Patient Story
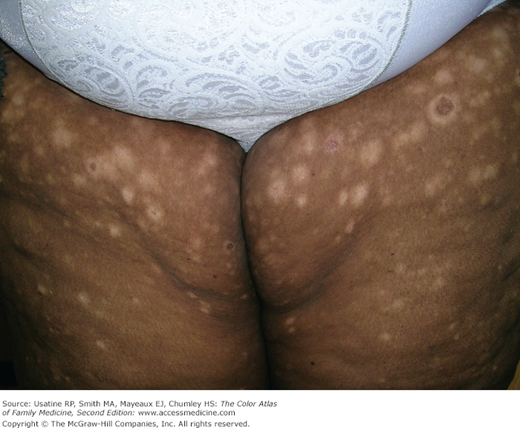
A 52-year-old black woman presented with a 7-month history of a hypopigmented rash in a symmetric distribution on her upper thighs and arms (Figures 176-1 and 176-2). She had been from evacuated New Orleans following Hurricane Katrina. She had waded through polluted waters for hours before being rescued by a boat. Four days passed before she had access to a shower at which time she noticed a single erythematous spot the size of a silver dollar on her left thigh. Over the next several weeks, it faded to hypopigmented macules and plaques and eventually spread to both thighs and arms. The physical examination revealed no lymphadenopathy. A hematoxylin and eosin (H&E) stain of a full-thickness punch biopsy revealed “cerebriform” lymphocytes at the dermal-epidermal junction characteristic of mycosis fungoides (MF), a type of cutaneous T-cell lymphoma (CTCL). Her blood tests were essentially normal, and she was HIV-negative. The patient reported no improvement with topical high-potency generic steroid to affected areas and is currently receiving narrow-band UVB treatment twice weekly.
Figure 176-1
The hypopigmented patches of mycosis fungoides on the thighs of a 52-year-old black woman. This is the patch stage of the disease. Although this mimicked vitiligo, the distribution and appearance warranted a biopsy that provided a definitive diagnosis of mycosis fungoides. (Courtesy of Richard P. Usatine, MD.)
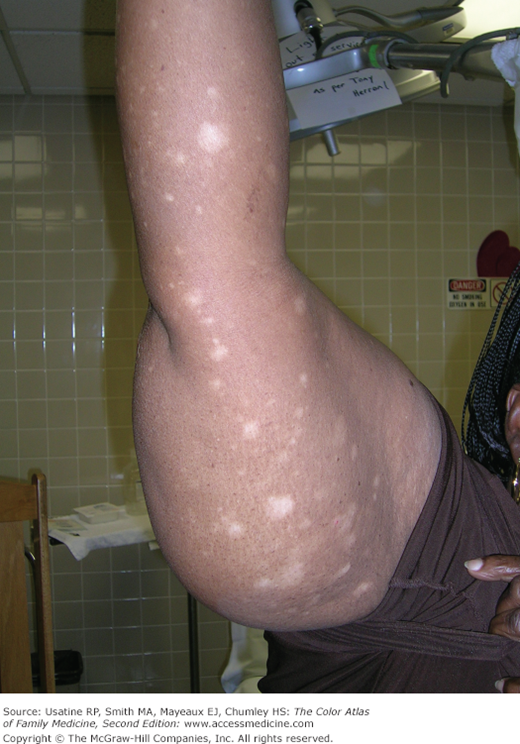
Figure 176-2
Hypopigmented patches on the arm of the woman in Figure 176-1 with mycosis fungoides. (Courtesy of Richard P. Usatine, MD.)
Introduction
CTCL clinically and biologically represent a heterogeneous group of non-Hodgkin lymphomas, with MF and Sézary syndrome being the most common subtypes.1
Epidemiology
- The annual incidence of CTCL in the United States has increased from 2.8 per 1 million (1973 to 1977) to 9.6 per 1 million (1998 to 2002) according to data from Criscione and Weinstock.2
- CTCL is a rare disease, with 1000 new cases per year in the United States, comprising approximately 0.5% of all non-Hodgkin lymphoma cases.3,4
- The two most common types of CTCL are MF (50% to 72%), which is generally indolent in behavior, and Sézary syndrome (1% to 3%), an aggressive leukemic form of the disease.2
- It is more common in African Americans than in whites, with an incidence ratio of 6:1.3
- It is more common in males, with a male-to-female ratio of 2:1.
- Median age at presentation is between 50 and 70 years,2 although pediatric and young adult cases do occur.1
Etiology and Pathophysiology
- The exact etiology of CTCL is unknown, but environmental, infectious, and genetic causes have been suggested. CTCL is a malignant lymphoma of helper T cells that usually remain confined to skin and lymph nodes (LNs). MF is a specific type of CTCL named for the mushroom-like skin tumors seen in severe cases.3
- Human T-lymphocytic virus (HTLV) types 1 and 2, HIV-1, cytomegalovirus (CMV), Epstein-Barr virus (EBV), and Borrelia burgdorferi have been suggested, but unproven, infectious causes of MF.4,5 Environmental exposure to Agent Orange may be responsible for some cases.3 There is one case report of possible conjugal transmission of MF between a heterosexual couple who developed advanced MF within 14 months of one another.5
- MF and Sézary syndrome (SS) are associated with specific human leukocyte antigen (HLA) types (Aw31, Aw32, B8, Bw38, and DR5).4 Genetic predisposition is also suggested by detection of HLA class II alleles DRB1*11 and DQB1*03 in association with sporadic and familial malignancy and familial clustering among Israeli Jews.4,6
- Metastasis, to the liver, spleen, lungs, GI tract, bone marrow, and the central nervous system (CNS) may occur via T-cell spread through the lymphatic system.3,4
- The reduction of T-cell receptor complexity contributes to immunosuppression in advanced MF and SS, and may manifest clinically as herpes simplex or zoster.7 Death is usually secondary to systemic infection, especially from Staphylococcus aureus and Pseudomonas aeruginosa.
- Host antitumor immunity also deteriorates, and patients have an increased risk for secondary malignancies, including higher-grade non-Hodgkin lymphoma, Hodgkin disease, secondary melanoma, and colon cancer in addition to cardiopulmonary complications.7
Diagnosis
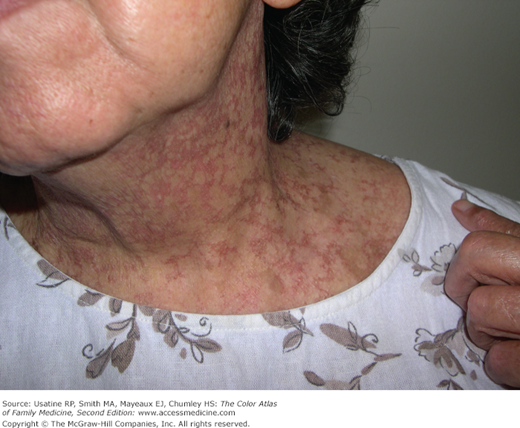
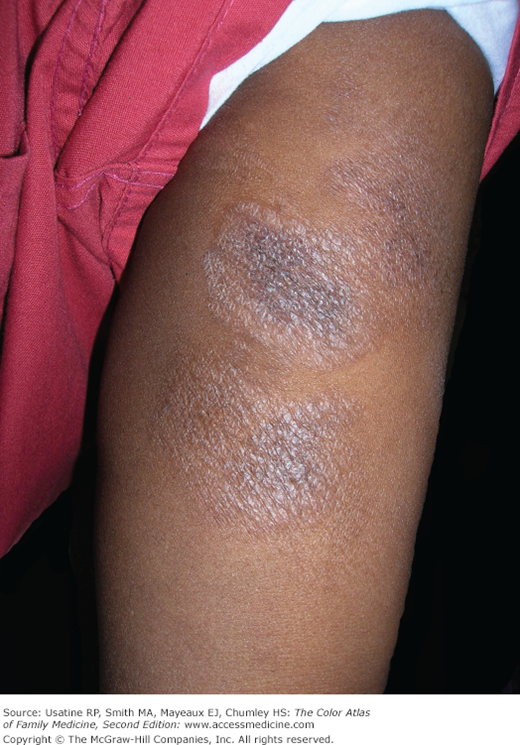
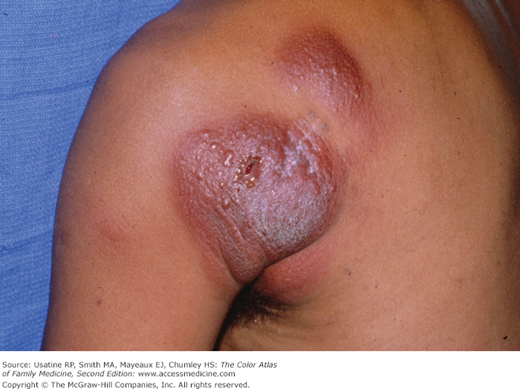
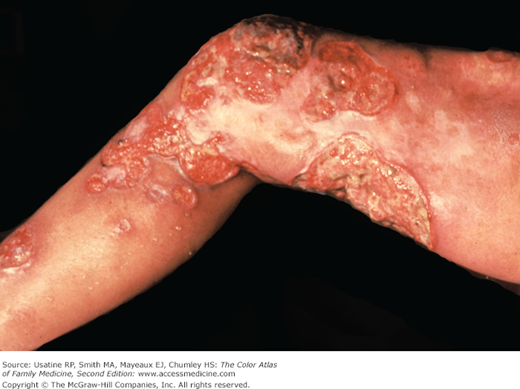
- The most common initial presentation involves patches or scaly plaques with a persistent rash that is often pruritic and usually erythematous (Figures 176-1, 176-2, 176-3, and 176-4).3 Patches may evolve to generalized, infiltrated plaques or to ulcerated, exophytic tumors (Figures 176-5 and 176-6).4,8
- Hypo- or hyperpigmented lesions, petechiae, poikiloderma (skin atrophy with telangiectasia), and alopecia with or without mucinosis are other findings. The folliculotropic variant of MF presents with spotty alopecia (Figure 176-7).
- A “premycotic” phase may precede definitive diagnosis for months to decades, which involves nonspecific, slightly scaling skin lesions that intermittently appear and may eventually resolve with topical steroids.
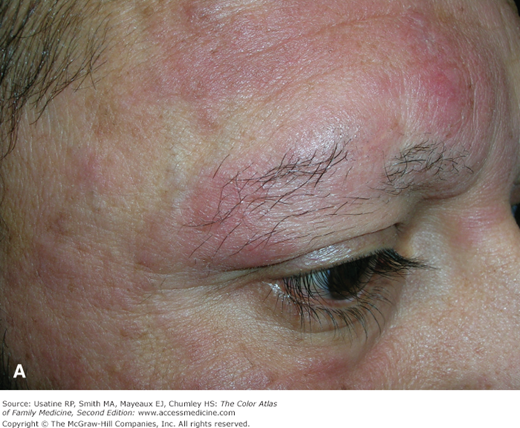
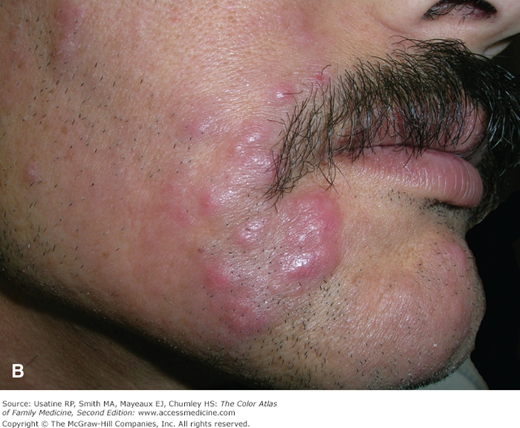
- SS is characterized by generalized exfoliative erythroderma, lymphadenopathy, and atypical Sézary cells in the peripheral blood. Diffuse infiltration of malignant T cells in SS may exaggerate facial lines, creating a leonine facies.8
- “Invisible MF” describes pruritus without visible lesions but the skin biopsy is positive for monoclonal T-cell infiltrates.4