Objectives
- Define the terms clearance and metabolic clearance rate, and differentiate between general clearance and specific renal clearance.
- List the information required to calculate clearance.
- State the criteria that must be met for a substance so that its clearance can be used as a measure of glomerular filtration rate; state which substances are used to measure glomerular filtration rate and effective renal plasma flow.
- Given data, calculate the clearance of any excreted substance.
- Predict whether a substance undergoes net reabsorption or net secretion by comparing its clearance with that of inulin or by comparing its rate of filtration with its rate of excretion.
- Given data, calculate net rate of reabsorption or secretion for any substance.
- Given data, calculate fractional excretion of any substance.
- Describe how to estimate glomerular filtration rate from creatinine clearance and describe the limitations of this estimate.
- Describe how to use plasma concentrations of urea and creatinine as indicators of changes in glomerular filtration rate.
The Clearance Concept
![]() Metabolic waste products, ingested substances, and excess salt and water are constantly being removed from the body (cleared) by a number of means, including disposal in the urine, in the feces, biochemical transformation in the liver, and for volatile substances, exhalation. The rate of removal can be expressed in several ways, a common one being the plasma half-life. Another way to express removal rate is clearance, which is the volume of plasma per unit time from which all of a specific substance is removed. Clearance in a biomedical context has both a general meaning and a specific renal meaning. The general meaning is simply that a substance is removed from the plasma by any of the mechanisms mentioned above. Its quantitative measure is called the metabolic clearance rate. Renal clearance, on the contrary, means that the substance is removed from the plasma and excreted in the urine. As explained below the clearance of certain substances is a method to measure glomerular filtration rate (GFR). Evaluation of GFR via renal clearance is commonly used clinically as an overall assessment of renal health. Repeated assessments over a period of time can indicate whether renal function is stable or deteriorating.
Metabolic waste products, ingested substances, and excess salt and water are constantly being removed from the body (cleared) by a number of means, including disposal in the urine, in the feces, biochemical transformation in the liver, and for volatile substances, exhalation. The rate of removal can be expressed in several ways, a common one being the plasma half-life. Another way to express removal rate is clearance, which is the volume of plasma per unit time from which all of a specific substance is removed. Clearance in a biomedical context has both a general meaning and a specific renal meaning. The general meaning is simply that a substance is removed from the plasma by any of the mechanisms mentioned above. Its quantitative measure is called the metabolic clearance rate. Renal clearance, on the contrary, means that the substance is removed from the plasma and excreted in the urine. As explained below the clearance of certain substances is a method to measure glomerular filtration rate (GFR). Evaluation of GFR via renal clearance is commonly used clinically as an overall assessment of renal health. Repeated assessments over a period of time can indicate whether renal function is stable or deteriorating.
Clearance Units
![]() The units of renal clearance are often confusing to the first-time reader, so let us be sure of the meaning. First, the units are volume per time (not amount of a substance per time). The volume is the volume of plasma that supplies the amount excreted in a given time. For example, suppose each liter of plasma contains 10 mg of a substance X, and 1 mg of substance X is excreted in 1 hour. Then 0.1 L of plasma supplies the 1 mg that is excreted, that is, the renal clearance is 0.1 L/h. The reader should appreciate that removing all of a substance from a small volume of plasma is equivalent to removing only some of it from a larger volume, which is actually the way the kidneys do it. If all of substance X is removed from 0.1 L in 1 hour, this is equivalent to removing half of it from 0.2 L, or one quarter of it from 0.4 L, and so on. The clearance is 0.1 L/h in all these cases.
The units of renal clearance are often confusing to the first-time reader, so let us be sure of the meaning. First, the units are volume per time (not amount of a substance per time). The volume is the volume of plasma that supplies the amount excreted in a given time. For example, suppose each liter of plasma contains 10 mg of a substance X, and 1 mg of substance X is excreted in 1 hour. Then 0.1 L of plasma supplies the 1 mg that is excreted, that is, the renal clearance is 0.1 L/h. The reader should appreciate that removing all of a substance from a small volume of plasma is equivalent to removing only some of it from a larger volume, which is actually the way the kidneys do it. If all of substance X is removed from 0.1 L in 1 hour, this is equivalent to removing half of it from 0.2 L, or one quarter of it from 0.4 L, and so on. The clearance is 0.1 L/h in all these cases.
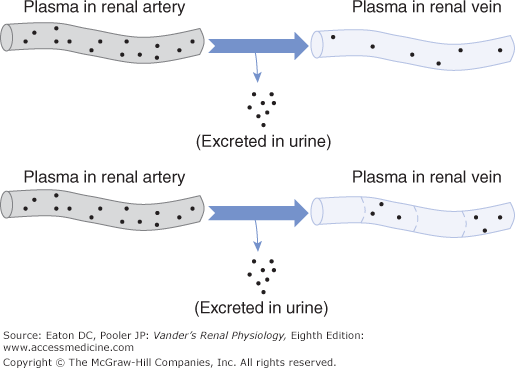
These concepts are illustrated in Figure 3–1. As the kidneys clear a substance, plasma leaving the kidney in the renal vein has a lower concentration of the substance than does plasma entering the kidney in the renal artery. This is equivalent to dividing the plasma into sequential segments in which all of the substance is removed from some segments and none from others.
Figure 3–1.
Renal clearance. When plasma is cleared of a solute, the solute concentration in venous plasma leaving the kidney is lower than in arterial plasma entering the kidney, as shown in the upper part of the figure. This is equivalent to dividing the plasma into segments in which all the solute is removed from some segments and none from others, as shown in the bottom of the figure. The volume of plasma from which all the solute has been removed, when expressed on a time basis, is the clearance of the solute in units of volume per time.
The general meaning and specific renal meaning of clearance are illustrated by comparing how the body handles 2 substances with similar-sounding names but very different properties: inulin and insulin. Insulin is the familiar pancreatic hormone involved in regulating blood glucose. It is a protein with a molecular weight of 5.8 kD and is small enough to be freely filtered by the glomerulus. Once in Bowman’s space, it moves along with every other filtered substance into the proximal convoluted tubule, where it is largely taken up by endocytosis and degraded into its constituent amino acids. Very little insulin escapes this uptake, and very little of the filtered insulin makes it all the way to the urine. Thus, the kidney takes part in clearing insulin from the blood, but because so little appears in the urine, the specific renal clearance is very low (<1 mL/min). However, the body has additional mechanisms for clearing insulin, and its metabolic clearance rate is quite high (half-life less than 10 minutes). Let us contrast this with inulin. Inulin is a polysaccharide starch of about 5-kD molecular weight that is not usually found in the body. Like insulin, it is freely filtered by the glomerulus, but it is not reabsorbed or secreted by the nephron. All the inulin that is filtered flows through the nephron and appears in the urine. Thus, the renal clearance of inulin is relatively large. Inulin in the blood is not taken up by other tissues, and the kidneys are the only excretion route. As we will see, this makes inulin a very special substance for measuring GFR.
Clearance measures the volume of plasma from which all of the substance is removed and excreted in a given time. |
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree