Operative Management of Pancreatic Trauma
David V. Feliciano
Injuries to the pancreas are noted in ∼5% to 6% of the patients undergoing laparotomy after sustaining blunt abdominal trauma or gunshot wounds of the abdomen and in 2% to 6% of those with stab wounds of the abdomen.
The retroperitoneal pancreas crosses the upper abdomen at the level of the first and second lumbar vertebrae, and “post-traumatic pancreatitis” occasionally results from a spinal fracture at this level. The gland has a thin mesothelial capsule and is 15 to 20 cm in length, 1.0 to 1.5 cm in thickness, and ∼3.0 cm in width.
The proximity of the pancreas to all the major named vessels of the upper abdomen complicates operative management of injuries, especially in patients with penetrating trauma. The head of the pancreas has a shared blood supply with the duodenum through the anterior and posterior branches of the superior and inferior pancreaticoduodenal arteries. In addition, the head overlies the inferior vena cava, right renal vessels, and the left renal vein as it enters the cava. The uncinate process encompasses the inferior pancreaticoduodenal artery and wraps around the superior mesenteric vein and artery. The neck of the pancreas overlies the superior mesenteric vein and may have to be divided to expose injuries to the confluence of this vein and the splenic vein or to the proximal portal vein. The body of the pancreas lies over the visceral portion of the suprarenal aorta (origins of celiac axis, superior mesenteric artery, and bilateral renal arteries) and the left renal artery and vein. Finally, the body and tail of the pancreas encircle or are intimately adherent to the splenic artery or vein.
The duct of Wirsung (main pancreatic duct) passes through the entire length of the gland just above a line halfway between the superior and inferior edges and enters the left side of the common bile duct to form the ampulla of Vater. The duct of Santorini (accessory pancreatic duct) most commonly branches out superiorly from the duct of Wirsung in the neck of the pancreas and enters the duodenum at the minor papilla ∼2.5 cm proximal to the major papilla.
Isolated injuries after blunt abdominal trauma are noted in only 20% of the patients with pancreatic injuries, and the most common associated injuries are to the duodenum, liver, and spleen. Associated injuries are almost always present in the patients undergoing laparotomy for penetrating wounds and depend on the location of the wound. Wounds of the head of the pancreas are most commonly associated with injuries to the liver, duodenum, and major vascular structures, whereas injuries to the body are frequently associated with perforations of the stomach and transverse colon. Wounds of the tail of the pancreas are associated with injuries to the splenic flexure of the colon, splenic vessels, and the spleen.
A direct blow with compression of the upper abdomen and its viscera/vessels against the spine is the most common blunt mechanism of injury. Examples would include compression from the lower rim of the steering wheel in an unrestrained driver in a deceleration-type motor vehicle crash, by a misplaced lap-type restraint device in a child, or by direct contact with the handlebars of a bicycle in a frontal crash. Many patients with blunt injuries to the pancreas have minimal clinical symptoms and signs when first evaluated after trauma. The major reason for this is the retroperitoneal location of the organ, which precludes the early development of peritonitis. The second reason is the tamponading effect of the retroperitoneum which may prevent significant blood loss or extravasation of pancreatic juice from the injury in the absence of other vascular injuries. Therefore, the surgeon may not be able to rely on the traditional serial physical examinations, diagnostic peritoneal lavage, or surgeon-performed ultrasound to make an early diagnosis of a blunt injury.
When symptoms are present, the most common is deep epigastric steady pain occasionally associated with nausea and vomiting. Pain in the upper lumbar area has not been a common complaint in the author’s experience unless a fracture of an adjacent vertebra is present. Because the epigastric pain is usually mild, it was not uncommon in the
pre-CT era for a patient with a major injury such as complete transection of the pancreas over the spine to be discharged from the emergency room with a missed diagnosis.
pre-CT era for a patient with a major injury such as complete transection of the pancreas over the spine to be discharged from the emergency room with a missed diagnosis.
Patients with penetrating wounds to the abdomen that injure the pancreas almost always have associated intra-abdominal injuries as noted earlier and present with the classic indications for an emergency laparotomy, namely, peritonitis, hypotension, and, rarely, evisceration.
With the difficulty in making a diagnosis of a blunt pancreatic injury as described earlier, there is reliance on laboratory testing and the use of contrast-enhanced CT in the modern era. Unfortunately, the laboratory finding of hyperamylasemia on admission to the emergency center is not a precise marker for an injury to the pancreas. Salivary rather than pancreatic amylase elevations are present in 30% to 40% of patients admitted with trauma secondary to acute alcoholic intoxication. Also, approximately one-third of patients with blunt transection of the pancreatic duct have a normal amylase level on admission. Therefore, the presence of hyperamylasemia, while raising suspicion of a pancreatic, duodenal, or enteric injury, does not mandate an exploratory laparotomy in the absence of the aforementioned hypotension, peritonitis, or evisceration. A progressive rise in the amylase level over the first 24 to 48 hours of hospitalization is, however, strongly suggestive of injury to the pancreas or duodenum or for the development of the rare entity of posttraumatic pancreatitis.
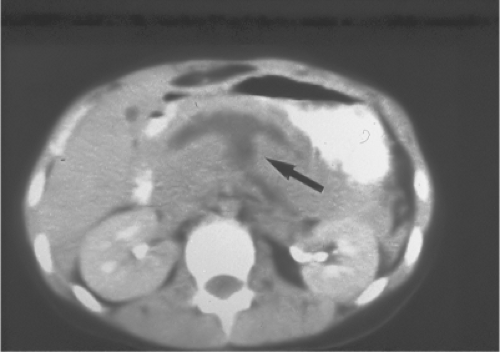
Contrast-enhanced CT using a 64-slice scanner is the current diagnostic modality of choice in hemodynamically stable and asymptomatic or minimally symptomatic patients with possible or suspected injuries to the pancreas. This would include patients who have sustained blunt abdominal trauma or those who have sustained a penetrating injury to the flank or back. In the latter groups, triple-contrast (intravenous, oral or by nasogastric tube, and rectal) CT has been performed for nearly 25 years. CT findings suggestive of injury to the pancreas include the following: hematoma of transverse mesocolon; thickening of the left anterior renal fascia; fluid in the lesser sac or between the pancreas and splenic vein; duodenal hematoma or laceration; injury to the left kidney, adrenal gland, or spleen; and Chance (transverse) fracture in the lumbar spine. CT findings diagnostic of injury to the pancreas include the following: parenchymal hematoma or laceration; obvious transection of the parenchyma with fluid in the lesser sac (Fig. 1); disruption of the head of the pancreas; and diffuse swelling characteristic of posttraumatic pancreatitis. Injuries to the pancreas noted on contrast-enhanced CT or at laparotomy are defined according to the Organ Injury Scale developed by the American Association for the Surgery of Trauma in 1990 (Moore EE et al. J Trauma 1990;30:1427–9). As with most other Organ Injury Scales, these range from Grade I (Minor pancreatic contusion or superficial laceration) to Grade V (massive disruption of the pancreatic head); see Table 1. Pitfalls in diagnosing pancreatic injuries on CT include the presence of minimal extraperitoneal fat in some patients, artifacts from dense oral contrast, and nonopacification of adjacent duodenum or small bowel so that the edges of the pancreas are difficult to define.
In the presence of an equivocal CT with or without associated hyperamylasemia or when CT is not available, endoscopic retrograde cholangiopancreatography (ERCP) is appropriate to rule out an injury to the main pancreatic duct. A separate classification system of pancreatic injuries diagnosed by ERCP is available as well (Takishima T, et al. J Trauma 2000;48:745–52).
Table 1 Pancreas Organ Injury Scale of the American Association for the Surgery of Trauma | |||||||||||||||||||||||||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| |||||||||||||||||||||||||||||||||||||||||||||
Nonoperative Management
In the absence of hypotension, peritonitis, evisceration, and CT scan evidence of
significant injuries to other organs or vessels, Grade I and II pancreatic injuries (do not involve duct) are managed nonoperatively. Though a rare Grade II injury (“major contusion/laceration”) may progress to a parenchymal pseudocyst, it is very uncommon to have to intervene for a peripancreatic fluid collection during the period of observation with this low magnitude of injury. A follow-up abdominal CT scan at 5 to 7 days after injury is appropriate when a significant Grade II injury is present, or earlier whenever new symptoms in the upper abdomen or increasing hyperamylasemia develop.
significant injuries to other organs or vessels, Grade I and II pancreatic injuries (do not involve duct) are managed nonoperatively. Though a rare Grade II injury (“major contusion/laceration”) may progress to a parenchymal pseudocyst, it is very uncommon to have to intervene for a peripancreatic fluid collection during the period of observation with this low magnitude of injury. A follow-up abdominal CT scan at 5 to 7 days after injury is appropriate when a significant Grade II injury is present, or earlier whenever new symptoms in the upper abdomen or increasing hyperamylasemia develop.
In all patients who are to undergo an emergency or urgent laparotomy after sustaining abdominal trauma, preparations are similar. An identification bracelet is placed on the patient, venous blood is withdrawn for routine laboratory tests and for type-and-crossmatch of blood products, and an intravenous line is initiated at the same site.
Rapid evaluation of the patient’s pericardial sac (rule out tamponade after either blunt or penetrating truncal trauma), pleural cavities, and, if necessary, abdominal cavity is attained by a surgeon-performed ultrasound using a 3.5-MHz probe.
A second- or third-generation cephalosporin antibiotic is administered intravenously. A nasogastric tube and a bladder catheter are inserted in either the emergency room or operating room depending on the patient’s hemodynamic state. In the patients who are in ATLS Class III or IV shock, a phone call is made to the blood bank to initiate a massive transfusion protocol. This protocol now commonly known as “damage control resuscitation” emphasizes the administration of blood and blood products (rather than overuse of crystalloids such as lactated Ringer’s solution) for the patients who are bleeding. While rarely attained, the desired goal of “damage control resuscitation” is to infuse packed red blood cells, fresh frozen plasma, and platelet packs in a 1: 1: 1 ratio. An example of such a protocol (after administration of the initiation package) is as follows.
| PRBC | FFP | Platelet | Cryo |
|---|---|---|---|
| 6u | 6 (AB) | 1 aph. | — |
| 6u | 6 (TS) | — | 10 u pooled |
| 6u | 6 (TS) | 1 aph. | — |
| 6u | 6 (TS) | — | 10 u pooled |
As hypothermia occurs in patients in shock, those undergoing evaluation in poorly heated trauma rooms or CT-suites, or during subsequent prolonged trauma laparotomies, prophylaxis against this problem is initiated in the emergency center. Standard maneuvers would include wrapping the patient’s head and covering the trunk and lower extremities with a warming device and infusing all blood products and fluids through in-line warmers.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree