Chapter 7 THE GASTROINTESTINAL TRACT
Introduction
 The overall prevalence of GI diseases is not exactly known, but the estimate is that approximately 70 million people are affected yearly.
The overall prevalence of GI diseases is not exactly known, but the estimate is that approximately 70 million people are affected yearly.
 Gastrointestinal diseases account for 50 million physician office visits per year.
Gastrointestinal diseases account for 50 million physician office visits per year.
 Approximately 10 million people are hospitalized for GI diseases yearly, which account for 15% of all hospitalizations.
Approximately 10 million people are hospitalized for GI diseases yearly, which account for 15% of all hospitalizations.
 Approximately 200,000 people die every year from GI diseases, mostly neoplasms.
Approximately 200,000 people die every year from GI diseases, mostly neoplasms.
Gastrointestinal disease may have many causes. The relative clinical significance of various GI diseases is presented graphically in Figure 7-1.
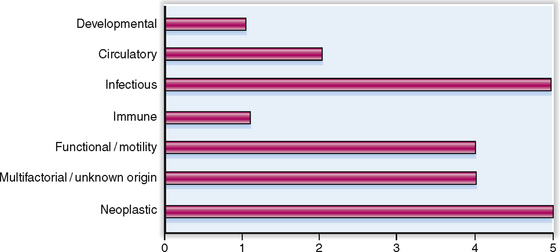
Figure 7-1 Relative clinical significance of various gastrointestinal diseases grouped by their cause.
Anatomy and Physiology
Absorption Uptake of nutrients and fluid from the intestinal lumen into the circulation. Most of the absorption of nutrients occurs in the small intestine, but some nutrients are absorbed in the stomach and the large intestine as well.
Anus Terminal part of the gastrointestinal tract, lined in part by columnar mucosa similar to the rest of the large intestine, and in part by squamous epithelium.
Appendix Usual term for vermiform (“wormlike”) appendix, an outpouching of the cecum.
Chyme Semifluid mixture of partially digested food and digestive juices formed in the stomach and passed into the small intestine.
Digestion Complex process leading to the breakdown of food into water-soluble elementary components that can be readily absorbed.
Duodenum Part of the small intestine linking the stomach with the jejunum.
Enteroendocrine cells Neuroendocrine cells found into the small and large intestine. They secrete various polypeptide hormones (e.g., cholecystokinin, gastrin) and can be impregnated with silver stains (thus called “argentaffin”). These cells contain membrane-bound cytoplasmic granules, which can be seen by electron microscopy. In microscopic sections they are best demonstrated by immunohistochemistry using antibodies to chromogranin or synaptophysin (staining all neuroendocrine cells) or antibodies to specific polypeptide hormones. These cells give rise to tumors known as carcinoids or neuroendocrine carcinomas.
Enterokinase Enzyme in the brush border of enterocytes in the small intestine. It activates trypsinogen.
Esophagus Intrathoracic tubular organ lined by squamous epithelium connecting the pharynx with the stomach.
Ingestion Process that begins with the intake of food, followed by chewing (mastication), moistening by saliva, and swallowing (deglutition).
Large intestine (colon) Part of the lower gastrointestinal tract connecting the ileum and the anus. It consists of several parts: cecum, ascending colon, transverse colon, descending colon, sigmoid colon, and rectum.
Mucosa-associated lymphoid tissue (MALT) Lymphoid tissue organized into follicles that are found inside the mucosa of the gastrointestinal or respiratory system. These aggregates may be seen microscopically or macroscopically, as in the small intestine where they form Payer’s patches.
Small intestine Longest part of the gastrointestinal tract, connecting the stomach with the large intestine. It comprises the duodenum, jejunum, and ileum.
Stomach Part of the gastrointestinal tract between the esophagus and the duodenum. It begins at the cardia and ends at the pylorus. The main part of the stomach is called the body. The upper part of the stomach is called the fundus, and the lower the pyloric antrum. The stomach contributes to digestion by secreting hydrochloric acid, pepsin, and several gastroenteric hormones such as gastrin.
Clinical and Laboratory Findings and Procedures
Achlorhydria Secretory failure of the stomach that makes it unable to produce hydrochloric acid.
Anorexia Loss of appetite or refusal to eat.
Constipation Reduced defecation caused by delayed transit of intestinal contents. For practical purposes it means passing fewer than three stools per week.
Diarrhea Increase in stool frequency or volume. In Western countries it usually means that the stool weighs more than 300 g/day and contains more water than normal. It is said that the stool takes the form of its container.
Dyspepsia Term used for a variety of symptoms pertaining to the upper gastrointestinal tract and stomach. Such symptoms include abdominal pain, bloating, nausea, or general discomfort after feeding.
Dysphagia Subjective feeling of difficulty while swallowing food or fluids. It can be caused by anatomic obstruction of the esophagus or functional disturbances in esophageal motility.
Encopresis Involuntary or voluntary defecation in adults or children older than 4 years of age.
Endoscopy Examination of the inside of a hollow organ using a flexible or rigid endoscopic instrument. Depending on the organ examined the endoscopic procedures are called esophagoscopy, rectoscopy, colonoscopy, and so on.
Flatulence Passing of gases from the anus.
Hematemesis Vomiting of blood.
Hematochezia Passing of blood from the rectum.
Ileus Failure of caudal progress of bowel contents because of defective propulsive motility of the intestines (“adynamic or paralytic ileus”).
Laparoscopy Procedure for visualizing the internal organs with an endoscopic instrument introduced into the abdominal cavity through the abdominal wall.
Melena Passing of black stools, typically due to bleeding from the upper gastrointestinal tract. The black color results from the interaction of the hydrochloric acid with the blood in the stomach or the small intestines.
Nausea Unpleasant subjective sensation in the throat or epigastrium usually accompanied by an urge to vomit.
Vomiting Forceful expulsion of the upper gastrointestinal contents through the mouth. It is typically associated with nausea. It is mediated by involuntary spasmodic contractions of the abdominal and chest musculature and the relaxation of the lower esophageal sphincter. If no gastrointestinal contents are expulsed the process is called retching or dry heaves. Rumination is effortless regurgitation of the swallowed food without nausea and spasmodic contractions.
