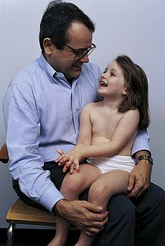
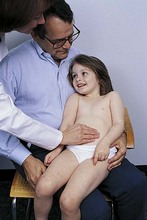
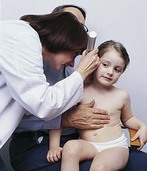
While child plays on the floor, evaluate musculoskeletal and neurologic system while developing a rapport with child.
Observe child’s spontaneous activities.
Ask child to demonstrate skills such as throwing a ball, building block towers, drawing geometric figures, coloring.
Evaluate gait, jumping, hopping, range of motion.
Muscle strength: Observe child climbing on parent’s lap, stooping, and recovering.
CHILD ON PARENT’S LAP
Perform examination on parent’s lap; the adult and the patient generally enjoy the experience more and you, sitting on a stool, preferably with your eyes at the child’s eye level, will find it easier than the examining table.
Begin with child sitting and undressed except for diaper or underpants.
Upper extremities
Inspect arms for movement, size, shape; observe use of hands; inspect hands for number and configuration of fingers, palmar creases.
Elicit biceps and triceps reflexes.
Take blood pressure at this point or later.
Lower extremities
Child may stand for much or part of examination.
Inspect legs for movement, size, shape, alignment, lesions.
Inspect feet for alignment, longitudinal arch, number of toes.
Palpate femoral and dorsalis pedis pulses.
Elicit plantar, Achilles, and patellar reflexes.
Head and neck
Inspect shape, alignment with neck, hairline, position of auricles.
Palpate anterior fontanel for size (age appropriate); head for sutures, depressions; hair for texture.
Measure head circumference (up to age 36 months).
Inspect neck for webbing, voluntary movement.
Palpate neck: thyroid, muscle tone, lymph nodes, position of trachea.
Chest, heart, lungs
Inspect chest for symmetry, respiratory movement, size, shape, precordial movement, deformity, nipple and breast development.
Palpate anterior chest, locate point of maximal impulse, note tactile fremitus in talking or crying child.
Auscultate anterior, lateral, and posterior chest for breath sounds; count respirations.
Auscultate all cardiac listening areas for S
1 and S
2, splitting, murmurs; count apical pulse.
CHILD RELATIVELY SUPINE, STILL ON LAP, DIAPER LOOSENED
Auscultate for bowel sounds.
Palpate: Identify size of liver and any other palpable organs or masses.
Palpate femoral pulses; compare with radial pulses.
Palpate for inguinal lymph nodes.
Inspect external genitalia.
Males: Palpate scrotum for descent of testes and other masses; crossing the legs in the tailor position helps bring testes down.
CHILD STANDING
Inspect spinal alignment as child bends slowly forward to touch toes.
Observe posture from anterior, posterior, lateral views.
CHILD ON PARENT’S LAP
The following steps, often delayed to the end of the examination by many, are more easily performed with a child of appropriate age sitting on a parent’s or surrogate’s lap:
Inspect eyes: Corneal light reflex, red reflex, extraocular movements, funduscopic examination.
Perform otoscopic examination. Note position and description of pinnae.
Inspect mouth and pharynx. Note number of teeth, deciduous or permanent, and any special characteristics.
Note: By the time child is of school age, it is usually possible to use an examination sequence very similar to that for adults.) See pp. 306-316 for examples of forms used to chart physical growth.
AGE-SPECIFIC ANTICIPATED OBSERVATIONS AND GUIDELINES*
Again this is a suggested outline, always modified by human variation, and that all percentages are subject to Gaussian distribution. History building can be facilitated by referring to baby books, report cards, pictures, and other materials the family may have at home. Of course, you must in a nonemergent situation begin with a full history and physical examination when you first see the patient (at whatever age).
2 WEEKS OF AGE
History (particular attention)
Pertinent perinatal history
Social: Sleeping arrangements, housing
Umbilicus: Healing, discharge, granulation
Diet: Feeding modality, schedule
Development: By this age:
80% will lift and turn head when in prone position
40% will follow an object to midline visually
35% will vocalize, become quiet in response to a voice
45% will regard a face intently, diminishing activity for the moment
Physical examination (particular attention)
Establish growth curves (weight, height, head circumference).
Test reflexes: Moro, root, grasp, step.
Anticipatory guidance (particular attention)
Sleep (emphasize supine position and avoidance of soft and fuzzy threats to safe breathing)
Feeding: Use of pacifier (need to suck)
Use of bulb syringe (nasal stuffiness)
Safety: Falling, crib sides, car seats
Illness: Temperature taking
Crying (holding the baby)
Plans and problems
What risks have revealed themselves as you got to know the family? What are apparent problems? Start a problem list and make appropriate dispositions.
Consider need for hemoglobin or hematocrit value.
Consider immunization needs and, throughout, attempt to follow American Academy of Pediatrics guidelines; on each visit, discuss benefits, risks, side effects of immunizations (always remember risks for the immunocompromised).
2 MONTHS OF AGE
History (particular attention)
Expressions of parental concern
Child’s apparent temperament
Feeding patterns, frequency
Stooling pattern, frequency, color, consistency, straining
Be certain there is no probability of immunocompromise in patient or relevant family members or other contacts (before starting immunizations).
Social issues:
Smoking, other concerning habits
Any apparent high-risk concerns
Development: By this age
Gross motor:
80% will lift head to 45 degrees in prone position.
45% will lift head to as much as 90 degrees in prone position.
25% will roll over stomach to back.
Fine motor:
99%+ will follow a moving object to midline.
85% will follow a moving object past midline.
Language:
Almost all will diminish activity at the sound of a voice.
35% will spontaneously vocalize.
Many will vocalize responsively.
Psychosocial:
Almost all will diminish activity when regarding a face.
Almost all will respond to a friendly, cooing face with a social smile.
50% may smile spontaneously or even laugh aloud.
Physical examination (particular attention)
Growth curves (weight, height, head circumference)
Anticipatory guidance
Feeding (delay or at least downplay solids; avoid citrus, wheat, mixed foods, eggs; minimize water)
When and if mother returns to work
Visual and auditory stimulus (mobiles, mirrors, rattles, singing and talking to baby)
Sibling rivalry (if there are siblings)
Babysitters (checking references, ensuring immunization status, reliability)
Safety (rolling over, playpen, car seat, discourage walker, no smoking)
Sleep (reemphasize location and supine position)
Smoking and contribution to poor health
Plans and problems
Review immunizations and implement as appropriate.
List problems (e.g., allergies, medications, any areas of concern), and make appropriate plans and, if necessary, referrals.
Consider need for hemoglobin or hematocrit value.
4 MONTHS OF AGE
History (particular attention)
Infant’s sleep cycle and temperament
Feeding patterns, frequency, mother’s feelings if she is breast-feeding
Stooling pattern, frequency, color, consistency, straining
Social issues:
Amplification of early impressions of home’s social structure
Smoking, other concerning habits
Any apparent high-risk concerns
Development: By this age
Gross motor:
80%, when prone, will lift chest up with arm support.
80% will roll over from stomach to back.
35% will have no head lag when pulled to sitting position, and many will then hold head steady when kept in that position.
Fine motor:
60% will reach for a dangling object.
Almost all will bring hands together.
Almost all will follow a face or object up to 180 degrees.
Language:
Almost all will laugh aloud.
20% will appear to initiate vocalization.
Psychosocial:
80% will smile spontaneously.
Many will regard their own hand for several seconds.
Physical examination (particular attention)
Update growth curves (weight, height, head circumference).
Anticipatory guidance
Introduction of solid food (cereal)
Stool changes with changes in diet
Thumb sucking, pacifiers, bottles at bedtime
Safety (aspiration, rolling over, holding baby with hot liquids, reemphasize earlier discussions [e.g., car seat])
Reemphasis on environmental stimulus
Further discussion of babysitters
Use of antipyretics (e.g., acetaminophen)
Plans and problems
Review immunizations and implement as appropriate.
Maintain problem list, making appropriate plans and, if necessary, referrals.
Consider need for hematocrit or hemoglobin value.
6 MONTHS OF AGE
History (interim details)
Further exploration of social issues
If either parent has not attended these care visits regularly, encourage his or her participation, and address relevant issues.