimigraine activity through their influence on cerebral arteries and circadian rhythms. They also may help to regulate secretion of hormones from the anterior pituitary gland that help to relax vascular structures.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree



 It is essential that adequate evaluation and diagnostic testing be completed to confirm the diagnosis of migraine. Some headaches that patients may call migraines are actually other pathologic conditions; some of these headaches represent significant problems that must not be ignored.
It is essential that adequate evaluation and diagnostic testing be completed to confirm the diagnosis of migraine. Some headaches that patients may call migraines are actually other pathologic conditions; some of these headaches represent significant problems that must not be ignored. 