Gastrointestinal Diseases
Achalasia Inability to relax, specifically used to describe spasms of the lower esophageal sphincter that cause dysphagia and proximal dilatation of the esophagus.
Anastomosis Communication between two hollow organs surgically attached to one another.
Angiodysplasia Acquired vascular abnormality most often located in the large intestine of older persons. It is an important cause of occult intestinal bleeding.
Atresia Congenital absence of a lumen of a hollow organ (e.g., esophageal or intestinal atresia) or an orifice (e.g., atresia of the anus).
Barrett’s esophagus Esophageal disease characterized by intestinal metaplasia of the normal squamous epithelium.
Carcinoid Low-grade malignant tumor of neuroendocrine cells. May be found anywhere in the gastrointestinal tract and the bronchi, but most often in the small intestine.
Carcinoma of the colon and rectum Adenocarcinoma, originating in various parts of the large intestine.
Carcinoma of the esophagus Adenocarcinoma or squamous cell carcinoma, most frequently found in the lower third of the esophagus.
Carcinoma of the stomach Adenocarcinoma, originating in various parts of the stomach.
Celiac disease Also known as celiac sprue or gluten-sensitive enteropathy. An autoimmune intestinal disease characterized by malabsorption related to intolerance of certain grains (gluten, gliadin).
Colitis Inflammation of the large intestine. It may be acute or chronic, diffuse or segmental. It may be caused by infection or toxins or it may be idiopathic, as in ulcerative colitis and Crohn’s disease.
Crohn’s disease Inflammatory bowel disease of unknown origin. It is transmural and typically affects the terminal ileum and the right side of the colon in a discontinuous manner.
Dumping syndrome Syndrome caused by rapid passage of food from the stomach into the small intestine, most often encountered in persons who have partial gastric resection of gastrointestinal anastomoses. Clinically it is characterized by dizziness, sweating, nausea, tachycardia, and subsequent diarrhea.
Enteritis Inflammation of the small intestine that may involve the entire small intestine or only some of its parts (e.g., duodenitis, ileitis). It is often associated with colitis and thus called enterocolitis. It is typically associated with diarrhea or, if chronic, with malabsorption. It may be infectious or autoimmune (e.g., celiac disease) or idiopathic (e.g., Crohn’s disease).
Familial polyposis coli Autosomal dominant syndrome characterized an occurrence of multiple colonic polyps that almost invariably undergo malignant transformation into colon cancer.
Gastritis Inflammation of the mucosa of the stomach. It may be acute or chronic, atrophic or hypertrophic, erosive or nonerosive. It may be caused by infections (e.g., Helicobacter pylori), chemicals and drugs (e.g., alcohol and nonsteroidal anti-inflammatory drugs), or autoimmune mechanisms.
Gastroesophageal reflux disease (GERD) Set of clinical symptoms related to the reflux of gastric acid into the esophagus due to inadequate function of the lower esophageal sphincter, diaphragmatic hernia, or increased intra-abdominal pressure compressing the stomach.
Gastrointestinal stromal tumor (GIST) Benign or malignant tumor composed of undifferentiated stromal cells. Such tumors may be found anywhere in the gastrointestinal tract from the esophagus to the anus and even in the mesentery and extraintestinal sites of the abdomen.
Gastrointestinal tumors Tumors originating in the gastrointestinal tract, including benign tumors (tubular and villous adenomas); adenocarcinomas of the esophagus, stomach, and intestines; squamous cell carcinoma of the esophagus; carcinoids and neuroendocrine carcinomas; lymphomas and various benign and malignant stromal tumors.
Hemorrhoids Dilated veins of the internal or external hemorrhoidal plexus, often harboring thrombi.
Hereditary nonpolyposis colorectal carcinoma (HNPCC) Autosomal dominant condition characterized by the appearance of adenocarcinomas of the large intestine. It is related to the mutation of the mismatch repair genes and microsatellite genetic instability.
Hernia Protrusion of abdominal contents (e.g., intestinal loops) outside of the abdominal cavity. Includes inguinal, diaphragmatic, and umbilical hernias, but also several other less common forms.
Irritable bowel syndrome Functional disturbance of unknown origin characterized by recurrent bouts of abdominal pain, bloating, and diarrhea alternating with constipation.
Ischemic bowel disease Intestinal changes related to acute or chronic ischemia, usually related to atherosclerotic narrowing of intestinal arteries or thrombi and emboli. May manifest in the form of minor functional disturbances (e.g., pain, colic, diarrhea, or constipation), hematochezia, or catastrophic extensive intestinal necrosis.
Lactase deficiency Deficiency of lactase in the intestinal mucosa, characterized by diarrhea precipitated by ingestion of milk or milk-containing food.
Malabsorption syndrome Gastrointestinal syndrome characterized by incomplete absorption of nutrients and fluids from the intestinal lumen. It may be caused by intestinal, pancreatic, biliary, or gastric diseases.
Obstruction Failure of passage or caudal progression of food in the upper alimentary tract or intestinal contents due to a mechanical barrier. May be caused by tumors; fecal impaction; foreign bodies; or intestinal adhesions, hernia, volvulus, and intussusception.
Peptic ulcer disease Multifactorial inflammatory disease, often related to H. pylori infection, causing a bleeding defect in the duodenal and gastric mucosa.
Peritonitis Inflammation of the peritoneal lining of the abdominal cavity, which may be caused by infection and chemicals (sterile peritonitis).
Pneumoperitoneum Accumulation of air inside the abdominal cavity, usually due to perforation of the stomach or intestines.
Pyloric stenosis Narrowing of the pyloric part of the stomach due to hyperplasia and hypertrophy of the pyloric sphincter. Most often encountered in male infants.
Ulcer Mucosal defect caused by ischemia, infection, or complex mechanisms such as occurs in peptic ulcers of the stomach and duodenum.
Ulcerative colitis Inflammatory bowel disease of unknown origin involving the colon in a diffuse manner and presenting with confluent mucosal ulcerations.
Varices Abnormally dilated veins, usually found in the esophagus, stomach, or the hemorrhoidal plexus of the rectum and anus.
Normal Structure and Function
NORMAL ANATOMY AND HISTOLOGY
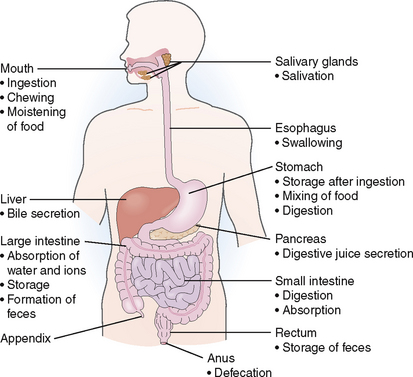
The GI, or alimentary, tract includes the hollow organs stretching from the mouth to the anus, that is, the GI tract proper; and the solid organs, such as the salivary glands, the liver, and pancreas, that are attached to them (Fig. 7-2). In this chapter we deal only with the GI tract proper, whereas the liver and the pancreas are described in subsequent chapters.
The gastrointestinal tract can be divided for practical purposes into two parts: the upper and the lower GI tract.
The wall of the gastrointestinal tract consists of several distinct histologic layers arranged in a similar manner from the pharynx to the anus.
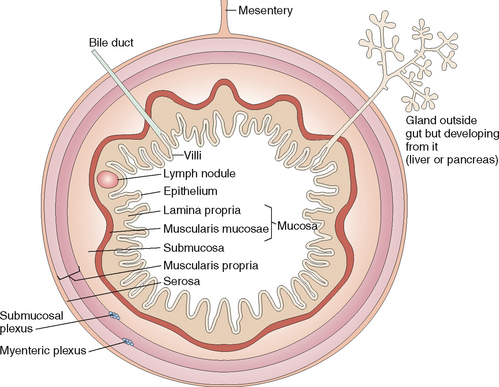
The viscera of the GI tract have a stereotypic structure and consist of four principal layers: the mucosa, submucosa, muscularis propria, and serosa (Fig. 7-3).
 Mucosa. The mucosa consists of an epithelial lining and the connective tissue lamina propria mucosae. The mouth and esophagus are covered with squamous epithelium that provides protection against the coarse particles found in ingested food. In the stomach and the intestines the mucosa is composed of secretory or absorptive glandular cells that are important for digestion and absorption of food. The lamina propria consists of connective tissue, vessels, and scattered cells of the mucosa-associated lymphoid tissue (MALT).
Mucosa. The mucosa consists of an epithelial lining and the connective tissue lamina propria mucosae. The mouth and esophagus are covered with squamous epithelium that provides protection against the coarse particles found in ingested food. In the stomach and the intestines the mucosa is composed of secretory or absorptive glandular cells that are important for digestion and absorption of food. The lamina propria consists of connective tissue, vessels, and scattered cells of the mucosa-associated lymphoid tissue (MALT).
 Submucosa. It is composed of loose connective tissue containing numerous blood and lymphatic vessels, cells of the MALT, and submucosal (Meissner’s) nerve plexus. The submucosa is an important passageway for the blood and lymph entering or exiting the mucosa.
Submucosa. It is composed of loose connective tissue containing numerous blood and lymphatic vessels, cells of the MALT, and submucosal (Meissner’s) nerve plexus. The submucosa is an important passageway for the blood and lymph entering or exiting the mucosa.
 Muscle layer (muscularis propria). The muscle layer of the esophagus and small and large intestines consists of an internal circular sublayer and an external layer containing smooth muscle cells arranged longitudinally. The stomach has an additional oblique middle layer of smooth muscles. The myenteric (Auerbach’s) nerve plexus is located between the muscle sublayers of the intestines.
Muscle layer (muscularis propria). The muscle layer of the esophagus and small and large intestines consists of an internal circular sublayer and an external layer containing smooth muscle cells arranged longitudinally. The stomach has an additional oblique middle layer of smooth muscles. The myenteric (Auerbach’s) nerve plexus is located between the muscle sublayers of the intestines.
 Serosa. The external surface of the stomach and the intestines is covered with a layer of mesothelium lying on loose connective tissue that separates it from the muscle layer. The esophagus does not have a serosa and is instead enveloped by a connective tissue adventitia. In the abdominal cavity the serosa allows smooth movement of the intestines as they glide over each other’s surface during peristalsis and contraction.
Serosa. The external surface of the stomach and the intestines is covered with a layer of mesothelium lying on loose connective tissue that separates it from the muscle layer. The esophagus does not have a serosa and is instead enveloped by a connective tissue adventitia. In the abdominal cavity the serosa allows smooth movement of the intestines as they glide over each other’s surface during peristalsis and contraction.
The gastrointestinal tract is subdivided into several functional units by smooth muscular sphincters that regulate the passage of contents from one part of the tract to another.
 Upper esophageal sphincter. It is located at the upper end of the esophagus and is composed of striated muscle. Its tone is maintained by impulses from vagal postganglionic neurons. This sphincter participates in the swallowing reflex and prevents the reflux of swallowed food from the esophagus into the pharynx.
Upper esophageal sphincter. It is located at the upper end of the esophagus and is composed of striated muscle. Its tone is maintained by impulses from vagal postganglionic neurons. This sphincter participates in the swallowing reflex and prevents the reflux of swallowed food from the esophagus into the pharynx.
 Lower esophageal sphincter. Located at the esophagogastric junction, its relaxation during peristalsis allows the passage of food from the esophagus into the stomach. It also prevents gastroesophageal reflux. It is under the control of intrinsic nervous plexus, which is influenced by the vagus nerve.
Lower esophageal sphincter. Located at the esophagogastric junction, its relaxation during peristalsis allows the passage of food from the esophagus into the stomach. It also prevents gastroesophageal reflux. It is under the control of intrinsic nervous plexus, which is influenced by the vagus nerve.
 Pyloric sphincter. This sphincter is located at the end of the pylorus. It represents the thickened middle layer of the gastric muscularis propria. Opening of this sphincter allows the passage of chyme from the stomach into the duodenum.
Pyloric sphincter. This sphincter is located at the end of the pylorus. It represents the thickened middle layer of the gastric muscularis propria. Opening of this sphincter allows the passage of chyme from the stomach into the duodenum.
 Ileocecal sphincter (valve). The small intestine does not have any sphincters, and the first sphincter the chyme encounters after leaving the stomach is the ileocecal valve. It regulates the passage of chyme from the small into the large intestine. It opens on distention of the terminal ileum by chyme and closes on dilatation of the cecum.
Ileocecal sphincter (valve). The small intestine does not have any sphincters, and the first sphincter the chyme encounters after leaving the stomach is the ileocecal valve. It regulates the passage of chyme from the small into the large intestine. It opens on distention of the terminal ileum by chyme and closes on dilatation of the cecum.
 The internal and external anal sphincters. These sphincters prevent involuntary passage of feces but relax during defecation, allowing the passage of stools. The external sphincter, which is composed of skeletal muscle, can be contracted or relaxed at will. If the sphincter is relaxed, defecation occurs. The internal sphincter is involved in the defecation reflex, regulating the entry of feces into the anal canal.
The internal and external anal sphincters. These sphincters prevent involuntary passage of feces but relax during defecation, allowing the passage of stools. The external sphincter, which is composed of skeletal muscle, can be contracted or relaxed at will. If the sphincter is relaxed, defecation occurs. The internal sphincter is involved in the defecation reflex, regulating the entry of feces into the anal canal.
The mucosal lining of the stomach and the intestines contains several highly specialized cells arranged in an anatomic site-specific manner.
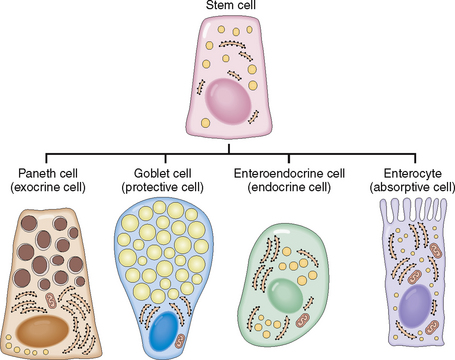
The mouth and esophagus on one end and the anus on the other end of the GI tract are lined by squamous epithelium. All other parts of the GI tract are lined by mucosa that contains, with some minor site-specific modifications, five cell types: (1) protective cells, (2) absorptive cells, (3) exocrine secretory cells, (4) endocrine secretory cells, and (5) stem cells considered to be the precursors of all the other more differentiated cells. Obviously some cells have more than one function and could belong to more than one of these categories. These five cells types seen in the small intestine are shown diagrammatically in Figure 7-4.
The main features of the epithelial cells lining the GI tract are as follows:
 Protective cells. The mouth and the esophagus are lined by squamous epithelium, the primary function of which is the protection of the body from the adverse effects of ingested material. In the stomach and the intestine the main epithelial protective cells are the mucus-secreting cells. One should not forget that the GI system contains immune cells, lymphocytes, and plasma cells, forming the so-called mucosa-associated lymphoid tissue (MALT). These nonepithelial cells interact with the epithelial cells and contribute to their protective function.
Protective cells. The mouth and the esophagus are lined by squamous epithelium, the primary function of which is the protection of the body from the adverse effects of ingested material. In the stomach and the intestine the main epithelial protective cells are the mucus-secreting cells. One should not forget that the GI system contains immune cells, lymphocytes, and plasma cells, forming the so-called mucosa-associated lymphoid tissue (MALT). These nonepithelial cells interact with the epithelial cells and contribute to their protective function.
 Absorptive cells. Since most of the absorption occurs in the small intestine, it is obvious that surface absorptive cells (enterocytes) predominate in this part of the GI tract. Surface absorptive cells are on their luminal surface lined by microvilli, which increase the absorptive surface of the cell membrane. The glycocalyx covering the microvilli is rich in digestive enzymes such as disaccharidases and dipeptidases that facilitate the absorption of carbohydrates. The large intestine contains absorptive cells whose main function is the passive reabsorption of water, which follows the active transport of sodium from the lumen.
Absorptive cells. Since most of the absorption occurs in the small intestine, it is obvious that surface absorptive cells (enterocytes) predominate in this part of the GI tract. Surface absorptive cells are on their luminal surface lined by microvilli, which increase the absorptive surface of the cell membrane. The glycocalyx covering the microvilli is rich in digestive enzymes such as disaccharidases and dipeptidases that facilitate the absorption of carbohydrates. The large intestine contains absorptive cells whose main function is the passive reabsorption of water, which follows the active transport of sodium from the lumen.
 Exocrine cells. These cells are found in all parts of the GI system below the esophagus.
Exocrine cells. These cells are found in all parts of the GI system below the esophagus.
 In the stomach the primary exocrine secretory cells are the parietal cells and the chief cells. The parietal cells secrete hydrochloric acid, the main component of the gastric digestive juice, and intrinsic factor, which is essential for the absorption of the vitamin B12 in the ileum. The chief cells, found only in the fundic glands of the gastric body, secrete pepsin, lipase, and several other enzymes important for the initial digestion of food. The neck of the gastric glands contains mucus-secreting cells, which secrete glycoproteins and glycosaminoglycans that coat the surface. This mucus is part of the gastric mucosal barrier that protects the gastric mucosa from autodigestion by hydrochloric acid and peptic enzymes secreted by other gastric cells.
In the stomach the primary exocrine secretory cells are the parietal cells and the chief cells. The parietal cells secrete hydrochloric acid, the main component of the gastric digestive juice, and intrinsic factor, which is essential for the absorption of the vitamin B12 in the ileum. The chief cells, found only in the fundic glands of the gastric body, secrete pepsin, lipase, and several other enzymes important for the initial digestion of food. The neck of the gastric glands contains mucus-secreting cells, which secrete glycoproteins and glycosaminoglycans that coat the surface. This mucus is part of the gastric mucosal barrier that protects the gastric mucosa from autodigestion by hydrochloric acid and peptic enzymes secreted by other gastric cells. In the small intestine the secretory cells include cells that are devoted to secretion only, such as the Paneth cells and the mucus-secreting goblet cells, and enterocytes (surface absorptive cells), which have other functions as well. The function of Paneth cells has not been elucidated completely. The mucus produced by mucous cells has a protective and lubricating function. The mucus also contains bactericidal substances including immunoglobulin A produced by the plasma cells residing in the intestinal mucosa. In contrast to the enterocytes lining the surface villi that are involved in absorption, the enterocytes in the intestinal crypts participate in exocytosis of fluids and minerals. These cells contribute about 3 L of fluid per day to the intestinal contents. Exocytosis includes several mechanisms, most notably: active transport, diffusion, and facilitated diffusion.
In the small intestine the secretory cells include cells that are devoted to secretion only, such as the Paneth cells and the mucus-secreting goblet cells, and enterocytes (surface absorptive cells), which have other functions as well. The function of Paneth cells has not been elucidated completely. The mucus produced by mucous cells has a protective and lubricating function. The mucus also contains bactericidal substances including immunoglobulin A produced by the plasma cells residing in the intestinal mucosa. In contrast to the enterocytes lining the surface villi that are involved in absorption, the enterocytes in the intestinal crypts participate in exocytosis of fluids and minerals. These cells contribute about 3 L of fluid per day to the intestinal contents. Exocytosis includes several mechanisms, most notably: active transport, diffusion, and facilitated diffusion. The large intestine contains numerous goblet cells whose main function is to produce mucus. This mucus protects the surface of the intestines and serves as a lubricant facilitating the passage of solidified feces.
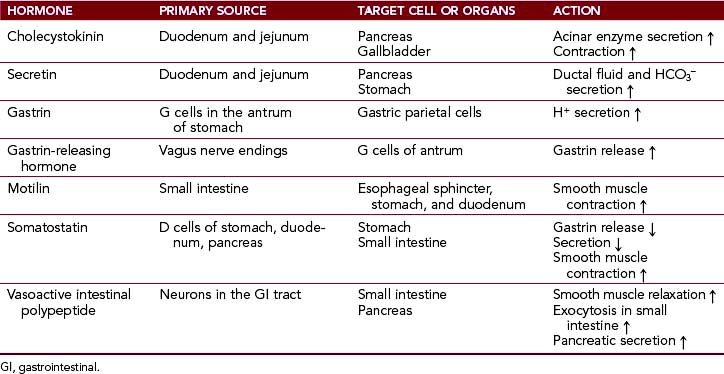
The large intestine contains numerous goblet cells whose main function is to produce mucus. This mucus protects the surface of the intestines and serves as a lubricant facilitating the passage of solidified feces. Endocrine cells. These cells are part of the diffuse enteroendocrine system and are scattered throughout the GI tract. Similar cells are found in the respiratory tract and in the islets of Langerhans. Enteroendocrine cells secrete biogenic amines, such as histamine and serotonin, and polypeptide hormones that can be classified as (1) true hormones, (2) paracrine hormones, and (3) neurocrine hormones (Table 7-1).
Endocrine cells. These cells are part of the diffuse enteroendocrine system and are scattered throughout the GI tract. Similar cells are found in the respiratory tract and in the islets of Langerhans. Enteroendocrine cells secrete biogenic amines, such as histamine and serotonin, and polypeptide hormones that can be classified as (1) true hormones, (2) paracrine hormones, and (3) neurocrine hormones (Table 7-1).
 True hormones are released into the circulation and act on distant target organs. For example, the duodenum secretes cholecystokinin (CKK) and secretin, which enter the blood and act on the receptors in the pancreas and the biliary system.
True hormones are released into the circulation and act on distant target organs. For example, the duodenum secretes cholecystokinin (CKK) and secretin, which enter the blood and act on the receptors in the pancreas and the biliary system. Paracrine hormones act on cells that are adjacent to the cells that produced them. For example, somatostatin is a hormone produced by many enteroendocrine cells, and it acts by inhibiting the functions of adjacent cells.
Paracrine hormones act on cells that are adjacent to the cells that produced them. For example, somatostatin is a hormone produced by many enteroendocrine cells, and it acts by inhibiting the functions of adjacent cells. Neurocrine hormones act on smooth muscle cells and exocrine cells by mimicking the action of sympathetic and parasympathetic nerves. For example, vasoactive intestinal polypeptide (VIP) stimulates intestinal exocytosis while relaxing circular intestinal smooth muscle cells. Enkephalins have the opposite effect. Most of the neurocrine hormones are actually synthesized by the nerve cells in the intestinal wall.
Neurocrine hormones act on smooth muscle cells and exocrine cells by mimicking the action of sympathetic and parasympathetic nerves. For example, vasoactive intestinal polypeptide (VIP) stimulates intestinal exocytosis while relaxing circular intestinal smooth muscle cells. Enkephalins have the opposite effect. Most of the neurocrine hormones are actually synthesized by the nerve cells in the intestinal wall.The innervation of the gastrointestinal tract comprises an intrinsic and an extrinsic component interacting with one another and the neuroendocrine cells.
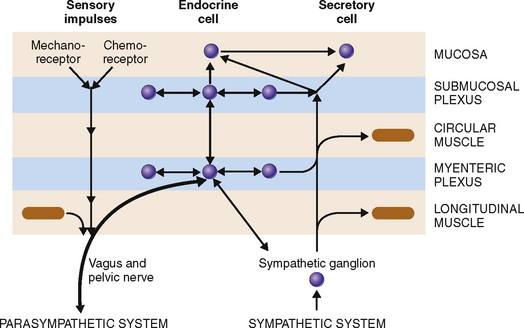
The sympathetic innervation stems from four ganglia: celiac, superior mesenteric, inferior mesenteric, and hypogastric. Adrenergic stimuli from these ganglia act on the nerve cells of the myenteric and submucosal plexus, or directly on the smooth muscle cells and endocrine and exocrine cells of the GI mucosa (Fig. 7-5).
PHYSIOLOGY
 Motility. The musculature of the GI tract consists predominantly of smooth muscle cells, and thus it is not surprising that most of its movements are involuntary. These movements are under the control of the autonomic nervous system and intramural nerve plexus and are often coordinated into reflexes controlled by the autonomic centers in the medulla and the pons.
Motility. The musculature of the GI tract consists predominantly of smooth muscle cells, and thus it is not surprising that most of its movements are involuntary. These movements are under the control of the autonomic nervous system and intramural nerve plexus and are often coordinated into reflexes controlled by the autonomic centers in the medulla and the pons.
 Secretion. Different parts of the GI tract have different functions, and so the secretions in the stomach differ from those of the small intestine. Keep in mind that the salivary glands, the liver, and the pancreas secrete copious amounts of digestive juices that are essential for normal digestion.
Secretion. Different parts of the GI tract have different functions, and so the secretions in the stomach differ from those of the small intestine. Keep in mind that the salivary glands, the liver, and the pancreas secrete copious amounts of digestive juices that are essential for normal digestion.
 Intestinal fluid and electrolyte transport. Huge amounts of fluids enter into the GI tract daily and are mostly reabsorbed, resulting in only 200 g of waste removed by defecation.
Intestinal fluid and electrolyte transport. Huge amounts of fluids enter into the GI tract daily and are mostly reabsorbed, resulting in only 200 g of waste removed by defecation.
 Digestion. Breakdown of foods into the basic nutrients is a prerequisite for their absorption.
Digestion. Breakdown of foods into the basic nutrients is a prerequisite for their absorption.
 Absorption. This is the final stage in the uptake of nutrients, but it is also essential for the intake of fluid, minerals, vitamins, drugs, and other exogenous substances.
Absorption. This is the final stage in the uptake of nutrients, but it is also essential for the intake of fluid, minerals, vitamins, drugs, and other exogenous substances.
 Defecation. The undigested nutrients and some waste products are eliminated from the body through the anus.
Defecation. The undigested nutrients and some waste products are eliminated from the body through the anus.
The initial processing of the food begins with chewing and swallowing.
 Ingestion. Intake of food occurs in most instances by voluntary opening of the mouth and biting of solid food or sucking of fluids.
Ingestion. Intake of food occurs in most instances by voluntary opening of the mouth and biting of solid food or sucking of fluids.
 Chewing (mastication). Breakdown of solid food into smaller morsels is accomplished by coordinated movements of the jaws, known as chewing. It is in part based on voluntary movements and in part on a chewing reflex coordinated from the centers in the brainstem. It involves a coordinated action of masticatory muscles such as the masseter, medial pterygoid, and temporalis muscle.
Chewing (mastication). Breakdown of solid food into smaller morsels is accomplished by coordinated movements of the jaws, known as chewing. It is in part based on voluntary movements and in part on a chewing reflex coordinated from the centers in the brainstem. It involves a coordinated action of masticatory muscles such as the masseter, medial pterygoid, and temporalis muscle.
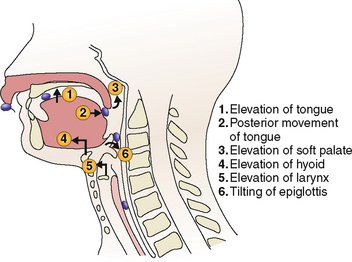
 Swallowing (deglutition). Food that has been reduced to smaller morsels is swallowed. Swallowing has three phases: an initial voluntary phase (oral phase), followed by two involuntary phases (pharyngeal and esophageal phases) (Fig. 7-6).
Swallowing (deglutition). Food that has been reduced to smaller morsels is swallowed. Swallowing has three phases: an initial voluntary phase (oral phase), followed by two involuntary phases (pharyngeal and esophageal phases) (Fig. 7-6).
 Pharyngeal phase. Once the bolus enters the oropharynx, it activates the swallowing center in the medulla and lower pons, which propels the food into the esophagus. At the same time the reflex leads to the closure of the glottis and vocal cords so that the food does not enter into the respiratory system.
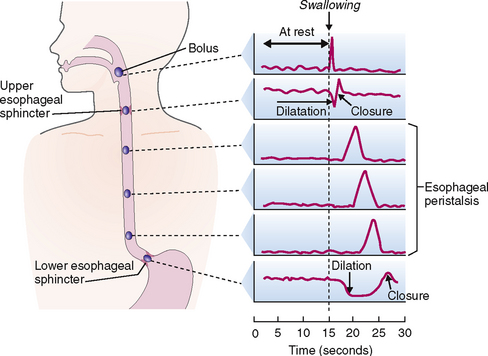
Pharyngeal phase. Once the bolus enters the oropharynx, it activates the swallowing center in the medulla and lower pons, which propels the food into the esophagus. At the same time the reflex leads to the closure of the glottis and vocal cords so that the food does not enter into the respiratory system. Esophageal phase. Once the bolus has entered into the esophagus it is propelled caudally by esophageal peristalsis. Two forms of peristalsis are recognized: primary and secondary. Primary peristalsis, which is initiated by swallowing, is under the control of the vagus nerve, emerging from the swallowing centers in the medulla. As soon as food enters the esophagus, the upper esophageal sphincter contracts, preventing the regurgitation of the food (Fig. 7-7). The peristaltic waves of primary peristalsis are slow, and when a person is eating in an erect position the food drops faster due to gravity than to peristaltic propulsion. It should be noticed that the vagus nerve controls both the striated muscle in the upper esophagus and the smooth muscle cells. Vagotomy abolishes the primary esophageal reflex. Secondary peristalsis, which is initiated by the entry of food into the esophagus, is mediated by intramural mechanical stretch receptors. It is coordinated by intramural nerves, and vagotomy does not abolish it. This type peristalsis leads to the opening of the lower esophageal sphincter, and it persists until the food is passed to the stomach. Once the food has passed into the stomach the lower esophageal sphincter contracts, preventing reflux from the stomach.
Esophageal phase. Once the bolus has entered into the esophagus it is propelled caudally by esophageal peristalsis. Two forms of peristalsis are recognized: primary and secondary. Primary peristalsis, which is initiated by swallowing, is under the control of the vagus nerve, emerging from the swallowing centers in the medulla. As soon as food enters the esophagus, the upper esophageal sphincter contracts, preventing the regurgitation of the food (Fig. 7-7). The peristaltic waves of primary peristalsis are slow, and when a person is eating in an erect position the food drops faster due to gravity than to peristaltic propulsion. It should be noticed that the vagus nerve controls both the striated muscle in the upper esophagus and the smooth muscle cells. Vagotomy abolishes the primary esophageal reflex. Secondary peristalsis, which is initiated by the entry of food into the esophagus, is mediated by intramural mechanical stretch receptors. It is coordinated by intramural nerves, and vagotomy does not abolish it. This type peristalsis leads to the opening of the lower esophageal sphincter, and it persists until the food is passed to the stomach. Once the food has passed into the stomach the lower esophageal sphincter contracts, preventing reflux from the stomach.In the stomach the food is transformed into chyme, which is passed into the duodenum.
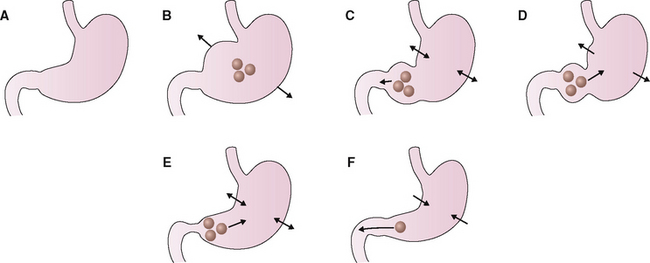
 Filling. The swallowing of food initiates a vasovagal reflex that leads to the relaxation of the lower esophageal reflex in the proximal part of the stomach. This process is called receptive relaxation. The entry of food into the stomach evokes active dilatation of the fundus, known as gastric accommodation. This dilatation is believed to be mediated by intrinsic gastric innervation and is modulated by the vagus nerve (Fig. 7-8).
Filling. The swallowing of food initiates a vasovagal reflex that leads to the relaxation of the lower esophageal reflex in the proximal part of the stomach. This process is called receptive relaxation. The entry of food into the stomach evokes active dilatation of the fundus, known as gastric accommodation. This dilatation is believed to be mediated by intrinsic gastric innervation and is modulated by the vagus nerve (Fig. 7-8).
 Mixing. The gastric contractions needed for the mixing of food are initiated by a pacemaker that is located on the greater curvature and composed of interstitial cells of Cajal. Under the influence of hydrochloric acid the food is broken down into small morsels and transformed into a coarse mixture. This mush is propelled into the antrum, where it is churned. The food hitting the closed pyloric sphincter initiates a contraction of the antrum, which returns the food into the proximal stomach. This propulsion, grinding, and retropulsion are repeated several times, mincing the food into smaller and smaller particles until it is transformed into a semifluid material called chyme. Expulsion of food leads to gastric emptying, as follows.
Mixing. The gastric contractions needed for the mixing of food are initiated by a pacemaker that is located on the greater curvature and composed of interstitial cells of Cajal. Under the influence of hydrochloric acid the food is broken down into small morsels and transformed into a coarse mixture. This mush is propelled into the antrum, where it is churned. The food hitting the closed pyloric sphincter initiates a contraction of the antrum, which returns the food into the proximal stomach. This propulsion, grinding, and retropulsion are repeated several times, mincing the food into smaller and smaller particles until it is transformed into a semifluid material called chyme. Expulsion of food leads to gastric emptying, as follows.
 Gastric emptying. During food mixing the pyloric sphincter is closed as tightly as possible. Nevertheless small amounts of chyme escape into the duodenum. The entry of acid chyme, and especially if it contains lipids and proteins, evokes an enterogastric reflex, which slows down gastric emptying. The purpose of this reflex is to prevent premature emptying of the stomach and overly rapid filling of the duodenum. Nevertheless, as the mixing progresses, more and more food accumulates in the pyloric antrum, causing its gradual dilatation. The relaxation of the pyloric sphincter permits the outflow of food into the duodenum. It should be noticed that gastric emptying is also under hormonal control. Gastrin enhances the contraction of the pyloric sphincter, thereby diminishing gastric emptying. Cholecystokinin and secretin released from the duodenum filling with acid chyme also reduce the rate of gastric emptying.
Gastric emptying. During food mixing the pyloric sphincter is closed as tightly as possible. Nevertheless small amounts of chyme escape into the duodenum. The entry of acid chyme, and especially if it contains lipids and proteins, evokes an enterogastric reflex, which slows down gastric emptying. The purpose of this reflex is to prevent premature emptying of the stomach and overly rapid filling of the duodenum. Nevertheless, as the mixing progresses, more and more food accumulates in the pyloric antrum, causing its gradual dilatation. The relaxation of the pyloric sphincter permits the outflow of food into the duodenum. It should be noticed that gastric emptying is also under hormonal control. Gastrin enhances the contraction of the pyloric sphincter, thereby diminishing gastric emptying. Cholecystokinin and secretin released from the duodenum filling with acid chyme also reduce the rate of gastric emptying.
The processing of food in the stomach is accomplished primarily through the action of hydrochloric acid.
Proteins are not the only food component broken down in the stomach. Gastric lipase breaks down short-chain fatty acids, but in principle most lipids are not digested in the stomach. Carbohydrates continue to be digested by the salivary amylase, which is, however, soon inactivated by acid. Thus, most of the components of a food bolus are only partially digested in the stomach, and very little of these are absorbed. Most absorption involves water-soluble small molecules, which pass freely with the water into the blood.
Secretion of gastric juices is under neural and hormonal control.
Secretion of gastric juices occurs in three phases as follows:
 Cephalic phase. It accounts for approximately 30% of the total gastric secretory response. The cephalic phase involves a central nervous system (CNS) reflex that can be initiated by thinking about food, or by seeing, smelling, or tasting it. The stimuli are transmitted through the vagus nerve. Acetylcholine (ACh) released from the nerve endings of the vagus nerve acts directly on parietal cells to secrete HCl (Fig. 7-9). Acetylcholine released from the vagus nerve also stimulates the enteroendocrine cells, indirectly evoking both stimulatory and, to a lesser degree, inhibitory stimuli. These indirect effects on parietal cells include the action of ACh on the following cells:
Cephalic phase. It accounts for approximately 30% of the total gastric secretory response. The cephalic phase involves a central nervous system (CNS) reflex that can be initiated by thinking about food, or by seeing, smelling, or tasting it. The stimuli are transmitted through the vagus nerve. Acetylcholine (ACh) released from the nerve endings of the vagus nerve acts directly on parietal cells to secrete HCl (Fig. 7-9). Acetylcholine released from the vagus nerve also stimulates the enteroendocrine cells, indirectly evoking both stimulatory and, to a lesser degree, inhibitory stimuli. These indirect effects on parietal cells include the action of ACh on the following cells:
 Enterochromaffin-like cells (ELCs). These cells are stimulated by ACh to release histamine. Histamine is the strongest secretagogue and acts by binding to histamine-2 (H2) receptors on the surface of parietal cells.
Enterochromaffin-like cells (ELCs). These cells are stimulated by ACh to release histamine. Histamine is the strongest secretagogue and acts by binding to histamine-2 (H2) receptors on the surface of parietal cells. G cells. Acetylcholine also stimulates the release of gastrin from G cells. Gastrin binds to specific receptors on parietal cells, stimulating them to produce HCl. Gastrin also acts on ECLs, stimulating them to release histamine. Chronic stimulation of ECLs with gastrin (e.g., in Zollinger-Elllison syndrome) may even cause ECL hyperplasia.
G cells. Acetylcholine also stimulates the release of gastrin from G cells. Gastrin binds to specific receptors on parietal cells, stimulating them to produce HCl. Gastrin also acts on ECLs, stimulating them to release histamine. Chronic stimulation of ECLs with gastrin (e.g., in Zollinger-Elllison syndrome) may even cause ECL hyperplasia. D cells. Acetylcholine acts on D cells, which secrete somatostatin. Somatostatin acts on parietal cells, thus inhibiting HCl production. It also inhibits the release of gastrin from G cells.
D cells. Acetylcholine acts on D cells, which secrete somatostatin. Somatostatin acts on parietal cells, thus inhibiting HCl production. It also inhibits the release of gastrin from G cells. Gastric phase. It is initiated by the mechanical stimuli created by the bolus of food as it enters the stomach. This phase accounts for most of the gastric secretory activity. The distention of the stomach provokes vasovagal reflexes, resulting in the release of ACh like in the cephalic phase. Acid pH stimulates the release of pepsin from the chief cells. Pepsin cleaves proteins to amino acids, some of which, notably tryptophan and phenylalanine, stimulate enteroendocrine G cells to release gastrin; this further promotes HCl production. When the acidity of gastric contents drops below pH 3 the secretion of gastrin stops. The acidity of the contents also has an inhibitory effect on the parietal cells, and when it drops below pH 2, HCl secretion stops entirely.
Gastric phase. It is initiated by the mechanical stimuli created by the bolus of food as it enters the stomach. This phase accounts for most of the gastric secretory activity. The distention of the stomach provokes vasovagal reflexes, resulting in the release of ACh like in the cephalic phase. Acid pH stimulates the release of pepsin from the chief cells. Pepsin cleaves proteins to amino acids, some of which, notably tryptophan and phenylalanine, stimulate enteroendocrine G cells to release gastrin; this further promotes HCl production. When the acidity of gastric contents drops below pH 3 the secretion of gastrin stops. The acidity of the contents also has an inhibitory effect on the parietal cells, and when it drops below pH 2, HCl secretion stops entirely.
 Intestinal phase. This phase begins with the chyme reaching the duodenum. It accounts for only 10% of the gastric output. Initially, as long as the acidity of chyme entering the duodenum is above pH 3, the intestinal phase is characterized by prevailing stimulation of the gastric secretion. Later on, as the acidity of the chyme entering the duodenum drops below pH 3, the inhibitory effects predominate. These inhibitory stimuli include the vasovagal reflex, stimulating somatostatin release in the stomach, and inhibitory hormones, such as secretin, CKK, somatostatin, and gastric inhibitory polypeptide (GIP) released from the duodenum. Collectively these hormones inhibit gastric acid secretion and slow down gastric emptying. Secretin is considered to be the main inhibitor of HCl production: it acts directly on parietal cells, inhibits gastrin release, and stimulates the production of somatostatin in the duodenum and the stomach. Somatostatin released from gastric D cells is the most potent paracrine inhibitor of parietal cells. Distention of the ileum by chyme leads to the release of peptide YY, which slows down gastric emptying.
Intestinal phase. This phase begins with the chyme reaching the duodenum. It accounts for only 10% of the gastric output. Initially, as long as the acidity of chyme entering the duodenum is above pH 3, the intestinal phase is characterized by prevailing stimulation of the gastric secretion. Later on, as the acidity of the chyme entering the duodenum drops below pH 3, the inhibitory effects predominate. These inhibitory stimuli include the vasovagal reflex, stimulating somatostatin release in the stomach, and inhibitory hormones, such as secretin, CKK, somatostatin, and gastric inhibitory polypeptide (GIP) released from the duodenum. Collectively these hormones inhibit gastric acid secretion and slow down gastric emptying. Secretin is considered to be the main inhibitor of HCl production: it acts directly on parietal cells, inhibits gastrin release, and stimulates the production of somatostatin in the duodenum and the stomach. Somatostatin released from gastric D cells is the most potent paracrine inhibitor of parietal cells. Distention of the ileum by chyme leads to the release of peptide YY, which slows down gastric emptying.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree