Stroke
KEY CONCEPTS
![]() Stroke can be either ischemic (87%) or hemorrhagic (13%) and the two types are treated differently.
Stroke can be either ischemic (87%) or hemorrhagic (13%) and the two types are treated differently.
![]() Transient ischemic attacks (TIAs) require urgent intervention to reduce the risk of stroke, which is known to be highest in the first few days after TIA.
Transient ischemic attacks (TIAs) require urgent intervention to reduce the risk of stroke, which is known to be highest in the first few days after TIA.
![]() Carotid endarterectomy should be performed in ischemic stroke patients with 70% to 99% stenosis of the ipsilateral carotid artery, provided that it is done in an experienced center.
Carotid endarterectomy should be performed in ischemic stroke patients with 70% to 99% stenosis of the ipsilateral carotid artery, provided that it is done in an experienced center.
![]() Carotid stenting is an option for stroke patients eligible for carotid endarterectomy, especially in patients less than 70 years of age.
Carotid stenting is an option for stroke patients eligible for carotid endarterectomy, especially in patients less than 70 years of age.
![]() Early reperfusion (<4.5 hours from onset) with tissue plasminogen activator (tPA) has been shown to reduce the ultimate disability due to ischemic stroke.
Early reperfusion (<4.5 hours from onset) with tissue plasminogen activator (tPA) has been shown to reduce the ultimate disability due to ischemic stroke.
![]() Antiplatelet therapy is the cornerstone of antithrombotic therapy for the secondary prevention of noncardioembolic ischemic stroke.
Antiplatelet therapy is the cornerstone of antithrombotic therapy for the secondary prevention of noncardioembolic ischemic stroke.
![]() Oral anticoagulation is recommended for the secondary prevention of cardioembolic stroke in moderate- to high-risk patients.
Oral anticoagulation is recommended for the secondary prevention of cardioembolic stroke in moderate- to high-risk patients.
![]() Blood pressure lowering is effective in both the primary and secondary prevention of both ischemic and hemorrhagic stroke regardless of blood pressure.
Blood pressure lowering is effective in both the primary and secondary prevention of both ischemic and hemorrhagic stroke regardless of blood pressure.
![]() Blood pressure lowering in the acute ischemic stroke period (first 7 days) may result in decreased cerebral blood flow and worsened symptoms.
Blood pressure lowering in the acute ischemic stroke period (first 7 days) may result in decreased cerebral blood flow and worsened symptoms.
![]() Statin therapy is recommended for all ischemic stroke patients, regardless of baseline cholesterol, to reduce stroke recurrence.
Statin therapy is recommended for all ischemic stroke patients, regardless of baseline cholesterol, to reduce stroke recurrence.
![]() Stroke is the leading cause of disability among adults and the fourth leading cause of death in the United States, behind cardiovascular disease, cancer, and chronic lower respiratory diseases.1 Despite a 30% reduction in stroke mortality between 1995 and 2005, stroke occurs in the United States at a rate of almost 800,000 per year and resulted in 133,750,000 deaths in 2008.1,2 Aggressive efforts to organize stroke care at the local and regional levels and increased utilization of evidence-based recommendations and national guidelines may have contributed to the improved outcomes.
Stroke is the leading cause of disability among adults and the fourth leading cause of death in the United States, behind cardiovascular disease, cancer, and chronic lower respiratory diseases.1 Despite a 30% reduction in stroke mortality between 1995 and 2005, stroke occurs in the United States at a rate of almost 800,000 per year and resulted in 133,750,000 deaths in 2008.1,2 Aggressive efforts to organize stroke care at the local and regional levels and increased utilization of evidence-based recommendations and national guidelines may have contributed to the improved outcomes.
EPIDEMIOLOGY
There are currently 6.5 million stroke survivors in the United States, and stroke is the leading cause of adult disability.2 Of those free of the diagnosis of stroke or transient ischemic attack (TIA), however, almost 20% of individuals over the age of 45 years reported at least one stroke symptom,3 suggesting rampant underdiagnosing. Owing in part to the need for expensive posthospitalization rehabilitation and nursing home care, the annual cost of stroke in the United States is estimated to be $69 billion.2 Current projections are that death caused by stroke will increase exponentially in the next 30 years owing to aging of the population and our inability to control risk factors.4
African Americans have stroke rates that are twice those of whites, and the difference is exaggerated at younger ages.2 In addition, geographic disparity in stroke incidence exists, such that many states in the southeastern United States have stroke mortality rates 40% higher than the national average.2
Etiology
![]() Stroke can be either ischemic or hemorrhagic (87% and 13%, respectively, of all strokes in the 2012 American Heart Association [AHA] report).2 Hemorrhagic strokes include subarachnoid hemorrhage (SAH), intracerebral hemorrhage (ICH), and subdural hematomas. SAH occurs when blood enters the subarachnoid space (where cerebrospinal fluid is housed) owing to trauma, rupture of an intracranial aneurysm, or rupture of an arteriovenous malformation (AVM). By contrast, ICH occurs when a blood vessel ruptures within the brain parenchyma itself, resulting in the formation of a hematoma. These types of hemorrhages very often are associated with uncontrolled high blood pressure and sometimes antithrombotic or thrombolytic therapy. Subdural hematomas refer to collections of blood below the dura (covering of the brain), and they are caused most often by trauma. Hemorrhagic stroke, although less common, is significantly more lethal than ischemic stroke, with 30-day case-fatality rates that are two to six times higher.5,6
Stroke can be either ischemic or hemorrhagic (87% and 13%, respectively, of all strokes in the 2012 American Heart Association [AHA] report).2 Hemorrhagic strokes include subarachnoid hemorrhage (SAH), intracerebral hemorrhage (ICH), and subdural hematomas. SAH occurs when blood enters the subarachnoid space (where cerebrospinal fluid is housed) owing to trauma, rupture of an intracranial aneurysm, or rupture of an arteriovenous malformation (AVM). By contrast, ICH occurs when a blood vessel ruptures within the brain parenchyma itself, resulting in the formation of a hematoma. These types of hemorrhages very often are associated with uncontrolled high blood pressure and sometimes antithrombotic or thrombolytic therapy. Subdural hematomas refer to collections of blood below the dura (covering of the brain), and they are caused most often by trauma. Hemorrhagic stroke, although less common, is significantly more lethal than ischemic stroke, with 30-day case-fatality rates that are two to six times higher.5,6
Ischemic strokes are caused either by local thrombus formation or by embolic phenomena, resulting in occlusion of a cerebral artery. Atherosclerosis, particularly of the cerebral vasculature, is a causative factor in most cases of ischemic stroke, although 30% are cryptogenic. Emboli can arise from either intracranial or extracranial arteries (including the aortic arch) or, as is the case in 20% of all ischemic strokes, the heart. Cardiogenic embolism is presumed to have occurred if the patient has concomitant atrial fibrillation, valvular heart disease, or any other condition of the heart that can lead to clot formation.7 Distinguishing between cardiogenic embolism and other causes of ischemic stroke is important in determining long-term pharmacotherapy in a given patient.
Risk Factors
Risk factors for stroke can be subdivided into nonmodifiable, modifiable, and potentially modifiable. In addition, risk factors can be either well documented or less well documented.8 The main risk factors of stroke are listed in Table 10-1. Recommendations for risk factor reduction aggressively target the modifiable, well-documented risk factors, even in individuals with nonmodifiable risk.8 The nonmodifiable risk factors are age, race, sex, low birth weight, and family history. An individual’s risk of having a stroke increases substantially as he or she ages, with a doubling of risk for each decade older than 55 years of age. African Americans, Asian-Pacific Islanders, and Hispanics experience higher death rates than their white counterparts.2 Men are at a higher risk of stroke than women when matched for age, but women who suffer from a stroke are more likely to die from it.2
TABLE 10-1 Risk Factors for Ischemic Stroke

The most common modifiable, well-documented risk factors for stroke include hypertension, cigarette smoking, diabetes, atrial fibrillation, and dyslipidemia. The treatment of hypertension, beginning in the mid-20th century, is thought to be primarily responsible for the drastic reduction in stroke death rates between 1950 and 1980 in the United States.4 A second very important risk factor for stroke is cardiac disease. Patients with coronary artery disease, congestive heart failure, left ventricular hypertrophy, and especially atrial fibrillation are at increased risk of stroke.8 In fact, the presence of atrial fibrillation is one of the most potent risk factors for ischemic stroke, with stroke rates from 5% to 20% per year depending on the patient’s comorbid conditions.9 Other known risk factors for atherosclerosis are also known to place patients at risk of stroke. Diabetes mellitus, dyslipidemia, and cigarette smoking are known atherogenic states that lead to cerebrovascular disease and ischemic stroke.9
PATHOPHYSIOLOGY
Ischemic Stroke
Ischemic stroke results from an occlusion of a cerebral artery, leading to a reduction in cerebral blood flow. The pathophysiologic mechanisms of ischemic stroke are given in Figure 10-1. Normal cerebral blood flow averages 50 mL/100 g per minute, and this is maintained over a wide range of blood pressures (mean arterial pressures of 50 to 150 mm Hg) by a process called cerebral autoregulation. Cerebral blood vessels dilate and constrict in response to changes in blood pressure, but this process can be impaired by atherosclerosis, chronic hypertension, and acute injury, such as stroke. Arterial occlusion leads to severe reductions in cerebral blood flow leading to infarction. Tissue that is ischemic but maintains membrane integrity is referred to as the ischemic penumbra because it usually surrounds the infarct core. This penumbra is potentially salvageable through therapeutic intervention.
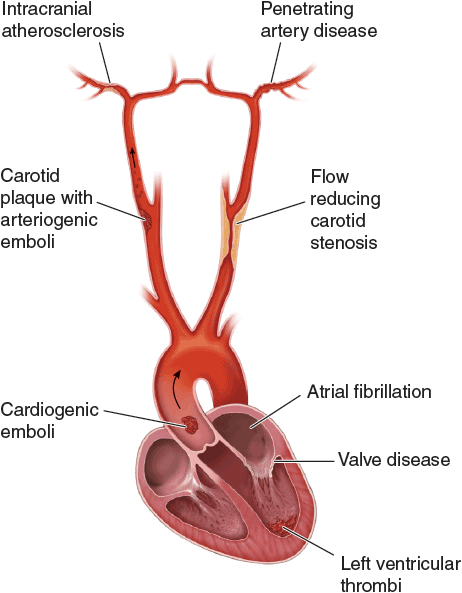
FIGURE 10-1 Pathophysiology of ischemic stroke. Diagram illustrating the three major mechanisms underlying ischemic stroke including occlusion of an intracranial vessel by an embolus that arises from a distant site (e.g., cardiogenic embolus), in situ thrombosis of an intracranial vessel, typically affecting the small penetrating arteries, and hypoperfusion caused by flow-limiting stenosis of a major extracranial artery. (Reproduced with permission from Longo DL, Fauci AS, Kasper DL, et al. Harrison’s Principals and Practice of Internal Medicine, 18th ed. New York: McGraw-Hill, 2012.)
Reduction in the provision of nutrients to the ischemic cell eventually leads to depletion of the high-energy phosphates (e.g., adenosine triphosphate [ATP]) and accumulation of extracellular potassium, intracellular sodium, and water, leading to cell swelling and eventual lysis. The increase in intracellular calcium that follows results in the activation of lipases, proteases, and endonucleases and the release of free fatty acids from membrane phospholipids. In addition, there is a release of excitatory amino acids, such as glutamate and aspartate, that perpetuates the neuronal damage and the accumulation of free fatty acids, including arachidonic acid, and results in the formation of prostaglandins, leukotrienes, and free radicals. In ischemia, the magnitude of free radical production overwhelms normal scavenging systems, leaving these reactive molecules to attack cell membranes and contribute to the mounting intracellular acidosis. All these events occur within 2 to 3 hours of the onset of ischemia and contribute to the ultimate cell death.10
Later targets for intervention in the pathophysiologic process involved after cerebral ischemia include inflammation and apoptosis, or programmed cell death, occurring many hours after the acute insult and can interfere with recovery and repair of brain tissue.10
Hemorrhagic Stroke
The pathophysiology of hemorrhagic stroke is not as well studied as that of ischemic stroke. However, it is known that the presence of blood in the brain parenchyma causes damage to the surrounding tissue through the mechanical effect it produces (mass effect) and the neurotoxicity of the blood components and their degradation products.5,6 Approximately 30% of ICHs continue to enlarge over the first 24 hours, most within 4 hours, and clot volume is the most important predictor of outcome, regardless of location.11,12 Hemorrhage volumes >60 mL are associated with 71% to 93% mortality at 30 days.5,6 Much of the early mortality of hemorrhagic stroke (up to 50% at 30 days) is caused by the abrupt increase in intracranial pressure that can lead to herniation and death.1 There is also evidence to support that both early and late edema contributes to worsened outcome after ICH.6
CLINICAL PRESENTATION Stroke
CLINICAL PRESENTATION (INCLUDING DIAGNOSTIC CONSIDERATIONS)
Stroke is a term used to describe an abrupt-onset focal neurologic deficit that lasts at least 24 hours and is of presumed vascular origin. A TIA is the same but lasts less than 24 hours and usually less than 30 minutes. The abrupt onset and the duration of the symptoms are determined through the history. The use of sensitive imaging techniques (magnetic resonance imaging [MRI] with diffusion-weighted imaging [DWI]) has revealed that symptoms lasting more than 1 hour and less than 24 hours are associated with infarction, making TIA and minor stroke clinically indistinguishable. The location of the CNS injury and its reference to a specific arterial distribution in the brain are determined through the neurologic examination and confirmed by imaging studies such as computed tomography (CT) scanning and MRI. The main arterial supply to the cerebral hemispheres is illustrated in Figure 10-2. Further diagnostic tests are performed to identify the cause of the patient’s stroke and to design appropriate therapeutic strategies to prevent further events.13
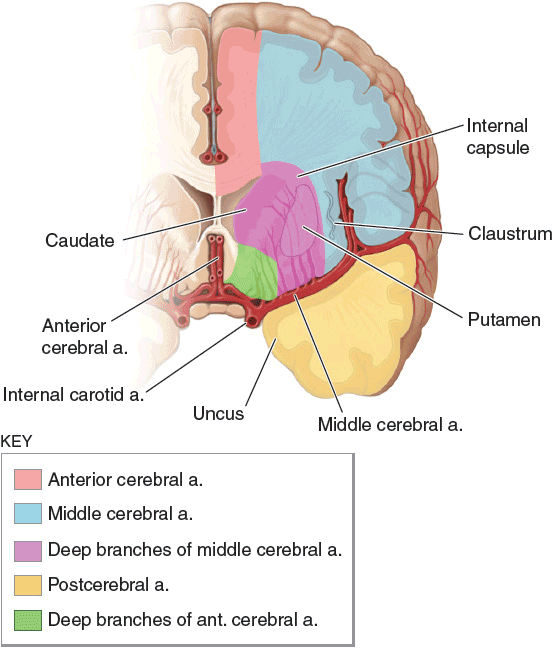
FIGURE 10-2 Diagram of a cerebral hemisphere in coronal section showing the territories of the major cerebral vessels branching from the internal carotid arteries. (Reproduced with permission from Longo DL, Fauci AS, Kasper DL, et al. Harrison’s Principals and Practice of Internal Medicine, 18th ed. New York: McGraw-Hill, 2012.)
TREATMENT
Stroke
Desired Outcomes
The goals of treatment of acute stroke are to (a) reduce the ongoing neurologic injury and decrease mortality and long-term disability, (b) prevent complications secondary to immobility and neurologic dysfunction, and (c) prevent stroke recurrence.14 Primary prevention of stroke is reviewed elsewhere.8
General Approach to Treatment
The initial approach to the patient with a presumed acute stroke is to ensure that the patient is supported from a respiratory and cardiac standpoint and to quickly determine whether the lesion is ischemic or hemorrhagic, based on a CT scan. Ischemic stroke patients presenting within hours of the onset of their symptoms should be evaluated for reperfusion therapy. ![]() TIAs also require urgent intervention to reduce the risk of stroke, which is known to be highest in the first few days after TIA.15 According to the American Stroke Association guidelines, patients with elevated blood pressure should remain untreated unless their blood pressure exceeds 220/120 mm Hg, or they have evidence of aortic dissection, acute myocardial infarction (AMI), pulmonary edema, or hypertensive encephalopathy. However, this level of blood pressure may be too high, and a number of clinical trials are currently testing more aggressive treatment of hypertension in the acute setting. If blood pressure is treated, short-acting parenteral agents, such as labetalol and nicardipine, or nitroprusside, are favored. Current recommendations regarding management of arterial hypertension in stroke patients are given in Table 10-2.14 In patients with SAH, if an aneurysm is found by angiography, endovascular coiling or clipping via a craniotomy should be performed to reduce the risk of rebleeding.16 In ICH, patients may require external ventricular drainage (EVD) if there is intraventricular blood and evolving hydrocephalus (enlargement of the ventricles). Once the patient is out of the hyperacute phase, attention is placed on preventing worsening, minimizing complications, and instituting appropriate secondary prevention strategies. The acute phase of the stroke includes the first week after the event.14
TIAs also require urgent intervention to reduce the risk of stroke, which is known to be highest in the first few days after TIA.15 According to the American Stroke Association guidelines, patients with elevated blood pressure should remain untreated unless their blood pressure exceeds 220/120 mm Hg, or they have evidence of aortic dissection, acute myocardial infarction (AMI), pulmonary edema, or hypertensive encephalopathy. However, this level of blood pressure may be too high, and a number of clinical trials are currently testing more aggressive treatment of hypertension in the acute setting. If blood pressure is treated, short-acting parenteral agents, such as labetalol and nicardipine, or nitroprusside, are favored. Current recommendations regarding management of arterial hypertension in stroke patients are given in Table 10-2.14 In patients with SAH, if an aneurysm is found by angiography, endovascular coiling or clipping via a craniotomy should be performed to reduce the risk of rebleeding.16 In ICH, patients may require external ventricular drainage (EVD) if there is intraventricular blood and evolving hydrocephalus (enlargement of the ventricles). Once the patient is out of the hyperacute phase, attention is placed on preventing worsening, minimizing complications, and instituting appropriate secondary prevention strategies. The acute phase of the stroke includes the first week after the event.14
TABLE 10-2 Blood Pressure Treatment Guidelines in Acute Ischemic Stroke Patients

Nonpharmacologic Therapy
Ischemic Stroke Surgical interventions in the acute ischemic stroke patient are limited. In less than 10% of patients with a large infarction in the middle cerebral artery territory, decompressive surgery to reduce intracranial pressure has been shown to significantly reduce mortality. However, the surgery must be performed within 48 hours of stroke onset to significantly improve functional outcome and this is at the cost of an increased number of surviving patients with severe disability.17 In cases of significant swelling associated with a cerebellar infarction, surgical decompression can be lifesaving. Beyond surgical intervention, however, the use of an organized, multidisciplinary approach to stroke care that includes early rehabilitation has been shown to be very effective in reducing the ultimate disability owing to ischemic stroke. In fact, the use of “stroke units” has been associated with outcomes similar to those achieved with early thrombolysis when compared with usual care.14
![]() In secondary prevention, carotid endarterectomy of an ulcerated and/or stenotic carotid artery is a very effective way to reduce stroke incidence and recurrence in appropriate patients and in centers where the operative morbidity and mortality are low. In fact, in ischemic stroke patients with 70% to 99% stenosis of an ipsilateral internal carotid artery, recurrent stroke risk can be reduced by up to 48% compared with medical therapy alone when combined with aspirin 325 mg daily.18 In patients less than 70 years of age, carotid stenting is a less invasive alternative and can be effective in reducing recurrent stroke risk.19 However, in patients with intracranial stenosis, aggressive medical management was shown to be superior to stenting in reducing recurrent stroke.20
In secondary prevention, carotid endarterectomy of an ulcerated and/or stenotic carotid artery is a very effective way to reduce stroke incidence and recurrence in appropriate patients and in centers where the operative morbidity and mortality are low. In fact, in ischemic stroke patients with 70% to 99% stenosis of an ipsilateral internal carotid artery, recurrent stroke risk can be reduced by up to 48% compared with medical therapy alone when combined with aspirin 325 mg daily.18 In patients less than 70 years of age, carotid stenting is a less invasive alternative and can be effective in reducing recurrent stroke risk.19 However, in patients with intracranial stenosis, aggressive medical management was shown to be superior to stenting in reducing recurrent stroke.20
Hemorrhagic Stroke In patients with SAH owing to a ruptured intracranial aneurysm, in AVMs, surgical intervention to either clip or ablate the offending vascular abnormality substantially reduces mortality owing to rebleeding.16 In the case of primary ICH, surgical evacuation appears to be of benefit if undertaken within 8 hours of onset and in patients with intermediate hemorrhage volumes (20 to 50 mL).12 Insertion of an EVD for hydrocephalus and subsequent monitoring of intracranial pressure are done commonly and are the least invasive of the procedures done in these patients.
Pharmacologic Therapy
Ischemic Stroke
Drug Treatments of First Choice: Published Guidelines The Stroke Council of the American Stroke Association and the American College of Chest Physicians have created and published guidelines that address the management of acute ischemic stroke.7,14 For acute treatment, the only two pharmacologic agents with class I recommendations are IV tissue plasminogen activator (tPA) within 4.5 hours of onset and aspirin within 48 hours of onset.7,14
![]() Early reperfusion (<4.5 hours from onset) with IV tPA has been shown to reduce the ultimate disability caused by ischemic stroke.21,22 Caution must be exercised when using this therapy, and adherence to a strict protocol is essential to achieving positive outcomes.14 The essentials of the treatment protocol can be summarized as (a) stroke team activation, (b) treatment as early as possible within 4.5 hours of onset, (c) CT scan to rule out hemorrhage, (d) meeting inclusion and exclusion criteria (Table 10-3), (e) administration of tPA 0.9 mg/kg over 1 hour, with 10% given as initial bolus over 1 minute, (f) avoidance of antithrombotic (anticoagulant or antiplatelet) therapy for 24 hours, and (g) close patient monitoring for elevated blood pressure, response, and hemorrhage.14
Early reperfusion (<4.5 hours from onset) with IV tPA has been shown to reduce the ultimate disability caused by ischemic stroke.21,22 Caution must be exercised when using this therapy, and adherence to a strict protocol is essential to achieving positive outcomes.14 The essentials of the treatment protocol can be summarized as (a) stroke team activation, (b) treatment as early as possible within 4.5 hours of onset, (c) CT scan to rule out hemorrhage, (d) meeting inclusion and exclusion criteria (Table 10-3), (e) administration of tPA 0.9 mg/kg over 1 hour, with 10% given as initial bolus over 1 minute, (f) avoidance of antithrombotic (anticoagulant or antiplatelet) therapy for 24 hours, and (g) close patient monitoring for elevated blood pressure, response, and hemorrhage.14
< div class='tao-gold-member'>




