http://evolve.elsevier.com/Edmunds/NP/
 Top 100 drug;
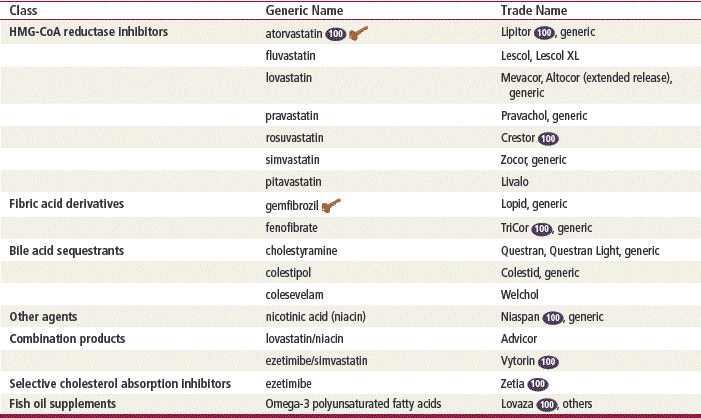
Top 100 drug;  key drug. Atorvastatin (Lipitor) is the most commonly prescribed antihyperlipidemic drug. Atorvastatin confers robust LDL lowering (30%-50%), has a relatively favorable drug–drug interaction profile, and is well tolerated. It is most important to note that atorvastatin (similar to most other statins) has consistent clinical outcome data to demonstrate that its use can significantly decrease cardiovascular morbidity and mortality.
key drug. Atorvastatin (Lipitor) is the most commonly prescribed antihyperlipidemic drug. Atorvastatin confers robust LDL lowering (30%-50%), has a relatively favorable drug–drug interaction profile, and is well tolerated. It is most important to note that atorvastatin (similar to most other statins) has consistent clinical outcome data to demonstrate that its use can significantly decrease cardiovascular morbidity and mortality.
Coronary heart disease is the single largest cause of mortality and cause of disability in both men and women in the United States. Hyperlipidemia is a primary, major risk factor for CHD. The use of statins to treat hyperlipidemia and to lessen the burden of heart disease is one of the greatest advances in cardiovascular therapeutics in recent history. This chapter describes appropriate patient selection, drug selection, and necessary monitoring when one is caring for patients with hyperlipidemia. The National Cholesterol Education Program (NCEP) guidelines are the most widely recognized clinical guidelines for hyperlipidemia, and their application is discussed. Students are encouraged to familiarize themselves with the NCEP guidelines to enhance their ability to provide evidence-based medicine to their patients.
Therapeutic Overview
Cholesterol and triglycerides are classified as lipids, and both are normal and vital constituents of plasma. Because they are hydrophobic and insoluble, they are transported in the plasma via lipoproteins. Five major classes of lipoproteins have been identified: chylomicrons, VLDLs, IDLs, LDLs, and HDLs. Chylomicrons and VLDLs are considered triglyceride-rich lipoproteins, whereas IDLs, LDLs, and HDLs are considered cholesterol-rich lipoproteins. Of the lipoproteins, evaluation of LDLs, which includes IDL and HDL levels, is of primary importance. These two lipoproteins differ in several respects, including their cholesterol transport activities. Simply stated, LDL transports cholesterol from the liver to peripheral tissues; conversely, HDL removes cholesterol from the periphery and transports it to the liver. Chylomicrons are the largest and least dense of the lipoproteins, followed in order of increasing density and decreasing size by VLDLs (or pre-β), intermediate low-density lipoproteins (ILDLs, or broad β), LDLs (or β), and HDLs (or α).
Pathophysiology
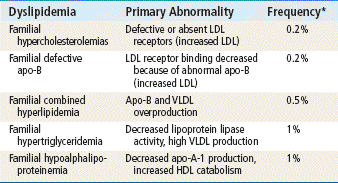
A variety of lipid disorders can occur as a primary event or an event that is related to some underlying disease. Dyslipidemia can result from genetic disorders, concomitant disease states, or environmental factors. Alterations in lipoprotein metabolism are complex and often multifactorial. The primary dyslipidemias are associated with overproduction or impaired removal of lipoproteins. Primary dyslipidemias and their associated abnormalities are listed in Table 24-1. Often, the cause of primary dyslipidemia is not identified and plays little or no role in the diagnosis and treatment of most patients.
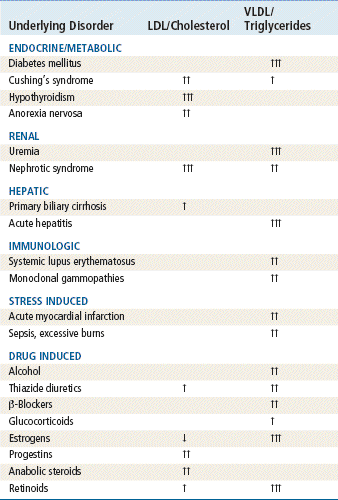
Table 24-2 provides a list of causes that contribute to secondary hyperlipidemia. If the clinician determines that a patient’s hyperlipidemia may be related to another process, correction or modification of this process should be sought before pharmacologic treatment is provided for the hyperlipidemia. Not mentioned in Table 24-2 is obesity, which may also produce lipoprotein alterations. In diabetes, triglyceride levels are related to the degree of glycemic control. In hypothyroidism, lipid abnormalities are corrected with thyroxine replacement. In uremia, an elevated triglyceride and low HDL level is observed. Elevated total cholesterol and triglycerides are seen in patients with nephrotic syndrome. In drug-induced hyperlipidemia, estrogens may increase HDL, whereas β-blockers, progestins, and anabolic steroids may decrease HDL.
Disease Process
Overwhelming scientific evidence supports a causal relationship between hyperlipidemia and CHD. Premature coronary atherosclerosis, leading to manifestations of CHD, is the most common and important consequence of hyperlipidemia. Elevated LDL cholesterol is a significant and positive predictor of CHD. Although cholesterol likely contributes to CHD in multiple ways, a major mechanism is LDL oxidation. Oxidation causes the lipoproteins to become “sticky” and facilitates their adhesion to the endothelium of blood vessels, thus causing atherosclerosis. An inverse correlation has been noted between HDL and CHD risk, so that elevated HDL cholesterol is considered protective against the development of CHD. Roughly 50% of Americans have cholesterol levels that place them at increased risk of CHD.
Most data point to an association between elevated triglycerides as an independent risk factor for CHD, although data are conflicting. Obesity, inactivity, cigarette smoking, excess alcohol, high carbohydrate intake, diseases (e.g., type 2 diabetes, renal failure, nephrotic syndrome), and drugs (e.g., corticosteroids, estrogens, retinoids) are known to be risk factors for elevated triglycerides.
Assessment
As a screening measure, a fasting lipoprotein profile should be obtained every 5 years in adults, beginning at the age of 20 years. Serum cholesterol should be assessed more frequently in patients who have risk factors for CHD. Lipid profiles should be obtained in the fasting state (>12 hours since last meal) for an accurate measurement of triglycerides and LDL. Patients should be evaluated for common secondary causes of hyperlipidemia (i.e., diseases and drugs). Assessment of the patient’s lifestyle, including diet and exercise, is crucial.
Mechanism of Action
These drugs (commonly called “statins”) are reversible, competitive inhibitors of HMG-CoA reductase, which is the rate-limiting enzyme in cholesterol biosynthesis. HMG-CoA reductase catalyzes the conversion of HMG-CoA to mevalonate, a cholesterol precursor, in the liver. Inhibition of this enzyme decreases cholesterol synthesis, particularly causing a decrease in the serum LDL level. Although the mechanism of action appears straightforward, most LDL lowering observed with these drugs results from secondary, compensatory changes produced by enzyme inhibition. Inhibition of HMG-CoA reductase reduces intracellular cholesterol concentrations, leading to increased synthesis and expression of LDL receptors in the liver. This upregulation of LDL receptors is a compensatory response intended to restore intracellular cholesterol homeostasis. As the concentration of LDL receptors increases, a rise in the catabolic clearance of LDL from the plasma is observed.
In addition to their impressive LDL-lowering effects, HMG-CoA reductase inhibitors increase HDL and decrease triglycerides modestly. These drugs also decrease levels of C-reactive protein, decreasing inflammatory processes that may be associated with atherosclerosis.
Fibric Acid Derivatives
Despite our lengthy experience with gemfibrozil, several uncertainties surround its precise mechanism of action. Its primary lipoprotein effect is to decrease triglyceride and raise HDL concentrations. The ability of gemfibrozil to lower triglycerides is attributed to an increase in lipoprotein lipase activity, which results in increased catabolism of VLDL. Gemfibrozil also may suppress lipolysis in adipose tissue, decrease free fatty acid flux, and lower the rate of triglyceride synthesis. The increase in HDL observed with gemfibrozil may result from increased synthesis of apolipoprotein A-1, or it may be indirectly related to the drug’s ability to lower VLDL. Gemfibrozil exerts a variable and minor effect on LDL levels.
Fenofibrate is a prodrug that is converted to its active metabolite, fenofibric acid. Fenofibric acid inhibits triglyceride synthesis and accelerates the removal of lipoproteins.
Bile Acid Sequestrants
Bile acid sequestrants are unique among the antihyperlipidemics because they are not absorbed systemically, and they are the safest drugs available for the treatment of hypercholesterolemia. Although they differ in their chemical structure, all are large copolymers that function as anion-exchange resins in the intestinal lumen. Here they bind to bile acids, forming an insoluble complex and producing a large increase in the fecal excretion of bile acids. The pathways involved in cholesterol and bile acid metabolism are intertwined and closely related. Although the resin agents are sequestering bile acids and are interrupting their enterohepatic recirculation, a 3- to 10-fold increase has been noted in the diversion of cholesterol into bile acid synthesis. This resultant decline in intracellular cholesterol concentrations leads to two compensatory changes: acceleration of HMG-CoA reductase activity, and upregulation of LDL cell surface receptors. The two homeostatic changes increase intracellular cholesterol concentrations for conversion to bile acids, either by increased cholesterol synthesis or by increased uptake and removal of LDL from plasma. Therefore, bile acid sequestrants increase the diversion of cholesterol to bile acid synthesis, lower intracellular stores of cholesterol, and result in increased catabolism of LDL by the liver.
Nicotinic Acid (Niacin) (Niaspan)
Niacin is believed to act on a hormone-sensitive lipase; this leads to inhibition of release of free fatty acids from adipose tissue (lipolysis). The inhibition of lipolysis leads to reduced free fatty acid transport to the liver and therefore decreased synthesis of VLDL. This decrease in VLDL in turn causes a reduction in LDL. An increase in lipoprotein lipase activity produced by nicotinic acid is believed to increase the rate of chylomicron triglyceride removal from the plasma. The mechanism underlying the increase in HDL is thought to result from reduced lipid transfer of cholesterol from HDL to VLDL and by delayed HDL clearance. The clinical benefits and potential harm for nicotinic acid are in question following the AIM-HIGH study addressed later in the chapter.
Selective Cholesterol Absorption Inhibitors
Ezetimibe is the first, and only, agent in a class of drugs referred to as selective cholesterol absorption inhibitors. Ezetimibe is known to localize in the intestinal wall, where it is converted to its active glucuronide metabolite. It appears to act on the brush border of intestinal epithelial cells, where it selectively inhibits the absorption of cholesterol from dietary and biliary sources. Reduced cholesterol absorption results in a decrease in the delivery of cholesterol to the liver. Less cholesterol is thus available in hepatic stores, allowing more cholesterol to be cleared from the blood. Ezetimibe does not affect the absorption of fat-soluble vitamins or triglycerides—a benefit over bile acid sequestrants. Ezetimibe and/or its glucuronide conjugates circulate enterohepatically, repeatedly delivering the agent back to the intestine and reducing systemic exposure. Clinical benefit of ezetimibe is questionable. Modifying chemicals (which serve as surrogate markers for actual bad outcomes) via different pharmacologic mechanisms unfortunately does not always result in clinical benefit that is meaningful to patients.
Fish Oil Supplements
Omega-3 polyunsaturated fatty acids (PUFAs), mainly eicosapentaenoic acid (EPA) and docosahexaenoic acid (DHA), are essential nutrients. Lovaza is a highly concentrated combination of esters of EPA and DHA. The primary mechanism of action for PUFAs is a reduction (approximately 45%) in the hepatic production of triglycerides, which reduces production of VLDL. HDL is largely unaffected and LDL may increase. Adverse events are usually mild and include eructation, dyspepsia, and taste perversion.
Treatment Principles
This chapter incorporates the updated Adult Treatment Panel (ATP) III guidelines for the treatment of hyperlipidemia from the National Cholesterol Education Program (NCEP, 2004). (See http://www.nhlbi.nih.gov/guidelines/cholesterol/index.htm.) Other useful hyperlipidemia guidelines from the American Association of Clinical Endocrinologists can be found at http://www.aace.com/pub/guidelines/. (New guidelines will be announced in 2013.)
USDHHS Expert Panel, Integrated Guidelines for the Cardiovascular Health and Risk Reduction in Children and Adolescents, National Heart Lung and Blood Institute: http://www.nhlbi.nih.gov/guidelines/cvd_ped/index.htm.
Evidence-Based Recommendations
Dyslipidemia is a major treatable risk factor for coronary artery disease. Lowering LDL results in significant decreases in coronary events, including transient ischemic attacks and stroke. As primary prevention, lipid-lowering therapies decrease risk of CHD events and mortality in patients without a history of CHD (1A). In persons with diabetes, LDL reduction produces a more substantial decrease in cardiovascular disease than does blood glucose control (1A). Patients without coronary artery disease should be evaluated with respect to their global cardiac risk to determine whether lipid-lowering therapy is indicated. Statin therapy should be considered as secondary prevention for all patients with coronary heart disease, peripheral vascular disease, or history of stroke. These medications have been shown to decrease coronary heart disease and mortality even if baseline LDL is <100 mg/dl (1A). Statins reduce 5-year overall mortality and cardiovascular morbidity and mortality; the greatest reductions occur in patients at greatest risk (1A). A new “black box” warning has been mandated by the FDA for statins because of the increased occurrence of muscle pain, diabetes, and memory loss in patients. In addition, the side effects and potential “harm” of statins are often minimized and not adequately discussed or addressed with patients. Also, the benefit of lowering cholesterol or LDL in older people and primary prevention in women are of questionable value. Little substantial data exist to support primary prevention in women, but this is rarely stated, and women and men are often classed together in discussions about prevention.
Cardinal Points of Treatment
The most widely recognized treatment guidelines for hyperlipidemia, those of the NCEP, were most recently updated in 2004, although it is anticipated that another update will be released in 2013. An important tenet of these guidelines is that the intensity of evaluation and treatment depends on the patient’s overall risk status for CHD (Box 24-1)—that is, those patients with preexisting CHD or with CHD risk equivalents or those who are at high risk (more than two risk factors) for CHD in the near future are treated more aggressively. Next, patients with two or more risk factors should be further classified into 10-year risk groups based on their Framingham point scores. (See Framingham tables at www.nhlbi.nih.gov/guidelines/cholesterol/risk.) Framingham scores are based on age, total cholesterol level, smoking status, HDL cholesterol, and systolic blood pressure. They are used to assess the individual’s 10-year risk of developing CHD. Three levels of 10-year risk are identified: >20%, 10% to 20%, and <10%. Those found to have a risk >20% are categorized as if they had a CHD risk equivalent (for further information, see NCEP guidelines).