Algorithm 26-1. Algorithm for the evaluation and management of renal injury.
2 Grade I and II injuries rarely require further management. The bulk of blunt grade III and nonvascular grade IV injuries should be managed nonoperatively, whereas only selected penetrating injuries in hemodynamically stable patients can be managed on observation protocols.11,12 Lacerations with associated collecting system injury (i.e., grade IV) can initially be managed with observation, although a subset of patients will require ureteral stenting due to persistent urinary extravasation. A proposed modification to the AAST OIS stratifies major renal lacerations into “high risk” and “low risk” based on the likelihood of intervention for hemodynamic instability.13 The CT imaging criteria of ICE, medial parenchymal laceration, and perirenal hematoma rim distance >3.5 cm have been validated to predict the need for intervention and may lead to further refinement in nonoperative management.14
3 The surgical team must perform immediate intervention (surgery or angioembolization in selected situations) in hemodynamically unstable patients with no or transient response to resuscitation.2 Unstable patients will usually be found to have an expanding or pulsatile retroperitoneal hematoma at laparotomy, and occasionally have hilar injury or pedicle avulsion. In patients undergoing laparotomy for concomitant intraperitoneal injuries, exploration should only be considered judiciously for grade III or IV renal injury due to higher rates of nephrectomy under such circumstances.15 If renal exploration is contemplated or necessary, demonstration of contralateral renal function is important in the event of ipsilateral nephrectomy. This can be achieved by manual palpation or preferably by intraoperative single-shot intravenous urogram (KUB 10 minutes following intravenous injection of 2 mL/kg contrast).6 Reasons for failure to demonstrate contrast excretion from the contralateral kidney may indicate solitary kidney, hilar injury, hypoperfusion, or global renal insufficiency secondary to chronic renal disease. Exploration of a solitary kidney should be performed only when absolute indications exist.
Table 26-1 American Association for the Surgery of Trauma Organ Injury Scale

The kidney and upper urinary tract are accessed through a midline abdominal incision, and the author obtains preliminary isolation of the renal vessels before renal exploration. Using the inferior mesenteric vein (IMV) as a landmark, a posterior peritoneal window is created medial to the IMV overlying the aorta, which allows access, dissection, and control of the proximal renal vasculature.16 When immediate nephrectomy is required, reflection of the right or left colon provides rapid access to the renal hilum.17 If this method is employed, manual compression followed by vascular clamping may be required. Renal cooling is not routinely employed due to time constraints and potential for worsening hypothermia. Once Gerota fascia is exposed and open, the kidney can be freed of its associated perinephric fat. The capsule of the kidney is routinely preserved for closure following renal reconstruction. During renal exploration, sharp debridement, hemostasis, collecting system repair, and bolstered closure of the renal capsule using absorbable suture is performed. A perinephric suction drain is placed away from the repair in the retroperitoneum and removed when drainage subsides, usually less than 50 mL/day. If concern exists as the nature of the drainage, an aliquot of fluid can be sent for creatinine concentration to evaluate for the presence of urine.
In the case of renal artery thrombosis, surgical revascularization is rarely helpful because of the time delay from injury to revascularization. Intervention is commonly limited to patients with solitary kidney or bilateral injuries.5 An emerging therapy is vascular stent placement across the injury or thrombosis; however, most series are limited and results mixed.18 Venous injuries often result in massive bleeding and may require nephrectomy. Isolated proximal left renal vein injuries can potentially be managed by ligation of the renal vein because collateral drainage is present via the gonadal, adrenal, and lumbar veins. Right renal venous injury requires repair, if feasible, or nephrectomy due to lack of collateral circulation.
Clinicians should perform follow-up imaging for renal trauma patients with deep lacerations (AAST grades III, IV, and V) and clinical signs of complications (e.g., fever, worsening flank pain, ongoing blood loss, and abdominal distention).2 CT best delineates delayed bleeding, persistent urinary extravasation, urinoma, and infection.5 Secondary bleeding after nonoperative or surgical repair, which usually is caused by a pseudoaneurysm, should be managed angiographically. Ureteral stenting or percutaneous drainage is indicated for persistent leak or abscess. Late complications are uncommon and include renin-mediated hypertension from chronic renal ischemia, arteriovenous malformations, and segmental arteriolar pseudoaneurysm.
Ureter
Ureteral injuries are rare (1%), with fewer than 10 presenting annually in busy trauma centers.19 These injuries often present without clear signs or symptoms, and many are missed at the initial assessment (an algorithm for the evaluation and management of ureteral trauma is shown in Algorithm 26-2). Clinicians should perform IV contrast-enhanced abdominal/pelvic CT with delayed imaging for stable trauma patients with suspected ureteral injuries.2 In the adult population, gunshot wounds followed distantly by stab wounds are the most frequent source of injury associated with external violence.20,21
4 Injury should be suspected when organs anatomically related to the ureter sustain injury: iliac vessels, bladder, colon, and lumbar spine or transverse processes. Significant deceleration and hyperextension mechanisms can result in ureteral avulsion as well. In children, the avulsion injury occurs at the UPJ due to increased hyperextensibility of the spine.
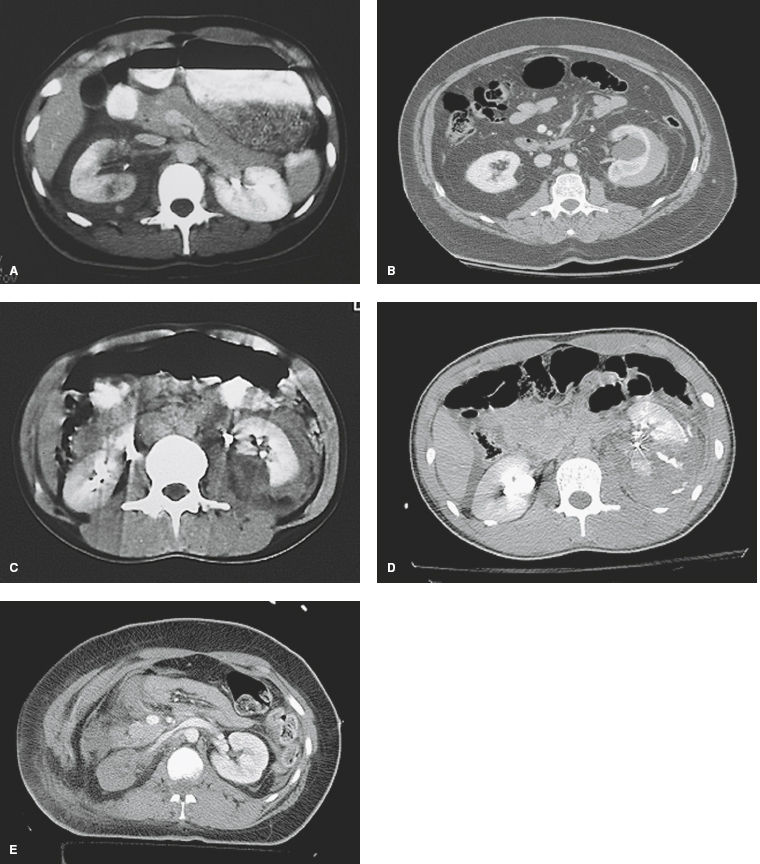
Figure 26-1. Grading of renal injury by computed tomography. A: Grade I, contusion; B: Grade II; C: Grade III; D: Grade IV, contrast extravasation; E: Grade V, devascularized.
Anatomically, the ureters begin posterior to the renal hilum at the UPJ. They course inferiorly through the retroperitoneum, along the anterior aspect of the psoas muscle. Upon entering the pelvis, the ureters run behind the gonadal vessels before crossing over the iliac vessels. Finally, the ureters continue caudally, and enter the inferior aspect of the bladder obliquely. The blood supply is segmental and arises from the adjacent anatomic structures within the retroperitoneum and pelvis (proximal-lateral, mid/true pelvis-medial, and inferior-posteriolateral).
Often, patients with penetrating ureteral injuries undergo surgical exploration for associated injuries. Surgeons should directly inspect the ureters during laparotomy in patients with suspected ureteral injury who have not had preoperative imaging.2 Traumatic ureteral contusions are best managed at the time of laparotomy with ureteral stenting or resection and primary repair depending on ureteral viability and clinical scenario.2

Algorithm 26-2. Algorithm for the evaluation and management of ureteral injury.
Surgeons should repair traumatic ureteral lacerations at the time of laparotomy in stable patients.2 Debridement as indicated precedes ureter reconstruction, and the level and length of ureteral defect dictates the type of repair (Fig. 26-2). UPJ disruptions require formal reconstruction by reanastomosis or ureteropyelostomy. For injuries occurring in the proximal to midureter without associated renal injury, simple mobilization of the colon without hilar control can be used to expose the ureters. Short upper and midureteral injuries are repaired by primary repair or spatulated reanastomosis over a stent, whereas low pelvic ureteric injuries are repaired by ureteroneocystostomy (Fig. 26-3). A refluxing implant is acceptable in children and adults.
When patients are hemodynamically unstable, surgeons should elect temporary urinary drainage followed by delayed definitive management.2 Damage control techniques for urinary diversion include debridement, drainage of the bladder and retroperitoneum, cutaneous ureterostomy diversion with a feeding tube, or ligation of the ureter with percutaneous nephrostomy tube placement.
Patients presenting with a delay in diagnosis often have symptoms of fever, flank pain, fullness, tenderness, atelectasis, or oliguria as a result of urinoma, hematoma, or abscess.19 Operative intervention at the time of delayed diagnosis can result in nephrectomy. Therefore, management options include ureteral stenting, nephrostomy tube placement, percutaneous urinoma drainage, and Foley catheter insertion. Reconstruction is planned at 3 to 6 months to allow for resolution of periureteral inflammation. Long-term complications of unrecognized ureteral injury include fistula, fluid collections, ureteral stricture, and obstructive uropathy.

Figure 26-2. Ureteral reconstruction by location of injury.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


