Autonomic Nervous System
OVERVIEW OF THE AUTONOMIC NERVOUS SYSTEM
Role of the Autonomic Nervous System
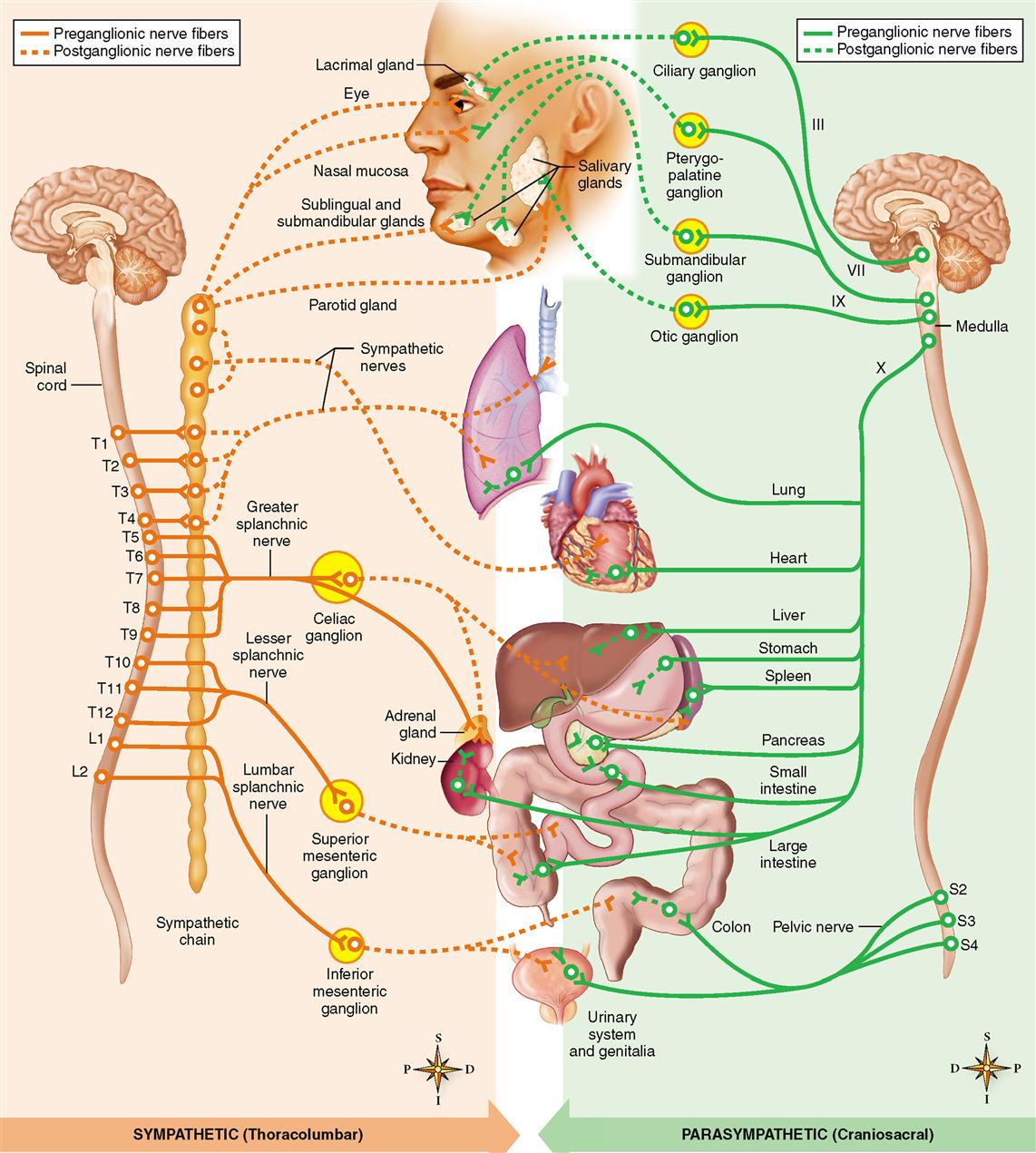
The autonomic nervous system (ANS) is a subdivision of the nervous system that regulates involuntary effectors (Figure 16-1). Because it controls involuntary effectors, we can think of the autonomic system as our system of subconscious regulation of body functions.
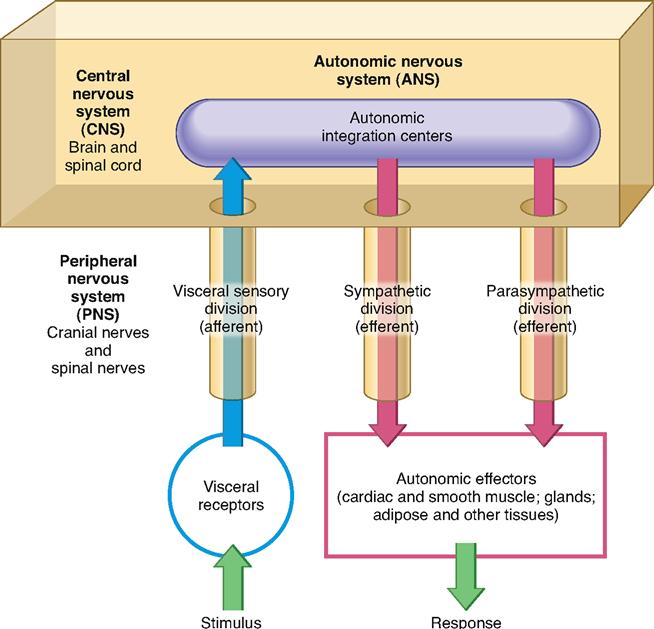
It is the ANS that carries efferent signals to the autonomic, or visceral, effectors—cardiac muscle, smooth muscle, glandular epithelia, and adipose and other tissues (Box 16-1). Some autonomic pathways connect to the skeletal muscles, which are ordinarily considered somatic effectors. In skeletal muscles, subconscious autonomic stimulation helps prevent fatigue during intense exercise—it does not directly control muscle contractions.
The major functions of the ANS are heartbeat regulation, smooth muscle contraction, glandular secretion, and metabolism regulation in ways that maintain homeostatic balance or respond to threats to that balance. Recall from the previous chapter that autonomic (visceral) reflexes can produce these effects over a visceral reflex pathway, which you can see illustrated as a simple reflex arc in Figure 16-1.
Divisions of the Autonomic Nervous System
Although the ANS also includes sensory (afferent) pathways that provide the feedback necessary to regulate effectors, we will emphasize the motor (efferent) pathways in this chapter. Sensory functions as a whole are discussed in the next chapter.
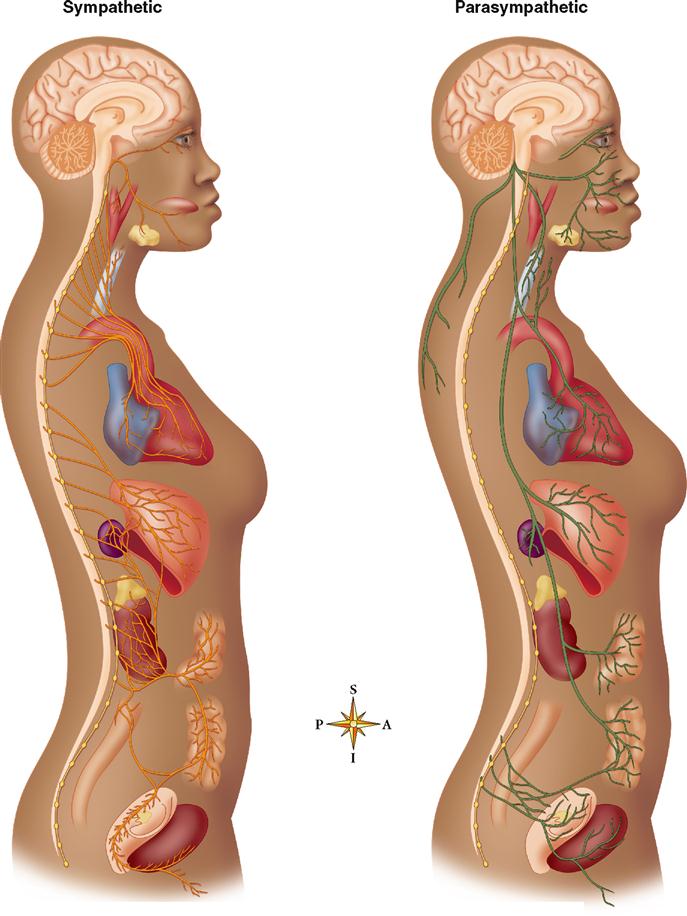
The ANS has two efferent divisions: the sympathetic division and the parasympathetic division. The sympathetic division consists of neural pathways that are separate from the parasympathetic pathways.
As you can see in Figure 16-2, however, even though the two divisions follow separate pathways, many autonomic effectors are dually innervated. That is, many autonomic effectors receive input from both sympathetic and parasympathetic pathways.
In dually innervated effectors, the effects of the two systems are often antagonistic: one inhibits the effector and the other stimulates the effector. This is similar to the antagonistic effects of an accelerator and brake in a vehicle. The opposing influences allow a dually innervated effector to be controlled with remarkable precision. Such antagonism also allows a dually innervated effector to participate in timed events, such as the sexual response, in which effectors must be stimulated and then rapidly inhibited (or vice versa) in a specific timed sequence.
Some autonomic effectors are singly innervated, receiving input from only the sympathetic division.
STRUCTURE OF THE AUTONOMIC NERVOUS SYSTEM
Basic Plan of Autonomic Pathways
Each efferent autonomic pathway, whether sympathetic or parasympathetic, is made up of autonomic nerves, ganglia, and plexuses. These structures, in turn, are made up of efferent autonomic neurons. They conduct impulses away from the brainstem or spinal cord to autonomic effectors. As with all efferent neurons, efferent autonomic neurons function in reflex arcs. Thus as with somatic motor regulation, efferent autonomic regulation ultimately depends on feedback from the sensory pathways.
A relay of two autonomic neurons conducts information from the central nervous system (CNS) to the autonomic effectors. The first is called a preganglionic neuron—an awkward name but a descriptive one. Preganglionic neurons conduct impulses from the brainstem or spinal cord to an autonomic ganglion, locating them before the ganglion—thus preganglionic. Within an autonomic ganglion, the preganglionic neuron synapses with a second efferent neuron. Because this second neuron conducts impulses away from the ganglion and to the effector, it is called the postganglionic neuron.
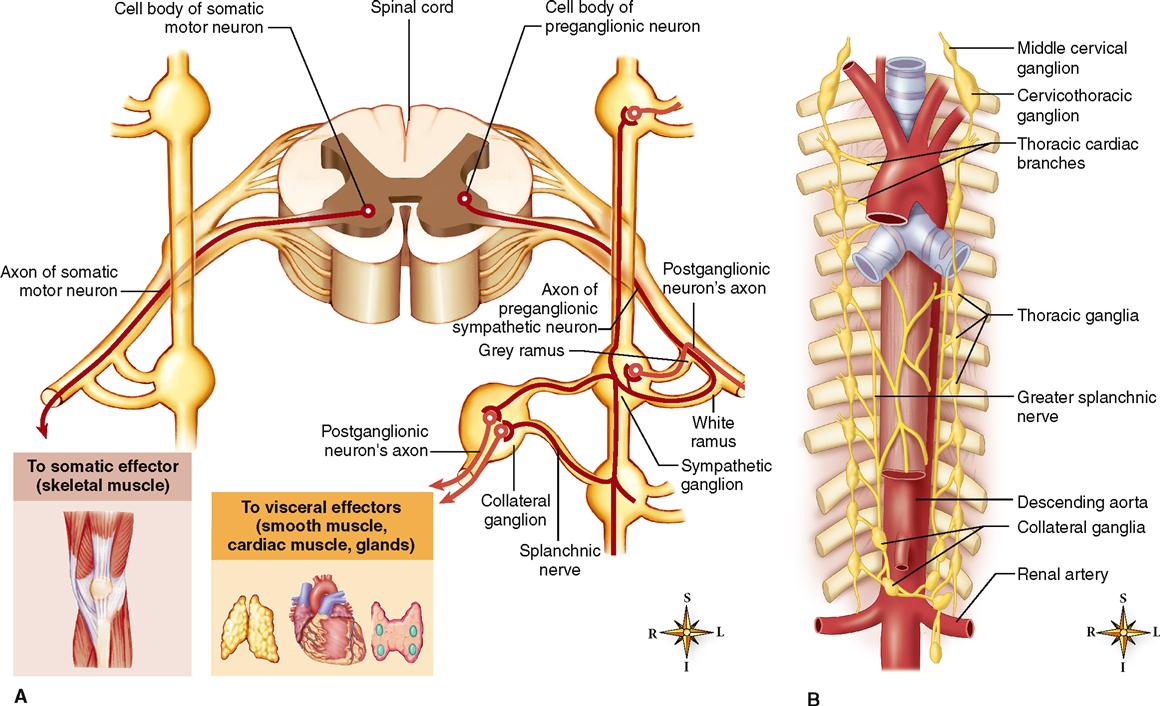
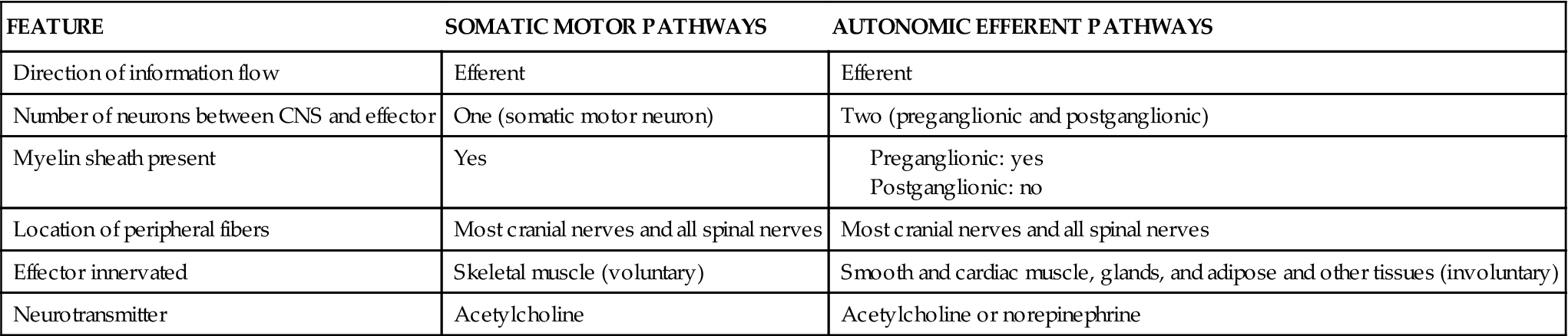
As you can see in Figure 16-3, A, this plan fundamentally differs from the efferent pathways of the somatic motor nervous system. Conduction to somatic effectors requires only one efferent neuron, the somatic motor neuron that originates in the anterior gray horn of the spinal cord. Conduction to autonomic effectors, however, requires a sequence of two efferent neurons from the CNS to the effector. Essential features of the somatic motor pathways and autonomic efferent pathways are further compared and contrasted in Table 16-1.
TABLE 16-1
Comparison of Somatic Motor and Autonomic Pathways
Structure of the Sympathetic Pathways
SYMPATHETIC PREGANGLIONIC NEURONS
Sympathetic preganglionic neurons begin within the spinal cord. Specifically, they have their dendrites and cell bodies within the lateral gray horns of the thoracic and lumbar segments of the spinal cord (see Figure 16-3, A). For this reason, the sympathetic division has also been called the thoracolumbar division.
Most of the ganglia of the sympathetic division lie along either side of the anterior surface of the vertebral column (see Figure 14-3, p. 423). Both gray rami and white rami are sympathetic rami. Sympathetic axon collaterals bridge the gap between adjacent ganglia that lie on the same side of the vertebral column. This arrangement forms a structure that resembles a chain of beads (see Figure 16-3, B). Thus the linked ganglia are often referred to as the sympathetic chain ganglia, or the sympathetic trunk.
Each chain runs from the second cervical vertebra in the neck all the way down to the level of the coccyx. There are usually 22 sympathetic chain ganglia on each side of the vertebral column: three cervical, eleven thoracic, four lumbar, and four sacral. Axons of sympathetic preganglionic neurons leave the cord by way of the ventral roots of the thoracic and first four lumbar spinal nerves. From there, they split away from other spinal nerve fibers by means of a small branch called the white ramus. The white ramus gets its name from the fact that most of the sympathetic preganglionic fibers within it are myelinated axons. Note in Figure 16-3 that the sympathetic preganglionic axon extends through the white ramus to a sympathetic chain ganglion.
If we trace the axon inside the sympathetic chain ganglion, we see that the preganglionic fiber may branch along any of three paths:
1. It can synapse with a sympathetic postganglionic neuron.
3. It can pass through one or more ganglia without synapsing.
Preganglionic neurons that pass through chain ganglia without synapsing continue on through splanchnic nerves to other sympathetic ganglia (see Figures 16-3 and 16-4). These collateral ganglia, or prevertebral ganglia, are pairs of sympathetic ganglia located a short distance from the spinal cord. The collateral ganglia are named for nearby blood vessels. For example, the celiac ganglion (also called the solar plexus) is a large ganglion that lies next to the celiac artery just below the diaphragm. Other examples include the superior mesenteric ganglion and the inferior mesenteric ganglion, each located close to the beginning of an artery of the same name.
Some of the preganglionic fibers that enter the celiac ganglion do not synapse there but continue on to the central portion (medulla) of the adrenal gland. Within the adrenal medulla, they synapse with modified postganglionic neurons. These modified postganglionic cells are actually endocrine cells that release hormones (mostly epinephrine) into the bloodstream. These chemical messengers may reach the various sympathetic effectors, where they enhance and prolong the effects of sympathetic stimulation.
SYMPATHETIC POSTGANGLIONIC NEURONS
Most of the sympathetic postganglionic neurons have their dendrites and cell bodies in the sympathetic chain ganglia or collateral ganglia.
Some postganglionic axons return to a spinal nerve by way of a short branch called the gray ramus, so named because most postganglionic fibers are unmyelinated (see Figure 16-3). Once in the spinal nerve, the postganglionic fibers are distributed with other nerve fibers to the various sympathetic effectors. On the other hand, some postganglionic fibers are distributed to sympathetic effectors by way of separate autonomic nerves. The course of postganglionic fibers through these autonomic nerves is complex, involving the redistribution of fibers in autonomic plexuses before they reach their respective destinations.
In the sympathetic division, preganglionic neurons are relatively short, and postganglionic neurons are relatively long.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree