http://evolve.elsevier.com/Edmunds/NP/
Irritable Bowel Syndrome
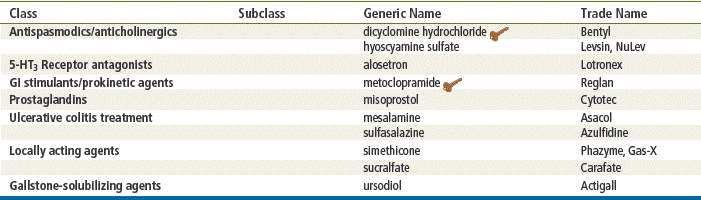
Antispasmodic agents (e.g., dicyclomine hydrochloride [Bentyl], hyoscyamine sulfate [Levsin]) are used primarily to treat patients with IBS and other functional GI disorders. A large number of antispasmodics are available on the market, but they are not used often. Only the two most common antispasmodic drugs are discussed in this chapter. Dicyclomine is used as the prototype.
Alosetron (Lotronex), a type 3 serotonin (5-HT3) antagonist, is available only through the Prescribing Program for Lotronex because of risk for ischemic colitis; this is not discussed in detail.
Therapeutic Overview of Irritable Bowel Syndrome
The pathophysiology of IBS is not fully understood, but bowel motility is affected. In normal bowel motility, segmenting contractions assist transit through the bowel. When these contractions increase, diarrhea occurs. When they decrease, constipation occurs. External factors include stress, psychologic factors, laxative abuse, food intolerance, and menstruation. Some evidence of inflammation in this process has been obtained.
Disease Process
IBS is a common chronic functional bowel disorder. Other names for IBS include spastic colitis, mucous colitis, nervous colitis, spastic colon, nervous colon, irritated colon, and unstable colon. Functional bowel disorders consist of combinations of chronic or recurrent GI symptoms that cannot be explained by structural or biochemical abnormalities. Generally, the diagnosis is a clinical one that is based on a cluster of symptoms combined with exclusion of a specific organic cause. Diagnostic criteria have been developed to make the diagnosis of IBS more consistent. The history of the patient is critical for diagnosis of IBS. Common symptoms include abdominal pain, altered bowel frequency and stool consistency (often alternating diarrhea and constipation), abdominal distention or bloating, and varying degrees of anxiety or depression. The new Rome III guidelines maintain that IBS of any subtype is characterized by a strong relationship between abdominal pain and defecation. These individuals have visceral hypersensitivity, or increased perception of gut-related events. In IBS with constipation (IBS-C), the onset of constipation generally corresponds with onset of pain at defecation. Patients with IBS-C may report abdominal pain, even if they empty their bowels regularly. The pain is described as sharp, burning, or cramping. The location is usually diffuse. A careful history is necessary to determine what the patient means by such words as “diarrhea,” “constipation,” and “regular.” Nocturnal diarrhea may indicate a serious problem. Patients may be classified into categories based on their predominant symptom: pain, constipation, or diarrhea. Care should be taken to rule out organic causes of symptoms such as celiac disease, lactose or fructose intolerance, and infectious processes.
Mechanism of Action
Treatment Principles
Standardized Guidelines for IBS
Evidence-Based Recommendations for IBS
Likely to be beneficial are the following:
 Psyllium fiber, certain antispasmodics, and peppermint oil are effective. See Table 31-2 for more on complementary and alternative therapies.
Psyllium fiber, certain antispasmodics, and peppermint oil are effective. See Table 31-2 for more on complementary and alternative therapies.TABLE 31-2
 Complementary and Alternative Products That May Have Interactions with Other Drugs
Complementary and Alternative Products That May Have Interactions with Other Drugs
| Condition | Product | Comments |
| Irritable bowel | Cat’s claw | Potential interaction with anticoagulants, aspirin, antiplatelet agents. May stimulate immune system. May protect against GI damage from NSAIDs. |
| Flaxseed | May slow down absorption of oral medications or other nutrients if taken at the same time. | |
| Grapefruit seed extract | Avoid concurrent administration of terfenadine, astemizole, cisapride; use other medications metabolized by the CYP 3A4 subsystem with caution. | |
| Evening primrose | Potential interaction with anticoagulants, aspirin, NSAIDs, antiplatelet agents; phenothiazines used to treat schizophrenia | |
| Peppermint | No known interactions | |
| Gallbladder/gallstones | Milk thistle Artichoke Goldenseal | No reported toxicities with any of these products |
| Gallbladder disease | Milk thistle Artichoke | No reported toxicities with either of these products |
Nonpharmacologic Treatment
Treatment of patients with IBS begins with patient education. The patient must be reassured that there is no organic cause for the symptoms. Teach that this is a chronic condition and that it will not lead to an organic problem.
Diet with adequate fiber is the cornerstone of treatment. Amounts of fiber and fluid usually have to be increased. Fiber should be increased gradually to avoid bloating. (See Chapter 28 for a list of high-fiber foods.) The patient should drink 6 to 8 glasses of water a day. The patient should identify and eliminate foods that cause symptoms. Foods that commonly cause problems include raw fruits and vegetables, high-fat foods, beverages such as carbonated beverages, coffee and other forms of caffeine, red wine and beer, and artificial sweeteners such as fructose and sorbitol. Exclude lactose intolerance.
Other important lifestyle changes include good bowel habits and exercise. See Chapter 28 for a discussion of bowel training. The best exercise is usually regular walking.
Pharmacologic Treatment
Treatment of patients with IBS varies with the severity and type of presenting symptoms, which usually occur as diarrhea or constipation. Patients who are experiencing symptoms that become lifestyle limiting should be prescribed a medication on a short-term basis and should be advised to modify diet and behavior and to participate in psychotherapy.
Antidepressants often are used over the long term to treat the patient with IBS and associated psychologic symptoms. TCAs have been used extensively. Through their effects on neurotransmitters, they are effective against abdominal pain. A common side effect is constipation, which makes them most useful in patients with diarrhea. SSRIs are used clinically but have shown inconsistent results. Paroxetine (Paxil) has been shown to be effective in improving bowel regularity but not in affecting pain. The other SSRIs do not have the mild anticholinergic effect that paroxetine has, and they may be more useful appropriate in patients with constipation.
How to Monitor
Patient Variables
Lower doses of antispasmodics should be prescribed to geriatric patients because this population may react with increased adverse effects such as agitation, excitement, confusion, or delusions.
Pediatrics
Safety and efficacy are not established. Hyoscyamine has been used in infant colic. Dicyclomine is contraindicated in infants younger than 6 months of age.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


 Key drug. Key drug chosen because dicyclomine has a lower incidence of side effects.
Key drug. Key drug chosen because dicyclomine has a lower incidence of side effects.