Surgical Treatment of Varicose Veins
William A. Marston
Overview
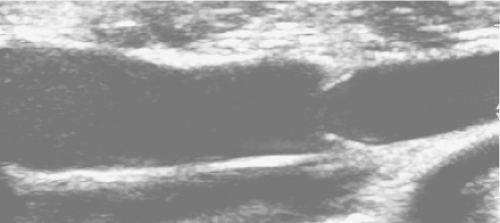
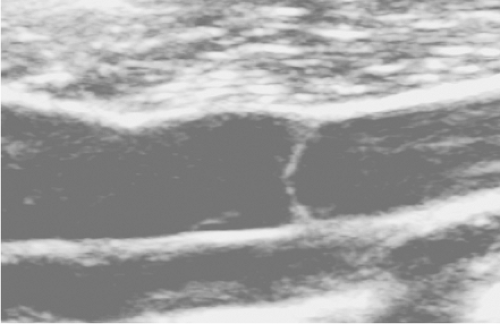
The venous drainage system of the lower extremity consists of three sets of veins: the deep veins, the superficial veins, and the perforating veins. All veins contain delicate one-way valves that normally open to allow blood to flow unimpeded toward the heart (Fig. 1) and prevent blood from flowing in a retrograde fashion after the valves close (Fig. 2). If the valves are damaged, they become incompetent and permit the reversal of venous blood flow into the dependent limb, which results in a pressure increase and distention of the affected vessel. With an increased venous pressure, often called venous hypertension, in the greater and/or lesser saphenous veins, smaller veins under the skin may also dilate and present as varicosities. Venous valve destruction can also occur in the deep and perforating veins, but this results in a different and more serious symptom complex, which is beyond the scope of this chapter.
Successful treatment of patients with symptomatic chronic venous insufficiency (CVI) requires a detailed analysis of the anatomic and physiologic correlates of venous dysfunction. Using this information the physician may determine whether correction of the source of CVI is possible and if so which procedures may be useful to do so. With the proliferation of minimally invasive procedures in the last decade, conventional surgical correction of venous insufficiency is performed less frequently. However, these procedures remain useful in some instances as the primary procedure of choice. Regardless of whether a surgical, endovenous, injection-based, or other procedure is performed, the goal is the same: correction of abnormal venous reflux or obstruction resulting in CVI. Patients with CVI require treatment for limb swelling, skin changes, and ulceration, as well as the pain and disability associated with these objective signs. Although cosmetic considerations should not be ignored, the primary concern in CEAP classes 3 to 6 is to effectively obliterate abnormal reflux and minimize recurrence for long-term symptom resolution.
Demographics
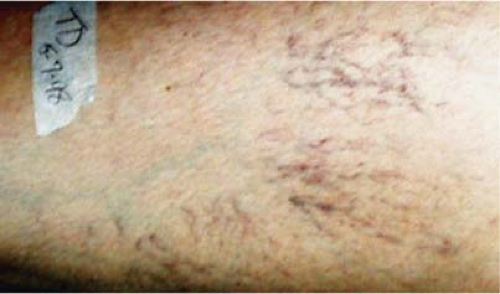
Various reports cite the incidence of varicose veins in the general population as ranging from 7% to 25%. The variability in these reports is attributable to whether spider veins (Fig. 3) are included in the definition for varicosities. Spider veins are estimated to occur in approximately 25% of the population (15% in males and 25% in females), and are manifested by dilated red streaks under the skin, often associated with a deeper blue reticular vein in that region. This condition is generally considered cosmetic, and sclerotherapy treatment is often curative.
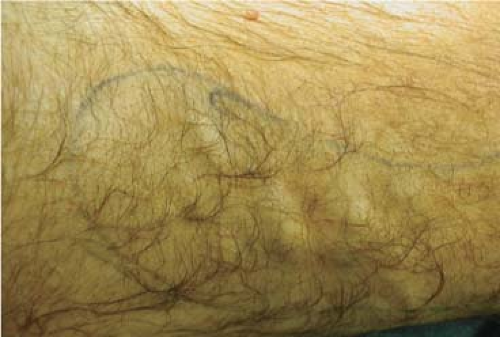
Larger varicosities, as shown in Figure 4, are more often associated with insufficiency of the greater or lesser saphenous vein and present as subcutaneous bulges in the thigh or calf region. Symptoms of mild pain, heaviness, or even swelling after prolonged standing are often associated with this condition and there are multiple treatment options available for this condition.
Classification of Venous Disease
Because of the broad spectrum of venous disease of the superficial veins of the lower extremity, an objective classification has been developed so that clinicians are better able to categorize the severity of the illness and more effectively evaluate the results of various treatment options. The most commonly used is the CEAP classification, which includes clinical, etiologic, anatomic, and pathologic signs. The clinical portion of the schemata is the most important to the practicing physician and is described in Table 1.
Diagnostic Testing for Patients with Cvi
The rational treatment of patients with CVI and its sequelae requires the use of noninvasive studies performed by experienced vascular technologists to identify dysfunction in the patient’s venous system. Information on both the anatomic sites of venous dysfunction and its hemodynamic importance are required to allow treatment plans to be formulated and optimal results to be achieved. Selecting surgical therapy without a knowledge of which vein segments are abnormal is essentially blind surgery and cannot result in optimal results.
Duplex Ultrasound
Imaging techniques using ultrasound combined with Doppler interrogation of the venous system have been validated as sensitive methods of diagnosis of deep venous thrombosis. Important information for patients with CVI that would be detected with this technique includes the presence or absence of venous obstruction or other changes typical of previous deep venous thrombosis. This information will help to determine whether the patient’s CVI is due to obstruction, reflux, or both (pathophysiology). The presence of outflow obstruction in the iliac veins and/or IVC can often be detected looking at flow patterns, phasicity, and respiratory variation in the common femoral vein. In addition to an examination of the deep and superficial systems, the perforator veins are carefully examined for evidence of incompetence.
Secondly, venous reflux in the deep and superficial venous systems is evaluated with the patient in the standing position using duplex ultrasound and either manual compression or a rapid inflation/deflation system to elicit reflux. Systematic interrogation of the common femoral, superficial femoral, popliteal, greater saphenous vein (GSV), and small saphenous veins (SSV) is conducted,
allowing an anatomic map of venous reflux in the limb to be constructed.
allowing an anatomic map of venous reflux in the limb to be constructed.
Using this information, the clinician can determine the etiology, anatomy, and pathophysiology of CVI for the patient. For example, the patient that has superficial and perforator disease may be differentiated from the patient with superficial and deep reflux, allowing alternate treatment plans to be selected. Although duplex evaluation provides detailed information on the anatomy of venous disease, it cannot define the importance of anatomic abnormalities in the venous function of the limb.
Table 1 CEAP Classification of Venous Diseasea | ||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| ||||||||||||||||||
Air Plethysmography
There are a number of tests available to better document the severity of valvular dysfunction. One of the most widely used is air plethysmography (APG). Plethysmography is defined as the determination of changes in volume, and various techniques of plethysmography have been evaluated in the noninvasive examination of the venous system. In general, these techniques exploit the finding that the venous system refills more rapidly in patients with poor valvular function than in patients with normal valvular function. The major parameters that may be measured with this examination are given in Table 2.
The venous-filling index (VFI) is arguably the most significant parameter that can be measured with APG. In 1988, Christopoulos et al. described the use of APG for evaluation of normal limbs and those affected with CVI. A VFI <2 mL/s was associated with clinically normal limbs, and increasing levels of VFI were associated with more severe symptoms. The VFI is believed to provide a reasonable approximation of the global function of the lower extremity venous system in
resisting reflux in the standing position. It has also been reported to be useful in predicting long-term symptom relief in patients undergoing corrective venous surgery.
resisting reflux in the standing position. It has also been reported to be useful in predicting long-term symptom relief in patients undergoing corrective venous surgery.
Table 2 Definition of Results of Air Plethysmography Testing | ||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
|
Indications for Intervention
The indications for intervention in patients with CVI are variable and depend on the severity of symptoms, options for correction, and the functional and medical status of the patient. Patients in CEAP clinical classes 3 and 4 suffering symptoms of swelling and skin changes may be managed with compression stockings and skin lubricants with general improvement. However, compliance with compression stocking use is generally believed to be poor in the long term. Patients who are candidates for a corrective procedure typically choose intervention, particularly younger, more active patients. In clinical classes 5 and 6, the primary indication for intervention is to reduce the risk of recurrent ulceration. Patients with active ulcers can expect ulcer healing in 10 to 12 weeks on average using various high compression bandaging systems. Unfortunately, larger ulcers and those of long duration heal more slowly in most cases. It is not clear whether intervention with correction of CVI will accelerate healing in these cases, but it is reasonable to perform corrective procedures if possible prior to ulcer healing.
Anatomically, any combination of superficial, perforator, and/or deep venous disease may result in severe CVI. Marston et al. reported that 29% of limbs with CVI and leg ulceration displayed superficial or superficial and perforator disease on standing reflux examination (Table 2). Small saphenous reflux may also be sufficient to cause leg ulceration with no other abnormalities, typically resulting in ulceration near the lateral malleolus. The contribution of incompetent perforators to global venous insufficiency remains controversial and will be discussed in detail below, but it is clear that some leg ulcers are associated with large incompetent perforators that should be ligated.
A significant percentage of patients with severe CVI are found to have abnormal venous function in multiple systems. Over 27% displayed both deep and superficial reflux in a study of 138 limbs with leg ulceration. It is not always clear whether these patients will experience an improvement in the severity of symptoms if the superficial or superficial and perforator abnormalities are corrected. This issue will be discussed in detail below.
Conventional Surgical Procedures for Correction of Cvi
Superficial Venous Reflux—Great Saphenous Vein
Traditional surgical techniques for removal of the great saphenous vein have typically employed ligation of the vein at the saphenofemoral junction (SFJ) and removal of the vein between the groin and knee or groin and ankle using a stripping technique. The goal of high ligation is to identify and divide all venous branches communicating with the SFJ to minimize the potential for recurrent reflux pathways resulting in recurrent symptoms. Unfortunately, it appears that many patients developing recurrent venous insufficiency do so because of neovascular generation of new venous communications reestablishing the SFJ, or dilation of preexisting venous tributaries. At this point it is theorized that the surgical procedure itself is the primary stimulus for neovascularization and there is hope that endovenous techniques may prove to be associated with a lower incidence of recurrent venous insufficiency after intervention.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree