Patient Story
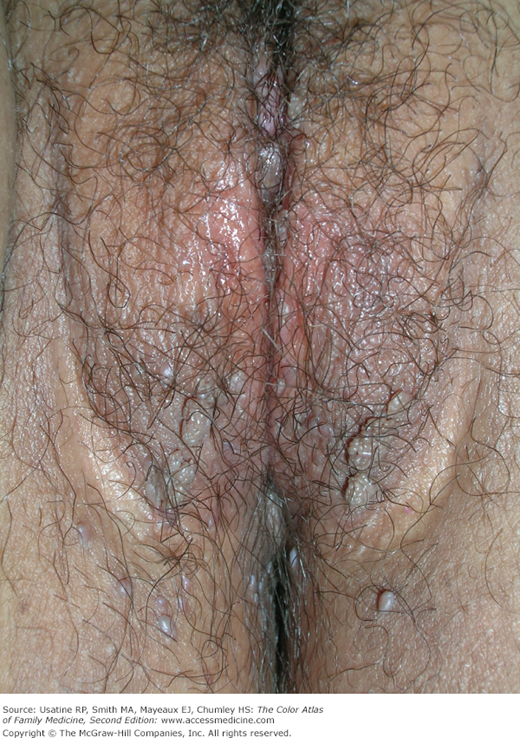
An 18-year-old woman presents with a concern that she might have genital warts (Figure 133-1). She has never had a sexually transmitted disease (STD) but admits to two new sexual partners in the last 6 months. She has not been vaccinated against human papillomavirus (HPV). The patient is told that her concern is accurate and she has condyloma caused by HPV (an STD). The treatment options are discussed and she chooses to have cryotherapy with liquid nitrogen followed by imiquimod self-applied beginning 2 weeks after cryotherapy. A urine test for gonorrhea and Chlamydia is performed and the patient is sent to the lab to have blood tests for syphilis and HIV. Fortunately, all the additional tests are negative. Further patient education is performed and follow-up is arranged.
Introduction
More than 100 types of HPV exist, with more than 40 that can infect the human genital area. Most HPV infections are asymptomatic, unrecognized, or subclinical. Low-risk HPV types (e.g., HPV types 6 and 11) cause genital warts, although coinfection with HPV types associated with squamous intraepithelial neoplasia can occur. Asymptomatic genital HPV infection is common and usually self-limited.1
Epidemiology
Etiology and Pathophysiology
Risk Factors
- Sexual intercourse and oral sex.
- Other types of sexual activity including digital-anal, oral-anal, and digital-vaginal contact.
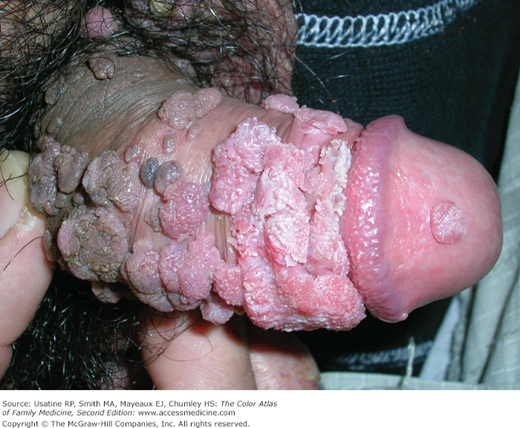
- Immunosuppression, especially HIV (Figure 133-2).
Diagnosis
- Diagnosis of genital warts is usually clinical based on visual inspection.1
- Genital warts are usually asymptomatic, and typically present as flesh-colored, exophytic lesions on the genitalia, including the penis, vulva, vagina, scrotum, perineum, and perianal skin.
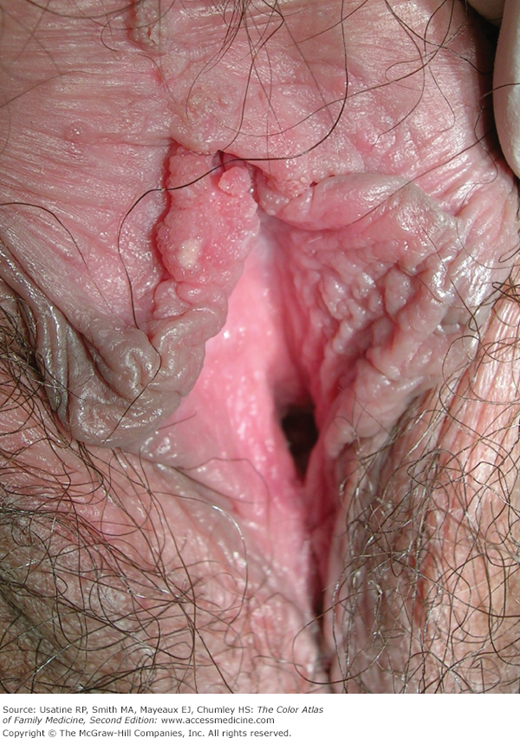
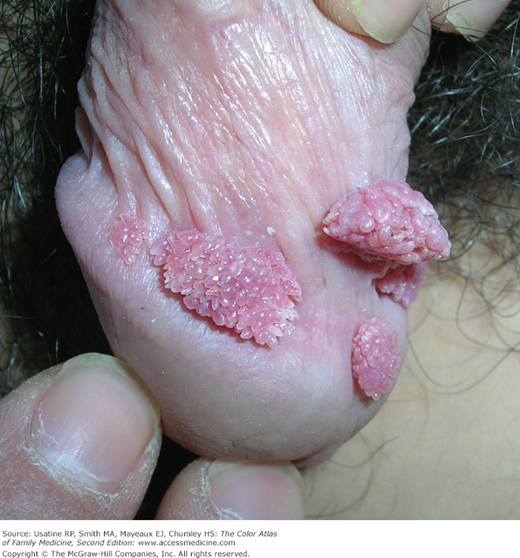
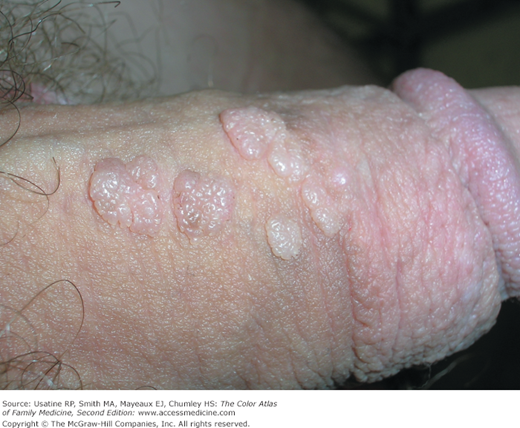
- External warts can appear as small bumps, or they may be flat, verrucous, or pedunculated (Figures 133-2, 133-3, and 133-4).
- Less commonly, warts can appear as reddish or brown, smooth, raised papules, or as dome-shaped lesions on keratinized skin.
- In women, the most common sites of infection are the vulva (85%) (Figure 133-1), perianal area (58%), and the vagina (42%) (Figure 133-3).
- In men, the most common sites of infection are the penis (Figures 133-4 to 133-5) and scrotum.
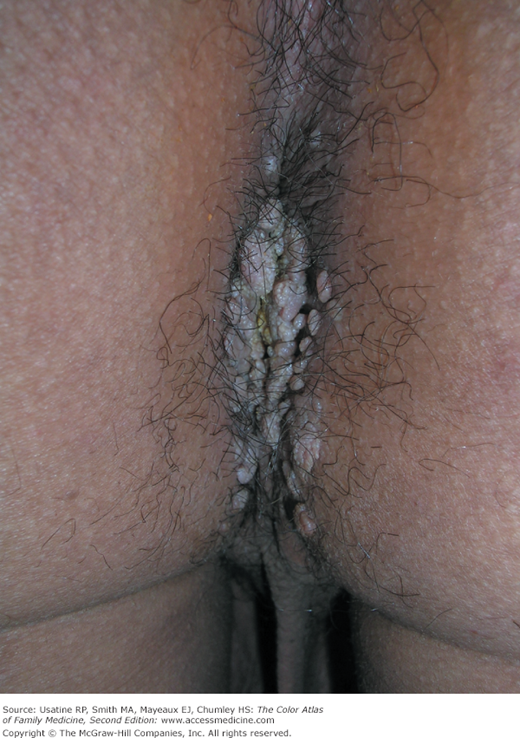
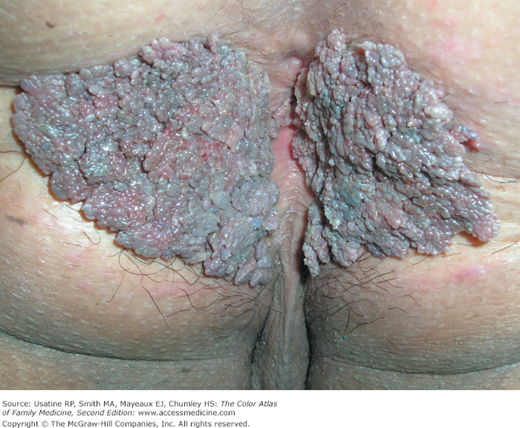
- Perianal warts (Figure 133-6) can occur in men or women who have a history of anal intercourse, and in those who do not have any such history (Figure 133-7).1
- Condyloma acuminata may be seen on the abdomen or upper thighs in conjunction with genital warts (Figure 133-8).
- Condyloma caused by HPV can be seen in obese individuals within the folds of the pannus (Figure 133-9).
- An RPR or VDRL should be ordered to screen for syphilis and a HIV test should be ordered as well. Genital warts are a sexually transmitted disease and patients who have one STD should be screened for others.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree