Patient Story
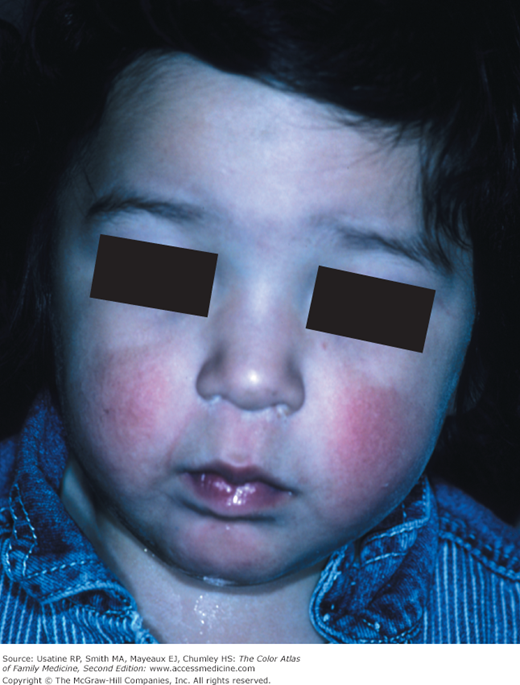
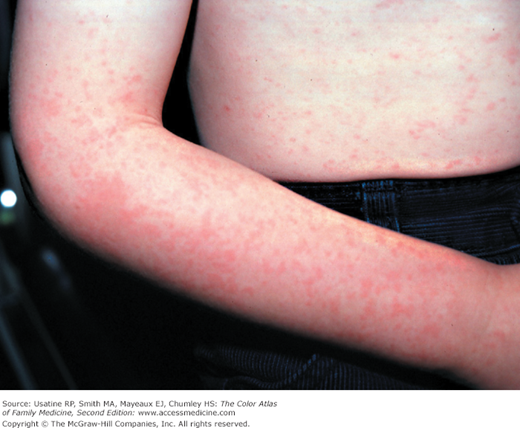
A 2-year-old boy presents with mild flu-like symptoms and a rash. He had erythematous malar rash and a “lace-like” erythematous rash on the trunk and extremities (Figures 127-1 and 127-2). The “slapped cheek” appearance made the diagnosis easy for fifth disease. The parents were reassured that this would go away on its own. The child returned to daycare the next day.
Introduction
Fifth disease is also commonly referred to as erythema infectiosum. The name derives from the fact that it represents the fifth of the six common childhood viral exanthems described. Transmission occurs through respiratory secretions, possibly through fomites, and parenterally via vertical transmission from mother to fetus and by transfusion of blood or blood products.
Epidemiology
- Fifth disease is common throughout the world. Antiparvovirus B19 immunoglobulin (Ig) G is found equally among Americans, Asians, and Europeans.1 The only known host for B19 is humans.
- Most individuals become infected during their school years.
- Fifth disease is very contagious via the respiratory route and occurs more frequently between late winter and early summer. Up to 60% of the population is seropositive for antiparvovirus B19 IgG by age 20 years.2 In some communities, there are cycles of local epidemics every 4 to 10 years.3
- Thirty percent to 40% of pregnant women lack measurable IgG to the infecting agent and are, therefore, presumed to be susceptible to infection. Infection during pregnancy can in some cases lead to fetal death.
Etiology and Pathophysiology
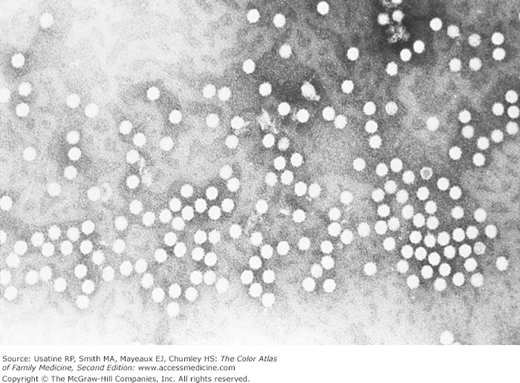
- Fifth disease is a mild viral febrile illness with an associated rash caused by parvovirus B19 (Figure 127-3).
- Most persons with parvovirus B19 infection never develop the clinical picture of fifth disease.
- Parvovirus B19 infects rapidly dividing cells and is cytotoxic for erythroid progenitor cells.
- After initial infection, a viremia occurs with an associated precipitous drop in the reticulocyte count and anemia. The anemia is rarely clinically apparent in healthy patients, but can cause serious anemia if the red blood cell count is already low. Patients with a chronic anemia such as sickle cell or thalassemia may experience a transient aplastic crisis.4
- Vertical transmission can result in congenital infection if a woman becomes infected during her pregnancy.5 The risk of a fetal loss or hydrops fetalis is greatest (loss rate of 11%) when the infection occurs within the first 20 weeks of gestation.6