Fig. 6.1
High-grade urothelial carcinoma. (a) High-grade urothelial carcinoma (HGUC). The sample is hypercellular showing numerous tumor cells that demonstrate pleomorphism and necrosis in the background (Voided urine, SP, low mag.). (b) High-grade urothelial carcinoma (HGUC). The sample was full of these abnormal cells with high N/C ratios and prominent nuclear profiles. The total sample was stained somewhat lightly, so observers are cautioned to use normal cells in the background as stain intensity controls. Also note the presence of lymphocytes in the sample that can be used as controls for nuclear size (Washing, TP, medium mag.)
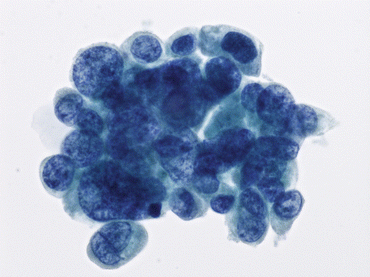
Fig. 6.2
High-grade urothelial carcinoma (HGUC) present as a cohesive group of malignant cells. The N/C ratio of 0.7 is noted in the majority of the tumor cells (Bladder washing, TP, high mag.)
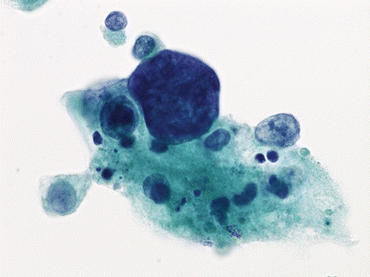
Fig. 6.3
Nuclear hyperchromasia is present in this cell from a patient with high-grade urothelial carcinoma (HGUC). Note the tumor necrosis clinging to the cells (Bladder washing, TP, high mag.)
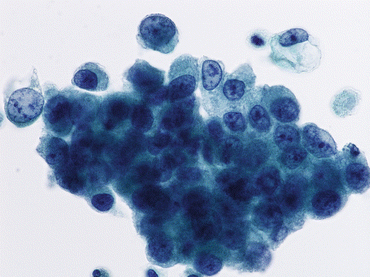
Fig. 6.4
High-grade urothelial carcinoma (HGUC) exhibits nuclear membrane irregularity with focal thickness of nuclear membranes. Nuclear shapes and sizes vary (Bladder washing, TP, high mag.)
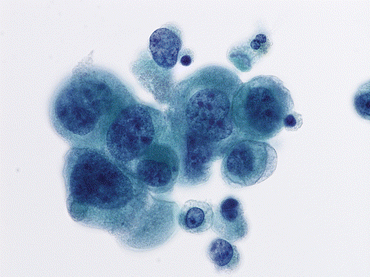
Fig. 6.5
High-grade urothelial carcinoma (HGUC) demonstrates coarse and clumped nuclear chromatin (Voided Urine, TP, high mag.)
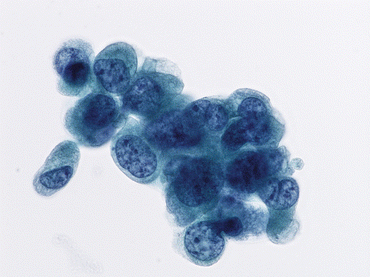
Fig. 6.6
High-grade urothelial carcinoma (HGUC) displays coarse chromatin and nuclear membrane irregularity (Bladder washing, TP, high mag.)
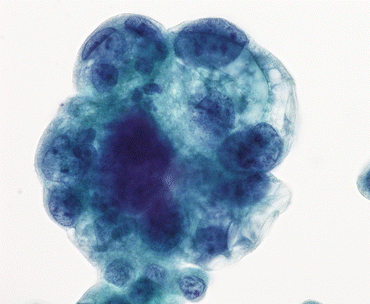
Fig. 6.7
High-grade urothelial carcinoma (HGUC) with cytoplasmic vacuolization reflects glandular differentiation. Nuclear membrane irregularity, hyperchromasia, and coarse chromatin typify HGUC (Bladder washing, TP, high mag.)
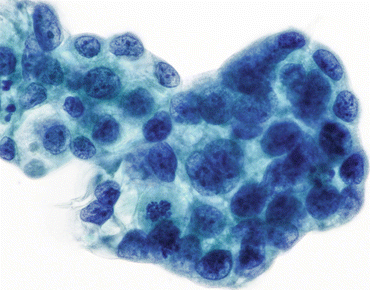
Fig. 6.8
High-grade urothelial carcinoma (HGUC) tumor cells exhibit nuclear hyperchromasia, nuclear membrane irregularity, coarse chromatin, and mitoses. Cytoplasm is frothy and N/C ratios vary, but nuclear features still place the sample in the HGUC category (Bladder washing, TP, high mag.)
Definition of HGUC with Squamous Differentiation
This is defined by the presence of keratinization and⁄or intercellular bridges as classic morphological features. Squamous cells are intermixed with malignant cells exhibiting classic features of HGUC. The squamous cells display hyperchromatic and spindle-shaped nuclei with clumped chromatin. The cytoplasm is dense, keratinized, and orangeophilic. Keratin flakes and necrosis are frequently observed in the background (Figs. 6.9 and 6.10) [21–23]. Diagnosis of squamous carcinoma of the urinary tract can only be determined by extensive examination of biopsy or cystectomy tissue.
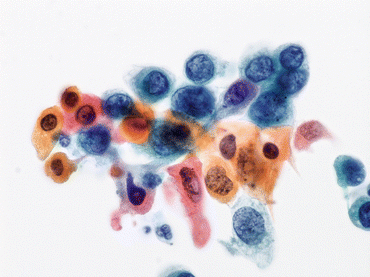
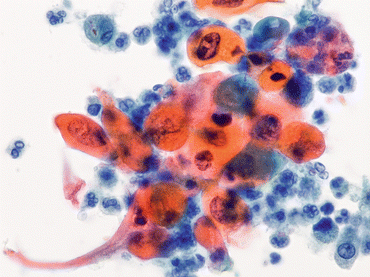

Fig. 6.9
A few cells exhibit classic features of high-grade urothelial carcinoma (HGUC) adjacent to cells of squamous differentiation (Bladder washing, TP, high mag.)

Fig. 6.10
Pronounced keratinization of tumor cells is present in this patient with a history of high-grade urothelial carcinoma (HGUC). The diagnosis of Urothelial Carcinoma vs. Squamous Carcinoma will depend upon the percentage of squamous differentiation once the bladder is removed and completely examined histologically (Bladder washing, TP, high mag.)
Definition of HGUC with Glandular Differentiation
Glandular differentiation is defined as the presence of true glandular formation within groups of tumor cells. Glandular cells are intermixed with malignant cells exhibiting classic features of HGUC (Figs. 6.11 and 6.12). Diagnosis of adenocarcinoma of the urinary tract can only be determined by extensive examination of biopsy or cystectomy tissue.
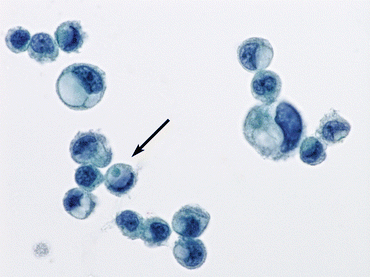
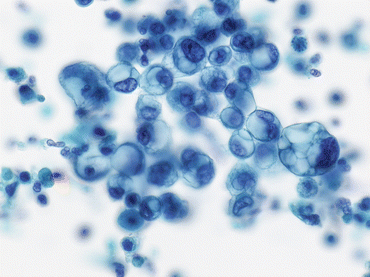

Fig. 6.11
Scattered high-grade urothelial carcinoma (HGUC) tumor cells demonstrate focal glandular differentiation (Bladder washing, TP, medium mag.)

Fig. 6.12
High-grade urothelial carcinoma (HGUC) tumor cells with glandular differentiation are from the same sample as Fig. 6.11 (Bladder washing, TP, high mag.)
Criteria of Malignancy
HGUC is diagnosed on the basis of the following criteria according to The Paris System consensus (see Explanatory Note):
Cellularity: At least 5–10 abnormal cells
N/C ratio: 0.7 or greater
Nucleus: Moderate to severe hyperchromasia
Nuclear membrane: Markedly irregular
Chromatin: Coarse/clumped
Other Notable Cytomorphologic Features
Cellular pleomorphism
Marked variation in cellular size and shapes, i.e., oval, rounded, elongated, or plasmacytoid (Comet cells)
Scant, pale, or dense cytoplasm
Prominent nucleoli
Mitoses
Necrotic debris
Inflammation
Explanatory Notes
Explanatory Note 1: Increased N/C ratio of at least 0.7 is used as a benchmark, in addition to severe hyperchromasia and/or marked nuclear irregularity, for guiding the cytopathologist in identifying malignancy. The majority of HGUC cells will exhibit N/C ratio greater than 0.7, although some cells may show N/C ratio in the range of 0.5–0.7.
Explanatory Note 2: Hyperchromasia is characterized by tumor cells showing a marked density of the nuclear chromatin. Hyperchromasia is moderate to severe in intensity, and should clearly separate the HGUC cells from benign cells present in the sample.
Explanatory Note 3: Prominent nucleoli can be identified in HGUC but may also be present in reactive urothelial cells. Reactive urothelial cells will not exhibit the other criteria of HGUC: hence prominent nucleoli accompanying other criteria of HGUC will be noted in the malignant cells.
Rate of Malignancy
The percentage of urinary cytology cases reported as “positive for malignancy” is relatively low and would be expected to vary based on the clinical and demographic characteristics (risk) of the population, and the practice habits of physicians who are ordering urinary cytology evaluations. Therefore, laboratories may have quite different rates of cases interpreted as “positive for malignancy”. It is also noteworthy that patients with cytologic results of “positive for malignancy” and “suspicious for malignancy” are often managed similarly. Thus many studies appropriately combine these two categories when evaluating the diagnostic accuracy of urinary cytology.
In Dr. Papanicolaou’s initial publication demonstrating the feasibility of using urinary cytology to detect bladder cancer, 27 of 83 cases, or 33 % were reported as positive for neoplasm [24]. Undoubtedly this cohort of patients was a selected and high-risk population. More contemporary, larger studies from laboratories have reported much lower rates of malignancy that have ranged from 1.7 to 5.8 % of all urinary cytology cases [25–27]. These studies also confirmed that bladder washings and upper urinary tract specimens tend to have a higher percentage of malignant cases as compared to voided urine specimens.
The Paris System working group also made an international outreach attempt to further ascertain the rate of malignancy in various academic and nonacademic practice settings. The data from this study are included in Table 6.1. The cytopathology laboratories contributing these data included both academic and nonacademic practices, and provided data for the year 2013. The rate of malignancy or cases identified as “positive for malignancy” ranged from 1.0 to 6.3 %. In addition, cases that were suspicious for malignancy showed a range of 0.2 to 5.4 %. This again, demonstrates a low number of cases being finalized as equivocal, in most clinical laboratories. The cases that were designated as “Negative for malignancy” ranged from 64.8 to 96.1 %, which demonstrates that the majority of the samples reviewed are benign.
Table 6.1
The Paris Group outreach survey for rate of malignancy in urinary cytologic specimens in clinical laboratories
Location | Type | Total number | Positive for malignant cells [PFMC] (%) | Suspicious for malignant cells [SFMC] (%) | Atypical NOS (%) | Negative (%) | Washing (%) |
|---|---|---|---|---|---|---|---|
Charlotte, NC
Stay updated, free articles. Join our Telegram channel
Full access? Get Clinical Tree
 Get Clinical Tree app for offline access
Get Clinical Tree app for offline access

|