Patient Story
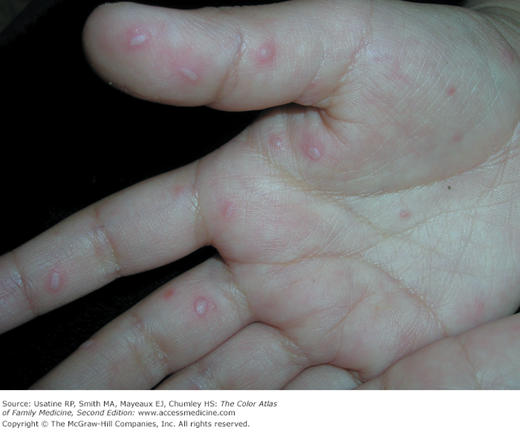
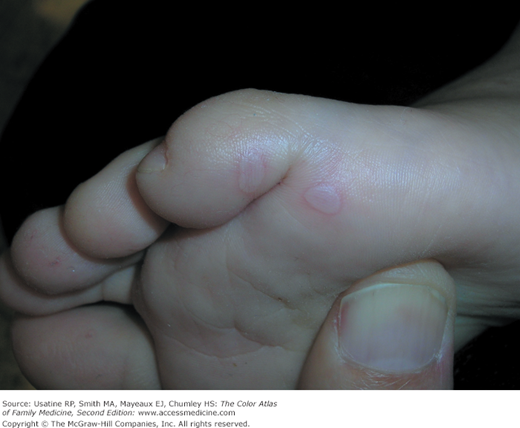
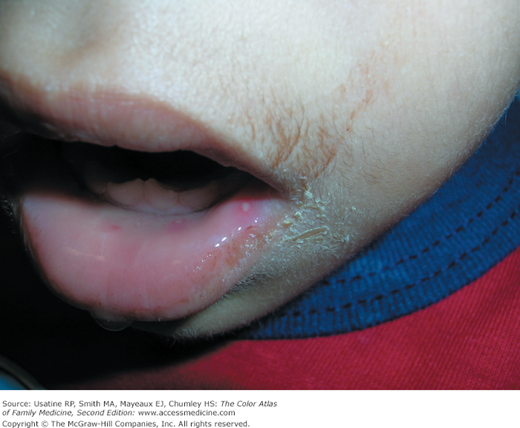
A 4-year-old boy presents to a free clinic for homeless families with a low-grade fever and lesions on his hands and feet (Figures 128-1 and 128-2). The mother notes that two other kids in the transitional living center also have a similar rash. Upon further investigation, the mouth lesions are noted (Figure 128-3). The mother is reassured that this is nothing more than hand, foot, and mouth disease and will go away on its own. Treatment includes fluids and antipyretics as needed.
Figure 128-2
Foot of the boy in Figure 128-1 with hand, foot, and mouth disease. Lesions tend to be on palms and soles, fingers, and toes. (Courtesy of Richard P. Usatine, MD.)
Introduction
Epidemiology
- Epidemics tend to occur every 3 years worldwide. In temperate climates, the peak incidence is in late summer and early fall.
- HFMD generally has a mild course, but it may be more severe in infants and young children.1,2
- There is no racial or gender predilection. Most cases affect children younger than 10-year-old.3
Etiology and Pathophysiology
- HFMD is most commonly caused by members of the enterovirus genus, especially coxsackie viruses. Epidemic infections are usually caused by coxsackievirus A16, and less commonly by other coxsackievirus A, coxsackievirus B, or enterovirus 71.2,3 Sporadic cases occur caused by other coxsackie viruses.
- Coxsackievirus infections are highly contagious. Transmission occurs via aerosolized droplets of nasal and/or oral secretions via the fecal-oral route, or from contact with skin lesions. During epidemics, the virus is spread from child to child and from mother to fetus.
- The incubation period averages 3 to 6 days. Initial viral implantation is in the GI tract mucosa, and it then spreads to lymph nodes within 24 hours. Viremia rapidly ensues, with spread to the oral mucosa and skin. Rarely, aseptic meningitis may occur. Usually by day 7, a neutralizing antibody response develops, and the virus is cleared from the body.
- When HFMD is caused by enteroviruses, it may also result in neurologic problems such as a polio-like syndrome, aseptic meningitis, encephalitis, acute cerebellar ataxia, acute transverse myelitis, Guillain-Barré syndrome, and benign intracranial hypertension. Rarely, cardiopulmonary complications such as myocarditis, interstitial pneumonitis, and pulmonary edema may occur.4,5 Rarely death may occur.6

Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree