Operative Treatment for Choledochal Cysts
Atsuyuki Yamataka
Yoshifumi Kato
Introduction
Choledochal cyst (CC), or dilatation of the common bile duct (CBD), was first reported by Douglas in 1852. The condition is relatively rare, with an estimated incidence in Western populations of 1 in 13,000 to 15,000 live births. However, it is far more common in the East, with rates as high as 1 per 1,000 live births having been described in Japan. Although the etiology remains unknown, CC is likely to be congenital. Pathologic features frequently include an anomalous junction of the pancreatic duct and CBD (pancreaticobiliary malunion: PBMU), intrahepatic bile duct (IHBD) dilatation with or without downstream stenosis, and various degrees of hepatic fibrosis.
Classification
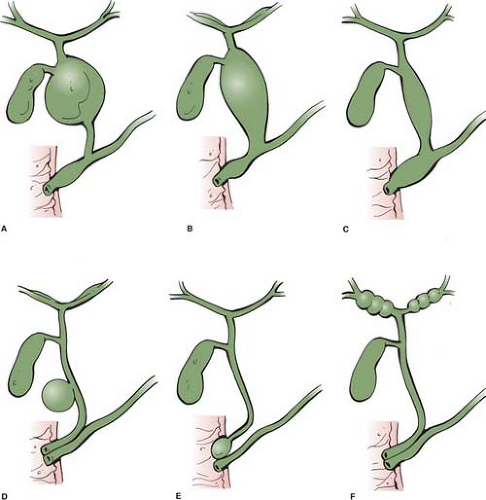
CC is usually classified into three groups, based on anatomy. However, other forms and subgroups have been described, based on cholangiographic findings of intrahepatic ducts or the presence of a long common duct shared by the liver and the pancreas or PBMU. Based on our experience, we prefer to classify CC into groups according to the presence or absence of PBMU (Fig. 1). The vast majority of CC is associated with PBMU. Thus, the following comments are related primarily to cystic (saccular), fusiform, and forme fruste choledochal cysts.
Malignancy
In all types of CC, bile duct mucosa shows erosion, epithelial desquamation, and papillary hyperplasia with regenerative atypia. Bile duct mucosa dysplasia without carcinoma can also be found frequently. In addition, metaplastic changes, such as mucous cells, goblet cells, and Paneth cells can also be seen. Hyperplasia and metaplasia increase with age and may progress to carcinoma in adult cases. An association between malignancy and CC was first reported in 1944. Since then, more than 100 cases of cholangiocarcinoma with CC have been reported, and the risk for developing carcinoma has been reported to range between 2.5% and 28%.
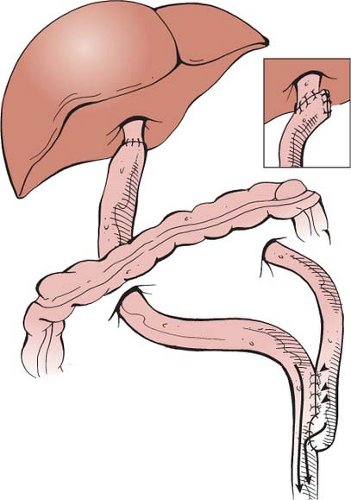
Cholangiocarcinoma has been documented in more than 10 patients younger than 20 years at the time of initial surgery for CC; the youngest case reported was an 11-year-old male. There are also case reports of malignances arising from the intrapancreatic terminal choledochus, hepaticojejunostomy anastomosis, and IHBD after primary cyst excision. Todani et al. reported a case of biliary carcinoma that developed 19 years after cyst excision and hepaticoduodenostomy. As a consequence of hepaticoduodenostomy, pancreatic enzymes can be easily and markedly activated by the presence of bile and enterokinase in intestinal secretions. Hepaticoduodenostomy has similar complications to those of internal drainage for CC and transduodenal sphincteroplasty for cholelithiasis, which have been reported to develop biliary carcinoma. Consequently, the authors recommend Roux-en-Y jejunostomy in order to eliminate any possible hazardous effect of activated pancreatic enzymes on bile duct mucosa. The authors have experienced two adults who died from cholangiocarcinoma, one at 54 years and the other at 29. The former patient had a cholecystectomy at the age of 32, then underwent secondary cyst excision and hepaticoenterostomy at the age of 48 and developed carcinoma in the dilated left IHBD. The latter patient underwent primary cyst excision at the age of 25 and carcinoma developed within the large residual intrapancreatic terminal choledochus. Both had exploratory laparotomies, and it seemed that persistent bile stagnation in the dilated IHBD could have been responsible for the carcinoma in the former patient, while the cause of carcinoma in the latter patient could not be determined. Continuous reflux of pancreatic secretions into the residual terminal choledochus, however, may have been the cause, because pancreatic secretions are known to injure the epithelium of the bile duct. If so, total excision of the intrapancreatic terminal choledochus could reduce the risk of malignancy.
CC can present at any age, but more than half of patients are initially seen within the first decade of life. Clinical manifestations differ according to the age at onset. Young infants may have obstructive jaundice, acholic stools, and hepatomegaly resembling biliary atresia, and may even have advanced liver fibrosis. But on surgical cholangiography, there is a patent communication with the duodenum and a well-developed IHBD tree. Young infants may also present with a large upper abdominal mass without jaundice. In young children, presenting symptoms can be divided roughly into two groups: right upper quadrant mass with intermittent jaundice due to biliary obstruction, seen in patients with saccular CC, and abdominal pain due to pancreatitis, which is characteristic of fusiform CC or forme fruste choledochal cysts. In adolescence and adulthood, CC has usually been misdiagnosed for many years as cholelithiasis, cirrhosis, portal hypertension, hepatic abscess, or biliary carcinoma. Surgical treatment in this group is much more difficult than in children, and the incidence of postoperative complications is quite high, even after primary cyst excision.
For thorough diagnosis of CC, it is important to identify dilatation of the extrahepatic bile duct as well as PBMU. Currently, abdominal ultrasonography (US) is probably the best screening method in patients who are suspected of having CC. US also clearly demonstrates IHBD dilatation and the state of the liver parenchyma. In recent years, CC has been detected at routine prenatal US as early as 15 weeks gestation. CC is typically cystic but not exclusively so. They can be mistaken for duodenal atresia, biliary atresia, ovarian cysts, duplication cysts, and mesenteric cysts. It has been suggested that cystic dilation of the CBD is a prenatal event, whereas fusiform dilation begins after birth.
Endoscopic retrograde cholangiopancreatography (ERCP) can accurately delineate the configuration of the pancreaticobiliary duct system in fine detail preoperatively; however, it is invasive and therefore unsuitable for repeated use and is contraindicated during acute pancreatitis.
Magnetic resonance cholangiopancreatography (MRCP) can provide excellent delineation of the pancreaticobiliary ducts, allowing detection of narrowing, dilatation, and filling defects with medium to high degrees of accuracy. MRCP is noninvasive and can also be used to assess the pancreatic and biliary ducts proximal to an obstruction. However, in children less than 3 years old, the pancreaticobiliary duct system may not be visualized clearly because of the small caliber of the ducts.
Percutaneous transhepatic cholangiography is also available, especially for patients with IHBD dilatation and severe jaundice, and intraductal US can delineate the distal parts of the CBD and pancreatic duct successfully.
Intraoperative cholangiography is unnecessary if the entire biliary system has been visualized preoperatively, but should be used if information about the pancreaticobiliary duct system is lacking.
Cyst excision is the definitive treatment of choice for CC because of the high morbidity and high risk for carcinoma associated with internal drainage, a commonly used treatment in the past. Recently, more attention has been paid to the treatment of conditions affecting the intrahepatic and intrapancreatic ducts, such as IHBD dilatation, focal stenosis, debris in the IHBD, and protein plugs or stones in the common channel. The best levels for transecting the common hepatic duct and excising the intrapancreatic bile duct are also highly controversial.
The Common Bile Duct
Usually more adhesions are found between saccular CC and the portal vein and hepatic artery than with forme fruste choledochal cysts, especially in older children. In adolescents and adults, adhesions are often very dense and great care is required during cyst excision.
Before excision, we always open the anterior wall transversely. After opening the anterior wall, the posterior wall is visible directly from the inside, facilitating the dissection of the portal triad. If the cyst is extremely inflamed and adhesions are very dense, mucosectomy of the cyst (Fig. 2) should be performed rather than attempting full-thickness dissection to minimize the risk for injuring the portal vein and hepatic artery. Even though the muscle layer is left intact, if the mucosa of the cyst is removed completely there will be no risk of malignancy.
The Distal Common Bile Duct
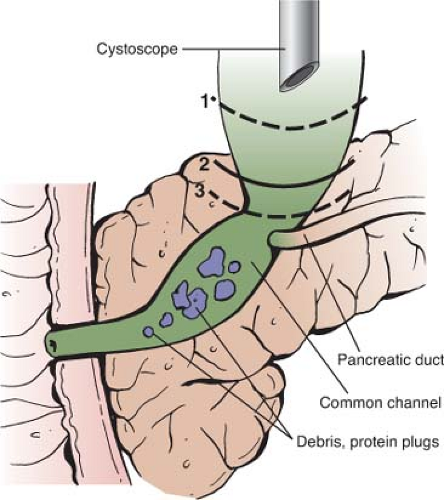
To prevent postoperative pancreatitis or stone formation, or both, in a residual cyst, the distal CBD should be resected as close as possible to the pancreaticobiliary ductal junction. In saccular CC, the distal CBD is sometimes so narrow that it cannot be identified and the likelihood of a residual cyst developing within the pancreas is low. In contrast, in forme fruste choledochal cysts, delineation of the diseased duct is more difficult, because the distal CBD is still wide at the pancreaticobiliary duct junction, and the likelihood of leaving some remnant of the CBD distally is high. If the distal CBD is resected along line 1 (Fig. 3), over time, a cyst will re-form around the distal CBD left within the pancreas, leading to recurrent pancreatitis, stone formation, or malignancy in the residual cyst. However, if the distal duct is resected along line 3 (see Fig. 3), that is, just above the pancreaticobiliary ductal junction, there is no residual duct within the pancreas and a cyst is unlikely to re-form.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree